Clear Sky Science · en
Dental, mandibular and parotid gland radiation doses in curatively treated head and neck squamous cell carcinoma: a retrospective cohort study
Why this matters for cancer patients’ everyday lives
People treated for head and neck cancer often worry not only about beating the disease, but also about what treatment will do to their teeth, jaw, and ability to eat and speak. Radiation therapy can save lives, yet it may damage the mouth and salivary glands, leading to pain, broken teeth, dry mouth, and even jawbone breakdown. This study looked closely at how much radiation different parts of the mouth actually receive in common treatment plans, and how careful aiming of the beams might spare teeth and glands while still effectively treating the cancer.
How radiation treatment and teeth are connected
Head and neck squamous cell carcinoma can arise in the tongue, throat, voice box, nasal passages, and nearby areas. Radiation therapy is a mainstay of treatment and typically delivers high doses to the tumor and its nearby lymph nodes. Because the beams pass through the jaws, they can weaken teeth, dry out saliva, and, in severe cases, damage the jawbone itself. To reduce these risks, dentists usually remove teeth that are likely to fail if they sit in areas expected to receive higher doses. Yet until now, there has been limited detailed information on how those doses are distributed across different regions of the mouth in real-world treatment plans.
What the researchers set out to measure
The team in Finland reviewed radiation plans for 91 adults treated with curative intent for head and neck cancer between 2018 and 2021. Using planning scans and specialized software, they divided the upper and lower teeth into six zones: front teeth and canines, and back teeth (premolars and molars) on the left and right. They also outlined the lower jawbone and the large parotid salivary glands. For each zone, they calculated the average dose and the near-maximum dose, paying special attention to whether it rose above 40 gray—a commonly used threshold where damage to teeth and supporting bone becomes more likely over time.
What they found about different tumor sites
The pattern of radiation exposure depended strongly on where the tumor started and whether radiation was given to both sides of the neck or only one. In cancers of the oral cavity and oropharynx (such as the tonsil), treatments that targeted both sides usually exposed much of the lower jaw and many back teeth to doses above the 40 gray threshold. In contrast, tumors lower in the throat or in the voice box tended to leave most teeth, especially upper teeth and front lower teeth, below that level simply because the radiation fields sat farther away. For cancers in the nasal area and nasopharynx, the upper teeth often lay in the higher-dose region, while the lower front teeth were largely spared.
How one-sided treatment can spare teeth and glands
A key comparison was between bilateral radiation (both sides of the neck) and ipsilateral radiation (mainly on the tumor side). When one-sided treatment was appropriate—for example in some oral cavity and oropharyngeal cancers that did not cross the midline—it could significantly spare teeth on the opposite side. In oral cavity cases treated this way, most teeth on the non-tumor side stayed below 40 gray, and the front upper teeth often received lower doses. The same trend appeared in the lower jaw: one-sided plans reduced the average dose to the mandible compared with two-sided plans. The parotid glands also benefited. While not all glands met published dose limits associated with better saliva function, a considerable share did, especially when treatment volumes were smaller or one side could be spared.
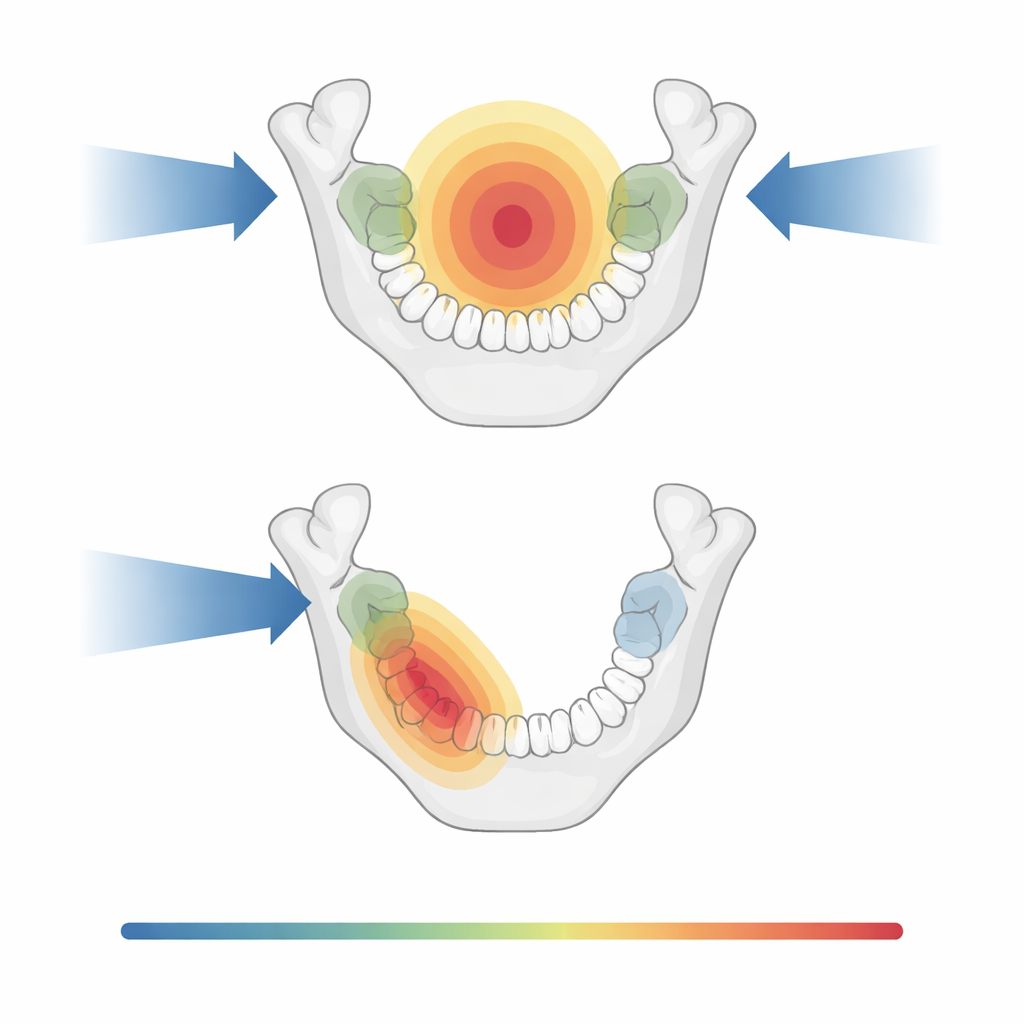
What this means for dental care and quality of life
The study did not track long-term tooth loss or jawbone death directly, but its maps of dose distribution provide a practical foundation for tailoring dental care to each patient. Knowing which tooth regions are likely to receive higher doses can help teams decide which teeth truly need to be removed before treatment and where implants or other restorations might be safe later on. The findings suggest that, when medically acceptable, more precise and one-sided radiation fields can reduce unnecessary extractions, preserve chewing function, and still keep cancer control as the top priority. In the long run, combining careful radiation planning with close cooperation between oncologists and dentists may allow more patients to complete curative treatment while keeping more of their natural teeth and a healthier, more comfortable mouth.
Citation: Kärkkäinen, V.E., Hietala, H., Koivunen, P. et al. Dental, mandibular and parotid gland radiation doses in curatively treated head and neck squamous cell carcinoma: a retrospective cohort study. BDJ Open 12, 30 (2026). https://doi.org/10.1038/s41405-026-00416-1
Keywords: head and neck cancer, radiation therapy, dental complications, salivary glands, osteoradionecrosis