Clear Sky Science · en
IFITM3-mediated neuroinflammation in epilepsy regulated by the let-7g-5p/STAT2 axis
Why brain inflammation matters in epilepsy
Epilepsy affects tens of millions of people worldwide, and for about one in three, current drugs do not fully control seizures. Scientists increasingly suspect that chronic inflammation inside the brain helps make seizures more frequent and harder to treat. This study explores a newly uncovered chain of molecules inside the brain’s immune cells that seems to fan—or cool—the inflammatory flames that accompany epilepsy. Understanding this chain could open the door to future treatments that work by calming the brain’s own immune response rather than just damping electrical activity.
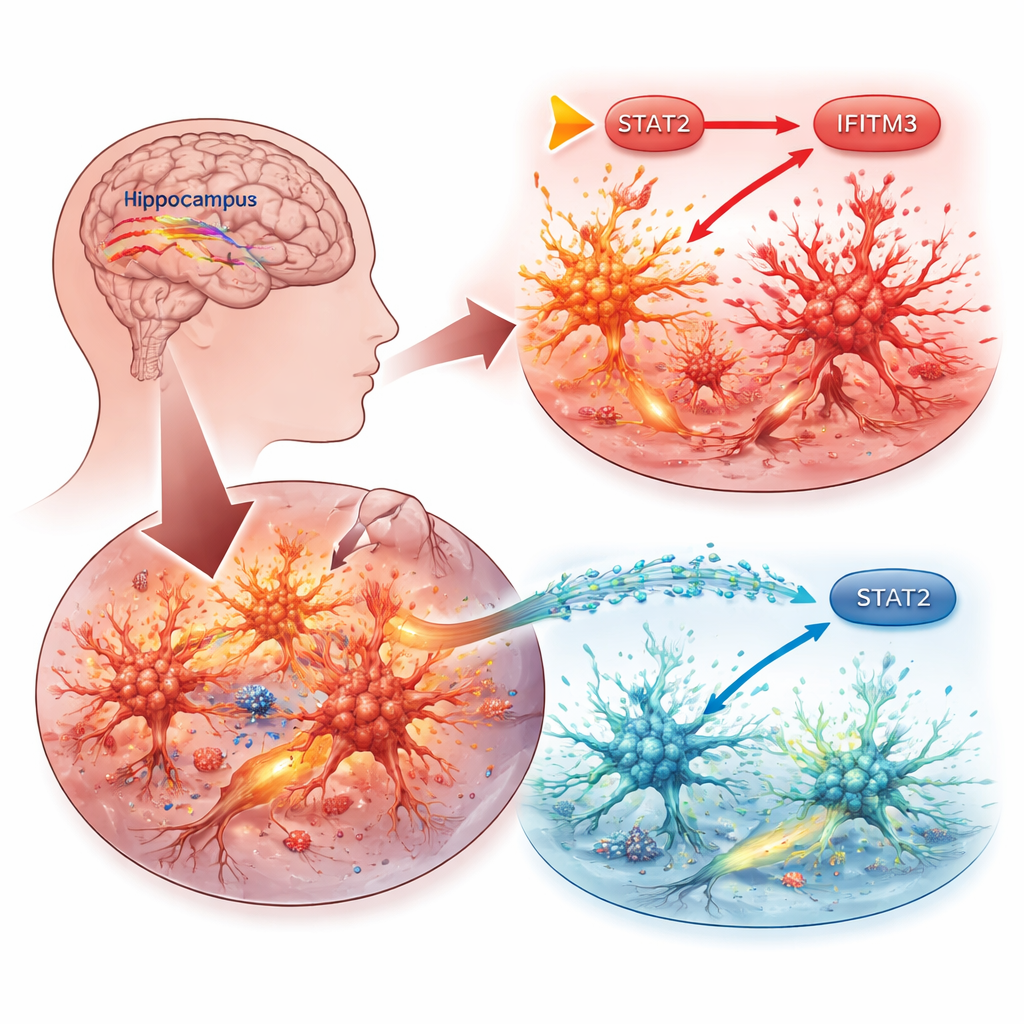
Brain’s immune cells in the spotlight
The work focuses on microglia, the brain’s resident immune cells. When seizures or other injuries strike, microglia switch into an activated state, releasing inflammatory chemicals that can damage nearby nerve cells and lower the threshold for more seizures. The researchers asked which specific molecules inside microglia drive this harmful cycle. They began by mining public genetic databases from mouse models of epilepsy and inflamed microglia, looking for genes that were consistently turned up. One candidate stood out: IFITM3, a protein best known for helping cells fend off viruses but increasingly linked to brain inflammation in conditions such as Alzheimer’s disease and stroke.
A molecular switch that worsens seizures
To test IFITM3’s role, the team used mouse microglial cells exposed to a bacterial mimic that strongly activates inflammation. When IFITM3 levels were high, the cells poured out inflammatory messengers such as interleukin-1β, interleukin-6, and tumor necrosis factor, and showed more signs of programmed cell death, including a fiery, pore-forming type called pyroptosis. Silencing IFITM3 had the opposite effect, sharply reducing inflammatory signals and cell death markers. The scientists then moved into living animals, creating a chronic seizure model in mice and using a virus to dial down IFITM3 in the brain. Mice with reduced IFITM3 had milder seizures on behavioral scoring scales, calmer brain-wave recordings, and lower levels of inflammatory and cell-death markers in brain tissue.
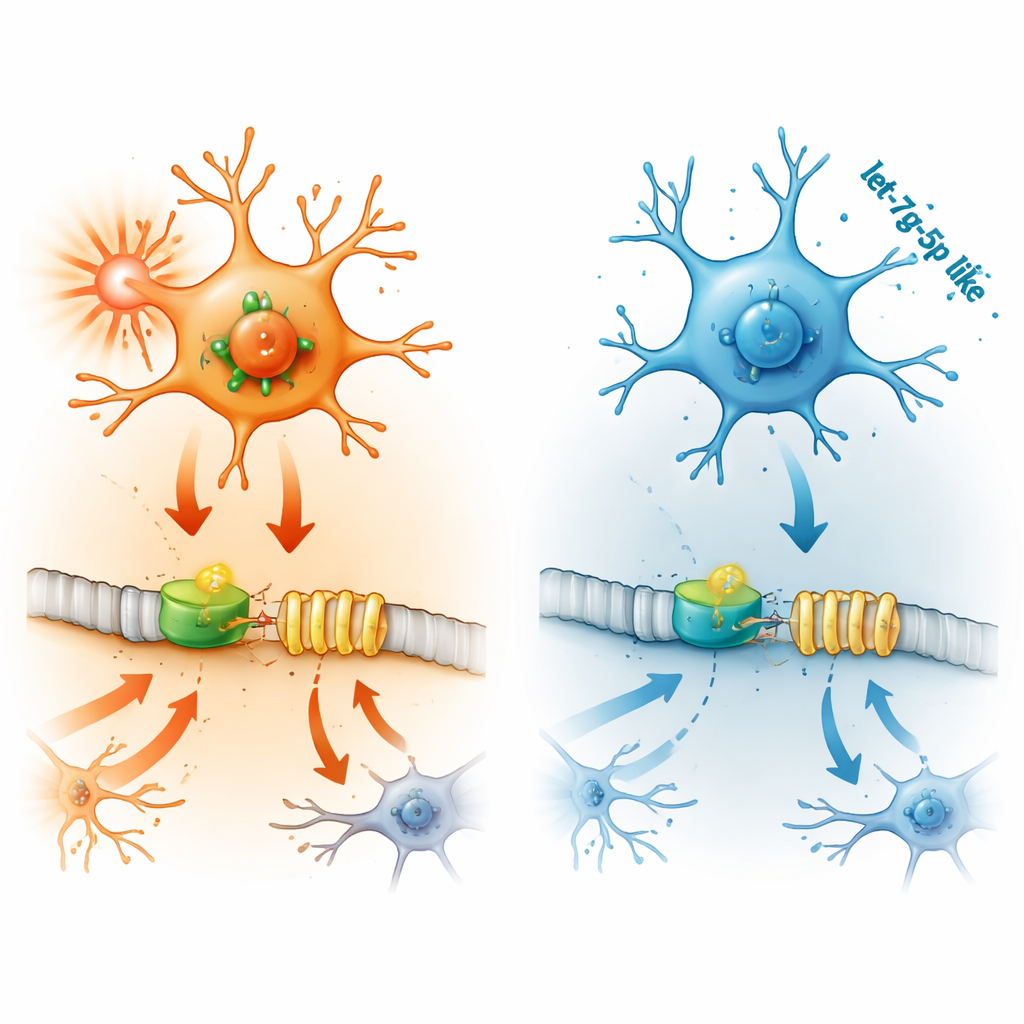
How upstream molecules turn IFITM3 on and off
Next, the researchers traced how IFITM3 gets switched on. They homed in on STAT2, a protein that carries signals from interferons—key immune molecules—to the cell’s DNA. In microglia, boosting STAT2 raised IFITM3 levels and intensified inflammation and cell death, while knocking STAT2 down had the reverse effect. Experiments using DNA reporter constructs showed that STAT2 binds directly to the IFITM3 gene’s control region to activate it. In epileptic mice, STAT2 was also elevated in brain regions prone to seizures, but turning off IFITM3 did not change STAT2 itself, confirming that STAT2 sits upstream as a master switch.
A small RNA that applies the brakes
The final link in the chain is let-7g-5p, a tiny regulatory RNA molecule. MicroRNAs like let-7g-5p fine-tune gene activity by latching onto target messages and blocking their translation into protein. In inflamed microglia and epileptic mouse brains, levels of let-7g-5p dropped. Laboratory tests showed that let-7g-5p binds directly to the tail region of STAT2’s genetic message, lowering STAT2 production. When the researchers added extra let-7g-5p to microglia, STAT2 and IFITM3 levels fell, inflammatory signals dropped, and cell death slowed. Blocking let-7g-5p had the opposite effect—but this could be rescued by simultaneously silencing STAT2, proving that let-7g-5p protects by targeting STAT2 and, in turn, IFITM3.
What this could mean for people with epilepsy
Together, these findings outline a simple but powerful story: STAT2 turns on IFITM3 in microglia, which ramps up brain inflammation and cell death, making seizures worse, while let-7g-5p acts as a natural brake on this process. In epilepsy, that brake appears to fail, allowing inflammation to spiral. Although these results come from cells and mice rather than patients, they highlight the let-7g-5p/STAT2/IFITM3 axis as a promising new target. Future therapies might aim to boost let-7g-5p or block STAT2 or IFITM3, not to cure epilepsy outright, but to cool the inflammatory environment that helps seizures persist and resist standard drugs.
Citation: Liu, J., Sheng, D., Li, X. et al. IFITM3-mediated neuroinflammation in epilepsy regulated by the let-7g-5p/STAT2 axis. Sci Rep 16, 14077 (2026). https://doi.org/10.1038/s41598-026-44357-z
Keywords: epilepsy, neuroinflammation, microglia, IFITM3, microRNA let-7g-5p