Clear Sky Science · en
High-salt diet aggravates allergic rhinitis through the NFAT5 signaling pathway
Why Salty Food Matters for Stuffy Noses
Many people think of salt mainly as a concern for blood pressure, yet it may also shape how our immune system reacts to pollen, dust, and other allergens. This study explores how a modern high-salt diet can worsen allergic rhinitis—the runny, itchy, stuffy nose that plagues millions during allergy season—and uncovers a hidden chain of events linking salty meals, gut microbes, and the delicate lining inside the nose. 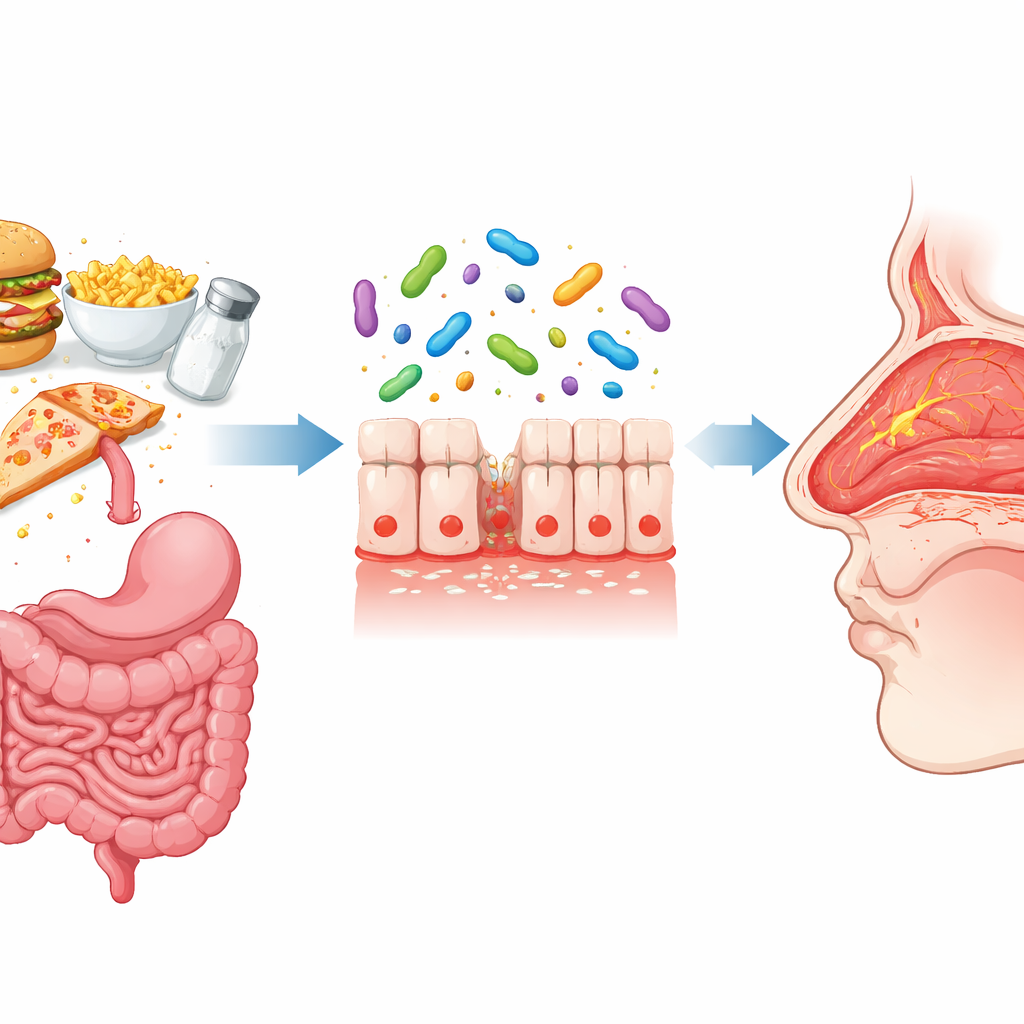
Everyday Salt and Everyday Allergies
Allergic rhinitis affects up to four in ten people worldwide and has been rising alongside Western-style eating habits. The researchers began by studying adults with diagnosed nasal allergies. Instead of relying on food questionnaires, they measured salt intake indirectly by tracking how much sodium people excreted in their urine over 24 hours. Those with higher urinary sodium—indicating a saltier diet—had higher levels of allergy antibody (IgE) in their blood and more severe nasal symptoms, especially congestion. While the sodium level in the blood itself barely changed, the amount passing through the body closely paralleled how miserable patients felt.
From Salty Diet to Stronger Allergic Attacks
To move beyond correlation, the team turned to mice with experimentally induced hay-fever–like disease. Some animals ate a normal diet, while others received chow enriched with salt. Mice on the high-salt diet sneezed more, scratched their noses more often, and showed thicker, more inflamed nasal lining. Their blood contained higher levels of allergen-specific IgE and histamine, the chemical that drives itching and swelling. In fluid washed from their noses, the researchers found boosted levels of “type 2” immune signals that are known to fuel allergic diseases, while other immune branches changed little. In short, extra salt pushed the animals’ immune systems further toward an allergy-prone setting.
Gut Changes and a Leaky Barrier
Because what we eat first passes through the intestines, the scientists examined how a salty diet reshaped the gut environment. Mice consuming extra salt had fewer types of gut microbes overall and a shift in balance between major bacterial groups, with more Firmicutes and fewer Bacteroidetes—an imbalance linked to inflammation in other studies. At the same time, key building blocks of the intestinal barrier, such as proteins that seal the spaces between cells and mucus-forming molecules, were reduced. Under the microscope, sections of the small intestine showed abnormal growth and immune-cell infiltration. These gut changes suggest that a salty diet can weaken the body’s barrier defenses, potentially allowing inflammatory signals to circulate and affect distant sites like the nose.
A Salt-Sensing Switch Inside Nasal Cells
Diving deeper, the team focused on a molecular pathway that helps cells sense and adapt to salty surroundings. In the nasal lining of allergic mice, a high-salt diet cranked up a sequence of signals known as the P38/MAPK–NFAT5–SGK1 pathway. When activated, this pathway heightened allergy-related activity in mast-cell–like immune cells and damaged the tight junctions that keep nasal epithelial cells welded together. Using cultured cells, the researchers showed that boosting salt levels turned on this pathway and increased both allergy mediators and barrier damage. Blocking any one of the key steps—P38, NFAT5, or SGK1—reduced these harmful effects and helped restore barrier-supporting proteins. 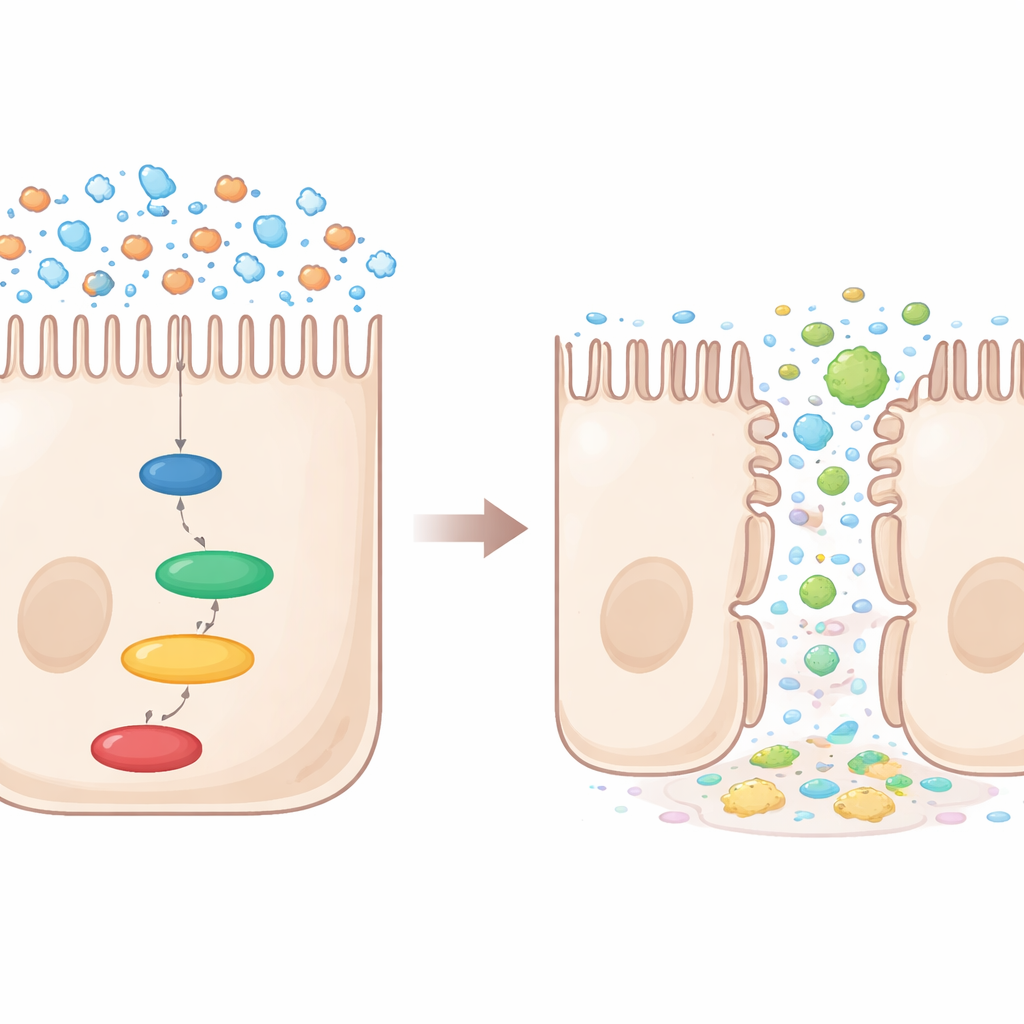
Can Cutting Salt Help Your Nose?
The investigators then asked whether the damage was permanent. In mice, even a short period on a high-salt diet made allergy symptoms worse, but switching back to a normal diet partly eased sneezing, scratching, and some inflammatory markers. However, levels of allergen-specific IgE stayed high, hinting that immune “memory” of the allergen is much harder to erase than the short-term irritation caused by salt. Taken together, the work suggests that a salty diet does more than burden the heart—it can aggravate nasal allergies by disturbing gut microbes, weakening protective barriers, and flipping on a salt-sensing signaling circuit in the nose. For people with hay fever or chronic nasal allergies, moderating salt intake may not replace medication, but it could become a practical, everyday step to reduce flare-ups and improve comfort.
Citation: Jiang, L., Wang, Y., Huang, J. et al. High-salt diet aggravates allergic rhinitis through the NFAT5 signaling pathway. npj Sci Food 10, 126 (2026). https://doi.org/10.1038/s41538-026-00760-4
Keywords: high-salt diet, allergic rhinitis, nasal barrier, gut microbiome, immune signaling