Clear Sky Science · en
Netrin-1 disrupt high-fat-diet-induced adipogenesis via the PPARγ and Wnt/β-catenin signaling pathways
Why this matters for everyday health
Obesity and type 2 diabetes are often blamed on “too much fat,” but the story is more subtle: how and where our bodies store extra calories can either protect us or push us toward disease. This study uncovers a surprising player in that story, a nerve-guiding protein called Netrin-1 that is also made by fat tissue. The researchers show that, under a high-fat diet, Netrin-1 can sabotage the body’s ability to remodel fat in a healthy way, worsening blood sugar control. Understanding this hidden brake on “good” fat expansion could open new doors for treating obesity-related diabetes.
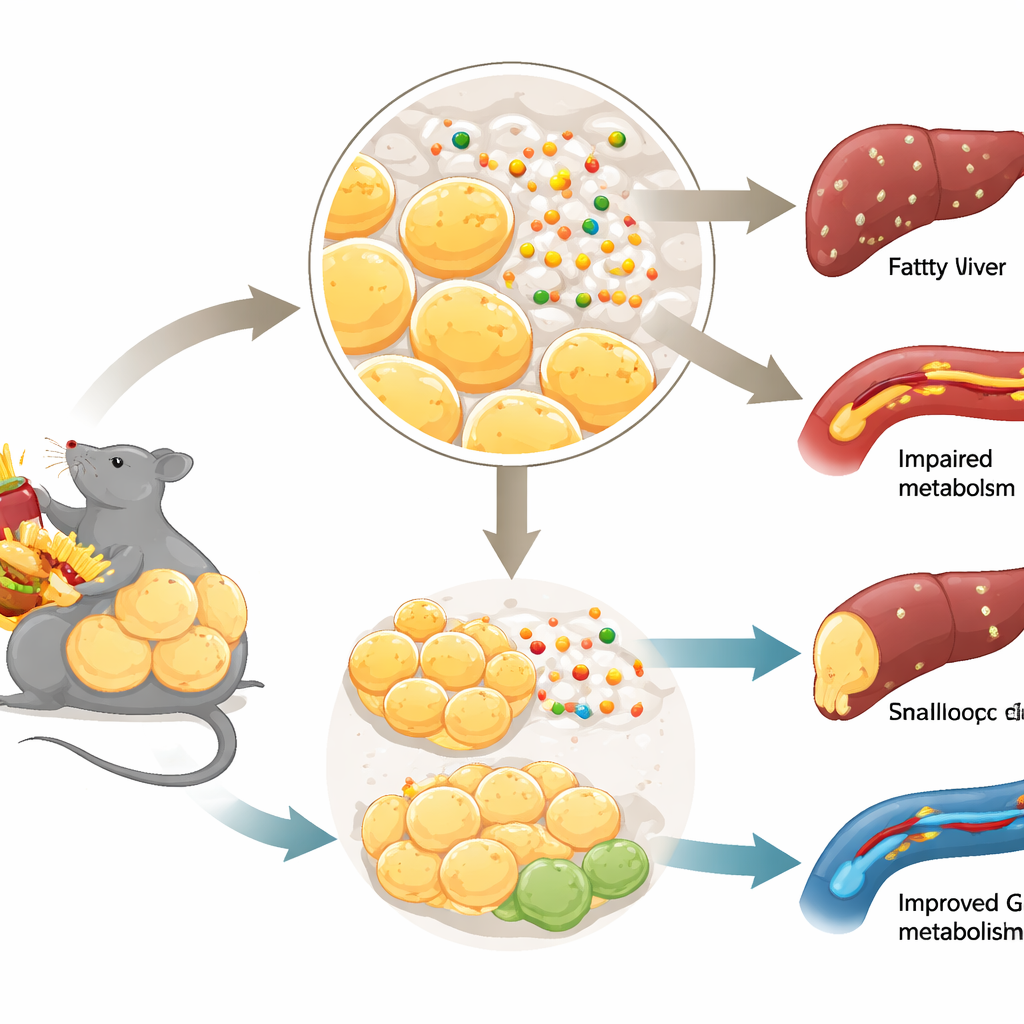
Good fat, bad fat, and sugar control
Not all body fat behaves the same. When excess calories are safely stored by creating many small fat cells—especially just under the skin—metabolism can remain surprisingly healthy. In contrast, when fat storage is blocked, fat cells become dysfunctional, and fat spills over into organs like the liver and muscles. This “bad” remodeling is linked to insulin resistance and type 2 diabetes. The team focused on how new fat cells are formed from precursor cells, a process called adipogenesis, and asked whether Netrin-1, long known for steering growing nerve fibers, might influence this process in fat tissue.
Turning off Netrin-1 makes high-fat diets less harmful
To test Netrin-1’s role, the researchers engineered mice that lack Netrin-1 specifically in fat tissue. When these animals were fed a high-fat diet for eight weeks, they actually gained more weight than normal mice—but their blood sugar control was better. They showed improved responses to insulin, lower fasting glucose, and reduced levels of circulating fats. Imaging and tissue measurements revealed that this extra weight was mostly due to expansion of subcutaneous white fat near the groin region, a depot often associated with metabolic protection. The enlarged fat mass was not caused by overstuffed cells, but rather by an increase in cell number and reduced scarring, both signs of healthier fat remodeling. Fat build-up in the liver was also diminished, suggesting that the expanded fat depot was safely storing excess lipids that might otherwise damage other organs.
Too much Netrin-1 pushes toward diabetes
The scientists then flipped the experiment and forced fat tissue to produce extra Netrin-1 using a gene-delivery virus. In both normal and high-fat-fed mice, this boosted Netrin-1 level did not strongly change body weight, but it did worsen glucose tolerance and raised blood fats. Fat depots tended to shrink relative to body size, while the liver showed more fat accumulation. Together with cell culture experiments, these findings indicate that Netrin-1 acts within fat tissue to blunt the formation of new, functional fat cells. When Netrin-1 is high, precursor cells divide less and are less able to mature into fat cells that efficiently store lipids and respond to insulin.
A molecular brake on building new fat cells
Digging deeper, the team showed that Netrin-1 dampens a master switch for fat cell development called PPARγ, while turning on a separate signaling route known as Wnt/β-catenin, which is known to oppose fat cell formation. In mouse and human datasets, Netrin-1 levels were higher in obesity and type 2 diabetes, and concentrated in precursor cells compared with mature fat cells. When Netrin-1 was artificially increased in precursor cells, they accumulated fewer fat droplets; activating PPARγ with a diabetes drug could largely rescue this effect, and blocking β-catenin also eased Netrin-1’s brake on fat cell maturation. Another layer of control came from low-oxygen stress inside overgrown fat depots: the hypoxia sensor HIF‑1α directly boosted Netrin-1 gene activity, linking high-fat-diet–induced oxygen shortage to this anti-adipogenic signal.
What this means for future treatments
In accessible terms, this work suggests that when we overeat, our fat tissue tries to grow new cells to park extra calories safely. But under a high-fat diet, local oxygen stress switches on Netrin-1, which then tells nearby precursor cells to stop becoming new fat cells. As a result, fat storage is pushed into less healthy patterns, blood sugar rises, and insulin works less effectively. By identifying Netrin-1 as a key messenger that links stressed fat tissue to poor metabolic health, the study points to a potential new therapeutic strategy: dialing down Netrin-1, or its downstream pathways, could help the body expand “good” fat depots and better buffer against type 2 diabetes, even when calorie intake is high.
Citation: Shi, H., Tang, J., Yan, X. et al. Netrin-1 disrupt high-fat-diet-induced adipogenesis via the PPARγ and Wnt/β-catenin signaling pathways. Commun Biol 9, 471 (2026). https://doi.org/10.1038/s42003-026-09749-x
Keywords: adipose tissue, Netrin-1, type 2 diabetes, high-fat diet, PPARγ signaling