Clear Sky Science · en
Bacterial protein-oleate complexes induce ferroptosis-like cell death in colorectal cancer cells by disrupting cell membranes and inhibiting the β-catenin-GPX4 axis
Turning Bacteria into Cancer Fighters
Colorectal cancer is one of the most common cancers worldwide and often learns to evade standard treatments. This study explores an unexpected ally in the fight against these tumors: a harmless bacterial protein that, when paired with a common fatty molecule, can selectively kill colorectal cancer cells. By understanding how this protein–fat complex attacks tumor cells while largely sparing healthy ones, researchers hope to open a new route to therapies that are both more effective and gentler on patients.
A New Weapon Built from Protein and Fat
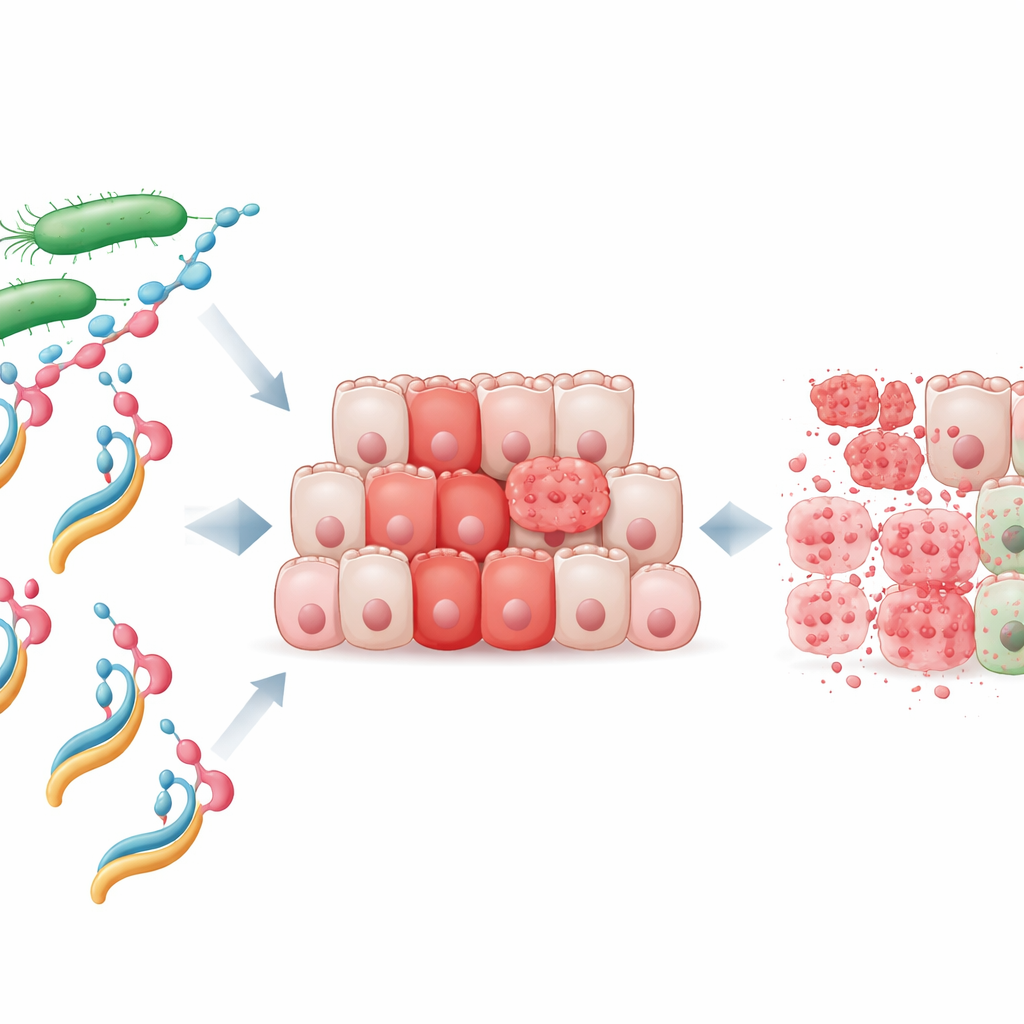
The researchers focused on a bacterial protein called NheA, which on its own is harmless and cannot even latch onto human cells. They mixed purified NheA with sodium oleate, a fatty acid–derived molecule, to create what they call the NheA–O complex. Similar human protein–fat complexes, such as the milk-derived HAMLET, are known to kill cancer cells, but until now no one had shown that a bacterial protein could be turned into a comparable tumor killer. Laboratory tests revealed that NheA–O rapidly reduced the survival of colorectal cancer cell lines, while the individual ingredients—protein or fat alone—had little effect. Importantly, normal colon cells were much less sensitive, suggesting that tumor cells have a special weakness that this complex can exploit.
Direct Attack on the Tumor Cell Surface
Using advanced imaging, the team watched how NheA–O behaves when it meets cancer cells. Labeled versions of the complex glowed strongly around the outer surface of tumor cells, showing that it binds tightly to their membranes. Three-dimensional images of cell clusters (spheroids) confirmed that NheA–O can penetrate deep into tumor-like structures. To isolate what happens at the surface, the researchers created giant membrane bubbles from cancer cells and exposed them to NheA–O. The complex clustered on these bubbles, shrank their area, and allowed normally excluded dye molecules to leak inside. Additional tests with artificial fat droplets made from tumor cell lipids showed that NheA–O caused progressive leakage, indicating that it physically destabilizes and perforates cancer cell membranes.
Shutting Down the Cell’s Power and Growth Programs
Once NheA–O disturbs the membrane, the damage spreads inward. The team found that treated cancer cells lost the electrical charge across their mitochondria—the tiny power plants inside cells—and their overall energy stores (ATP) dropped sharply, both in flat cultures and in 3D spheroids. At the same time, the complex weakened a central growth driver in colorectal cancer: the β‑catenin pathway. In patient data, high levels of β‑catenin and its partners are linked with poor survival. In the lab, NheA–O reduced the amount of β‑catenin in the nucleus, lowered its activity, and decreased the levels of its growth‑promoting targets. As a result, tumor cells formed fewer colonies, migrated more slowly, and built smaller, weaker spheroids—features that translate into reduced tumor expansion and spread.
Forcing a Rust-Like Death in Tumor Membranes
A key discovery of this work is that NheA–O triggers a special kind of cell death known as ferroptosis, which resembles a rusting process in the cell’s fats. The complex boosted levels of ACSL4, a protein that enriches membranes with vulnerable fatty building blocks, while lowering GPX4, a crucial “firefighter” enzyme that normally prevents these fats from oxidizing. As GPX4 levels fell, chemical markers of lipid damage in the membranes surged. Drugs that enhance ferroptosis made NheA–O even more lethal, whereas a ferroptosis blocker partially rescued the cells, reduced membrane damage, and restored some β‑catenin activity. Further experiments showed that NheA–O promotes tagging of GPX4 for destruction by the cell’s protein‑shredding machinery, and that cells already depleted of GPX4 were especially easy to kill.
What This Could Mean for Future Treatments
Taken together, the findings reveal a multi-pronged mode of action: NheA–O latches onto tumor cell membranes, disrupts their integrity, drains their energy factories, and forces a ferroptosis-like death by dismantling the protective GPX4 system and silencing β‑catenin–driven growth signals. Because it hits several vulnerabilities at once and largely spares normal colon cells in culture, this bacterial protein–fat complex emerges as a promising template for new colorectal cancer therapies. While these results come from carefully controlled cell models and will now need to be tested in animals and, eventually, humans, they broaden the concept that simple protein–lipid complexes—from milk or microbes—can be engineered into precise, potent anticancer agents.
Citation: Ullah, N., Yabrag, A., Ali, A. et al. Bacterial protein-oleate complexes induce ferroptosis-like cell death in colorectal cancer cells by disrupting cell membranes and inhibiting the β-catenin-GPX4 axis. Cell Death Discov. 12, 182 (2026). https://doi.org/10.1038/s41420-026-03097-9
Keywords: colorectal cancer, ferroptosis, bacterial protein, cell membrane disruption, GPX4 and β-catenin