Clear Sky Science · en
Sphingosine-1-Phosphate-derived 2-Hexadecenal is a central mediator of ocular neovascularization by inhibiting Sphingosine-1-Phosphate receptor 5
Why this study matters for eyesight
Vision loss from diseases like diabetic eye disease often comes from the growth of fragile, leaky blood vessels in the retina at the back of the eye. Current treatments can save sight, but they are expensive, invasive, and do not work for everyone. This study uncovers a previously hidden chemical culprit and a new target molecule on immune cells that together drive this harmful vessel growth, opening a possible path to safer, pill-like therapies in the future.
A hidden troublemaker made from a helpful fat
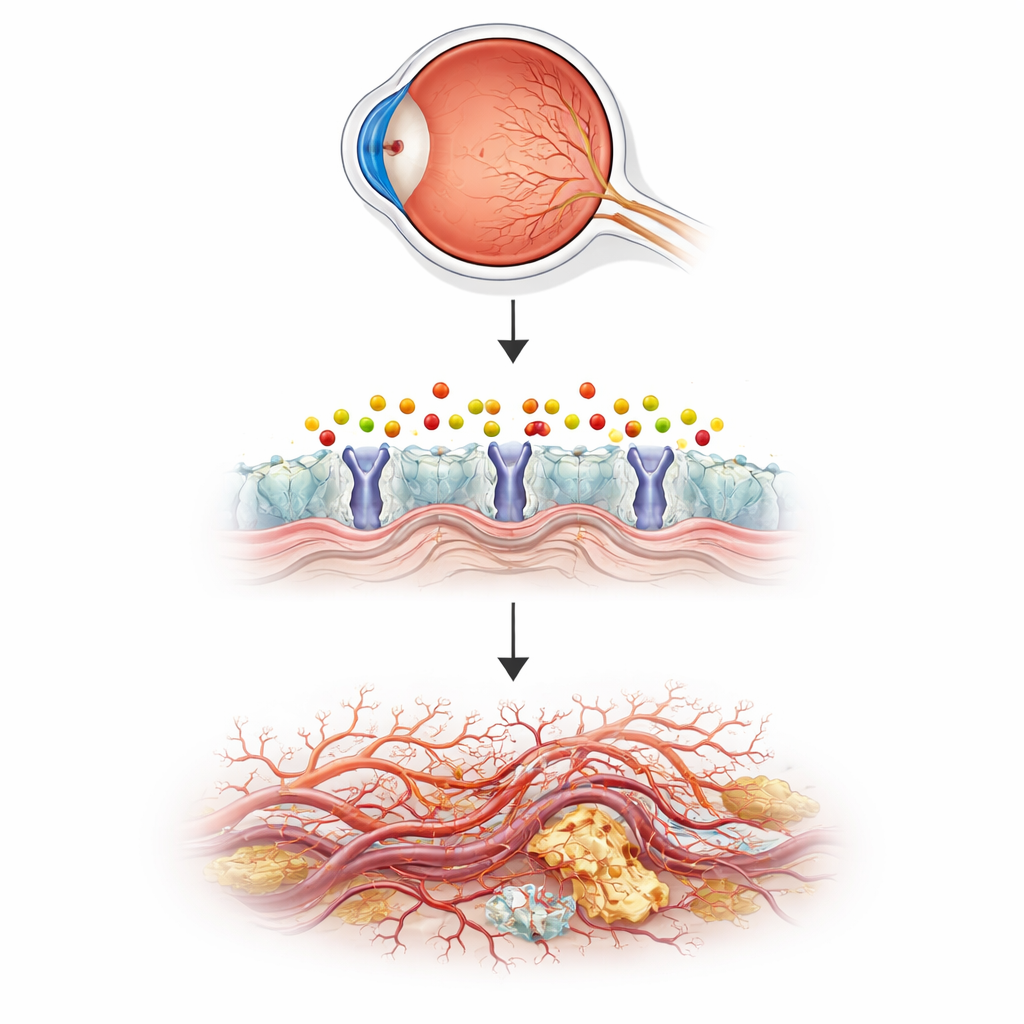
The story starts with a fat-like messenger called sphingosine‑1‑phosphate (S1P). S1P normally helps keep blood vessels stable and leak‑resistant, and drugs that act on its receptors are already used in diseases like multiple sclerosis. But when S1P is broken down, it can form a reactive by‑product called 2‑hexadecenal, a small, unstable aldehyde. Until now, almost nothing was known about what this by‑product does in living blood vessels, especially in the eye. The authors suspected that if 2‑hexadecenal is not cleared away properly, it might damage cells and disturb the fine network of vessels that nourishes the light‑sensing retina.
Using tiny fish to model sick human eyes
To test this idea, the team turned to zebrafish, a small aquarium fish whose transparent embryos let scientists directly watch blood vessels as they form. They disabled a gene called aldh3b1, which makes an enzyme that detoxifies 2‑hexadecenal, and followed vessel growth in the eye. Fish lacking this enzyme developed too many fine sprouts and branching vessels in the retina, in a pattern similar to early human disease, while larger body vessels stayed normal. When normal fish were simply bathed in 2‑hexadecenal, their eye vessels overgrew in the same way. A natural molecule called carnosine, which can soak up reactive aldehydes, reversed these changes, tying the abnormal growth directly to buildup of this single lipid‑derived chemical.
Iron imbalance and a fiery form of cell death
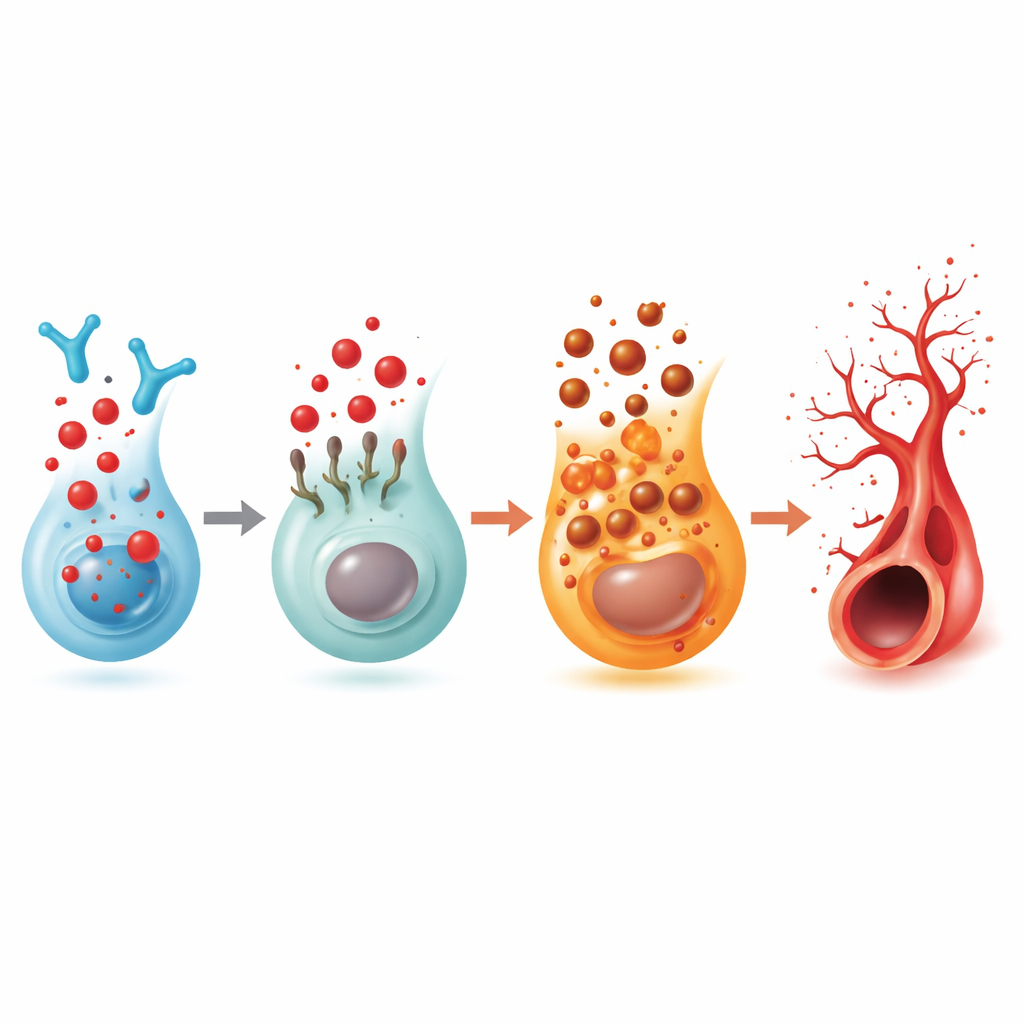
The researchers then asked how this small molecule could so powerfully reshape vessels. By combining gene‑activity profiling and detailed chemical analysis, they found that excess 2‑hexadecenal disrupted how cells handle iron and pushed them toward ferroptosis, a recently recognized, iron‑driven form of cell death marked by runaway fat oxidation. Markers of lipid damage and iron overload rose in the fish eyes, while key protective systems that normally stop ferroptosis, including a protein called FSP1 and the antioxidant enzyme GPX4, were dialed down. Blocking ferroptosis with a specialized inhibitor eased the abnormal vessel growth, while directly blocking FSP1 mimicked the disease‑like changes, placing this pathway at the center of the damage.
A receptor switch linking fat signals, immune cells, and vessels
Because 2‑hexadecenal comes from S1P, the team examined S1P’s five known receptors. Only one, called S1PR5, consistently dropped in the fish eyes when 2‑hexadecenal built up. Knocking down S1PR5 alone caused the same excess sprouting, and at the same time lowered FSP1, tying this receptor to the ferroptosis brake. A selective S1PR5‑activating drug restored more normal vessel patterns in both 2‑hexadecenal‑treated and enzyme‑deficient fish. Biophysical and computer‑modeling work showed that 2‑hexadecenal can bind directly to S1PR5 and trigger its internalization into cells, weakening its surface signal. In human single‑cell retina data, S1PR5 was found mainly on natural killer (NK) immune cells, and in samples from patients with advanced diabetic eye disease, S1PR5 levels were markedly higher while related pathways involving sphingolipids, immune signaling, and ferroptosis were altered in ways that match the zebrafish findings.
What this could mean for people with diabetic eye disease
Taken together, the study paints a simple but powerful picture: when the enzyme ALDH3B1 cannot clear the S1P‑derived aldehyde 2‑hexadecenal, this reactive by‑product disturbs the S1PR5 signal on immune cells, weakens an internal defense system against iron‑driven damage, and helps trigger a form of “rust‑like” cell death that encourages tangled, fragile vessels to invade the retina. Because S1PR‑targeting drugs already exist and some can be taken by mouth, this newly mapped 2‑hexadecenal–S1PR5–ferroptosis axis offers a plausible route to future treatments that might slow or prevent vision loss in diabetic retinopathy with fewer injections into the eye.
Citation: Qian, X., Ge, R., Chu, Y. et al. Sphingosine-1-Phosphate-derived 2-Hexadecenal is a central mediator of ocular neovascularization by inhibiting Sphingosine-1-Phosphate receptor 5. Nat Commun 17, 3488 (2026). https://doi.org/10.1038/s41467-026-71792-3
Keywords: diabetic retinopathy, retinal blood vessels, lipid signaling, ferroptosis, sphingosine-1-phosphate receptor