Clear Sky Science · en
NDUFA4L2 regulates the progression and chemotherapy sensitivity of HNSCC by inhibiting PANoptosis
Why this research matters
Chemotherapy is a lifeline for many people with head and neck cancers, yet tumors often learn to outsmart the drugs. This study uncovers how a single mitochondrial protein, NDUFA4L2, helps head and neck squamous cell carcinoma dodge the widely used drug cisplatin, and shows how switching this protein off can both kill cancer cells more effectively and wake up the immune system. The work points toward new ways to restore drug sensitivity by targeting how cancer cells burn sugar and die.
A stubborn cancer and a failing drug
Head and neck squamous cell carcinoma (HNSCC) is among the most common cancers worldwide and is often treated with cisplatin. Many tumors, however, become resistant, leaving patients with limited options. The authors focused on NDUFA4L2, a protein in the cell’s energy factories (mitochondria) that is switched on in low-oxygen conditions and alters how cells use fuel. By analyzing public single-cell datasets and examining patient tumor samples, they found that NDUFA4L2 is highly active in a distinct subgroup of tumor cells linked to poor survival. Tumors from patients whose cancers no longer responded to chemotherapy had especially high amounts of this protein, suggesting it plays a central role in resistance.
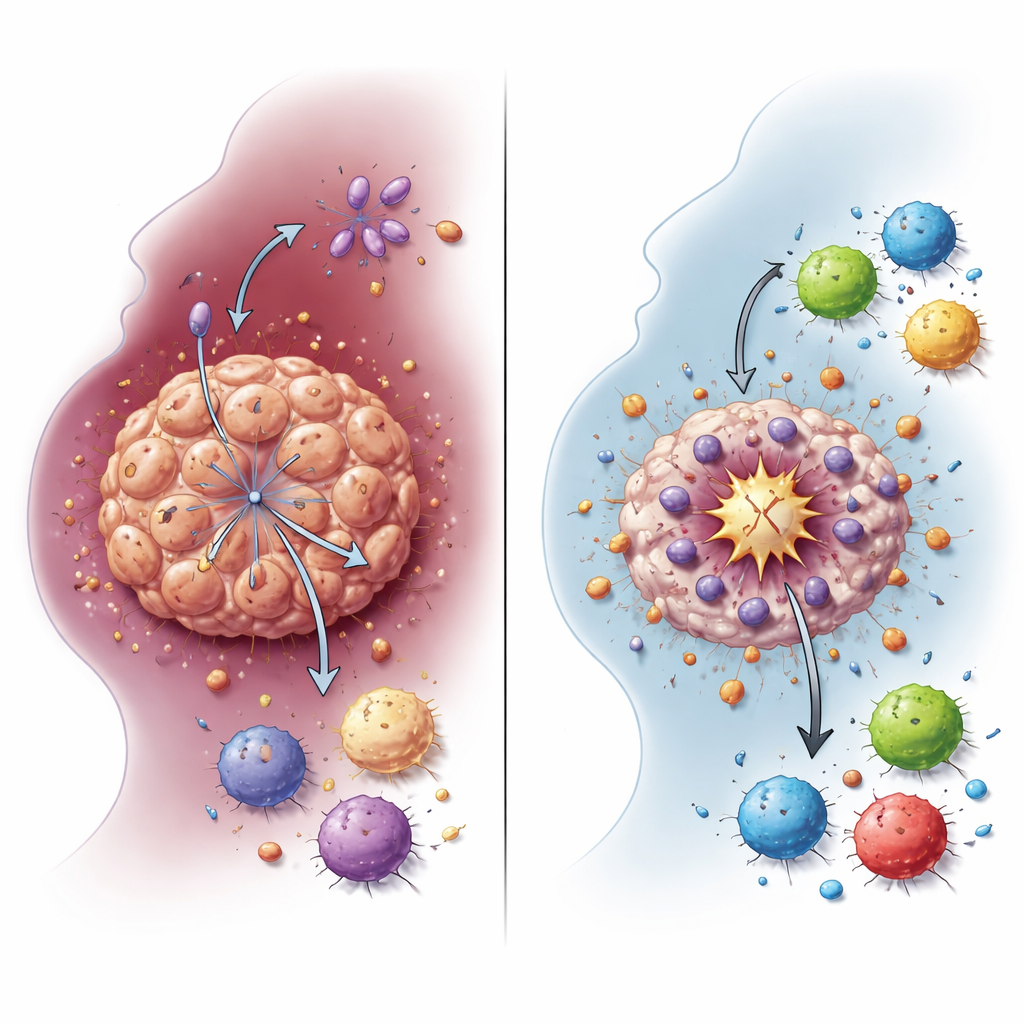
How a fuel switch shields tumor cells
Cancer cells often rely on a shortcut form of sugar burning called glycolysis, which produces large amounts of lactate even when oxygen is available. The team showed that NDUFA4L2 supports this glycolytic state in HNSCC cells. When NDUFA4L2 was removed from cell lines and from three-dimensional mini-tumors grown from patient samples, levels of lactate dropped sharply. Gene activity patterns shifted away from glycolysis and lactate metabolism, linking NDUFA4L2 directly to the cancer’s altered energy use. This fuel switch is not just a by-product of cancer growth: it turns out to be a shield that helps tumor cells survive cisplatin and avoid an especially potent form of cell death.
Forcing cancer cells into a triple death program
Cells can die through several regulated routes, including apoptosis, necroptosis, and pyroptosis. Recently, researchers have described PANoptosis, an integrated “all-in-one” death program that combines key parts of all three. In this study, knocking out NDUFA4L2 made HNSCC cells far more vulnerable to cisplatin. Under the microscope, treated cells showed telltale ballooning and rupture, and biochemical tests confirmed simultaneous activation of markers for apoptosis, necroptosis, and pyroptosis. Importantly, blocking any one pathway only partially rescued the cells, indicating that the full PANoptosis program was engaged. In mouse models of tongue tumors, removing NDUFA4L2 and giving cisplatin shrank tumors, extended survival, and boosted markers of this combined death response.
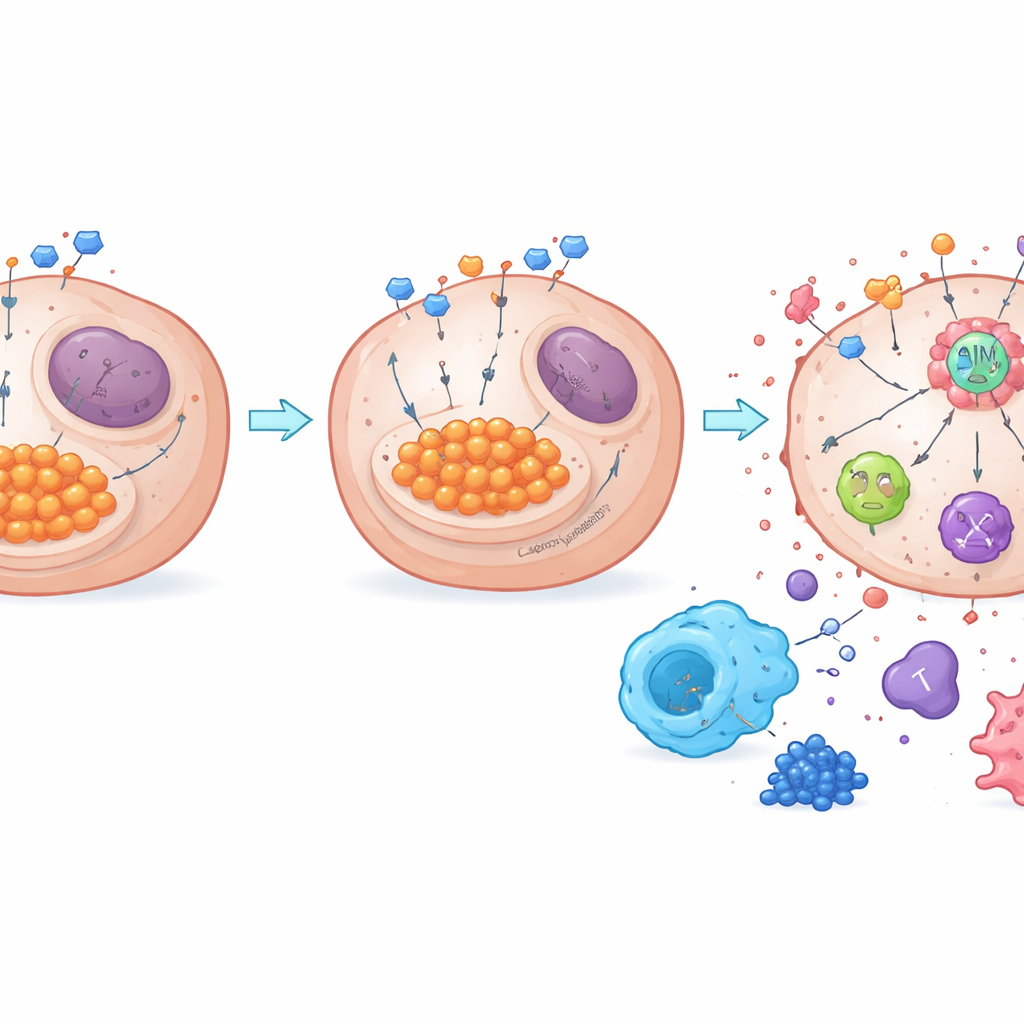
From sugar waste to immune awakening
The work also reveals how metabolism links to a key death-regulating sensor called AIM2. When glycolysis is high, excess lactate can chemically modify proteins in a process known as lactylation. The authors discovered that NDUFA4L2 keeps lactate levels high and promotes lactylation of AIM2, which appears to keep this sensor in a subdued state. Removing NDUFA4L2 lowered lactate, reduced AIM2 lactylation, and strengthened the assembly of an AIM2-based death complex that triggers PANoptosis. When AIM2 was experimentally reduced, the powerful killing effect of NDUFA4L2 loss plus cisplatin largely faded, confirming AIM2’s central role. In both mouse tumors and human samples, high NDUFA4L2 and lactylation were linked with more immunosuppressive macrophages and fewer cancer-fighting T cells, whereas blocking glycolysis or NDUFA4L2 shifted the balance toward a more active immune environment.
What this means for future treatments
To a lay observer, this study shows that certain head and neck cancers survive chemotherapy by rewiring how they use sugar and by muting a built-in self-destruct switch. By dialing down NDUFA4L2 or blocking glycolysis, the researchers were able to lower lactate, reactivate the AIM2 death sensor, trigger an aggressive triple-mode cell death program, and make cisplatin work better in cells, organoids, and mice. At the same time, the tumor’s surroundings became more welcoming to immune attack. These findings suggest that drugs aimed at NDUFA4L2, or at the metabolic and lactylation pathways it controls, could one day be combined with standard chemotherapy to overcome resistance and improve outcomes for patients with head and neck cancer.
Citation: Cui, JJ., Yang, Y., Zhao, JH. et al. NDUFA4L2 regulates the progression and chemotherapy sensitivity of HNSCC by inhibiting PANoptosis. npj Precis. Onc. 10, 154 (2026). https://doi.org/10.1038/s41698-026-01358-5
Keywords: head and neck cancer, chemotherapy resistance, cancer metabolism, programmed cell death, tumor microenvironment