Clear Sky Science · en
Lactic acid drives NLRP3 inflammasome activation and caspase-1–like cytokine cleavage via intracellular acidification
When a Workout Molecule Turns Against Us
Lactic acid is famous for the burn you feel in your muscles after a hard run, but it also builds up during severe infections like sepsis. This study reveals that lactic acid can act as more than a simple waste product: inside immune cells, it helps switch on powerful inflammatory machinery and can even chemically cut key immune messengers on its own. Understanding this double life of lactic acid could reshape how we view inflammation in sepsis, cancer, and other serious illnesses. 
How Immune Cells Sense Danger
Our first line of defense against infection relies on innate immune cells, such as macrophages, that quickly sense danger and release alarm signals. A central control hub inside these cells, called the NLRP3 inflammasome, responds to a wide range of threats and activates an enzyme that chops inactive cytokine precursors into their active forms. These active fragments, especially IL-1β and IL-18, are then secreted to rally other immune cells. While this response can help clear infections, when it runs too hot it contributes to life-threatening conditions like septic shock.
Fuel Use, Cell Acidity, and an Immune Switch
To power this rapid alarm system, macrophages shift their metabolism toward glycolysis, a fast way to break down sugar that produces lactic acid. The researchers showed that when NLRP3 is triggered, immune cells quickly increase lactic acid production and trap more of it inside. This build-up acidifies the cell interior and, in turn, strongly boosts inflammasome assembly, enzyme activation, and IL-1β release. Acidic conditions outside the cell block lactic acid from leaving, further deepening the internal acid shift and amplifying the response. Raising the surrounding fluid to a slightly alkaline pH prevented this acidification and almost completely shut down inflammasome activity without stopping lactic acid production itself.
Inside the Cell: A Chain Reaction to Inflammation
Diving deeper, the team found that lactic acid-driven acidification disrupts mitochondria, the cell's power stations, and increases reactive oxygen species, a type of chemical stress signal. At the same time, it activates a stress-sensing enzyme called PKR and promotes its physical interaction with the NLRP3 machinery. Both the mitochondrial stress and PKR activation turned out to be necessary for full inflammasome function. Blocking lactic acid production or making the environment more alkaline reduced these stress signals, weakened the PKR–NLRP3 partnership, and curbed the formation of the inflammasome complex. 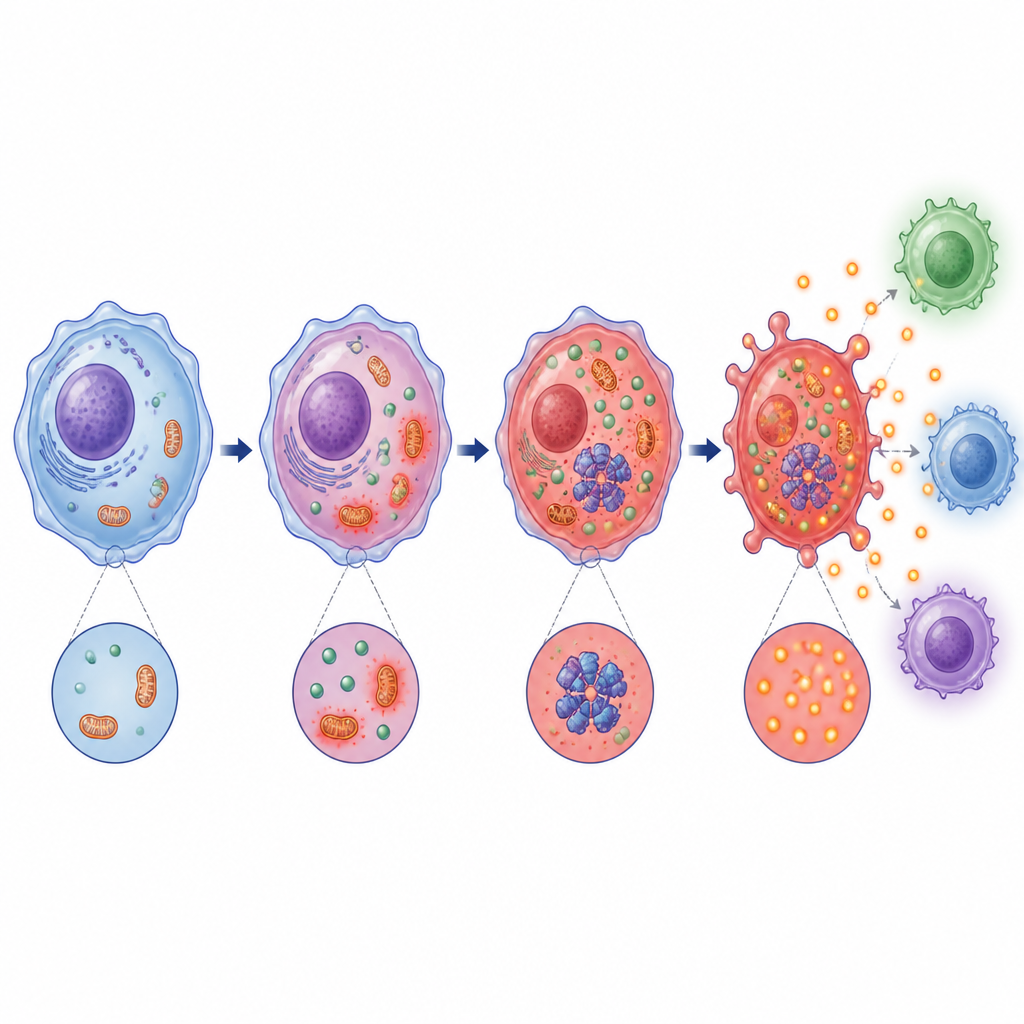
Lactic Acid as a Chemical “Scalpel”
Surprisingly, lactic acid also played a second, independent role. In cell extracts lacking intact inflammasome machinery, simply adding lactic acid was enough to cut the IL-1β and IL-18 precursors into mature-sized pieces that matched those produced by the usual enzyme. This chemical cutting required the acidic, undissociated form of lactic acid and depended on a specific site within IL-1β, the same site normally used by the enzyme. Other organic acids with similar chemical groups could do this to a lesser extent, while strong mineral acid alone was much less effective, suggesting that lactic acid's own structure helps drive this precise cleavage reaction under very acidic conditions.
What This Means for Sepsis and Other Diseases
To test these ideas in a living system, the researchers used a mouse model of polymicrobial sepsis, a severe, body-wide infection. Boosting blood lactate levels in septic mice increased IL-1β in the blood and belly cavity, drew more neutrophils to the infection site, lowered body temperature, and worsened survival. Treating the mice with a drug that blocks NLRP3 largely reversed these harmful effects, highlighting that the lactic acid surge feeds inflammation mainly through this pathway. Together, the findings suggest that lactic acid is a two-pronged driver of inflammation, both by reshaping cell metabolism to favor inflammasome activation and by directly processing key cytokines when acidity is extreme.
Why These Findings Matter
For a lay observer, the key message is that lactic acid is not just a harmless byproduct of exercise or illness. Inside stressed immune cells, it becomes a signal that says "turn up the fire," making inflammation stronger and harder to control. In conditions like sepsis, where both lactic acid and acidity rise, this can tip the balance from a helpful defense to dangerous, body-wide damage. By revealing how lactic acid pushes immune cells into this overactive state, and how it can directly shape inflammatory messengers, this work points toward new strategies to cool harmful inflammation by targeting cellular acid handling and the NLRP3 system.
Citation: Lin, HA., Lin, HC., Tsai, MH. et al. Lactic acid drives NLRP3 inflammasome activation and caspase-1–like cytokine cleavage via intracellular acidification. Cell Death Dis 17, 450 (2026). https://doi.org/10.1038/s41419-026-08708-y
Keywords: lactic acid, inflammasome, IL-1β, sepsis, immune metabolism