Clear Sky Science · en
The ATC12 small molecule inhibits the Aurora-A/TPX2 interaction and impairs the proliferation of breast cancer cells
Why this research matters for future cancer treatments
Many cancer drugs try to shut down enzymes that drive cell division, but they often hit too many targets and cause side effects, or they fail to work well in patients. This study explores a different tactic: instead of turning an enzyme off, it aims to break up a specific partnership between two proteins that cooperate to help breast cancer cells grow and survive. The researchers discover and test a new small molecule, called ATC12, that interferes with this partnership and slows the growth of cancer cells, including cells taken directly from patients’ tumors.
A crucial partnership inside dividing cells
Inside our cells, an enzyme called Aurora-A helps orchestrate cell division. Another protein, TPX2, binds to Aurora-A, helps position it correctly on the cell’s internal scaffolding, and stabilizes it. Together they form a functional pair that is often found at abnormally high levels in tumors, including breast cancers. Beyond its role in cell division, Aurora-A can accumulate in the nucleus of non-dividing cancer cells, where it boosts genes that favor tumor growth and spread. Evidence suggests that TPX2 also helps Aurora-A reach the nucleus. Traditional drugs that block Aurora-A’s activity by competing with ATP have shown limited success in clinical trials, partly because the ATP-binding site looks similar in many enzymes, leading to off-target effects. This has pushed researchers to look for more selective ways to curb Aurora-A’s cancer-promoting roles.

Designing a molecule to break a protein bond
The team used computer-based screening to search millions of purchasable molecules for candidates that could fit into the contact region where TPX2 binds Aurora-A. They focused on chemical features known to be crucial for this interaction, such as hydrophobic pockets and key binding “hot spots.” From an initial large pool, they narrowed the field to 184 compounds, and then to 15 top candidates that best matched the three-dimensional shape and chemistry of the interface. Laboratory tests using native mass spectrometry showed that four of these molecules could weaken the binding of a TPX2 fragment to Aurora-A. Further dose–response experiments identified two compounds, ATC7 and especially ATC12, as the most potent at displacing TPX2 from Aurora-A without blocking Aurora-A’s enzyme activity, indicating a specific effect on the partnership rather than on the catalytic site.
How ATC12 affects cancer cells and their behavior
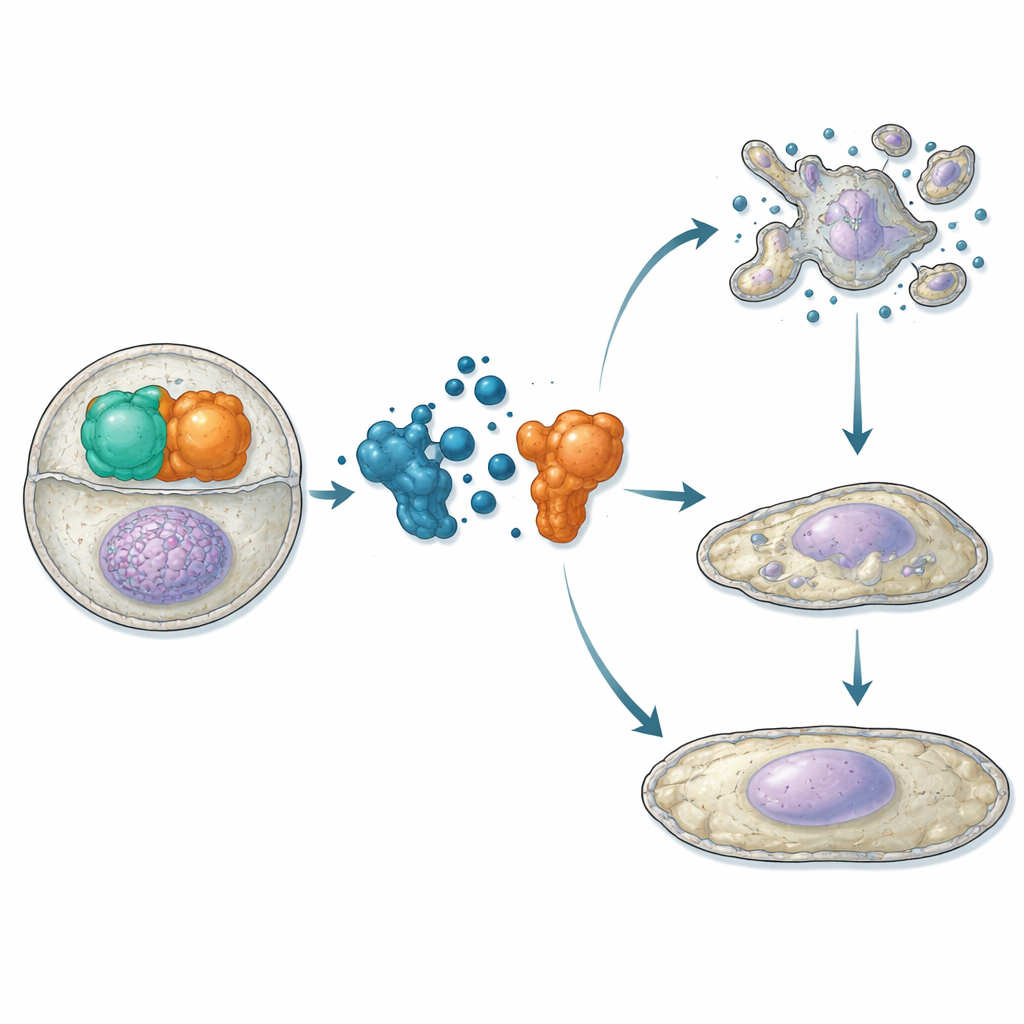
Having established that ATC12 binds Aurora-A and competes with TPX2 in vitro, the researchers moved to living cells. In osteosarcoma and breast cancer cell lines, they used proximity assays and microscopy to show that ATC12 treatment reduces the Aurora-A/TPX2 interaction both at the mitotic spindle and inside interphase nuclei, accompanied by decreased Aurora-A signal in these locations. In two breast cancer models—MCF7 (less aggressive, hormone receptor–positive) and MDA-MB-231 (highly aggressive, triple-negative)—ATC12 lowered cell viability in a dose-dependent manner, whereas a control compound that did not disrupt the interaction had no effect. Time-lapse imaging revealed that in MCF7 cells ATC12 greatly reduced the fraction of cells entering mitosis, prolonged the duration of mitosis for those that did divide, and led to extensive cell death with biochemical signs of apoptosis. In contrast, MDA-MB-231 cells showed slowed proliferation without significant death; instead, they exhibited increased levels of the cell-cycle brake p21, enlarged nuclei, and activation of senescence markers, indicating a shift into a permanent non-dividing state.
Testing ATC12 in 3D models and patient-derived organoids
To better mimic the behavior of tumors in the body, the scientists examined ATC12 in three-dimensional cultures. When breast cancer cells were grown as mammospheres—spherical clusters that enrich for stem-like, therapy-resistant cells—ATC12 reduced both their viability and size in both MCF7 and MDA-MB-231 backgrounds, whereas a standard Aurora-A kinase inhibitor did not shrink the spheres. The team then moved to organoids grown from biopsies of triple-negative breast cancer patients whose tumors had resisted chemotherapy. In these patient-derived organoids, ATC12 decreased cell survival in a clear dose-dependent fashion, with effective concentrations in the low micromolar range. Repeating the drug dose mid-treatment further enhanced the effect, suggesting that maintaining ATC12 levels over time may be important for sustained disruption of the Aurora-A/TPX2 complex.
What this means for cancer therapy
This work supports the idea that breaking specific protein partnerships can be a powerful way to disarm cancer cells while avoiding some pitfalls of traditional enzyme inhibitors. By targeting the Aurora-A/TPX2 complex, ATC12 interferes with both dividing and non-dividing cancer cells, provoking either cell death or stable senescence depending on the tumor’s genetic makeup. Its ability to impair growth in 3D mammospheres and in organoids from hard-to-treat triple-negative breast cancers highlights its promise as a starting point for new drugs, including refined molecules or degraders built on the same scaffold. While further optimization is needed to improve potency and stability, the study demonstrates that selectively disrupting the Aurora-A/TPX2 pair is a realistic and potentially valuable strategy for future anti-cancer treatments.
Citation: Boi, D., Fianco, G., Polverino, F. et al. The ATC12 small molecule inhibits the Aurora-A/TPX2 interaction and impairs the proliferation of breast cancer cells. Cell Death Dis 17, 356 (2026). https://doi.org/10.1038/s41419-026-08579-3
Keywords: Aurora-A, TPX2, breast cancer, protein–protein interaction inhibitor, organoids