Clear Sky Science · en
Reprogramming the tumor microenvironment with antibody against membrane-proximal AXL to overcome immune checkpoint blockade resistance
Why some tumors hide from the immune system
Cancer immunotherapy has transformed treatment for many patients, but it still fails in a large fraction of tumors that the immune system barely notices. These so-called “cold” tumors contain few attacking immune cells and often resist today’s powerful checkpoint drugs. This study explores a new kind of antibody that wakes up the body’s first-line defenses inside such tumors, helping turn a cold, silent cancer into one that is swarming with tumor-killing immune cells.
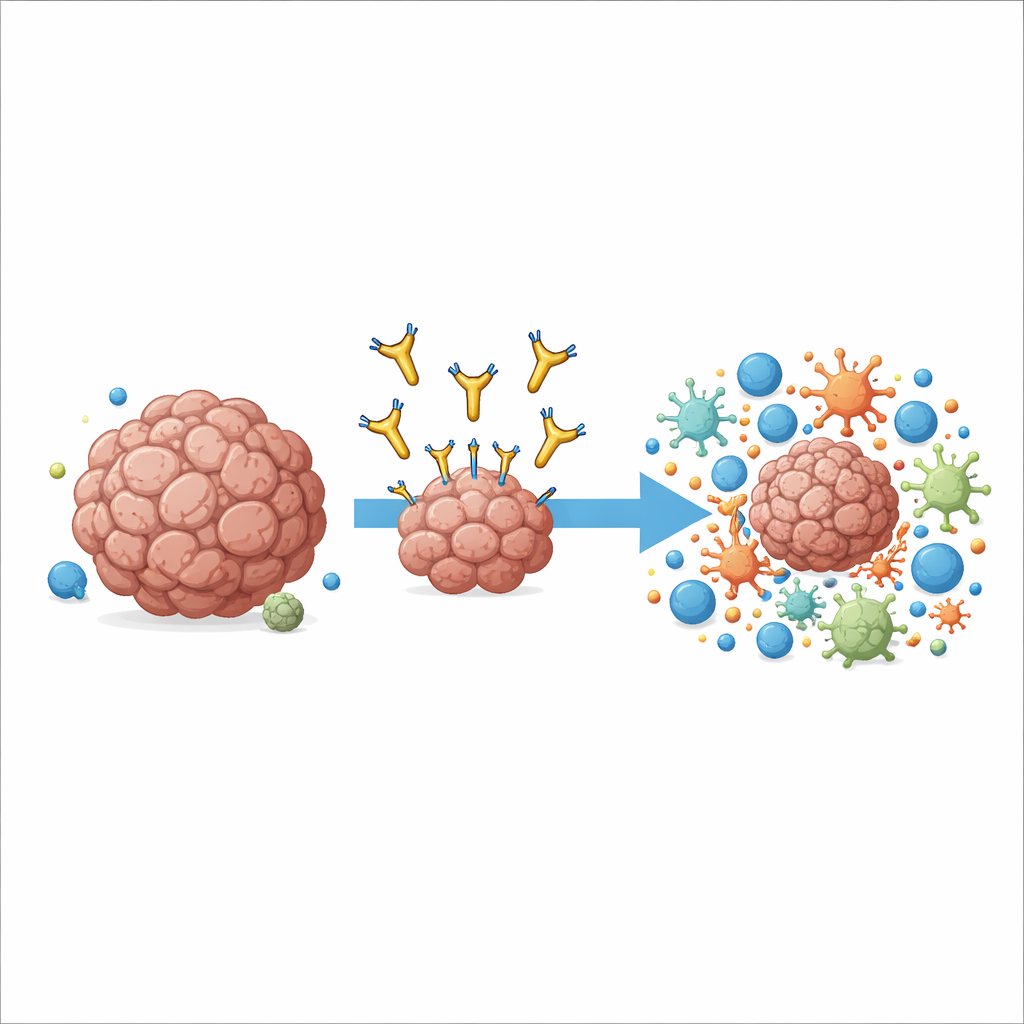
A new way to aim at a familiar cancer target
The work centers on a molecule called AXL, which sits on the surface of many cancer cells and some immune cells in the tumor. High AXL levels are linked to aggressive disease, spread to other organs, and resistance to standard immunotherapies. Earlier drugs tried to block AXL’s growth signal by latching onto its outermost tip, but they showed only modest benefits in clinical trials and sometimes caused side effects. The authors took a different approach: they built an antibody, named 6C5, that grabs AXL very close to the cell membrane instead of at the distant tip. This subtle shift in docking position turned out to be crucial for how the immune system could use the antibody as a handle.
Recruiting the body’s garbage collectors
Rather than directly poisoning cancer cells, 6C5 works by calling in and redirecting immune cells that specialize in engulfing and processing debris, especially macrophages and certain dendritic cells. In mouse models of melanoma and colon cancer engineered to carry human AXL, 6C5 powerfully slowed or even shrank tumors, including lung metastases, but only when tumor cells displayed AXL. The antibody had little effect in mice lacking T and B cells, showing that lasting tumor control depended on a full adaptive immune response. Detailed single-cell analyses of treated tumors revealed that 6C5 dramatically increased the number and activity of macrophages, dendritic cells, and killer T cells infiltrating the cancer mass, converting a sparse immune desert into a crowded battlefield.
How antibody-guided cleanup sparks wider immune attack
Mechanistic experiments showed that 6C5’s success hinges on how it tethers macrophages to tumor cells. By binding AXL close to the membrane, 6C5 forms compact clusters that macrophage receptors can grip efficiently, boosting a process called antibody-dependent cellular phagocytosis. Macrophages more readily swallowed antibody-coated tumor cells when 6C5 was present, but not when its tail region was altered to prevent engagement of macrophage receptors. This engulfment triggered production of type I interferons—potent alarm molecules—through a pathway that relied on the adaptor protein MyD88. These interferons, in turn, activated dendritic cells, increased their ability to present tumor fragments, and encouraged their migration to lymph nodes. There, they primed waves of cytotoxic CD8+ T cells, particularly a highly active subset marked by strong effector molecules, which then returned to the tumor to attack.
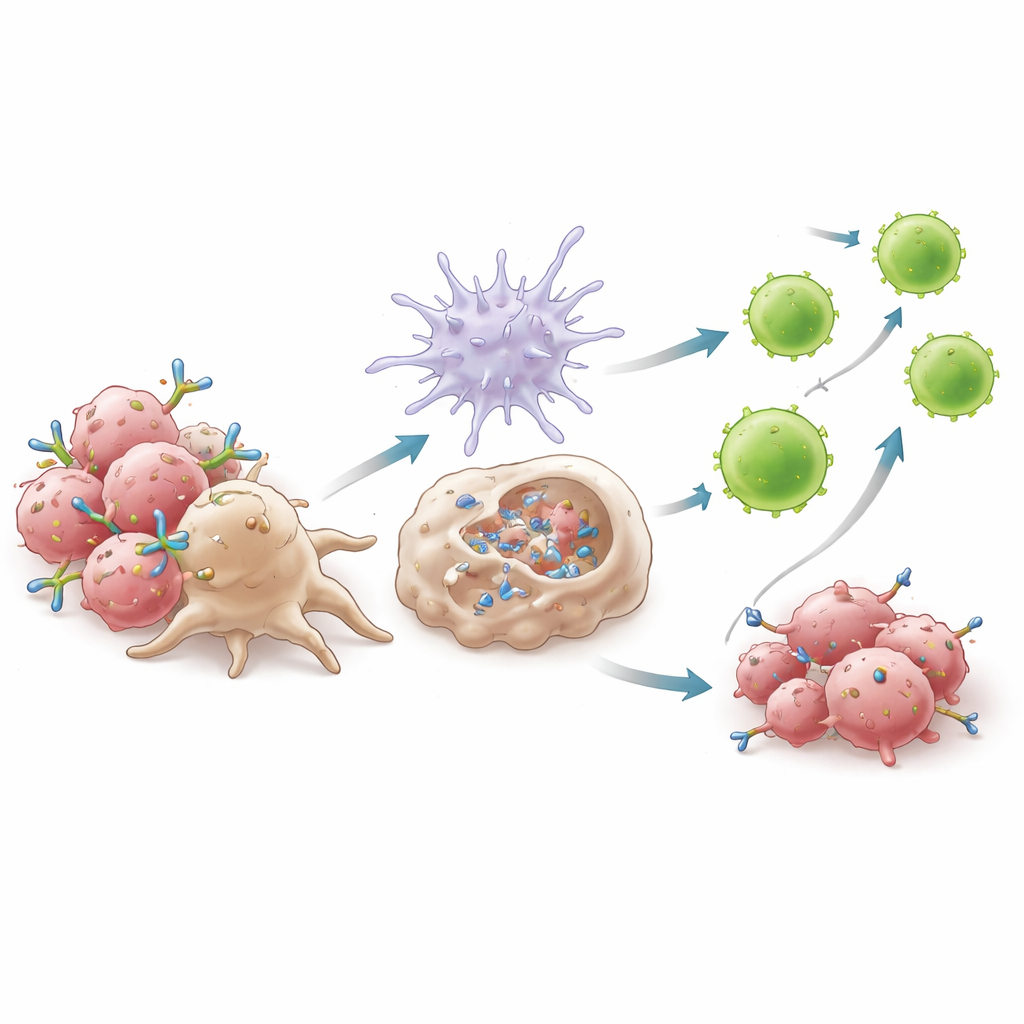
Unmasking a hidden brake within helper T cells
While 6C5 stirred a vigorous anti-tumor response, it also revealed an unexpected form of immune self-sabotage. The treatment expanded a population of CD4+ T cells that did not carry the classic Treg marker Foxp3 but behaved in a similarly suppressive way. These cells expressed very high levels of checkpoint molecules such as PD-1 and CTLA-4, produced less of the growth factor IL-2, and made more immunosuppressive signals. Depleting all CD4+ T cells enhanced tumor control but sacrificed long-term immune memory, underscoring that not all helper cells are harmful. Instead, the authors targeted this “Treg-like” PD-1–high subset indirectly. Combining 6C5 with dual checkpoint blockade (anti–PD-1 plus anti–CTLA-4) selectively reduced these suppressive cells in tumors, while preserving beneficial T cells and further improving tumor control.
Building durable protection with combination therapy
Because both Tregs and these PD-1–high helper cells are hungry consumers of IL-2, the team also tested a next-generation drug that couples a modified IL-2 signal to PD-1, focusing its action on exhausted tumor-infiltrating T cells. When 6C5 was paired with this PD-1–targeted IL-2 fusion, about half the mice cleared their tumors completely. Remarkably, all cured animals rejected a later tumor rechallenge, indicating robust and lasting immune memory. In contrast, simply removing CD4+ T cells lacked this durable protection. Together, these results show that tuning rather than wiping out the CD4+ compartment can unleash strong anti-cancer immunity without undermining the immune system’s ability to “remember” the tumor.
What this could mean for future cancer treatment
This study demonstrates that where an antibody binds on a tumor molecule can fundamentally change how it enlists the immune system. By targeting a membrane-proximal site on AXL, 6C5 acts less like a signal blocker and more like an immune amplifier—fueling macrophage cleanup, interferon alarms, dendritic cell activation, and potent killer T-cell attacks. At the same time, the work exposes new, non-classical suppressor T cells that emerge during therapy and shows how tailored combinations with checkpoint inhibitors or IL-2–based agents can neutralize these brakes. If similar antibodies and strategies prove safe and effective in humans, they may offer a way to convert stubborn immune-cold tumors into immune-hot ones that finally respond to immunotherapy.
Citation: Yang, Z., Cao, S., Zhang, J. et al. Reprogramming the tumor microenvironment with antibody against membrane-proximal AXL to overcome immune checkpoint blockade resistance. Sig Transduct Target Ther 11, 139 (2026). https://doi.org/10.1038/s41392-026-02664-x
Keywords: cancer immunotherapy, tumor microenvironment, AXL antibody, macrophage phagocytosis, immune checkpoint resistance