Clear Sky Science · en
Talimogene laherparepvec and atezolizumab in HER2-negative breast cancer following neoadjuvant chemotherapy: a window-of-opportunity phase II trial (SOLTI-1503 PROMETEO)
New hope for stubborn breast tumors
Many women with early breast cancer now receive strong chemotherapy before surgery. For some, this shrinks the tumor so much that no cancer can be found at the time of the operation, and their long‑term outlook is excellent. But others are left with a visible lump of cancer that has resisted treatment. These patients face a higher risk that the disease will come back. The PROMETEO study tested a new way to "wake up" the immune system against this remaining cancer using a cancer‑killing virus together with an immune‑boosting antibody.
Turning a virus into an ally
The trial focused on women whose tumors lacked the HER2 protein, a common type of breast cancer that can be either hormone‑driven or triple‑negative. All had already completed standard pre‑surgery chemotherapy yet still had a mass of at least one centimeter on scans and biopsy, showing that their cancers were resistant to drugs. Researchers used talimogene laherparepvec (T‑VEC), a modified herpes virus that infects and destroys cancer cells while releasing signals that attract immune cells. They paired it with atezolizumab, an antibody that blocks the PD‑L1 "brake" that tumors use to switch off immune attacks. The treatment was given during an 11‑week window between chemotherapy and surgery.
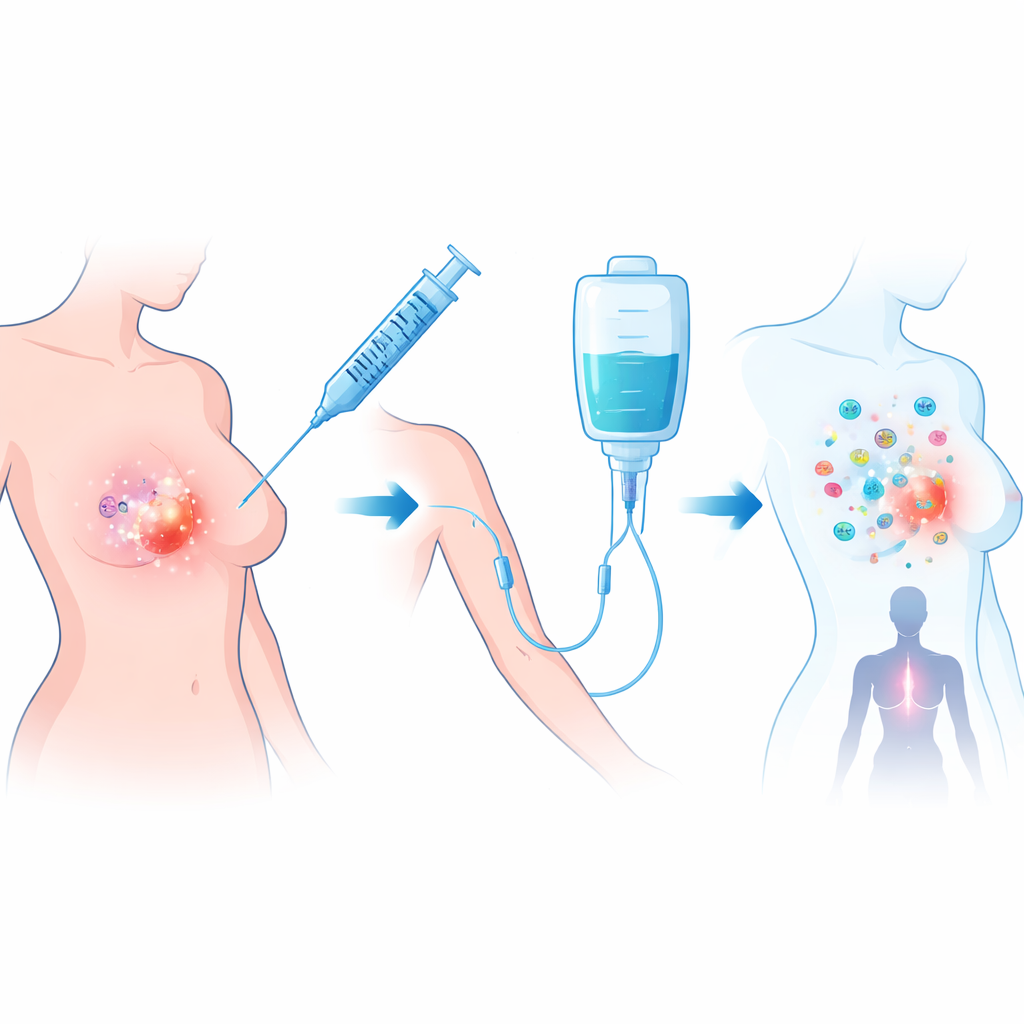
What the study found in the operating room
Twenty‑eight women were treated; most had hormone‑receptor positive, HER2‑negative tumors, and the rest had triple‑negative disease. Each patient received one low‑dose injection of T‑VEC directly into the breast tumor, followed by four higher‑dose injections together with atezolizumab infusions. When surgeons later removed the tumors, pathologists carefully measured how much cancer was left. In 7 of 26 evaluable patients—about one in four—no invasive cancer remained in the breast or lymph nodes, a result known as a pathologic complete response. This met the trial’s predefined goal and is noteworthy because all these tumors had already proven resistant to chemotherapy. The treatment was generally well tolerated, with mostly mild side effects such as fever, joint aches, and temporary changes in blood tests; there were no life‑threatening reactions or treatment‑related deaths.
Watching the immune system wake up
Because this was a "window‑of‑opportunity" trial, the team collected multiple biopsies before, during, and after the new treatment, providing a rare movie‑like view of how the tumor environment changed over time. Under the microscope, the researchers saw rising numbers of tumor‑infiltrating lymphocytes—white blood cells that can attack cancer—as treatment went on. Structures resembling tiny lymph nodes, called tertiary lymphoid structures, became more common, and the tumors more often showed signs of PD‑L1, the very target of atezolizumab. Gene‑activity analyses of the tumor samples echoed these visual changes: hundreds of immune‑related gene signatures, including those linked with B cells, T cells, and antibody production, increased sharply after T‑VEC alone and again after the combination therapy, and stayed high at surgery. These shifts appeared not only in patients whose tumors vanished but also in those with remaining disease, indicating that the strategy broadly re‑energized anti‑tumor immunity.
First hints about long‑term protection
The researchers also tracked patients after surgery to see whether the cancer returned. After a median follow‑up of nearly four years, only four women had experienced distant metastases, and none of these had achieved a complete disappearance of tumor at surgery. In contrast, all seven patients whose tumors were cleared remained free of recurrence. While the numbers are small and the study lacked a comparison group, this pattern supports the idea that eliminating visible cancer after treatment is closely tied to better long‑term outcomes, even in this high‑risk group.
What this could mean for patients
The PROMETEO trial shows that briefly adding a cancer‑killing virus plus an immune‑activating antibody between chemotherapy and surgery is feasible and appears safe for women with HER2‑negative breast cancer that has survived initial treatment. The approach triggered strong signs of immune activation inside resistant tumors and led to complete tumor disappearance in a meaningful fraction of patients, especially those with hormone‑receptor positive disease, where such responses are usually rare. Although larger randomized trials are needed to confirm whether this strategy truly improves cure rates, the results suggest that transforming the tumor into an inflamed, immune‑rich area just before surgery may offer a new way to lower the risk of relapse for patients who currently have limited options.
Citation: Pascual, T., Vidal, M., Cejalvo, J.M. et al. Talimogene laherparepvec and atezolizumab in HER2-negative breast cancer following neoadjuvant chemotherapy: a window-of-opportunity phase II trial (SOLTI-1503 PROMETEO). Nat Commun 17, 2817 (2026). https://doi.org/10.1038/s41467-026-69222-5
Keywords: oncolytic virus, breast cancer immunotherapy, HER2-negative, residual disease, neoadjuvant chemotherapy