Clear Sky Science · en
Functional cooperation between the B-cell receptor and NOTCH1 in regulating metabolic reprogramming in chronic lymphocytic leukemia
Why this matters for patients and families
Chronic lymphocytic leukemia (CLL) is the most common adult leukemia, and while many people live with it for years, some cases become aggressive and hard to treat. This study asks a simple but crucial question: what makes some CLL cells grow faster and resist treatment, and can that weakness be turned against them? The researchers uncover how two key switches on leukemia cells team up to overhaul the cells’ energy use, creating both a growth advantage and a hidden metabolic Achilles’ heel that doctors may be able to target.
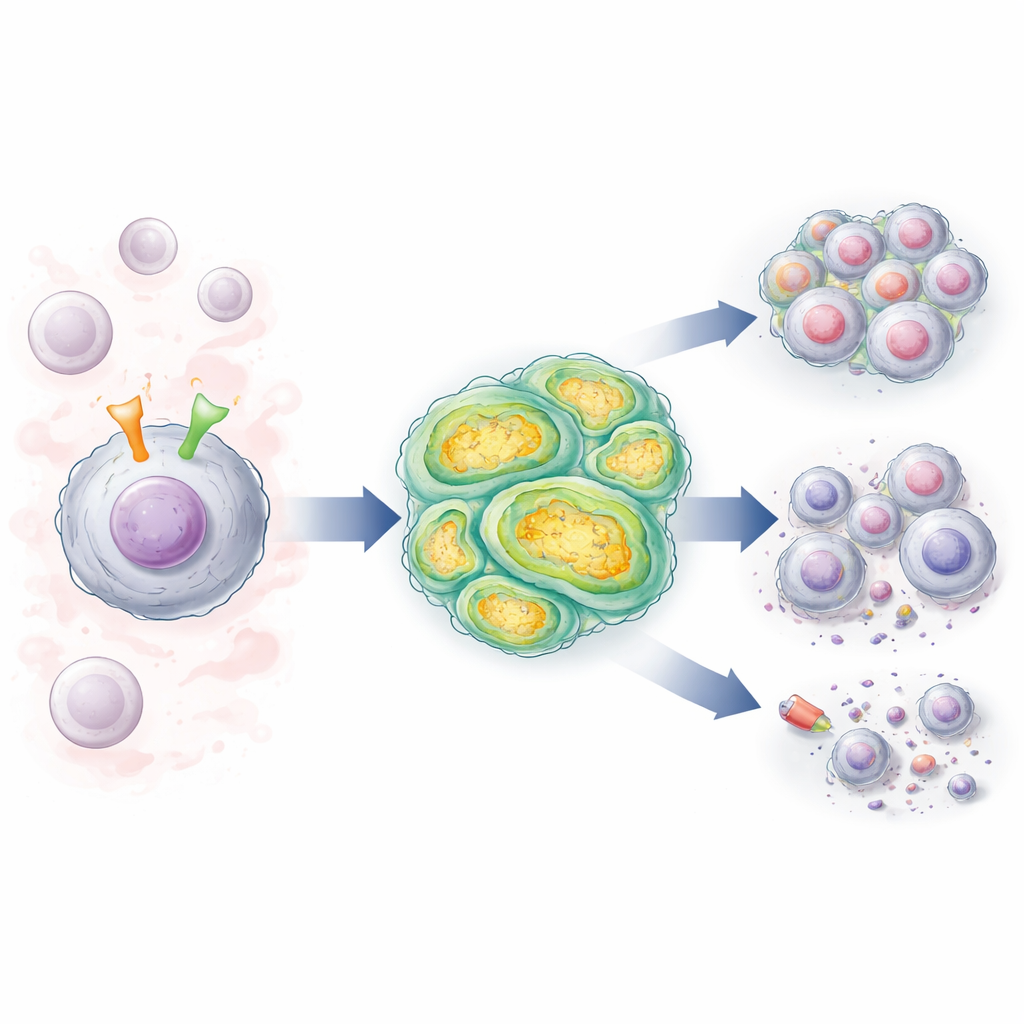
Two cell switches that talk to each other
CLL cells carry a surface antenna called the B-cell receptor (BCR), which senses signals in the blood and lymph nodes and pushes the cells to survive and divide. Many patients also have changes in a gene called NOTCH1, which encodes another surface molecule that, when activated, sends powerful growth and survival signals into the nucleus. The authors studied CLL cells from patients whose BCRs shared a high-risk, “unmutated” pattern, and compared cells with normal NOTCH1 to those with NOTCH1 mutations. They found that when the BCR was stimulated, it strongly boosted NOTCH1 activity, especially in the mutated cells, reinforcing a feedback loop that keeps leukemic signaling switched on.
Rewiring how leukemia cells make energy
Gene activity maps and direct measurements of energy use showed that NOTCH1-mutated CLL cells run their powerhouses—mitochondria—much harder than cells without the mutation. These cells burned more fuel through both glycolysis (sugar breakdown) and mitochondrial respiration, produced more cellular “battery” molecules (ATP), and generated more reactive oxygen species, all signs of a revved-up engine. Microscopy revealed that NOTCH1-mutated cells had more and larger mitochondria forming dense networks, supported by extra mitochondrial DNA. When the BCR was triggered, this already high metabolic activity climbed even further, indicating that signals from outside the cell can push an already primed energy system into overdrive.
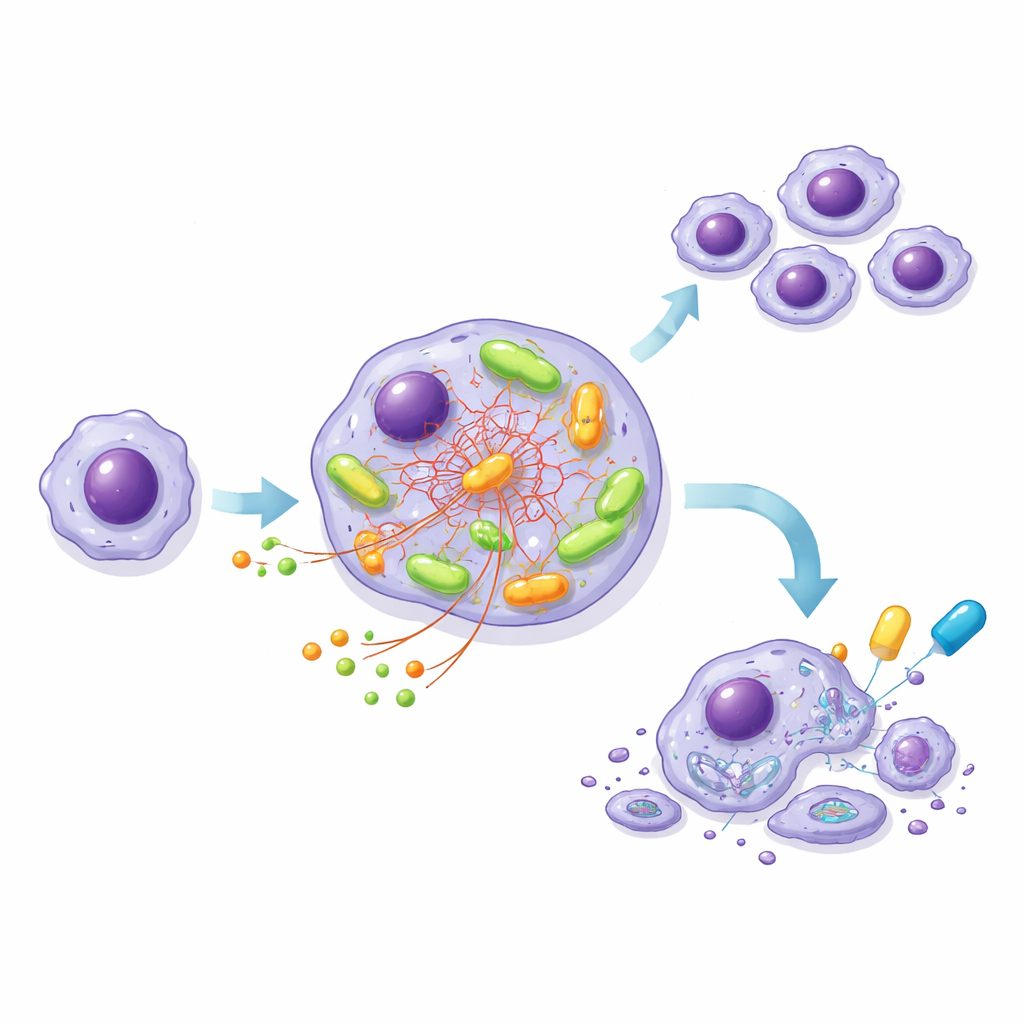
Building a model cell line to dissect the engine
Because patient CLL cells do not grow easily in the lab, the team engineered a leukemia-like cell line, MEC-1, in two versions: one with normal NOTCH1 and one with a truncated, overactive NOTCH1, both carrying the same high-risk BCR. This controlled system mirrored what was seen in patient samples. The mutant cells consumed more glucose, produced more ATP, and had higher oxygen use than their normal counterparts, especially after BCR activation. Detailed tracing experiments using labeled nutrients showed that, in mutant cells, glucose was shunted toward building blocks and protective molecules, while another nutrient, glutamine, became the main fuel feeding the central energy cycle inside mitochondria.
A master controller of mitochondria and a fuel addiction
To understand how NOTCH1 reshapes mitochondria, the researchers examined the chromatin landscape—the way DNA is packaged and marked for activity. They found that in mutant cells, the active form of NOTCH1 bound directly near a gene called TFAM, a key controller of mitochondrial DNA and function, and turned it up. Blocking TFAM reduced mitochondrial mass only in NOTCH1-mutated cells and triggered their death, showing that these cells are uniquely dependent on this mitochondrial program. Functionally, mutant cells grew faster than normal cells in mixed cultures. When the team blocked glutamine entry into cells, the growth advantage of mutant cells disappeared, and both the engineered cells and primary NOTCH1-mutated CLL cells became far more vulnerable, revealing a strong “addiction” to glutamine.
Turning a weakness into a treatment strategy
The study then tested whether this fuel dependence could help existing drugs work better. Venetoclax, a targeted drug that kills CLL cells by triggering mitochondrial cell death, was more effective against NOTCH1-mutated cells than against normal ones. Strikingly, combining glutamine transport blockade with venetoclax sharply increased leukemia cell death, and this synergy was specific to NOTCH1-mutated cells. Even a typically drug-resistant model carrying additional genetic damage became sensitive under this combination. In everyday terms, the mutation-heavy leukemia cells survive by running their mitochondria hot on glutamine; when that fuel line is cut and a pro-death signal is applied at the same time, their power system collapses and the cells cannot recover.
What this means going forward
In plain language, the authors show that a genetic change in NOTCH1, working together with signals received through the B-cell receptor, pushes certain CLL cells to build bigger, busier power plants and to rely heavily on the amino acid glutamine for energy and growth. That same dependence makes them unusually fragile when glutamine use is blocked, especially if combined with a drug like venetoclax that attacks mitochondria. Although more work in realistic patient-like settings is needed, this metabolic vulnerability offers a promising route to tailor treatment for people whose CLL carries NOTCH1 mutations, potentially improving outcomes by pairing standard targeted drugs with carefully chosen metabolic therapies.
Citation: Fascì, A., Vallone, F.E., Nabelsi, N. et al. Functional cooperation between the B-cell receptor and NOTCH1 in regulating metabolic reprogramming in chronic lymphocytic leukemia. Leukemia 40, 982–995 (2026). https://doi.org/10.1038/s41375-026-02912-7
Keywords: chronic lymphocytic leukemia, NOTCH1 mutation, cancer metabolism, mitochondria, glutamine dependence