Clear Sky Science · en
Activity of PROTAC MDM2 degrader in primary leukemia cells and PDX models
New Hope for Tough Blood Cancers
Many adults diagnosed with acute myeloid leukemia (AML) face limited treatment options and high chances of relapse. This study explores a next‑generation drug strategy that does not just block a cancer‑driving protein but actually destroys it inside leukemia cells. By aiming at a key regulator that normally keeps the body’s main tumor‑suppressor in check, the researchers show a way to reawaken the cell’s own defenses against cancer while sparing much of the healthy bone marrow.
How Leukemia Hijacks a Safety Switch
Our cells depend on a guardian protein called p53 to pause cell growth, repair DNA damage, or trigger cell suicide when something goes badly wrong. In many cancers, p53 itself is mutated and no longer works. In AML, however, p53 is often still intact but is held down by another protein, MDM2, which tags p53 for destruction. Many leukemia cells make too much MDM2, effectively muffling p53’s alarm system. Earlier drugs tried to block the interaction between MDM2 and p53, but this approach has a catch: as p53 briefly recovers, it actually drives cells to make more MDM2, creating a built‑in feedback loop that can limit how well these medicines work.
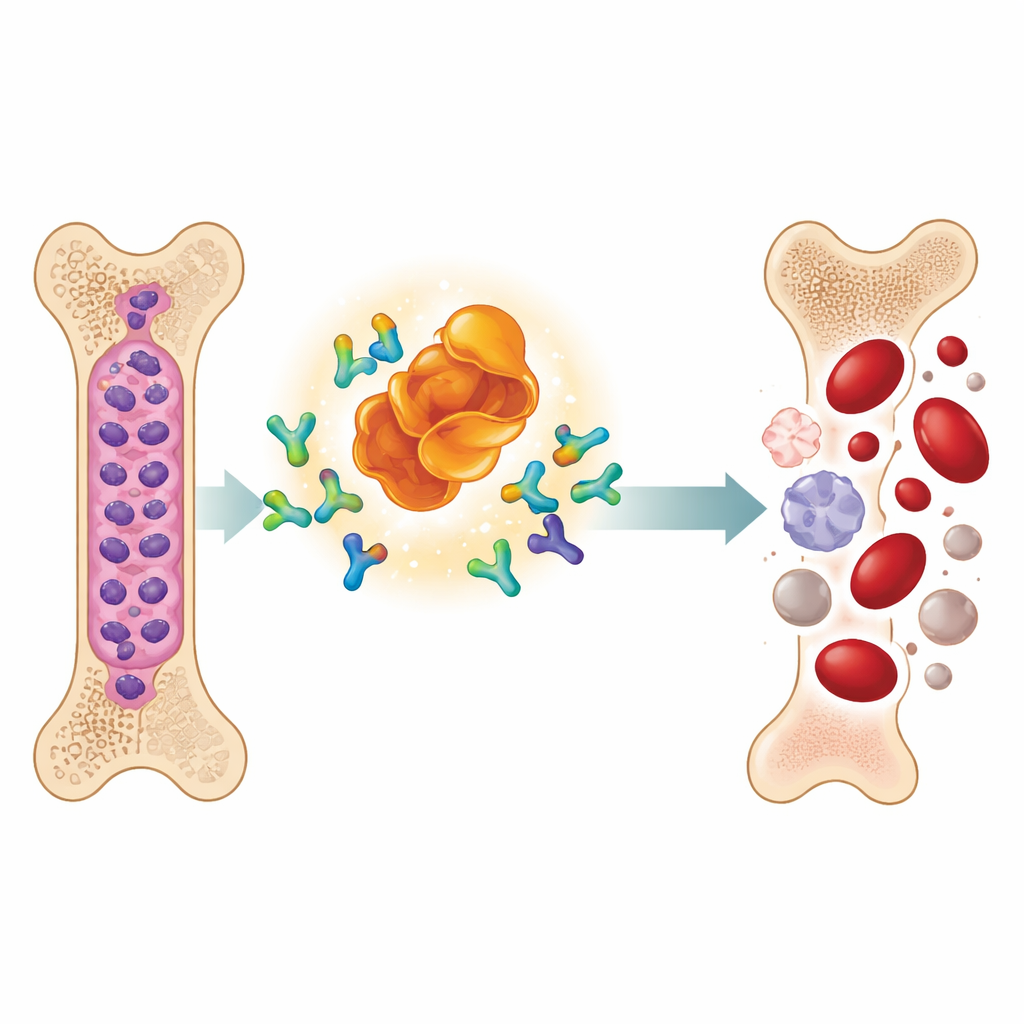
A New Type of Drug That Makes Cancer Proteins Vanish
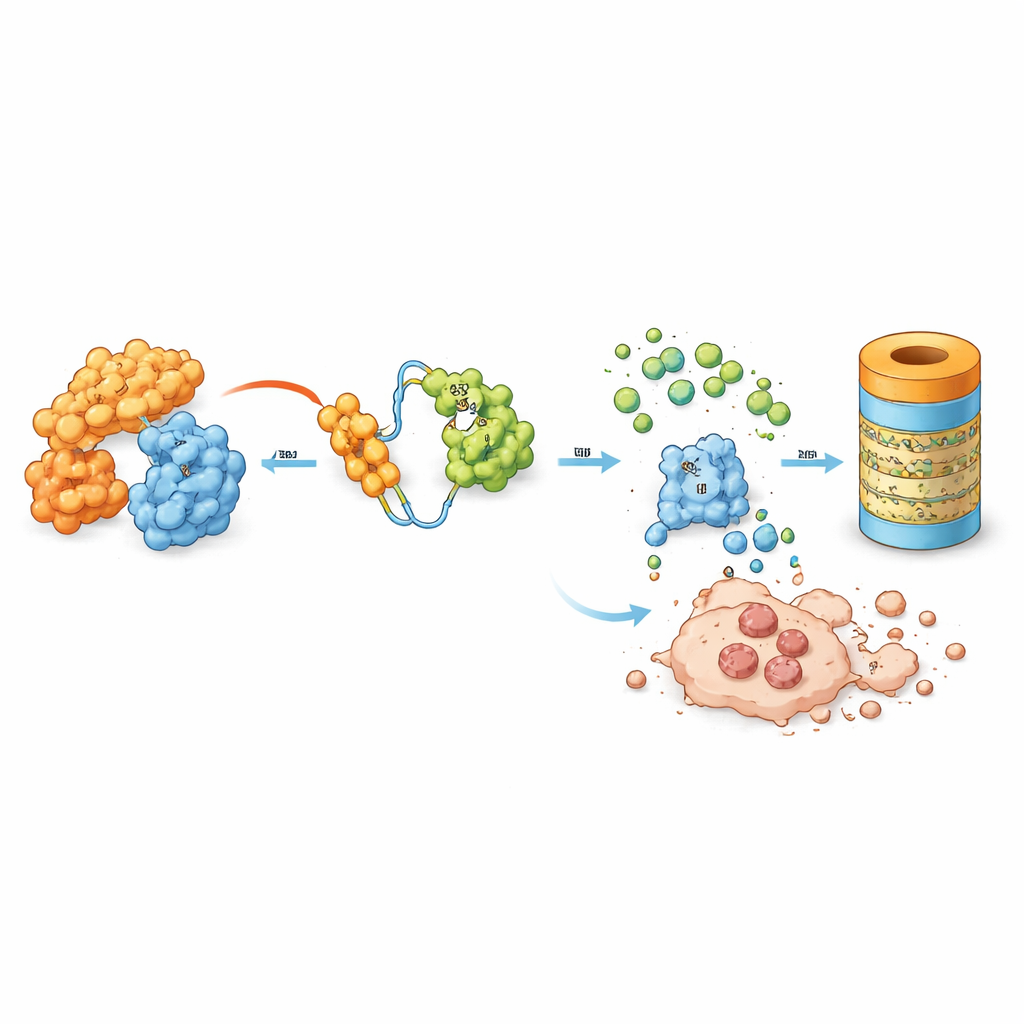
The team studied a designer molecule called MD‑265, part of a growing class of drugs known as PROTACs. Instead of simply sticking to MDM2 and disabling it, MD‑265 acts like a molecular matchmaker. One end binds MDM2, the other recruits a natural cellular disposal system. This brings MDM2 into close contact with the machinery that marks unwanted proteins for breakdown, leading the cell to shred MDM2 rather than just block it. In laboratory tests on leukemia stem cells taken from 100 AML patients, MD‑265 killed cancer cells at concentrations roughly a thousand times lower than a conventional MDM2 blocker built from the same core chemical scaffold. Leukemia samples that responded to the degrader also tended to respond to the inhibitor, but the degrader was far more potent.
Striking Cancer Cells Harder Than Healthy Cells
A major concern with any cancer drug is damage to normal tissues, especially the bone marrow cells that produce healthy blood. The researchers compared how MD‑265 affected leukemia stem cells and normal blood‑forming stem cells from healthy donors. Normal cells were about one hundred times less sensitive to the degrader than leukemia cells, suggesting a meaningful therapeutic window. When the team grew cells in a dish that allows them to form colonies, MD‑265 sharply reduced colony formation in sensitive AML samples but had much milder effects on normal stem cells. The small group of leukemias that resisted treatment generally carried damaged p53 or produced very little MDM2 and its close partner MDM4, highlighting which patients might not benefit from this strategy.
Putting the Drug to the Test in Mice
To mimic human disease more closely, the investigators transplanted leukemia stem cells from patients into specialized immune‑deficient mice, creating patient‑derived xenograft (PDX) models. Once human leukemia cells had taken hold in the blood, the mice were treated either with MD‑265, with a powerful oral MDM2 inhibitor already in clinical trials, or with a control solution. Both drugs initially shrank the leukemia burden, but important differences emerged over time. After several weeks, treatment was stopped. Leukemia rebounded quickly in mice that had received the inhibitor, while those treated with the degrader showed much slower regrowth and lived longer overall. Notably, MD‑265 did not cause the weight loss seen with prolonged inhibitor treatment, suggesting better tolerability.
What This Could Mean for Patients
Taken together, the findings show that directly breaking down MDM2 can more effectively revive p53’s tumor‑fighting power than simply blocking it, at least in AML cells that still carry normal p53 and rely on MDM2 to silence it. MD‑265 worked at very low doses, hit leukemia cells much harder than healthy blood‑forming cells, avoided the unwanted surge in MDM2 caused by older drugs, and significantly extended survival in mouse models built from patient samples. While this work is still pre‑clinical and safety and resistance must be studied carefully in future trials, it points toward a promising new class of leukemia treatments that work by dismantling a key cancer helper rather than merely getting in its way.
Citation: Kandarpa, M., Peterson, L.F., Potu, H. et al. Activity of PROTAC MDM2 degrader in primary leukemia cells and PDX models. Leukemia 40, 918–924 (2026). https://doi.org/10.1038/s41375-026-02957-8
Keywords: acute myeloid leukemia, p53 and MDM2, PROTAC degrader, targeted protein degradation, leukemia stem cells