Clear Sky Science · en
Spatially resolved osteoblast-traced transcriptomics uncovers TGF-β as a combination target with sclerostin in osteoporosis
Why this bone study matters
Osteoporosis causes bones to become fragile and easy to break, especially in older adults. Many current drugs either slow bone breakdown or briefly boost bone building, but they can have side effects and their benefits may fade. This study explores how quiet bone-forming cells can be switched back on, and suggests a new combination treatment strategy that could help strengthen bones more powerfully and lastingly.
Silent workers on the bone surface
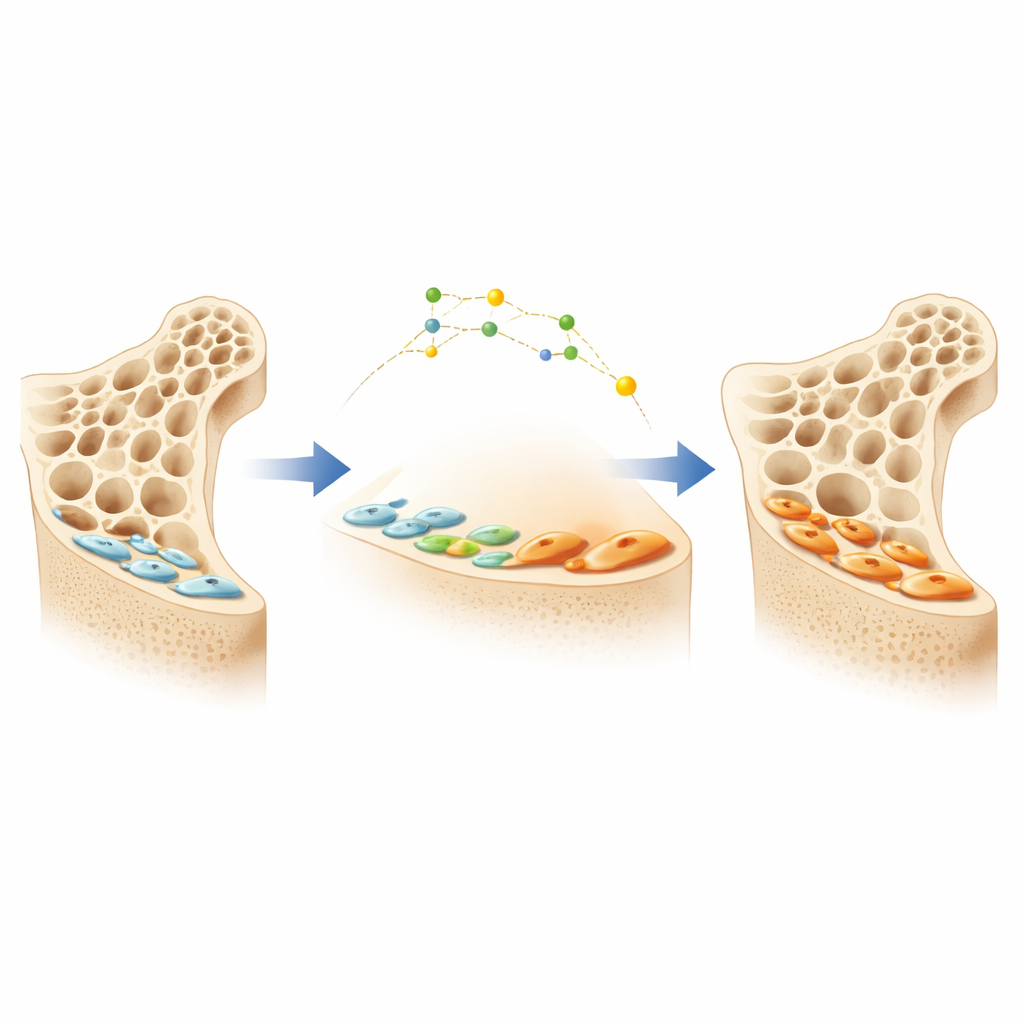
Bones are constantly remodeled by two main cell types: osteoclasts, which remove old bone, and osteoblasts, which lay down new bone. When osteoblasts finish a burst of work, many do not die; instead, they flatten out and become thin “bone lining cells” that sit quietly on the bone surface. These silent cells form a large hidden reserve of potential bone builders. A newer osteoporosis drug that blocks a protein called sclerostin can wake up these lining cells and turn them back into active osteoblasts, leading to rapid gains in bone mass. However, the details of how lining cells switch between quiet and active states have been unclear, making it hard to design smarter, longer-lasting therapies.
Tracking bone cells in place
The researchers developed an approach they call “spatially resolved osteoblast-traced transcriptomics” to watch these transitions directly inside mouse bone. First, they used a genetic labeling system so that mature osteoblasts and their descendants glowed green, allowing the team to follow them as they became lining cells or were reactivated by sclerostin-blocking antibodies. Then they combined this with a laser-based sampling method that can gently cut out tiny, precisely chosen regions from bone slices while keeping each cell’s RNA intact. By sequencing RNA from these regions, they could see which genes were turned on or off in active osteoblasts, quiet lining cells, and reawakened cells, all while preserving where those cells sat on the bone surface.
A key brake on bone-building
When the team compared the gene activity patterns of active, inactive, and reactivated osteoblasts, one signaling system stood out as a powerful brake: the pathway controlled by transforming growth factor beta (TGF-β). Quiet lining cells showed stronger TGF-β activity, while active osteoblasts—whether naturally active or reawakened by sclerostin blockade—showed weaker TGF-β signals. Single-cell sequencing, which analyzes thousands of individual bone cells, confirmed that the most active osteoblasts consistently had low TGF-β signaling. In lab-grown bone organoids, adding TGF-β pushed osteoblasts to become thinner, less proliferative, and more lining cell–like. These findings point to TGF-β as a switch that promotes quiescence and restrains bone-building activity.
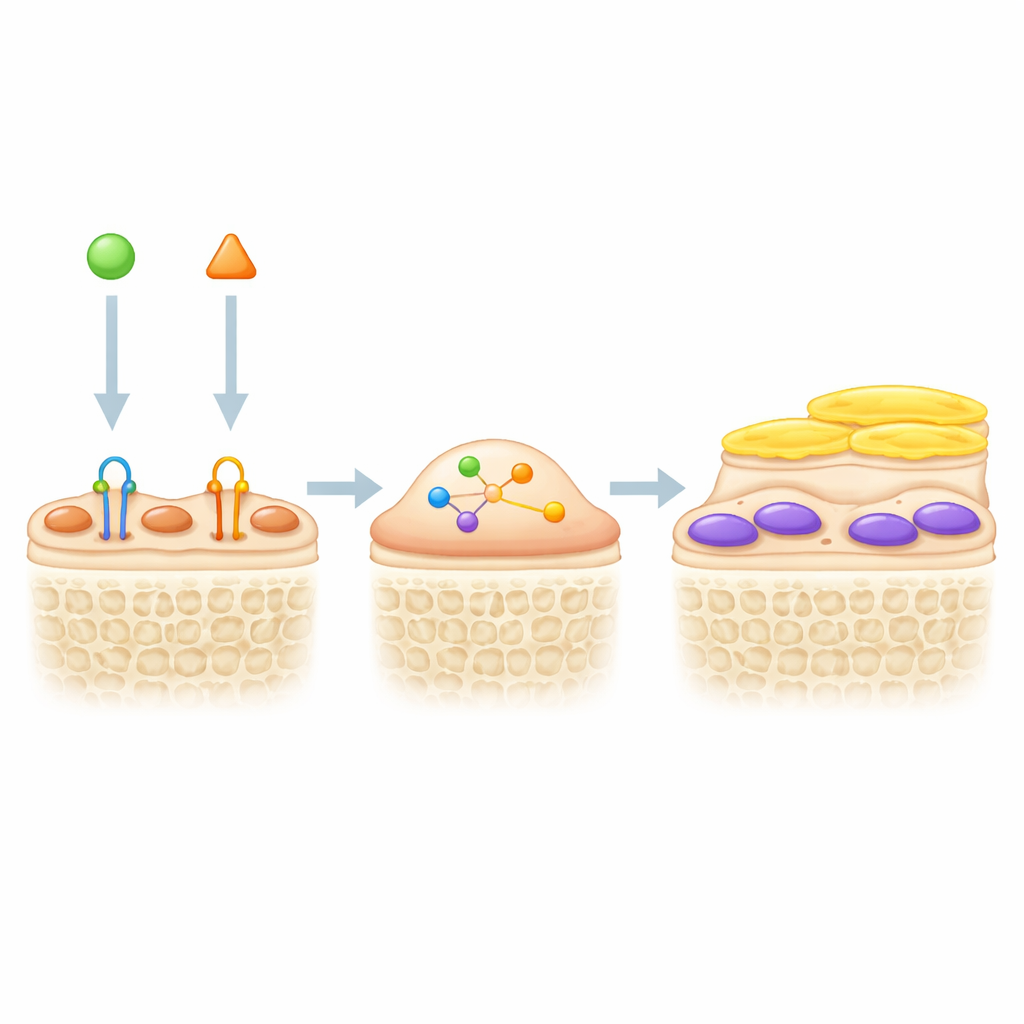
Combining two levers for stronger bones
Because sclerostin blockade wakes up lining cells and TGF-β keeps them quiet, the authors tested whether blocking both signals together would boost bone formation. In genetically labeled mice, a TGF-β–blocking antibody increased the thickness and number of active green osteoblasts on bone surfaces, especially when combined with sclerostin-blocking treatment. In a hindlimb unloading model, which mimics bone loss from inactivity or spaceflight, sclerostin blockade alone increased bone mass, but the dual treatment did even better. Mice receiving both antibodies had higher trabecular bone volume, thicker and more numerous bone struts, more bone formation, and fewer bone-resorbing cells than mice given either drug alone. Blood markers and tissue staining suggested that TGF-β inhibition not only helped reactivate lining cells but also reduced bone resorption, acting through mechanisms that complement sclerostin blockade.
What this could mean for patients
This work links a specific signaling pathway, TGF-β, to the decision bone cells make between resting and building, and shows that dialing down this signal can amplify the benefits of a powerful existing osteoporosis drug that targets sclerostin. While these experiments were performed in mice and important safety questions remain—because TGF-β acts in many organs—the study suggests that carefully tuned dual therapies could both stir sleeping bone builders and temper bone breakdown. In the long run, this strategy could translate into more robust, durable treatments for people living with osteoporosis and other conditions marked by excessive bone loss.
Citation: Choi, A., Lee, J.Y., Yoon, H. et al. Spatially resolved osteoblast-traced transcriptomics uncovers TGF-β as a combination target with sclerostin in osteoporosis. Bone Res 14, 37 (2026). https://doi.org/10.1038/s41413-026-00521-9
Keywords: osteoporosis, osteoblasts, bone remodeling, TGF-beta signaling, sclerostin inhibition