Clear Sky Science · en
Lipid alterations and endothelial dysfunction are associated with multiple sclerosis pathophysiology
Why Blood Fats and Blood Vessels Matter in Multiple Sclerosis
Multiple sclerosis is usually described as a disease of the brain and spinal cord, driven by the immune system attacking nerve insulation. Yet people with MS also live in bodies with beating hearts and circulating blood. This study asks a deceptively simple question with big implications: do changes in blood fats and blood vessel health outside the brain quietly shape how MS unfolds over time?
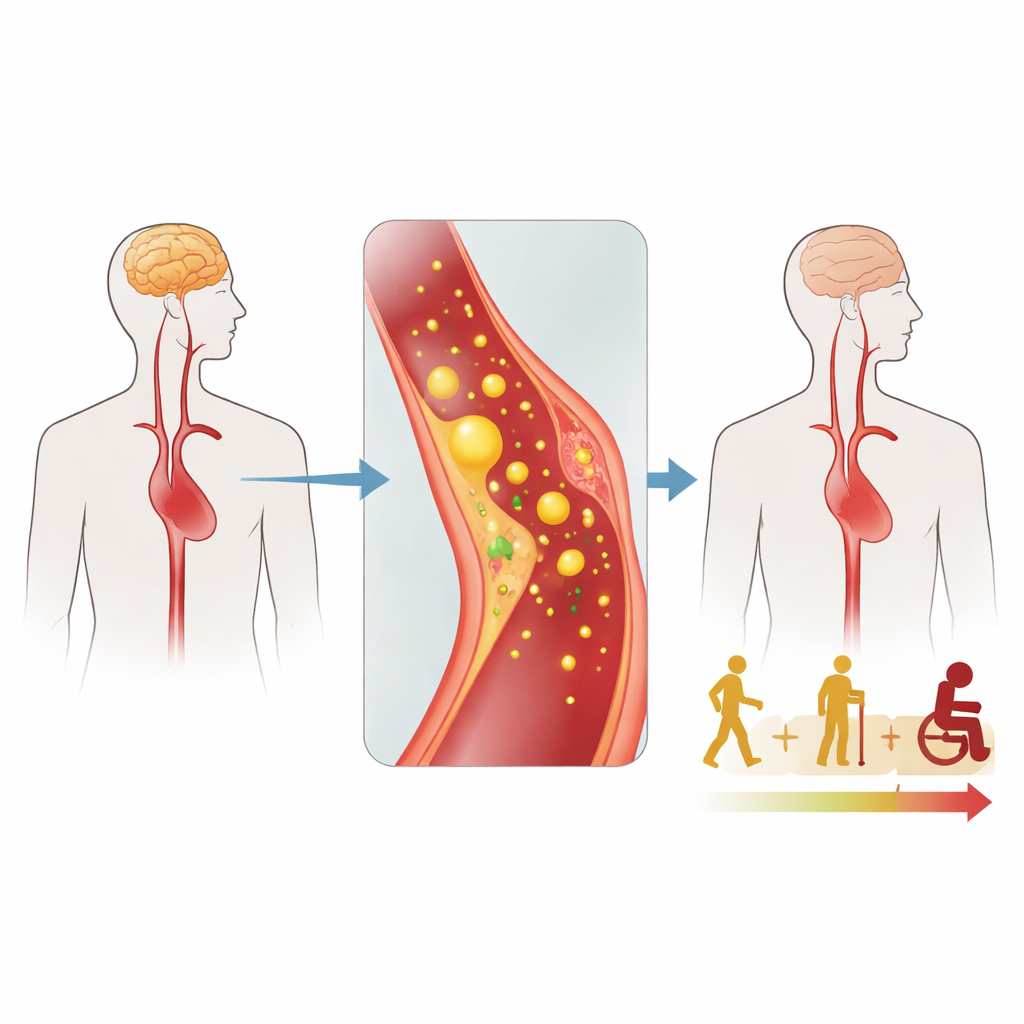
Looking Beyond the Brain
The researchers focused on people with relapsing–remitting multiple sclerosis, the most common early form of the disease, and compared them with healthy volunteers. Instead of only scanning the brain, they also drew blood and used ultrasound to look at the neck arteries that feed the brain. In the blood, they measured standard cholesterol markers and two molecules shed by activated blood vessel lining cells, called selectins. In the arteries, they measured the combined thickness of the inner and middle layers of the vessel wall, a structural feature known to change when vessels are repeatedly stressed or inflamed.
Unexpected Patterns in Cholesterol
Compared with healthy people, those with MS had clearly altered blood fat profiles. Total cholesterol, “bad” cholesterol carried by low-density particles, and the combined pool of all cholesterol outside the “good” fraction were all higher in the MS group. Even high-density cholesterol, often considered protective, was increased. Higher levels of several of these fats tracked with greater disability on a standard MS scale and with longer disease duration, hinting that disturbed fat handling in the body may go hand in hand with a heavier disease burden. These shifts are thought to reflect the breakdown of the fatty myelin coating in the brain and the brain’s attempt to clear and export excess cholesterol into the circulation.
Signals from the Vessel Wall
The story did not end with cholesterol. One of the vessel-activation markers, soluble E-selectin, was significantly higher in the MS group, indicating that the cells lining blood vessels were in a more activated, inflammatory state. Intriguingly, higher levels of “good” high-density cholesterol were linked to lower E-selectin, supporting the idea that this cholesterol fraction may help calm down irritated vessel walls. When the team looked more closely, they found that both E-selectin and its cousin P-selectin were tied to subtle structural changes in the carotid arteries, reinforcing the picture of a vascular system that is actively remodeling in response to ongoing immune activity.
Thinner Arteries, Not Clogged Ones
Perhaps the most surprising finding was what the ultrasound scans revealed. Despite having a more worrisome cholesterol pattern and a slightly higher body mass index, people with MS actually had thinner carotid artery walls than the carefully screened healthy controls. In the general population, thicker artery walls usually signal the build-up of atherosclerosis, the process that leads to heart attacks and strokes. Here, the opposite pattern suggests something different: instead of classic fatty clogging, the vessel walls in MS appear to be undergoing an immune-driven reshaping. Even so, within the MS group, people with greater disability and longer disease duration tended to have thicker walls than their peers, implying that this remodeling progresses alongside the illness.
What This Means for People Living with MS
Taken together, the results point to MS as more than a disease confined to the brain and spinal cord. Disturbed handling of cholesterol and a constantly alerted vessel lining appear to extend throughout the body and to track, albeit modestly, with how disabled a person becomes and how long they have lived with MS. At the same time, the unusual pattern of thinner artery walls argues that, at least in earlier stages, these changes do not simply mirror the artery clogging seen in heart disease. Instead, they likely reflect a different kind of immune-related reshaping of blood vessels. Recognizing this broader vascular component may open the door to new ways of monitoring MS and, eventually, to treatments that protect not only nerve fibers but also the delicate interface between blood and brain.
Citation: Damiza-Detmer, A., Pawełczyk, M., Bednarski, I. et al. Lipid alterations and endothelial dysfunction are associated with multiple sclerosis pathophysiology. Sci Rep 16, 14263 (2026). https://doi.org/10.1038/s41598-026-44767-z
Keywords: multiple sclerosis, cholesterol, blood vessels, endothelium, carotid ultrasound