Clear Sky Science · en
The role and regulatory mechanism of USP25 in pancreatic microcirculatory disturbance in severe acute pancreatitis
Why tiny blood vessels in the pancreas matter
Severe acute pancreatitis is a sudden attack on the pancreas that can rapidly become life-threatening. In the worst cases, not only do digestive cells in the organ die, but the tiniest blood vessels that feed the pancreas also clog and collapse, starving the tissue of oxygen. This study asks a practical question with big implications: which molecular switches make these microvessels fail, and can turning one of them off protect the pancreas?
A closer look at a dangerous flare-up
The authors focused on a severe form of the disease called severe acute pancreatitis, in which patients often end up in intensive care and face high risk of organ failure. Earlier work had shown that a protein called USP25 is higher in people and animal models with pancreatitis, and that it can fan the flames of inflammation. At the same time, another protein, TRAF6, is known as a key hub that relays stress and danger signals inside immune and tissue cells. Because both molecules are involved in inflammatory damage, the team suspected that USP25 might be worsening blood flow problems in the pancreas by acting through TRAF6.
Animal models reveal a harmful partnership
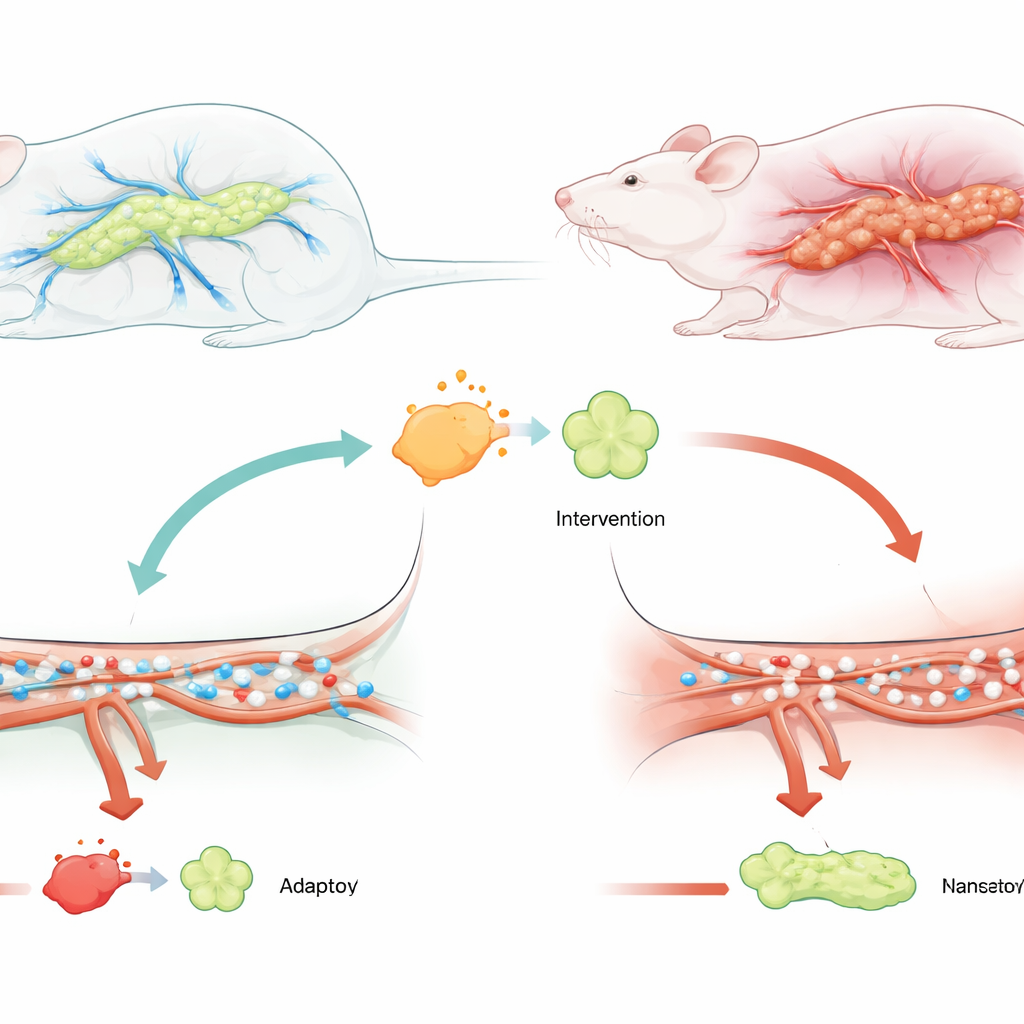
To test this idea, the researchers used rats in which severe pancreatitis was triggered by injecting a bile salt into the pancreatic duct, a widely used model of the disease. Some rats received a virus that lowered USP25 levels in the pancreas before the attack. Compared with untreated animals, rats with reduced USP25 had much lower blood markers of pancreatic injury, healthier-looking pancreatic tissue under the microscope, and far fewer signs of swelling, bleeding, and cell death. Importantly, measurements of microcirculation showed that red blood cells in treated rats flowed faster and through more tiny vessels, meaning that the worst blood flow blockages had eased.
How the molecular switch works inside cells
The team then zoomed in on individual pancreatic acinar cells, the enzyme-producing workhorses of the organ. In cultured rat acinar cells exposed to a pancreatitis-triggering compound, USP25 levels shot up, cell survival dropped, and more cells died. When USP25 was silenced, cells were more likely to live and released fewer inflammatory substances. Biochemical tests showed that USP25 physically binds to TRAF6 and shields it from being marked for destruction by the cell’s protein-recycling system. As a result, TRAF6 accumulates and keeps inflammation signaling switched on. When USP25 was blocked, TRAF6 became more heavily tagged for breakdown, its levels fell, and the harmful signaling quieted.
Proving TRAF6 is the key middleman
To be sure TRAF6 was the crucial go-between, the scientists artificially boosted TRAF6 levels even while USP25 was being blocked. In cells, this extra TRAF6 erased much of the protection conferred by USP25 inhibition: more cells died and inflammatory substances rose again. In rats, raising TRAF6 likewise undermined the benefits of lowering USP25. Microvessel blood flow worsened, chemical markers of vessel constriction and oxidative stress increased, and pancreatic tissue damage intensified. These rescue experiments support a simple chain of events: USP25 preserves TRAF6, TRAF6 drives inflammation, and that inflammation chokes off the pancreatic microcirculation.
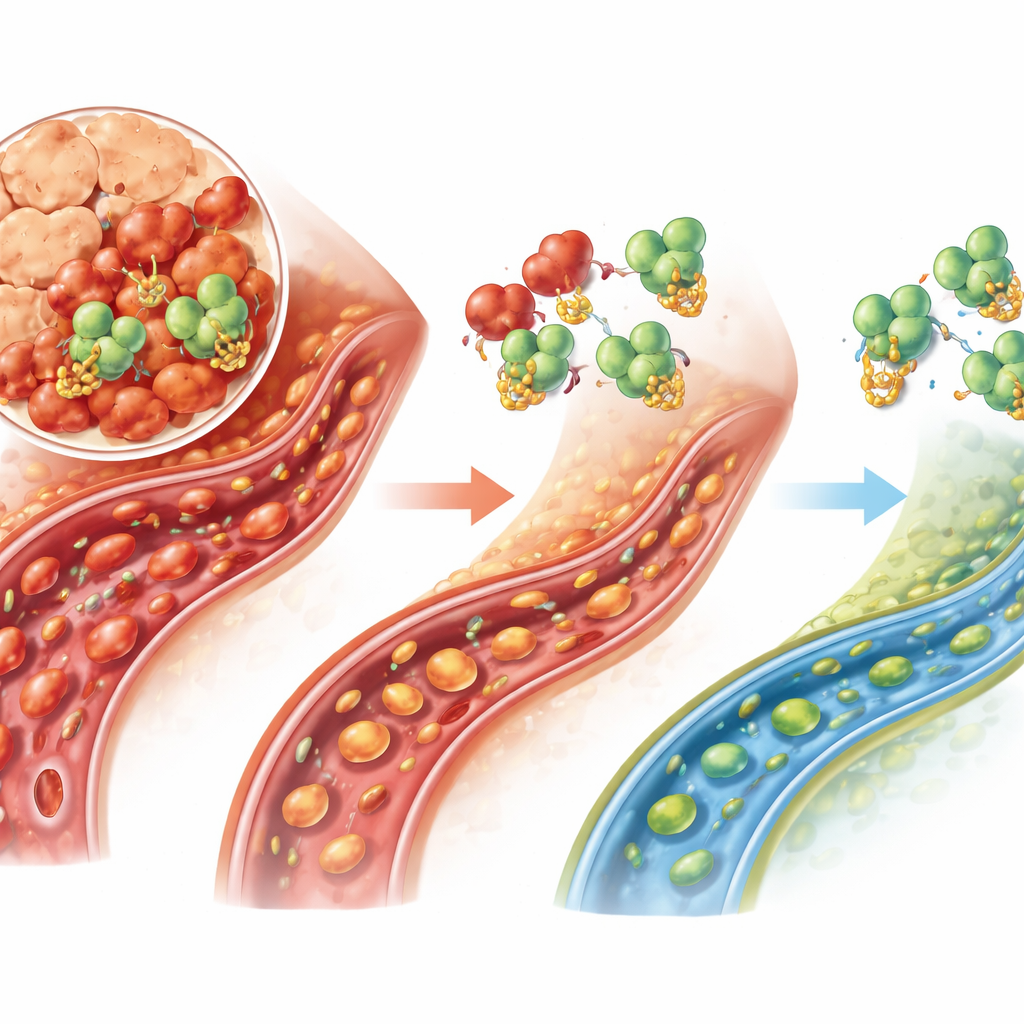
What this could mean for future treatments
For people facing severe acute pancreatitis today, care is mostly supportive—fluids, nutrition, and pain relief—because no drug directly halts the disease cascade. This study identifies a specific molecular axis, USP25 working through TRAF6, that appears to worsen tiny vessel failure and cell death in the pancreas. While the work is preclinical and based mainly on one animal model and a rat cell line, it points to USP25 as a promising target: blocking this enzyme could allow the body to dismantle TRAF6, dial down inflammation, and keep blood flowing through the pancreas when it is most at risk.
Citation: Zhang, Q., Zhang, X. & Shan, F. The role and regulatory mechanism of USP25 in pancreatic microcirculatory disturbance in severe acute pancreatitis. Sci Rep 16, 11570 (2026). https://doi.org/10.1038/s41598-026-39295-9
Keywords: severe acute pancreatitis, pancreatic microcirculation, USP25, TRAF6, inflammation