Clear Sky Science · en
Harnessing the immune microenvironment: advances in nasopharyngeal carcinoma immunotherapy
Why this matters for everyday health
Nasopharyngeal carcinoma is a throat cancer that is unusually common in certain parts of Asia and is closely linked to a widespread virus called Epstein–Barr virus. Many patients are diagnosed only after the disease has spread, and standard chemo and radiation do not help everyone. This article explains how scientists are learning to turn the body’s own immune system back on against this cancer, using new drugs, smart combinations of treatments, and better tests to match the right therapy to the right person.
A cancer shaped by a common virus
Nasopharyngeal carcinoma grows in a hard-to-see area behind the nose, so early symptoms are often missed. Almost all tumors of this type carry hidden Epstein–Barr virus, which quietly rewires infected cells. The virus makes tumor cells display signals that shut down attacking immune cells, hide key ID tags used for immune recognition, and call in other cells that dampen immune responses. Under the microscope, these tumors are packed with immune cells, yet many of those cells are exhausted or blocked. This strange mix of heavy immune presence and strong immune paralysis makes the disease both a challenge and an ideal test bed for new immune-based treatments.
Turning immune brakes into treatment targets
The most dramatic progress has come from drugs called immune checkpoint inhibitors, which release molecular “brakes” on T cells, the body’s main cancer-killing soldiers. In large clinical trials, medicines that block the PD-1/PD-L1 pathway, when added to standard chemotherapy, have extended survival and become the new first-line treatment for people with recurrent or metastatic disease. Similar drugs are now being moved earlier in the course of illness, combined with chemotherapy and precise radiotherapy for patients whose tumors are still confined to the head and neck region but are at high risk. Early results show higher complete response rates and longer periods without relapse, suggesting that resetting the immune system before or during radiation can deepen and stabilize control of the cancer. 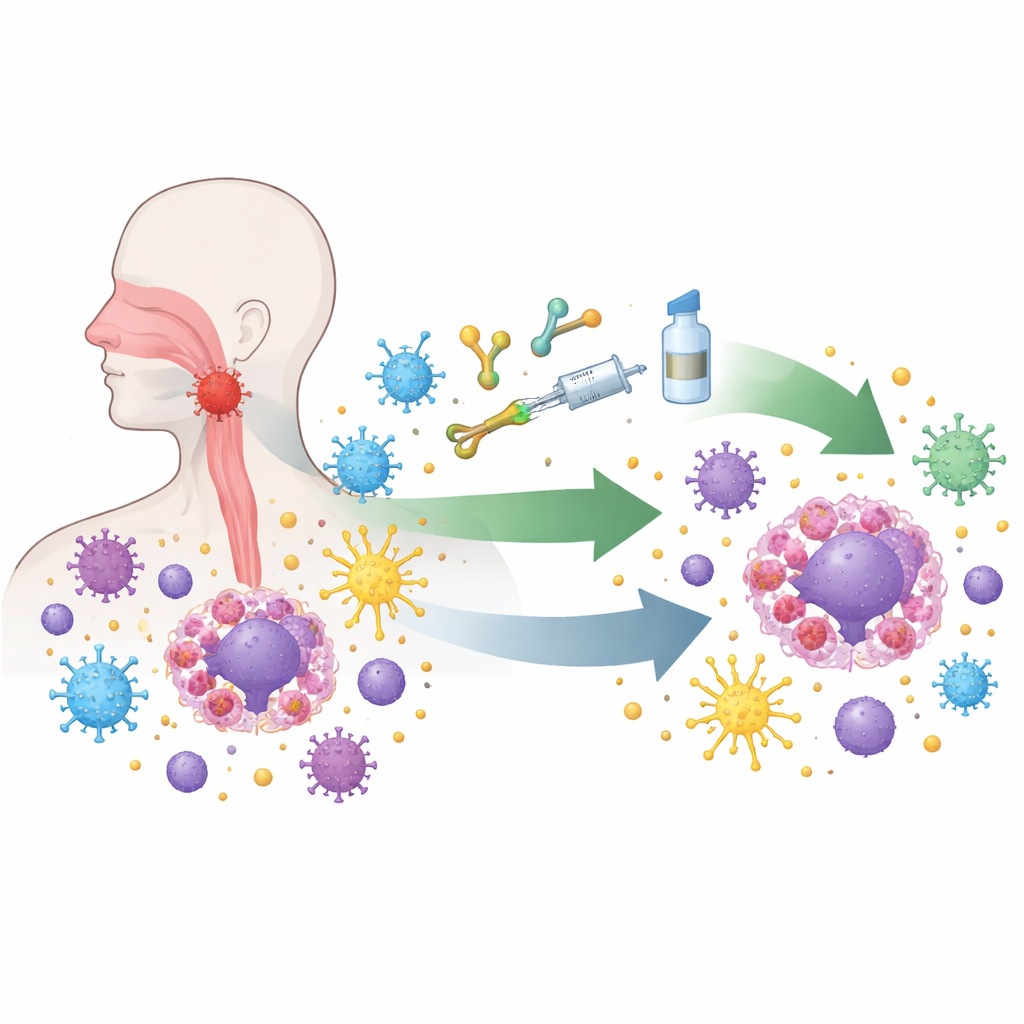
Combining forces for stronger responses
Because the virus and the tumor microenvironment use many overlapping tricks to suppress immunity, single drugs rarely solve the problem. Researchers are testing bispecific antibodies that hit two checkpoints at once, as well as combinations of immunotherapy with drugs that target blood vessel growth, reshape the tumor’s supporting tissue, or modulate metabolism. Radiotherapy itself can act like an in-situ vaccine by causing cancer cells to die in a way that alerts immune cells; adding checkpoint blockers can amplify this effect, especially in patients with a limited number of metastases. For selected patients, surgery followed by immunotherapy or extended maintenance immune treatment after initial chemo–immunotherapy can keep disease in check for years, though side effects and quality of life need careful monitoring.
Next-generation vaccines, cell therapies, and smart diagnostics
Because Epstein–Barr virus is so central to this cancer, scientists are designing vaccines and cell therapies that specifically recognize viral components. Experimental messenger RNA vaccines encoding trimmed-down viral proteins, often combined with natural killer cells or engineered T cells, have produced strong anti-tumor effects in animal models, though early large human trials have highlighted how difficult it is to translate these gains into routine care. In parallel, a wave of new biomarkers aims to guide decisions more precisely. Blood tests that track fragments of viral DNA, proteins carried in tiny vesicles, or simple inflammation and cholesterol markers can help estimate risk and follow treatment response. Advanced imaging analysis and artificial intelligence applied to routine scans and tissue slides can map the immune landscape of each tumor, predicting who is most likely to benefit from particular immunotherapies and who may need more aggressive combinations. 
Facing resistance and personalizing care
Despite these advances, many tumors either never respond to immunotherapy or find ways to escape after an initial response, often driven by the virus’s continued influence on the tumor’s habitat. The authors argue that the next leap forward will come from understanding this evolving ecosystem at single-cell and spatial resolution and using that knowledge to design cleaner combinations that hit multiple weak points without overwhelming the patient with side effects. They envision tailored treatment pathways in which viral load, immune cell patterns, imaging features, and simple blood markers are integrated by artificial intelligence to choose and adjust therapy over time. For patients and clinicians, the key takeaway is that nasopharyngeal carcinoma is shifting from a cancer dominated by chemotherapy and radiation to one where harnessing and guiding the immune system—while outsmarting a clever virus—offers a path to longer, better lives.
Citation: Zhu, Y., Liu, Y., Yin, Z. et al. Harnessing the immune microenvironment: advances in nasopharyngeal carcinoma immunotherapy. Cell Death Discov. 12, 144 (2026). https://doi.org/10.1038/s41420-026-02999-y
Keywords: nasopharyngeal carcinoma, Epstein–Barr virus, cancer immunotherapy, immune checkpoint inhibitors, tumor microenvironment