Clear Sky Science · en
DPEP2 suppresses hyperinflammation via metabolic reprogramming of macrophages in sepsis
Why calming the body’s overreaction matters
Sepsis is a life-threatening condition in which the body’s immune system, trying to fight infection, goes into overdrive and starts damaging its own organs. Despite antibiotics and modern intensive care, many people still die because this runaway inflammation is hard to control without shutting down vital defenses. This study uncovers a natural “brake” molecule in frontline immune cells and shows how boosting it with a gene-based therapy could quiet harmful inflammation while preserving the ability to fight germs.
A hidden brake inside infection-fighting cells
The researchers focused on monocytes and macrophages, immune cells that circulate in the blood and patrol organs, sounding the alarm when microbes invade. Using cutting-edge single-cell and bulk RNA sequencing on blood from patients in the early phase of sepsis, they mapped gene activity cell by cell. One gene, called DPEP2, stood out: it was strongly active in healthy monocytes and macrophages but consistently reduced in patients with sepsis. Lower DPEP2 levels were tightly linked with worse organ failure scores, higher levels of inflammatory molecules in the blood, and a higher risk of death. Patients who survived had more DPEP2-positive monocytes than those who did not, suggesting this molecule helps restrain the immune system’s most dangerous impulses.
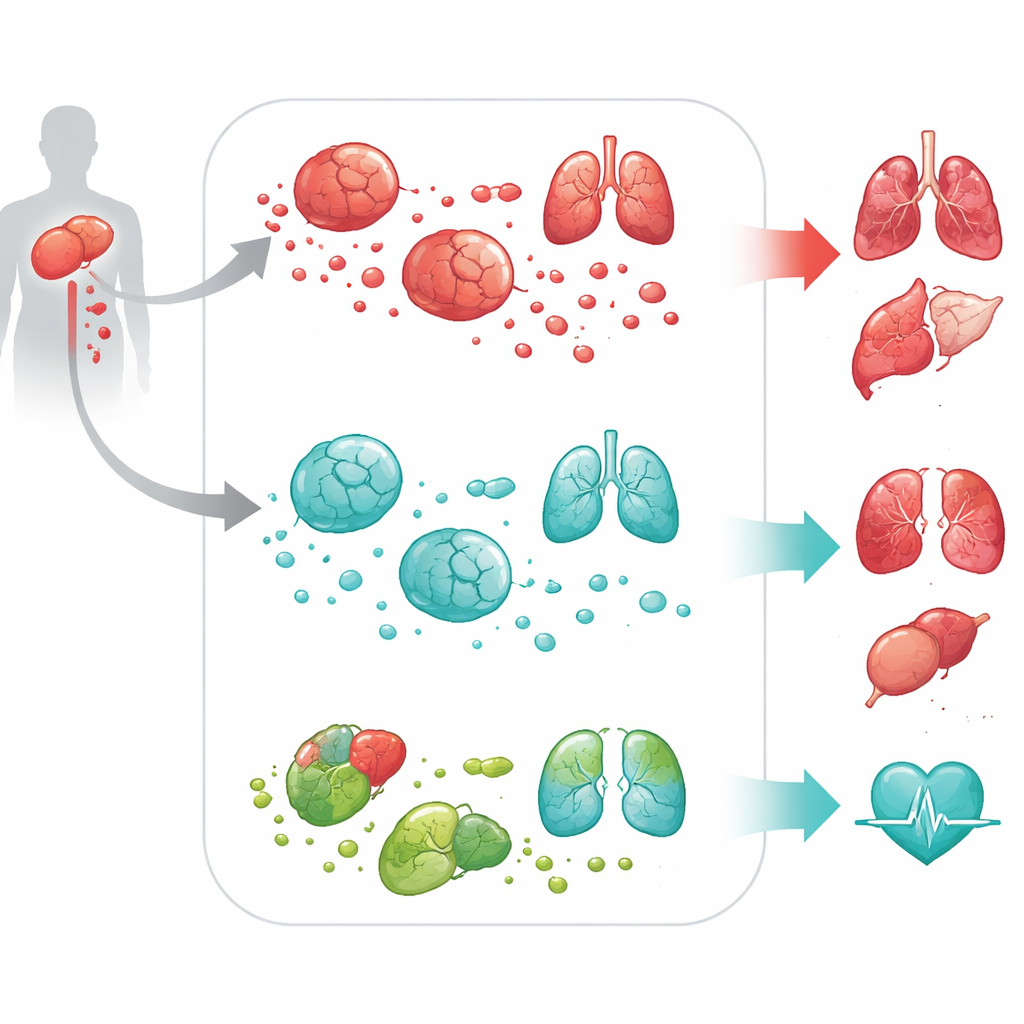
From gene signal to whole-body damage
To test whether DPEP2 was merely a bystander or an active protector, the team turned to cell and animal models. In mouse and human macrophages grown in the lab, switching off DPEP2 caused these cells to pump out far more inflammatory cytokines when stimulated with bacterial components. In mice subjected to a standard, surgery-based model of sepsis, animals lacking DPEP2 – either throughout the body or specifically in macrophages – fared much worse. They had higher levels of inflammatory molecules in the bloodstream, more severe lung, liver, kidney, heart, and brain injury, and significantly higher death rates. These experiments showed that DPEP2 is not just a marker of disease severity but an active defender against overwhelming inflammation.
How a fat-processing enzyme tames fire
DPEP2 works by reshaping how macrophages handle certain fatty molecules that act as powerful local hormones. In particular, it helps break down a compound called leukotriene D4 into a less inflammatory product, and its loss causes leukotriene D4 to build up. That buildup, in turn, pushes more of the cell’s fatty building blocks toward making prostaglandin E2, another strong driver of inflammation. Together, these lipids feed into a major switch inside the cell known as NF-κB, which controls genes for many inflammatory cytokines. When DPEP2 is missing or low, this network of fat-based signals runs unchecked, stepping on NF-κB and causing macrophages to flood the body with damaging inflammatory factors.
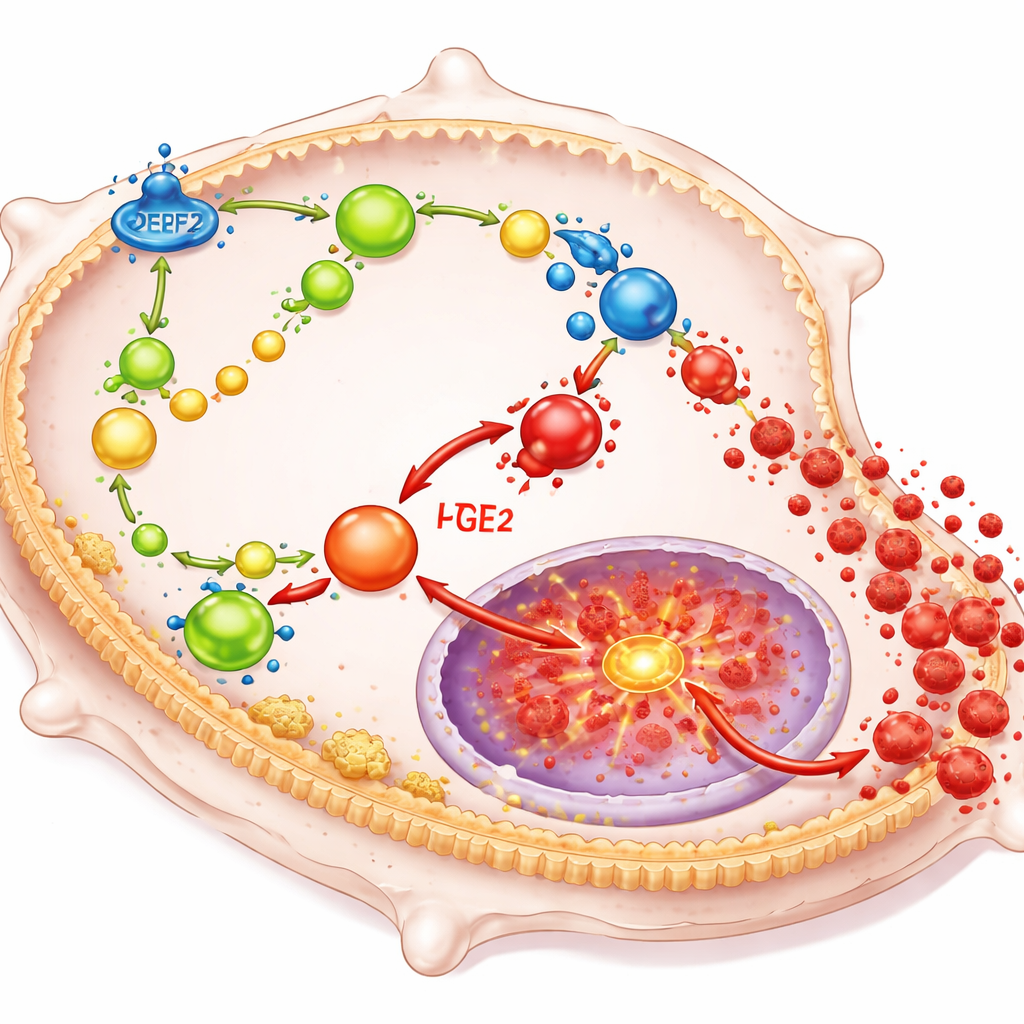
Rewriting immune cells with mRNA
Armed with this mechanistic insight, the scientists asked whether restoring DPEP2 could help rescue animals from sepsis. They designed lipid nanoparticles—tiny fat bubbles similar to those used in mRNA vaccines—to deliver Dpep2 mRNA specifically into monocytes and macrophages. After intravenous injection, these particles briefly boosted DPEP2 levels in the target cells. In septic mice treated with the Dpep2-loaded nanoparticles, inflammation markers dropped, lung and organ damage eased, and survival improved compared with control animals. Importantly, the treatment worked without obvious toxicity and faded after about a day and a half, aligning with the critical early window when sepsis deaths most often occur.
What this means for future sepsis care
This work reveals DPEP2 as a crucial natural safeguard that keeps infection-fighting cells from tipping the body into lethal self-damage. By showing that DPEP2 levels in blood monocytes reflect disease severity, the study suggests it could serve as a useful blood biomarker to flag patients at highest risk. Even more striking, the success of the Dpep2 mRNA–nanoparticle therapy in mice points to a new class of precision treatments: instead of broadly suppressing immunity, clinicians might one day fine-tune specific metabolic switches inside immune cells to cool the inflammatory storm in sepsis while preserving host defense.
Citation: Luo, W., Xu, W., Yin, Q. et al. DPEP2 suppresses hyperinflammation via metabolic reprogramming of macrophages in sepsis. Nat Commun 17, 3710 (2026). https://doi.org/10.1038/s41467-026-70466-4
Keywords: sepsis, macrophages, immunometabolism, lipid mediators, mRNA therapy