Clear Sky Science · en
ENA1 deficiency attenuates Saccharomyces ‘boulardii’ probiotic yeast virulence in immunosuppressed mouse fungaemia model
Why a Helpful Yeast Can Sometimes Turn Harmful
Many people swallow probiotic yeast pills to calm an upset gut or prevent diarrhea during antibiotic treatment. One of the most popular choices is a yeast often sold under the name Saccharomyces boulardii. While it helps many patients, doctors are seeing a worrying trend: in some very sick or immune‑weakened people, this friendly yeast can slip from the intestine into the bloodstream and cause serious, sometimes deadly, infections. This study asks a pressing question for modern medicine: can we redesign this probiotic so it keeps its gut benefits but becomes much less able to cause dangerous bloodstream infections?
Growing Concerns in Fragile Patients
Hospitals around the world increasingly report cases where the probiotic yeast shows up in the blood of patients in intensive care units, after surgery, or during severe illness. These people often have weakened defenses and invasive devices like catheters, which give microbes new routes into the body. In some hospitals, infections linked to this probiotic yeast occur almost as often as those from classic disease‑causing fungi. Yet, until now, most research on this yeast has focused either on its health benefits or on ways to engineer it to make drugs, with little attention to what actually makes it risky for vulnerable patients. The authors set out to bridge this gap by studying both its helpful and harmful sides in the same project.
Tracking Virulence Inside Mice
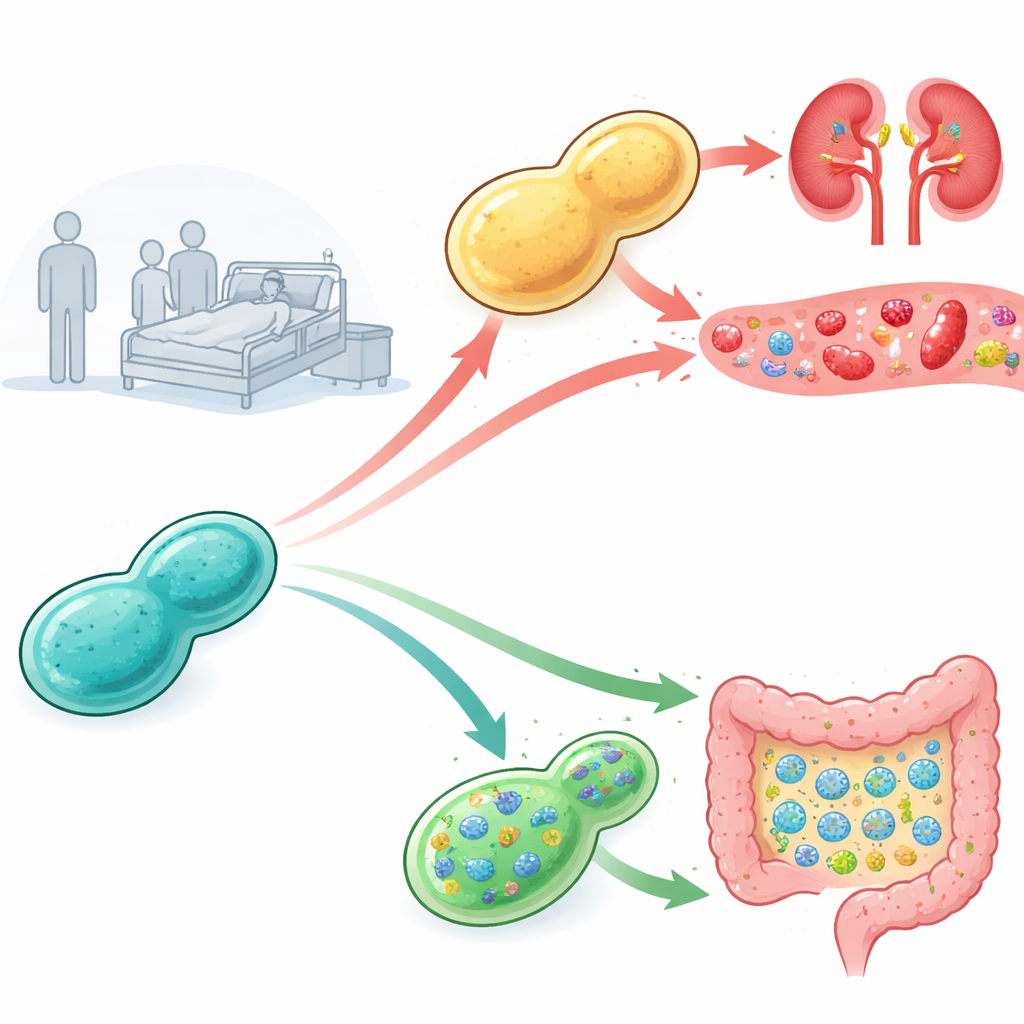
The researchers collected probiotic yeast from commercial products and from hospital patients and tested how dangerous each was in mice with weakened immune systems. All mice injected with yeast from commercial products survived, but some patient‑derived yeasts caused high death rates and heavy fungal growth in the kidneys, a sign of severe bloodstream infection. To understand why, the team isolated many sub‑lineages of the yeast before and after infection and challenged them with different stresses on laboratory plates. They noticed that the more virulent patient isolates, and especially the versions that had passed through mice, were unusually tolerant to salty conditions containing sodium or lithium salts, hinting that the ability to withstand harsh internal environments might be tied to their capacity to cause disease.
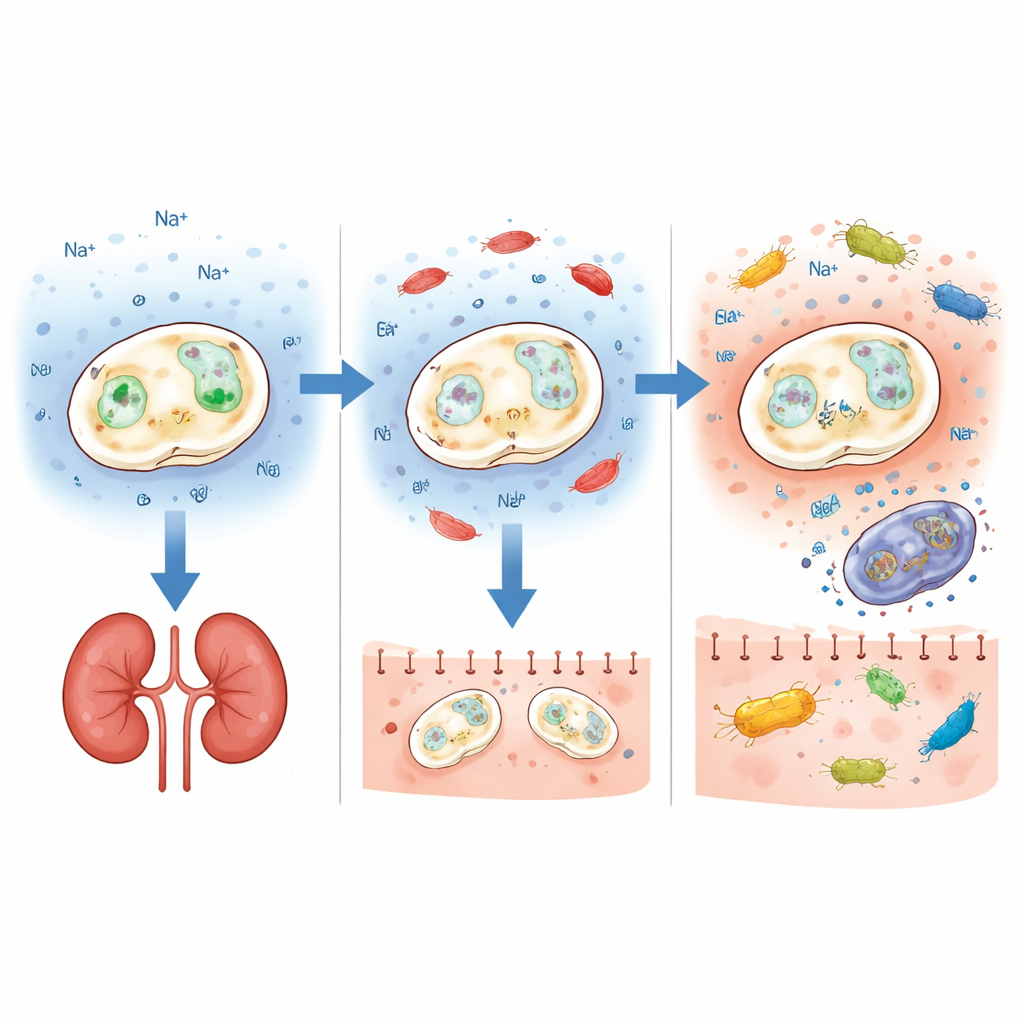
Disarming a Key Survival Pump
Salt tolerance in yeast depends on membrane transporters that pump ions in and out of the cell. The authors focused on two such genes, ENA1 and NHA1, which help cells survive salt and alkaline stress. Using CRISPR gene editing, they deleted each gene separately in six different probiotic backgrounds, including both commercial and clinical isolates. The results were strikingly clear for one gene: when ENA1 was removed, every tested strain caused much less harm in mice. All animals survived short‑term bloodstream infection, and fungal levels in the kidneys stayed relatively low, even when the starting strain was originally quite virulent. In contrast, deleting NHA1 did not give a consistent safety benefit and sometimes even made strains more harmful, underlining how the impact of a genetic change can depend strongly on the broader genetic background.
Keeping the Benefits, Adding a Bonus Weapon
A safer probiotic is only useful if it still performs its intended job in the gut. The team therefore checked whether ENA1‑deficient strains could still grow well in standard culture media and under gut‑like conditions, including moderate acidity, bile salts, and the pH levels found along the small intestine and large intestine. The ENA1 knockout behaved much like the original probiotic, except it struggled only under unusually high alkaline or salty conditions not typical of the healthy gut. In live mice given daily doses by mouth, the modified yeast colonized the intestine to similar levels as the commercial strain and was cleared at a similar pace once dosing stopped. The altered strain also shifted the composition and diversity of the gut bacterial community in much the same way as the original probiotic, suggesting that its overall gut impact remained intact.
Building a Safer Platform for Future Therapies
Beyond safety, the authors showcased what a “designer” probiotic could do. In a proof‑of‑concept step, they replaced the ENA1 gene with DNA encoding Leucocin C, a short antibacterial peptide targeted against Listeria, a serious foodborne pathogen. The engineered yeast still showed drastically reduced ability to cause bloodstream infections in mice, grew well in lab tests, survived freeze‑drying procedures used in commercial production, and secreted an active peptide that inhibited Listeria in culture. Taken together, these results suggest that knocking out ENA1 creates a promising platform strain: a yeast that is far less likely to cause life‑threatening fungaemia in fragile patients, yet retains its probiotic behavior and can be further equipped to fight harmful bacteria. In simple terms, the study demonstrates that it is possible to transform a sometimes risky helper into a safer, programmable ally for future gut‑based therapies.
Citation: Imre, A., Kovács, R., Jakab, Á. et al. ENA1 deficiency attenuates Saccharomyces ‘boulardii’ probiotic yeast virulence in immunosuppressed mouse fungaemia model. Commun Biol 9, 542 (2026). https://doi.org/10.1038/s42003-026-09763-z
Keywords: probiotic yeast, fungemia, gene editing, microbiome, designer probiotics