Clear Sky Science · en
AMPK is dispensable for physiological podocyte and glomerular functions but prevents glomerular fibrosis in experimental diabetes
Why kidney filter cells matter in diabetes
Our kidneys quietly filter blood thousands of times a day, and a key part of that filter is made of cells called podocytes. These cells wrap around tiny blood vessels in structures known as glomeruli, keeping proteins in the blood while letting waste and water pass into the urine. This study asks a deceptively simple question with big implications for people with diabetes: does a major energy-sensing switch in cells, called AMPK, truly protect these filter cells and prevent scarring of the kidney? The answer turns out to be subtle—AMPK is not needed for day‑to‑day kidney function, but becomes crucial when diabetes stresses the system.
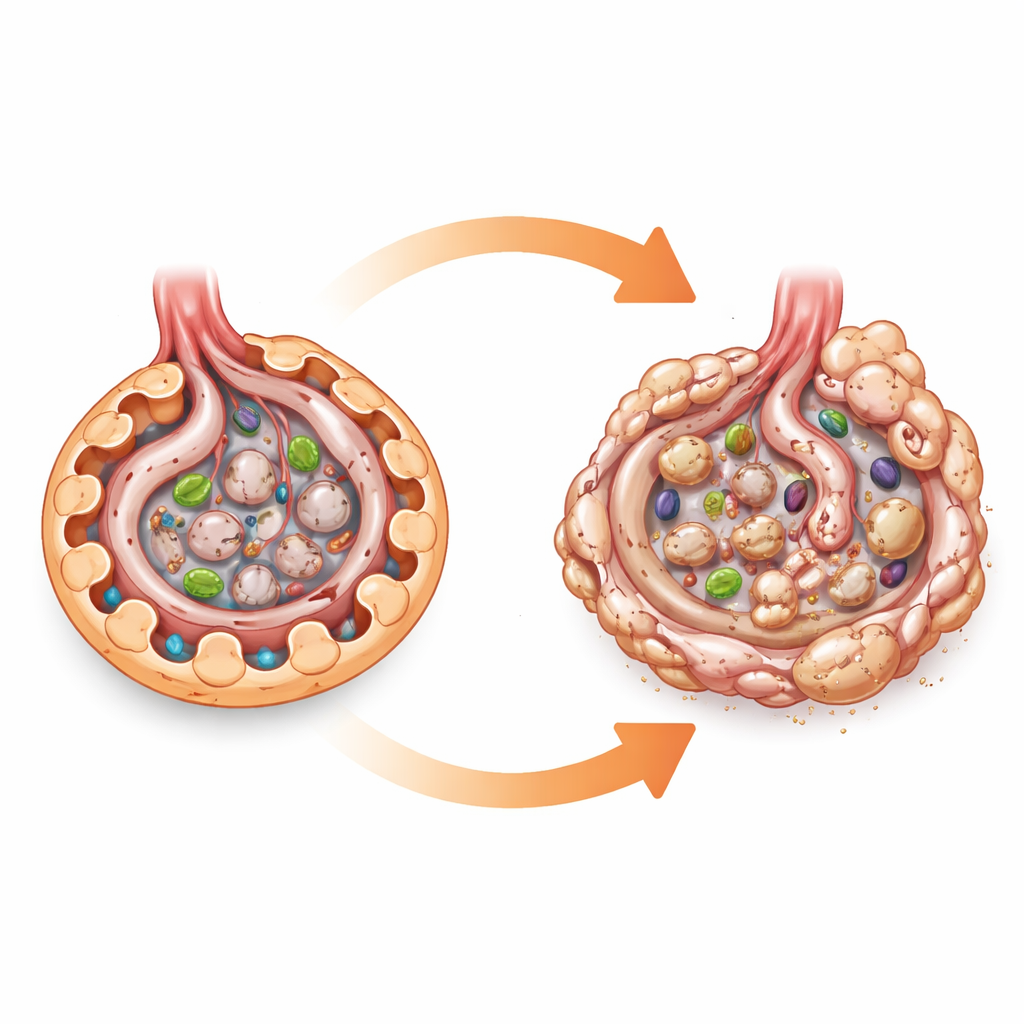
A cellular fuel gauge under the microscope
AMPK can be thought of as a cellular fuel gauge. When energy is low, it turns on processes that burn fat and sugar and supports cleanup systems such as autophagy, which helps cells recycle worn‑out components. Because diabetes overloads kidney cells with sugar and nutrients, many researchers have assumed that a drop in AMPK activity directly harms podocytes and drives diabetic kidney disease. Most of this belief came from cell culture studies and from animals treated with drugs that turn AMPK on, which can have many other effects. To test AMPK’s role more cleanly, the authors engineered mice that lacked both major AMPK subunits specifically in podocytes, while leaving AMPK intact in the rest of the body.
Surprisingly normal kidneys in the absence of AMPK
When these engineered mice were followed for two years on a normal diet, their kidneys looked and worked just like those of their normal littermates. Podocyte numbers were preserved, the fine structure of the glomeruli remained intact, and urine tests showed no excess protein leakage. Even key processes that AMPK is known to influence—such as a growth pathway called mTORC1 and the cell’s internal recycling system—were not obviously disturbed in these podocytes. This suggests that in a healthy, well‑fed state, podocytes can keep up their work without relying on AMPK, perhaps by leaning on backup pathways that perform similar jobs.
Diabetes reveals hidden weaknesses
The picture changed sharply when diabetes was induced, using both a type 1‑like model and a combined high‑fat, low‑dose toxin model that mimics aspects of type 2 diabetes. Under the same high blood sugar levels, mice lacking AMPK in podocytes developed more severe kidney injury than normal diabetic mice. Their glomeruli were larger and more scarred, and they leaked more albumin into the urine, a key clinical sign of kidney damage. Detailed staining showed heavier buildup of collagen and “stress” proteins in the glomeruli, pointing to an acceleration of glomerular fibrosis—the gradual replacement of delicate filtering tissue with stiff scar.
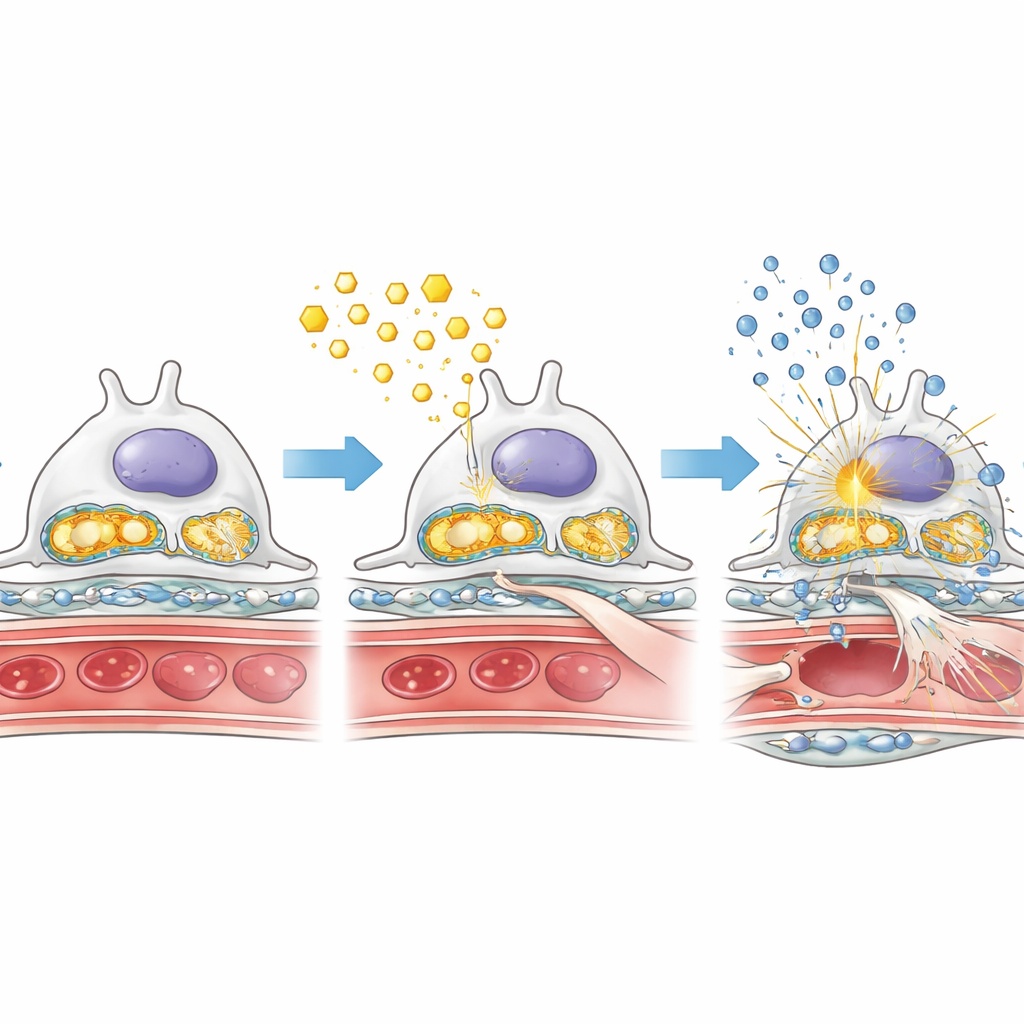
Fat overload, damaged powerhouses, and inflammatory alarms
To understand why the lack of AMPK worsened damage, the researchers looked closely at how podocytes handled fats and sugars under diabetic conditions. In diabetic mice without podocyte AMPK, fat droplets accumulated within glomeruli, while a key enzyme for burning fatty acids was reduced. At the same time, enzymes that drive rapid sugar breakdown were more active, hinting at a shift toward a less efficient, more “fermenting” style of metabolism that can favor scarring. The cell’s energy factories—mitochondria—were also affected: their support proteins were lower, and their genetic material leaked into the cell fluid. This leaked mitochondrial DNA appears to trigger an internal alarm system known as the cGAS–STING pathway, which in turn activates inflammatory switches like NF‑κB and increases production of inflammatory molecules. Together, these changes create a toxic mix of fat overload, mitochondrial damage, and chronic inflammation inside the kidney filter.
Ripples from podocytes to neighboring cells
Podocytes do not work in isolation; they sit directly across from glomerular endothelial cells, which line the blood side of the filter. The study found that when podocyte AMPK was missing in diabetes, these neighboring endothelial cells were more likely to adopt a fibroblast‑like state, a process called endothelial‑to‑mesenchymal transition. In this state they contribute more actively to scar formation. These endothelial cells showed the same metabolic signatures seen in podocytes: less capacity to burn fat and more reliance on glycolysis. This suggests that stressed podocytes can indirectly push neighboring cells toward harmful behavior, amplifying fibrosis across the whole glomerulus.
What this means for people with diabetes
In everyday life, podocytes seem able to function without much help from AMPK. But under the chronic stress of diabetes, the remaining AMPK activity in normal podocytes becomes a quiet defender, helping them burn fat properly, protect their mitochondria, and keep inflammatory alarms in check. When that safety net is removed, fat and sugar handling go awry, mitochondria break down, inflammatory pathways flare, and scarring spreads through the kidney filter. These findings support the idea that therapies which gently boost AMPK activity, or mimic its protective effects on metabolism and inflammation, could help slow or prevent diabetic kidney disease—by reinforcing the resilience of podocytes and their close neighbors rather than by changing blood sugar alone.
Citation: Srivastava, S.P., Kopasz-Gemmen, O., Kunamneni, A. et al. AMPK is dispensable for physiological podocyte and glomerular functions but prevents glomerular fibrosis in experimental diabetes. Cell Death Discov. 12, 204 (2026). https://doi.org/10.1038/s41420-026-03078-y
Keywords: diabetic kidney disease, podocytes, AMPK, glomerular fibrosis, cellular metabolism