Clear Sky Science · en
Association between FTO rs9939609 genotype and breast cancer risk after bariatric surgery in the Swedish Obese Subjects study
Why genes, weight loss surgery, and breast cancer matter
Many women know that excess body weight can raise the chance of developing breast cancer, and that major weight loss may lower that risk. But not everyone benefits in the same way. This study asks a simple but important question: does a common gene variant help determine which women gain the most cancer protection from bariatric (weight loss) surgery?
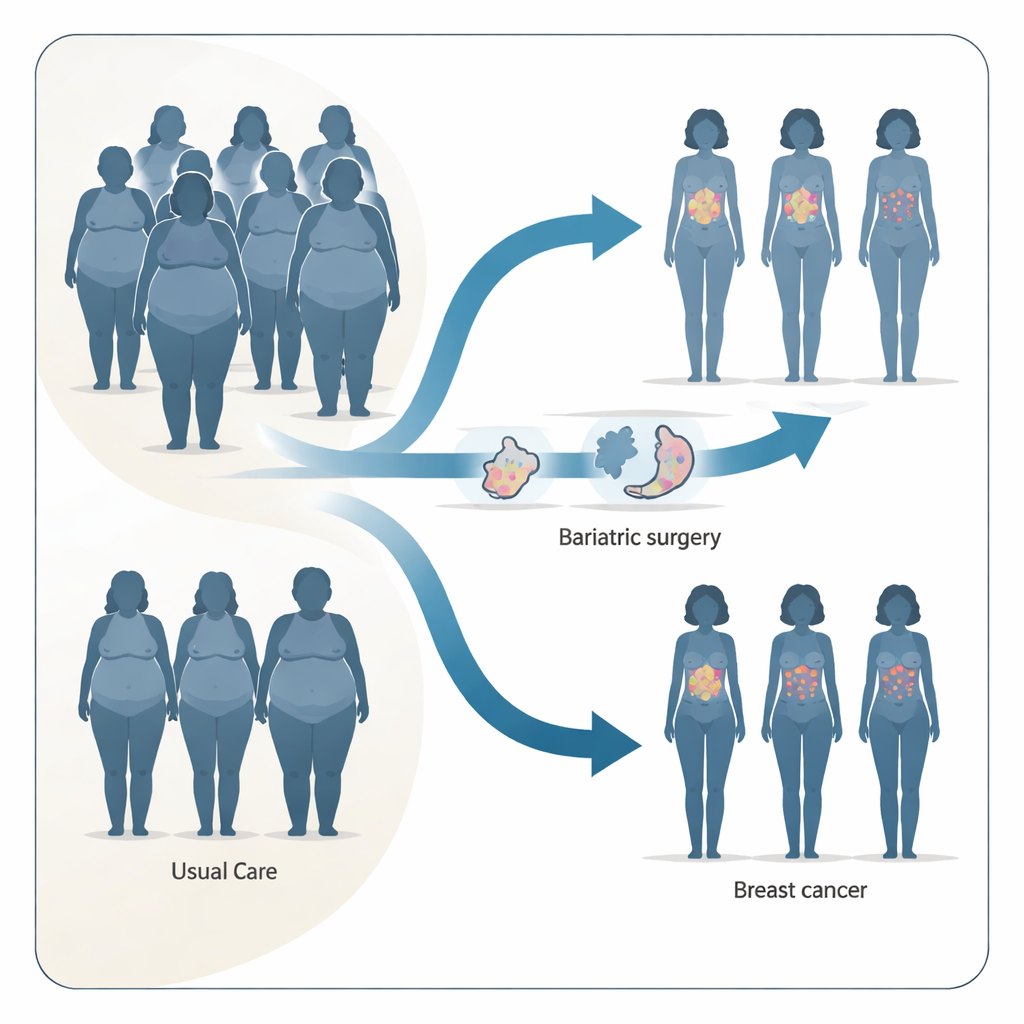
A long-term look at women with severe obesity
The research drew on the Swedish Obese Subjects study, a large, long-running project that has followed thousands of adults with severe obesity for up to 33 years. For this analysis, the scientists focused on 2596 women, roughly half of whom chose bariatric surgery while the others received usual non-surgical care. Over more than two decades, the team tracked who developed breast cancer, using Sweden’s national cancer registry, which reliably captures nearly all cancer cases in the country.
A common gene difference tied to weight and cancer
The spotlight of the study is a small DNA change in a gene called FTO, which has been repeatedly linked to higher body weight, larger food intake, and conditions like type 2 diabetes. This particular variation, known as rs9939609, comes in two versions. Women can have no copies of the so-called risk version (TT), one copy (TA), or two copies (AA). Earlier work suggested that carrying the A version might slightly raise breast cancer risk, but past studies mainly compared women with and without cancer at a single point in time and did not look at what happens after large, intentional weight loss.
Who benefited most from weight loss surgery?
Over a median of almost 24 years of follow-up, 135 women developed breast cancer. When the researchers compared surgery with usual care, they found that bariatric surgery was clearly linked to fewer breast cancers among women who carried at least one copy of the A version of the FTO variant. In these women, surgery was associated with roughly half the risk of breast cancer compared with similar women who did not have surgery, even after accounting for age, starting weight, smoking, and alcohol use. In contrast, among women with the TT version, bariatric surgery did not show a meaningful reduction in breast cancer risk compared with usual care.
The added role of insulin and metabolism
The team also examined fasting insulin levels, a marker related to how the body handles blood sugar and a possible driver of cancer growth. They divided women into those with insulin levels above or below the group’s median at the start of the study. Among women with both high starting insulin and at least one A version of the FTO variant, bariatric surgery was linked to an even stronger reduction in breast cancer risk, on the order of two-thirds lower than in similar women who did not have surgery. However, in women without the risk version of the gene, or in those with lower insulin levels, surgery did not show the same clear cancer benefit. Interestingly, when insulin levels were tracked over time, they improved after surgery in general, but did not differ meaningfully between the gene groups, suggesting that the gene’s influence may not simply work through insulin changes alone.
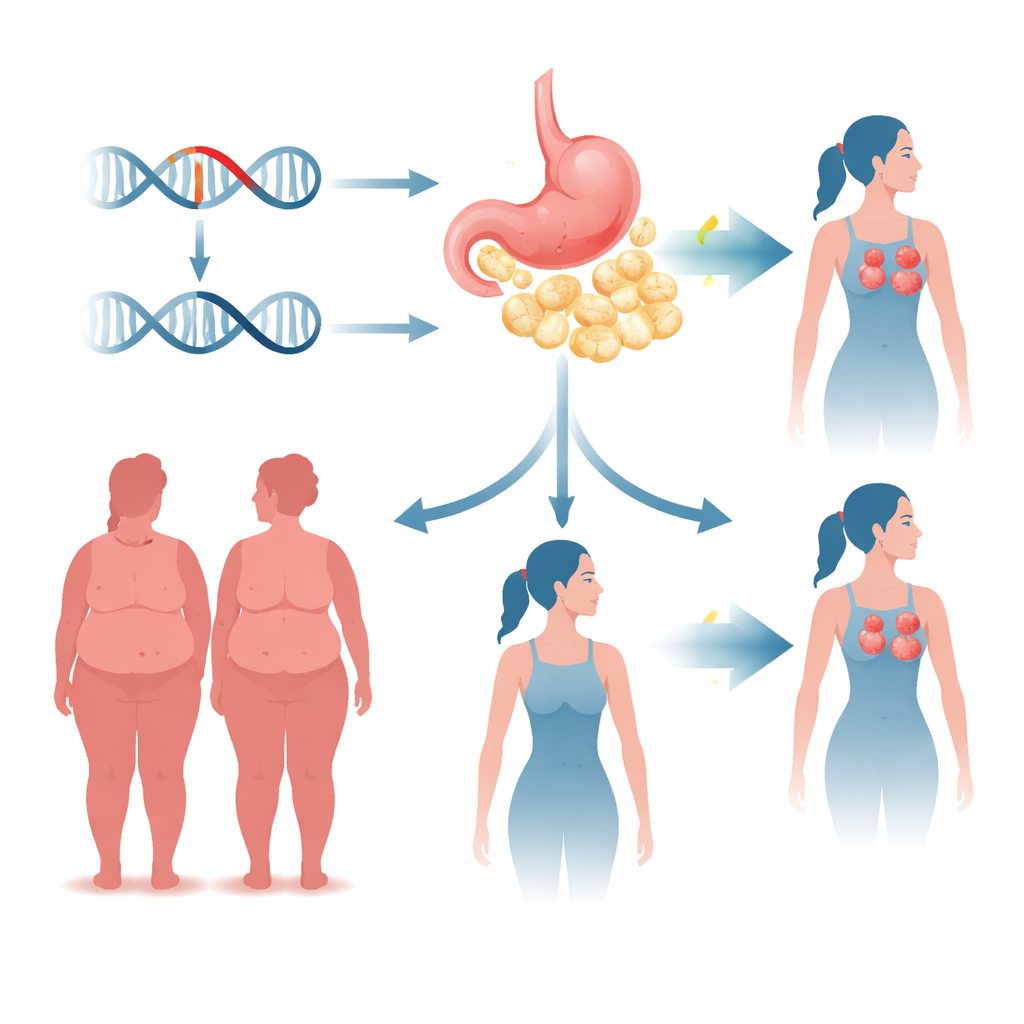
What this means for women and future care
To a lay reader, the bottom line is that a common genetic difference appears to shape how strongly major weight loss through bariatric surgery protects against breast cancer in women with obesity. Women carrying the FTO risk variant, especially those with higher insulin levels, seemed to gain the greatest reduction in risk, while women without that variant did not clearly share this benefit. The study does not suggest that genes alone should decide who receives surgery, and it cannot prove cause and effect, but it does point toward a future in which genetic and metabolic profiles might help tailor weight-loss treatments for cancer prevention. More research in other groups and with newer weight-loss methods will be needed before such personalized approaches can be used in everyday care.
Citation: Langegård, E., Kristensson, F.M., Andersson-Assarsson, J.C. et al. Association between FTO rs9939609 genotype and breast cancer risk after bariatric surgery in the Swedish Obese Subjects study. Sci Rep 16, 14429 (2026). https://doi.org/10.1038/s41598-026-51884-2
Keywords: breast cancer, bariatric surgery, FTO gene, obesity, insulin