Clear Sky Science · en
Comparative effectiveness of alloplastic and biologic grafts in maxillary sinus augmentation: a systematic review
Why this matters for people with missing back teeth
When people lose their back teeth in the upper jaw, the bone in that area often shrinks and a nearby air space, the maxillary sinus, expands. This combination can leave too little bone to safely anchor dental implants. To rebuild the area, dentists lift the floor of the sinus and pack the space with graft material that will support new bone growth. This article reviews which grafts work better: biologic materials taken from people or animals, or fully synthetic “alloplastic” materials made in a lab.
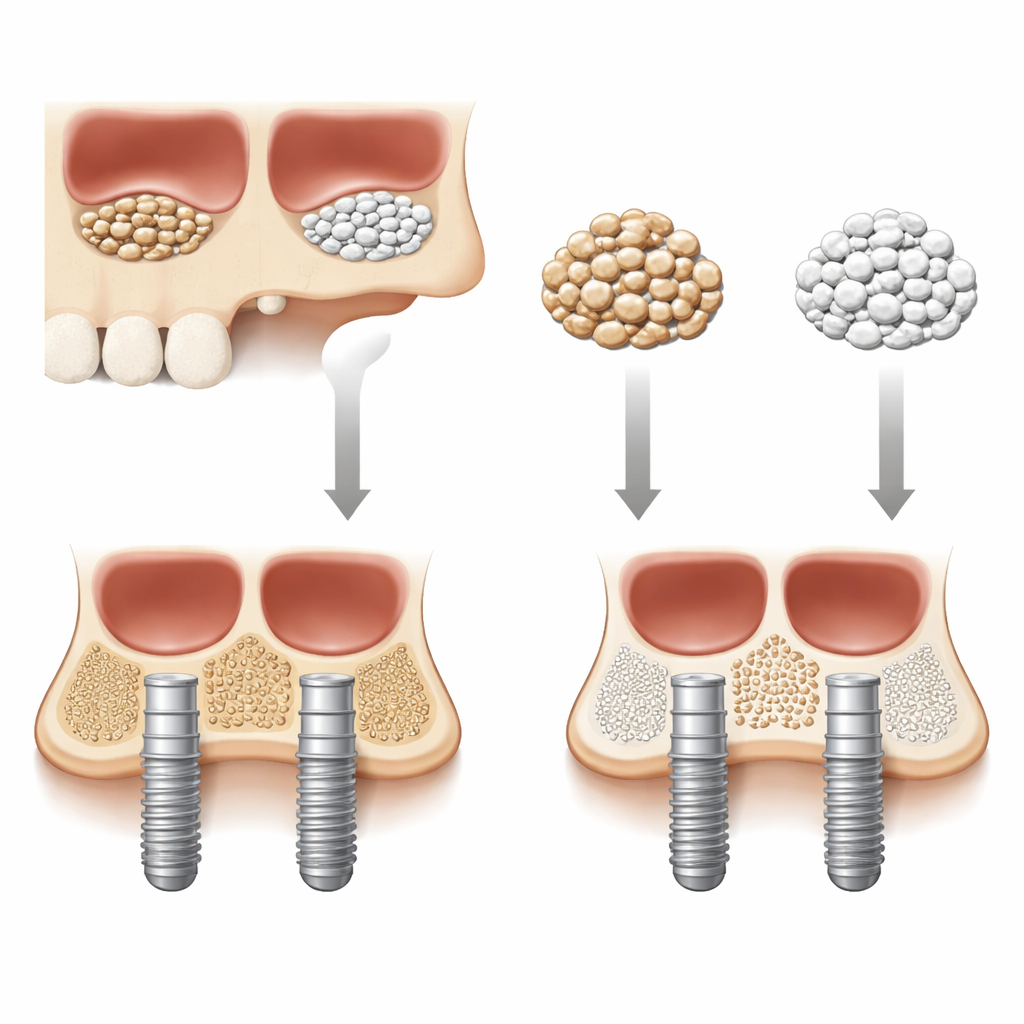
Different ways to rebuild lost jawbone
Surgeons can choose from several types of grafts. Autografts are pieces of a patient’s own bone, often taken from the jaw; they are considered the traditional gold standard because they contain living bone cells and natural growth signals. Allografts come from donated human bone, while xenografts are processed bone from animals, usually cattle or pigs, that is cleaned to leave only a mineral scaffold. Alloplastic grafts are entirely artificial granules made from ceramics such as hydroxyapatite, beta-tricalcium phosphate, biphasic calcium phosphate, or bioactive glass. They avoid the need for a second surgical site and remove concerns about disease transmission, but dentists still question whether they can match the healing ability of biologic bone.
How the researchers compared graft options
The authors systematically searched eight major medical databases for human clinical studies published between 2010 and 2025. They included randomized trials and clinical cohort studies in which patients received sinus lift surgery with at least two different graft types, such as synthetic versus animal-derived materials. To be eligible, studies had to report on new bone formation, how much graft material remained over time, changes seen on scans, implant survival, or complications. In total, 18 studies involving a range of grafts and follow-up times from five months to several years were analyzed. Because the procedures, materials, and measurement methods varied widely, the team summarized the findings qualitatively instead of combining them into a single pooled statistic.
What they found about new bone and graft behavior
Across the studies, the patient’s own bone generally produced the highest amount of new bone in the early healing period, followed by donor and animal grafts. Alloplastic materials usually created somewhat less new bone during the same time frame and left more residual particles behind. This pattern suggests that biologic grafts are integrated and remodeled more efficiently, while synthetic particles tend to persist longer. That slower turnover can be a mixed blessing: synthetic grafts often helped maintain space and volume under the sinus, but some trials showed that animal-derived materials were even better at holding their shape over time. Advanced scans and microscopic analyses also revealed that synthetic grafts showed more signs of active remodeling, whereas animal grafts acted as a stable long-lasting scaffold.
What this means for implant success and patient outcomes
Despite these biological differences, implant survival was high—typically above 90 percent—for all graft types studied. In many trials, synthetic and biologic grafts supported implants equally well, though animal or donor grafts sometimes showed slightly less marginal bone loss or fewer failures. Alloplastic materials had another clear advantage: they did not require a second surgery to harvest bone and carried no risk of immune reaction or disease transmission from human or animal sources. This makes them particularly attractive for patients with medical conditions, those needing grafts on both sides, or those who wish to avoid extra surgery. However, the overall certainty of the evidence was rated low, due to modest sample sizes, mixed study quality, and limited long-term follow-up.
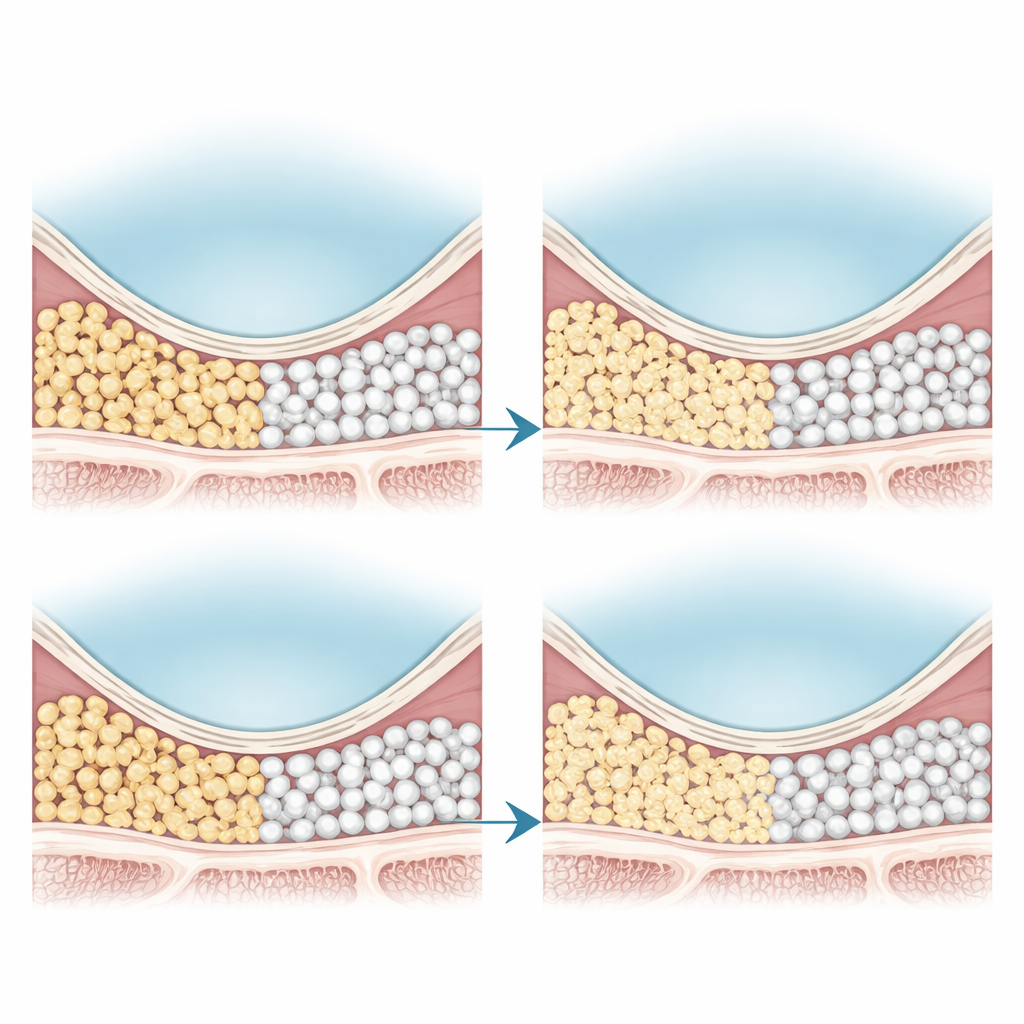
Take‑home message for patients considering implants
Overall, the review concludes that a patient’s own bone remains the most powerful option for rebuilding the sinus area, with animal and donor grafts close behind, and synthetic grafts somewhat less active in forming new bone. Even so, synthetic materials still provide enough support for successful implants in many cases and can be the preferred choice when avoiding extra surgery or reducing medical risks is more important than maximizing early bone growth. Because the existing studies are small and varied, the authors emphasize the need for large, long-term clinical trials to refine graft selection. For patients, the key message is that several safe and effective options exist; the “best” graft depends on personal health, anatomy, and priorities, and should be chosen in close discussion with the treating dentist or surgeon.
Citation: Thomas, J.V., Martande, S., Meenathathil, J.T. et al. Comparative effectiveness of alloplastic and biologic grafts in maxillary sinus augmentation: a systematic review. BDJ Open 12, 46 (2026). https://doi.org/10.1038/s41405-026-00435-y
Keywords: sinus lift, dental implants, bone graft materials, synthetic bone grafts, maxillary sinus augmentation