Clear Sky Science · en
Hydrogen sulfide rescues IFNγ/TNFα-induced intestinal epithelial barrier dysfunction by enhancing oxidative phosphorylation
Why the Gut’s Thin Wall Matters
The lining of our intestines is just one cell thick, yet it separates the outside world in our gut from the rest of the body. When this barrier becomes “leaky,” bacteria and toxins can slip through, fueling inflammation not only in the digestive tract but also in the liver, brain, and other organs. This study explores how a small sulfur-containing molecule, which slowly releases hydrogen sulfide gas, can help protect this fragile wall during inflammation by boosting the cells’ energy production.
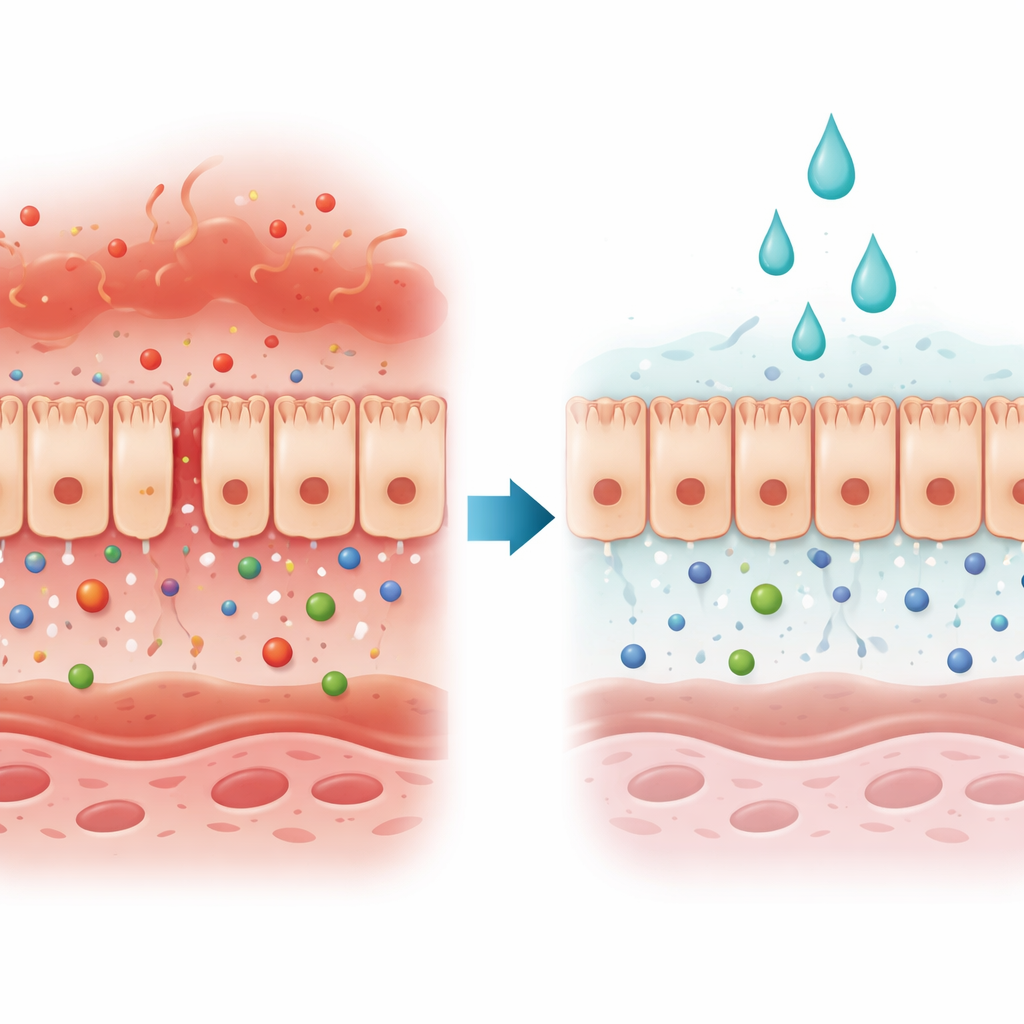
The Body’s Gatekeeper Under Attack
Intestinal epithelial cells form a continuous sheet that acts like a selective gate: it blocks harmful invaders while letting nutrients and water pass. In many gut and liver diseases, this gate fails because the spaces between cells open up or the cells die. The authors focused on a type of injury driven by two immune signals, interferon‑gamma and tumor necrosis factor‑alpha, which are abundant in inflammatory bowel disease. Together, these signals weaken the barrier and make it easier for substances in the gut to reach the bloodstream.
A Sulfur Donor with a Split Personality
The researchers studied 4‑hydroxithiobenzamide (TBZ), a compound that can release hydrogen sulfide, a gas that our own cells also produce at low, protective levels. In laboratory-grown intestinal cell layers and human intestinal organoids, TBZ had a curious, context‑dependent effect. On its own, it slightly increased leakiness between cells. But when the barrier had already been damaged by inflammatory signals, TBZ largely restored its function. It reduced electrical signs of barrier breakdown and brought the passage of a fluorescent tracer molecule back toward normal, even though it did not prevent cell death triggered by the cytokines.
Powering Up the Cell’s Energy Plants
To uncover how TBZ exerts this protective action, the team examined global gene activity in treated cells. They found that TBZ strongly turned on genes linked to oxidative phosphorylation — the process by which mitochondria, the cell’s “power plants,” make most of its ATP energy. Key components of mitochondrial complex IV and related transport proteins were upregulated, suggesting that TBZ was tuning the energy machinery rather than classic inflammation pathways. Follow‑up experiments confirmed this: under inflammatory conditions, TBZ boosted mitochondrial ATP production without changing glycolysis, indicating a targeted rise in high‑efficiency energy output.
When Mitochondria Falter, the Barrier Fails
The authors then tested whether this energy boost was required for barrier repair. They used sodium azide, a chemical that blocks complex IV in mitochondria. At a dose that did not kill the cells outright, sodium azide nearly shut down oxidative phosphorylation while leaving glycolysis largely intact. In inflamed cells treated with TBZ, adding sodium azide erased the protective barrier effect: electrical resistance dropped again and the fluorescent tracer leaked through more readily. Even though the cells shifted somewhat toward glycolysis as compensation, total ATP fell and the barrier did not recover, tying intact mitochondrial respiration directly to barrier integrity.
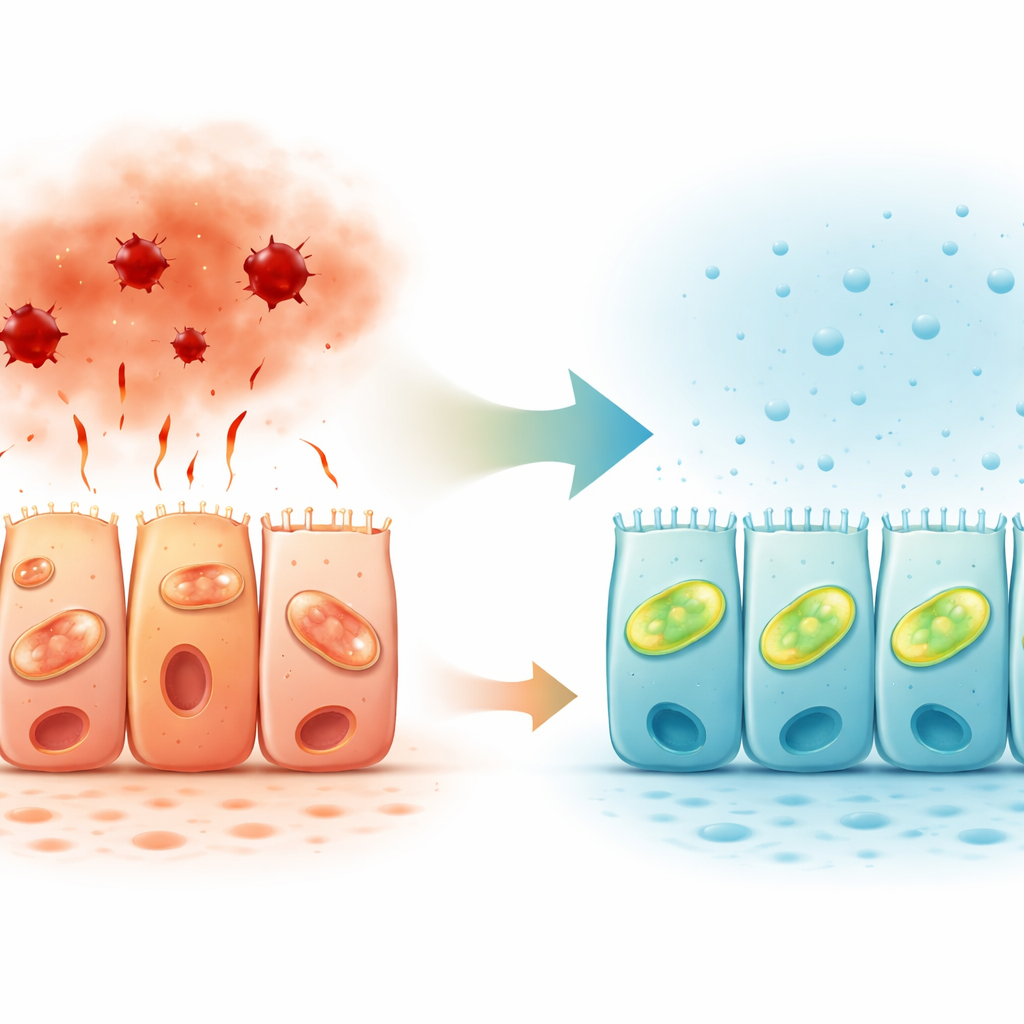
Natural Gas Signals in the Gut Lining
Looking at human colon tissue, the researchers also mapped where hydrogen sulfide–producing enzymes are found. Two such enzymes were most strongly expressed in the upper, gut‑facing side of epithelial cells, especially in the ascending colon. This polarized pattern supports the idea that hydrogen sulfide acts locally at the surface where the barrier meets the gut contents, fine‑tuning how cells respond to stress. Combined with previous work showing reduced hydrogen sulfide pathways in inflammatory bowel disease, the findings suggest that diminished gas signaling may contribute to barrier failure in patients.
What This Means for Future Treatments
Altogether, the study shows that a hydrogen sulfide–releasing compound can rescue an inflamed, leaky intestinal barrier by dialing up mitochondrial energy production, specifically through oxidative phosphorylation, even though it does not stop inflammatory cell death itself. For a layperson, the message is that keeping the gut wall tight may depend as much on feeding the cells’ power plants as on blocking inflammation. Drugs inspired by TBZ, or targeted hydrogen sulfide donors, could one day help stabilize the gut barrier in conditions like inflammatory bowel disease or liver disease. However, because TBZ can also increase leakiness when inflammation is absent, the work also highlights the need to match such therapies carefully to the right context and dose.
Citation: de Oliveira, J.P., van Sligtenhorst, M., Akkaya, C. et al. Hydrogen sulfide rescues IFNγ/TNFα-induced intestinal epithelial barrier dysfunction by enhancing oxidative phosphorylation. Sci Rep 16, 10208 (2026). https://doi.org/10.1038/s41598-026-40348-2
Keywords: intestinal barrier, hydrogen sulfide, mitochondria, inflammation, epithelial cells