Clear Sky Science · en
Central and peripheral analgesia in irradiated rats: reserpine-induced pain model
Why easing long‑lasting pain matters
Many people live with daily pain that standard painkillers only partly relieve and that often come with troubling side effects. This study explores an unusual helper: very low doses of gamma radiation, the same type of energy used at much higher levels to treat cancer. Using a rat model that mimics some features of chronic widespread pain, the researchers asked whether a single low radiation dose could safely reduce pain and what might be happening inside the body and brain when it does.
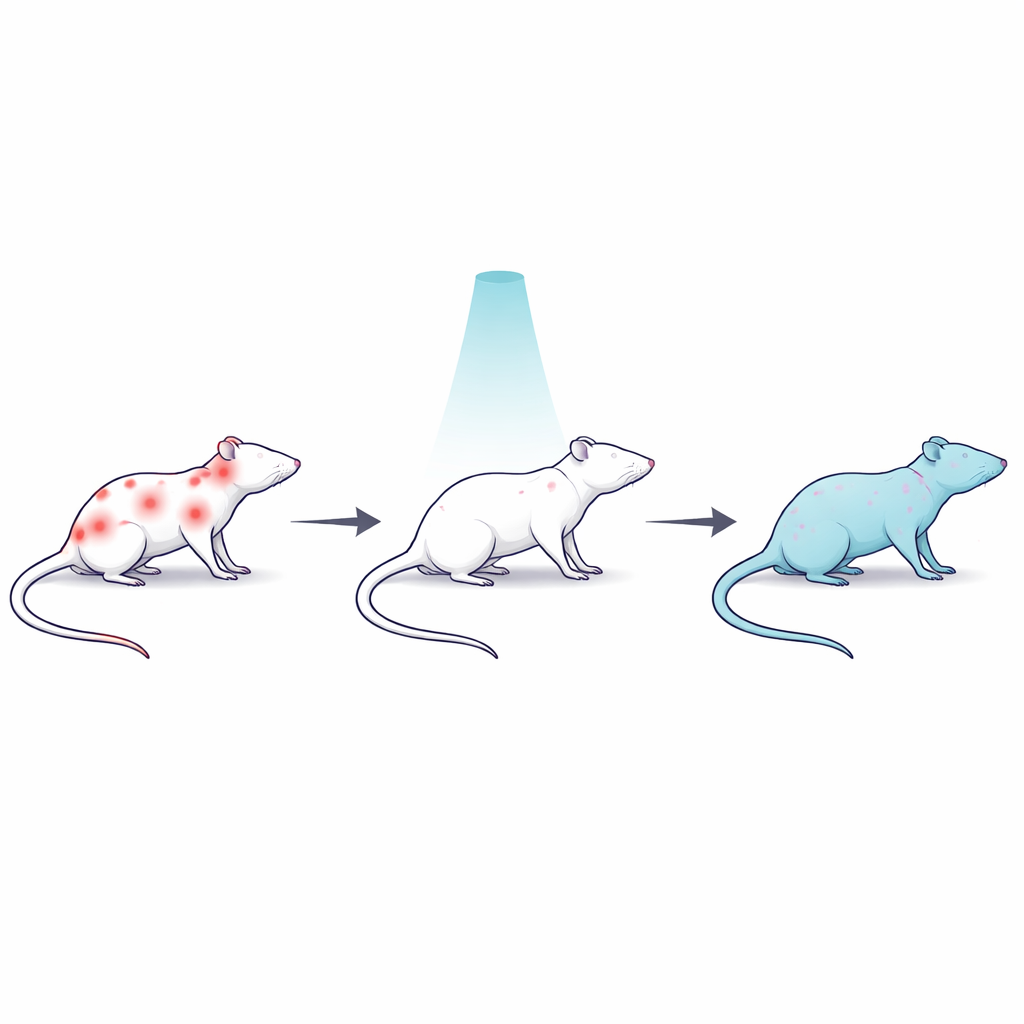
A rat model of stubborn, body‑wide pain
To study difficult‑to‑treat pain, the scientists used the drug reserpine, which drains key brain chemicals involved in mood and pain control and produces long‑lasting muscle and body pain in rats. Thirty male rats were divided into several groups: a healthy control group; a reserpine group with untreated pain; a reserpine group that received a single whole‑body low dose of gamma radiation; a similar irradiated group that also received naloxone, a drug that blocks opioid receptors in the brain; and a reserpine group treated with the common anti‑inflammatory painkiller diclofenac. This design allowed the team to compare radiation with a standard drug and to test whether the body’s own opioid‑like systems contributed to any pain relief.
Testing pain and probing the brain
The researchers measured pain in two ways. In the tail‑flick test, the rat’s tail is placed in warm water and the time until it flicks away reflects pain sensitivity in the nerves outside the brain and spinal cord. In Haffner’s tail‑clip test, a small clip is gently applied near the tail base, and the time before the rat reacts by turning to bite reflects pain processing in the spinal cord and brain. After these tests, the scientists collected blood and brain tissue to measure markers linked to pain and tissue stress: substance P and tumor necrosis factor‑alpha (both associated with pain and inflammation) in the blood, and nitric oxide and malondialdehyde (signals of oxidative, or “rust‑like,” stress) plus dopamine (a messenger involved in mood and pain control) in the brain.
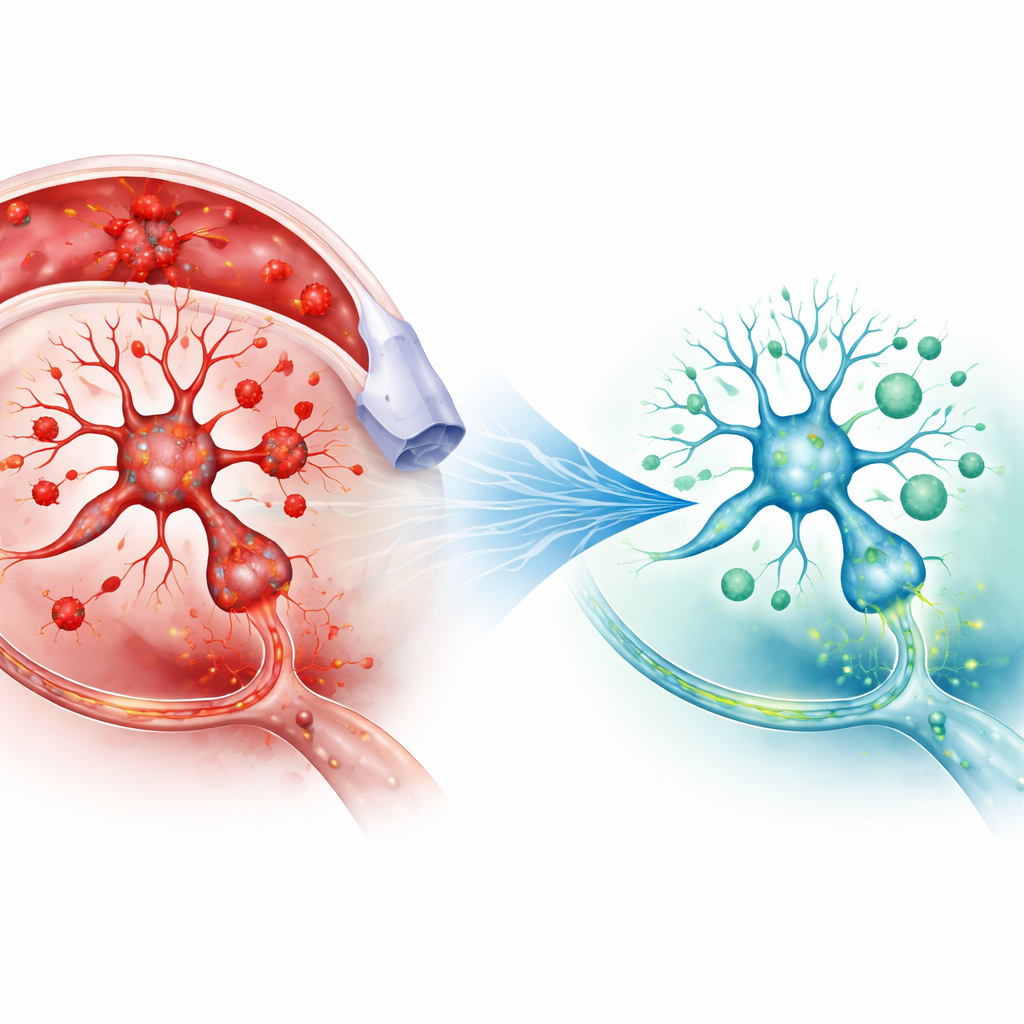
Radiation’s surprising pain‑relief pattern
Reserpine made the rats much more sensitive to pain in both tests and disturbed their internal chemistry: oxidative stress markers and inflammatory signals rose, while brain dopamine fell. A single low dose of gamma radiation reversed many of these changes. Pain responses in both tests were delayed, meaning the rats tolerated more discomfort before reacting. For pain carried by nerves in the tail, radiation’s effect was similar to that of diclofenac. For pain involving the brain and spinal cord, radiation again reduced sensitivity, but this benefit largely disappeared when naloxone was given first. That pattern suggests that low‑dose radiation triggers, at least in part, the body’s own opioid‑like pain‑dampening systems in addition to calming overactive nerves.
Less chemical “storm,” more balance
On the chemical level, radiation clearly softened the internal “storm” stirred up by reserpine. Levels of nitric oxide and malondialdehyde in the brain dropped toward normal, pointing to less oxidative stress. Brain dopamine content, which had been depressed by reserpine, rebounded after irradiation. In the bloodstream, the elevated inflammatory messenger tumor necrosis factor‑alpha and the pain‑linked neuropeptide substance P both fell after the low dose. Blocking opioid receptors with naloxone did not undo these antioxidant and anti‑inflammatory shifts, indicating that radiation’s chemical calming and its opioid‑related signaling effects are at least partly separate. Diclofenac also improved many of these measures, but unlike standard drugs, low‑dose radiation did so with a single exposure and without the known digestive and cardiovascular risks of long‑term anti‑inflammatory pills.
What this could mean for future pain care
In everyday terms, the study suggests that a carefully controlled, low dose of gamma radiation can make pain‑sensing nerves less jumpy, help restore protective brain chemicals, and quiet both oxidative and inflammatory signals that help drive chronic pain. The work was done in a single rat model with one radiation dose and only one short time point, so it cannot yet be directly translated to patients. Still, it supports clinical observations that low‑dose radiotherapy can ease stubborn joint and tendon pain, and it points to concrete biological pathways—antioxidant defenses, inflammation control, and opioid‑related nerve circuits—that future targeted therapies, whether based on radiation or drugs, might safely harness to help people living with chronic pain.
Citation: Saif-Elnasr, M. Central and peripheral analgesia in irradiated rats: reserpine-induced pain model. Sci Rep 16, 12193 (2026). https://doi.org/10.1038/s41598-026-44637-8
Keywords: chronic pain, low-dose radiation, oxidative stress, inflammation, opioid pathways