Clear Sky Science · en
Efficient control of enterochromaffin versus islet differentiation from human pluripotent stem cell-derived pancreatic progenitors
Turning Stem Cells into Custom-Made Insulin Factories
For people with type 1 diabetes, replacing the lost insulin-producing cells of the pancreas could one day free them from insulin injections. Scientists can already coax human stem cells into forming mini–pancreatic clusters that resemble the body’s insulin factories, but these lab-grown “islets” are a mixed bag: alongside the desired insulin-producing cells, unwanted cell types often appear. This study asks a practical question with big implications for future therapies: can we reliably steer stem cells toward the good pancreatic cell types while limiting off-target ones?
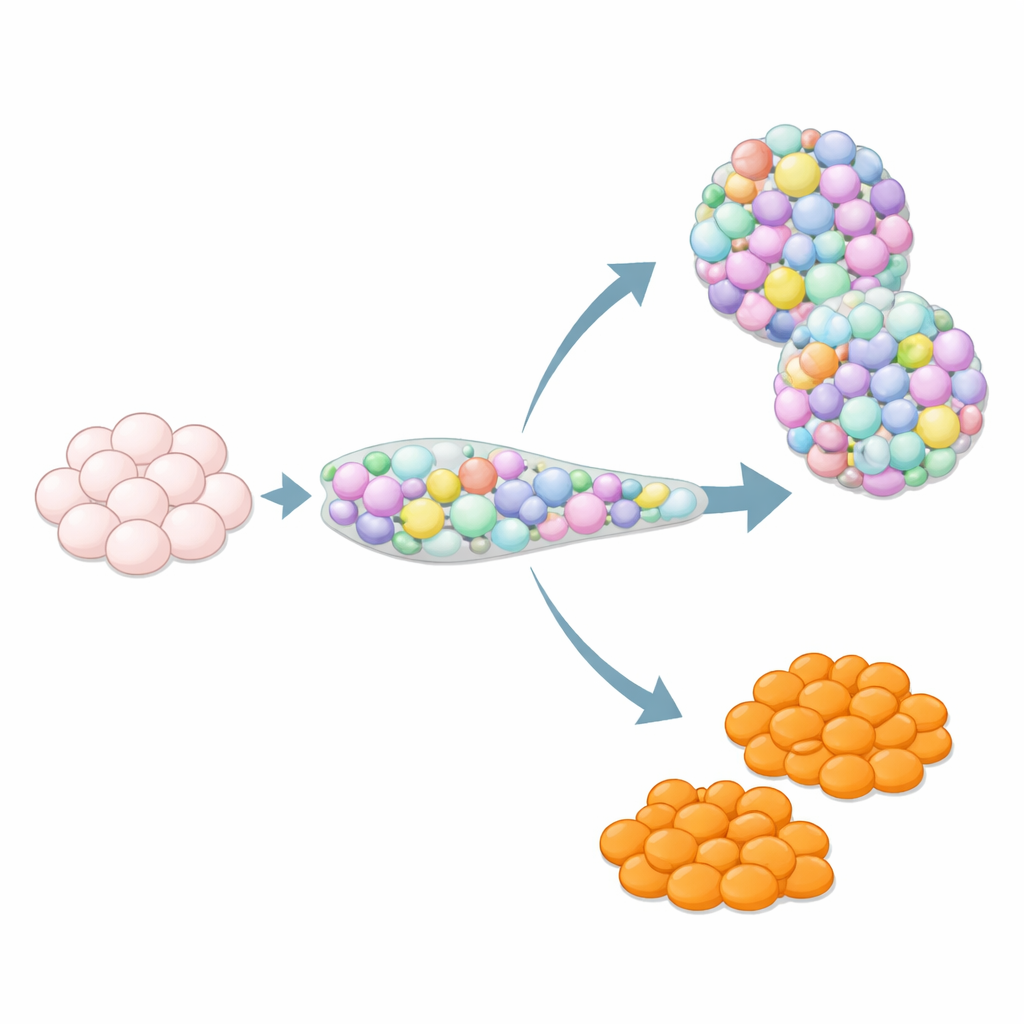
Why Extra Cell Types Can Be a Hidden Problem
When stem cells are guided toward becoming pancreas tissue, they do not always follow the script. Among the surprise guests are cells resembling enterochromaffin cells, a rare gut cell type that normally lives in the stomach and intestine and helps control gut movement and signaling by releasing serotonin. In stem-cell–derived islets, these enterochromaffin-like cells show up frequently, even though they are not part of normal human pancreatic islets. Their effect on islet performance and safety is uncertain, so many researchers see them as contaminants. At the same time, because real gut organoids often struggle to make enough enterochromaffin cells, these off-target cells could be valuable for studying gut biology—if scientists can control when they appear.
Building a Better Starting Point
The authors began by improving the earliest steps of turning human pluripotent stem cells into the “primitive streak” and then into definitive endoderm, the tissue that eventually gives rise to the pancreas and other organs. They found that briefly disrupting the cells’ internal scaffolding with a compound called latrunculin A made this first transition more robust, especially in densely plated cultures that usually respond poorly. This tweak produced more uniform early endoderm and, downstream, more pancreatic progenitors and insulin-producing beta-like cells. Importantly, the same early adjustment also improved formation of other endoderm-based lineages such as lung and mesodermal cells, suggesting a broadly useful way to reduce variability in stem-cell differentiation.
Steering the Fate: Pancreatic Versus Gut-Like Cells
With a stronger starting population of pancreatic progenitors, the team systematically tested combinations of signaling molecules at later stages to see how they shaped the final mix of endocrine cell types. Some treatments, including inhibitors of MAPK/ERK and BMP pathways, pushed progenitors strongly toward enterochromaffin-like cells, whereas others, such as growth factors FGF2, betacellulin and BMP4, suppressed these cells and instead favored classic pancreatic types like alpha, beta, and delta cells. They showed that simply increasing a well-known pancreatic marker, NKX6-1, early on was not enough to prevent the appearance of enterochromaffin-like cells. Rather, the outcome depended on an interaction between early patterning (how progenitors were primed) and later patterning (the signals they received during endocrine commitment). By mixing and matching these steps, the researchers created recipes that yielded either beta-cell–enriched islet-like clusters with strong glucose-stimulated insulin secretion, or clusters highly enriched in enterochromaffin-like cells.
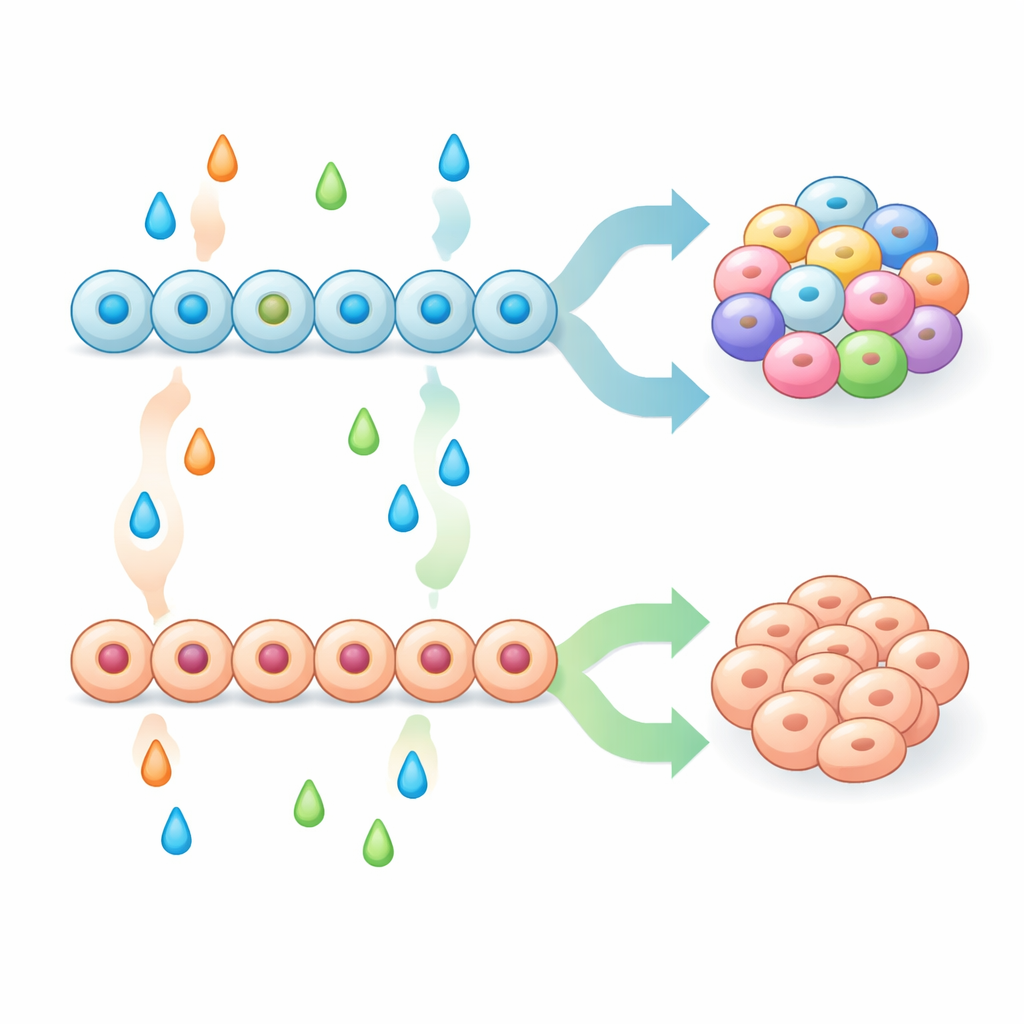
Clues from Mouse Models and Gene Activity
To test whether pancreatic tissues naturally have the capacity to produce enterochromaffin-like cells, the team examined mice engineered to lose a key regulatory gene, Isl1, in developing endocrine cells. In these animals, the islets contained many cells with features of enterochromaffin cells, including serotonin production and expression of the transporter SLC18A1. Single-cell gene profiling in both mice and human stem-cell–derived islets revealed that these pancreatic enterochromaffin-like cells share many molecular traits with intestinal enterochromaffin cells, but also carry pancreatic hallmarks such as NKX6-1 and insulin-related genes. A striking shared feature was prolonged activity of the transcription factor Neurogenin 3 (NGN3), which normally switches on only briefly during endocrine development. In the enterochromaffin-like lineage, NGN3 stayed active for longer, in both mouse and human systems, hinting that the timing of this key factor may help decide whether a progenitor becomes a pancreatic islet cell or an enterochromaffin-like cell.
Designing Cell Clusters for Therapy and Research
By mapping how early priming and late signaling cues interact, this work offers a roadmap for designing “made-to-order” endocrine clusters from human stem cells. For therapeutic use in diabetes, protocols that minimize enterochromaffin-like cells and maximize mature beta-like cells should yield safer, more predictable grafts with better insulin responses. Conversely, the ability to generate large, pure populations of enterochromaffin-like cells from pancreatic progenitors opens a new route to study serotonin-producing gut cells and their diseases. In simple terms, the study shows that stem-cell–derived pancreas models are not stuck with random outcomes: with carefully chosen chemical signals at the right times, scientists can tilt the balance toward desired cell types and away from unwanted ones.
Citation: Misra, P.S., McGaugh, E.C., Huang, H. et al. Efficient control of enterochromaffin versus islet differentiation from human pluripotent stem cell-derived pancreatic progenitors. Nat Commun 17, 4137 (2026). https://doi.org/10.1038/s41467-026-70666-y
Keywords: stem cell–derived islets, beta cell replacement, enterochromaffin cells, pancreatic progenitors, type 1 diabetes