Clear Sky Science · en
Molecular subtypes and the (in vitro) response of glioblastoma to temozolomide
Why this brain cancer study matters
Glioblastoma is the most common and deadly form of brain cancer in adults, and even the current standard drug, temozolomide, usually buys only months of extra life. This study asks a question with direct relevance for patients and clinicians: can the molecular "personality" of a glioblastoma help predict how it will respond to treatment, and why some tumors so quickly become drug‑resistant?
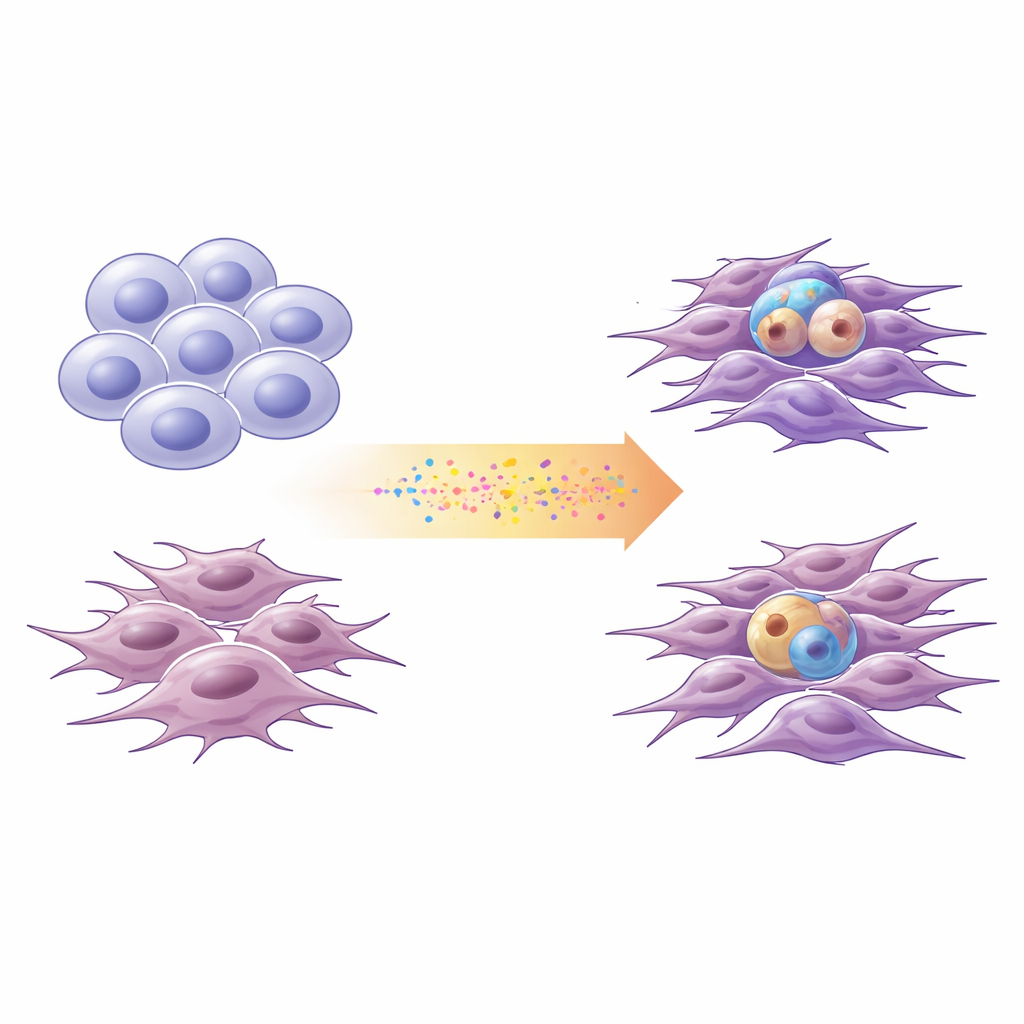
Two main flavors of glioblastoma
Researchers increasingly describe glioblastoma cells along a spectrum between two broad states. "Proneural" cells resemble immature nerve cells: they divide in a stem‑like way and can generate diverse descendants. "Mesenchymal" cells look more like stressed, hardened survivors: they are more mobile, invasive, and associated with inflammation. Using cells freshly derived from four patients, plus a standard lab cell line, the team profiled DNA changes and gene activity to place each culture on this proneural–mesenchymal axis. They confirmed that this simplified two‑state scale captured most of the transcriptional diversity seen in large public glioblastoma datasets.
Stem‑like behavior and the CD44 puzzle
Stem‑like properties—such as the ability to grow as free‑floating spheroids and to regenerate a mixed population—are often blamed for therapy resistance. The authors quantified a published four‑gene stemness program and found a striking pattern: cells at the proneural end of the spectrum consistently showed higher stemness scores, while mesenchymal cells scored lower. At the same time, they revisited a controversial surface molecule, CD44, sometimes called a stem cell marker. In their hands, higher CD44 tracked with the mesenchymal state and lower stemness, not the other way around, both in their own cultures and in independent datasets. When they physically separated low‑CD44 and high‑CD44 cells from a proneural culture, the low‑CD44 group behaved more like stem cells—more plastic and able to repopulate the original mix—whereas the high‑CD44 group looked more differentiated and mesenchymal‑like.
How tumor cells talk to their surroundings
CD44 is best known as a receptor for hyaluronic acid, a sugar‑rich component of the brain’s extracellular matrix. The team broadened their view to include many hyaluronic‑acid‑binding proteins. They found that mesenchymal cells were enriched in surface receptors that can latch onto and internalize this matrix, while proneural cells made more matrix‑building components that help shape a protective niche. Functionally, when they combined temozolomide with extra hyaluronic acid, mesenchymal cells slowed their migration, consistent with their heavier use of surface receptors, whereas proneural cells were less affected. This points to subtype‑specific ways in which the tumor and its microenvironment may reinforce one another.
Temozolomide pushes cells toward a tougher state
The core of the study addresses how these different cell states respond to temozolomide. In the first 24 hours, increasing drug doses curtailed the growth of mesenchymal cells, but barely touched the division rate of proneural cells. Over 72 hours and across a wide range of doses, overall drug sensitivity (the classic IC50 measure) did not simply follow subtype. However, when the team mimicked repeated clinical dosing—treating, allowing recovery, then treating again—proneural cultures stood out: after one exposure they became less proliferative but markedly more resistant to a second round, whereas mesenchymal cultures changed little in their sensitivity. Gene‑expression analysis showed that near‑toxic temozolomide doses drove a broad "mesenchymal shift" in all cells: pathways linked to inflammation and tissue remodeling rose, while stemness‑associated programs dropped, especially in initially proneural cells. Yet these proneural‑derived cells retained relatively high stem‑like potential, hinting that they may temporarily contract but later fuel relapse.
Oxygen levels tilt the balance of resistance
Real tumors are patchy in oxygen supply, and low‑oxygen pockets are known to foster treatment resistance. Using cobalt chloride to trigger a hypoxia‑like response, the researchers found that oxygen status interacted strongly with subtype. Under simulated hypoxia, proneural cells reduced proliferation but boosted metabolic activity, and when exposed to temozolomide in this state they survived better and migrated more. Mesenchymal cells, in contrast, tended to become more vulnerable to the drug under the same hypoxic signal. When the team plotted how hypoxia changed temozolomide potency against the stemness score, the cultures fell into two camps: high‑stemness, proneural‑like cells that became more drug‑resistant, and low‑stemness, mesenchymal‑like cells that became more sensitive.
What this means for patients and future therapies
For a lay reader, the key message is that not all glioblastomas are biologically alike, and these differences matter for how tumors endure and adapt to treatment. Tumors richer in proneural, stem‑like cells appear especially capable of weathering temozolomide, shifting toward a tougher mesenchymal‑like state while preserving a core of resilient cells, particularly under low‑oxygen conditions. The study suggests that CD44 and other hyaluronic‑acid‑related molecules are better viewed as hallmarks of this hardened mesenchymal identity, not simple stem cell flags. While based on a modest number of cell models and largely correlative, the work supports using a simple proneural–mesenchymal scale, plus stemness measures, to stratify glioblastomas and to design therapies that pre‑empt or disarm the most adaptable, relapse‑driving cells.
Citation: Rancati, S., Campolungo, M., Dalmolin, D.G. et al. Molecular subtypes and the (in vitro) response of glioblastoma to temozolomide. BJC Rep 4, 24 (2026). https://doi.org/10.1038/s44276-026-00228-8
Keywords: glioblastoma, temozolomide resistance, cancer stem cells, tumor hypoxia, molecular subtypes