Clear Sky Science · en
Lipid homeostasis plays a critical role in inherited and acquired retinal diseases
Why Fats in the Eye Matter
The light-sensing cells at the back of the eye are some of the most energy-hungry cells in the body, constantly rebuilding their outer surface so we can see clearly. To do this, they need a steady, well-controlled supply of fats and related molecules. This review article explains how that “fat economy” of the retina normally works, what happens when it goes off balance, and how this breakdown contributes to common blinding diseases such as retinitis pigmentosa, diabetic retinopathy, and age-related macular degeneration. It also explores emerging treatments that aim to protect sight by restoring healthy lipid balance.
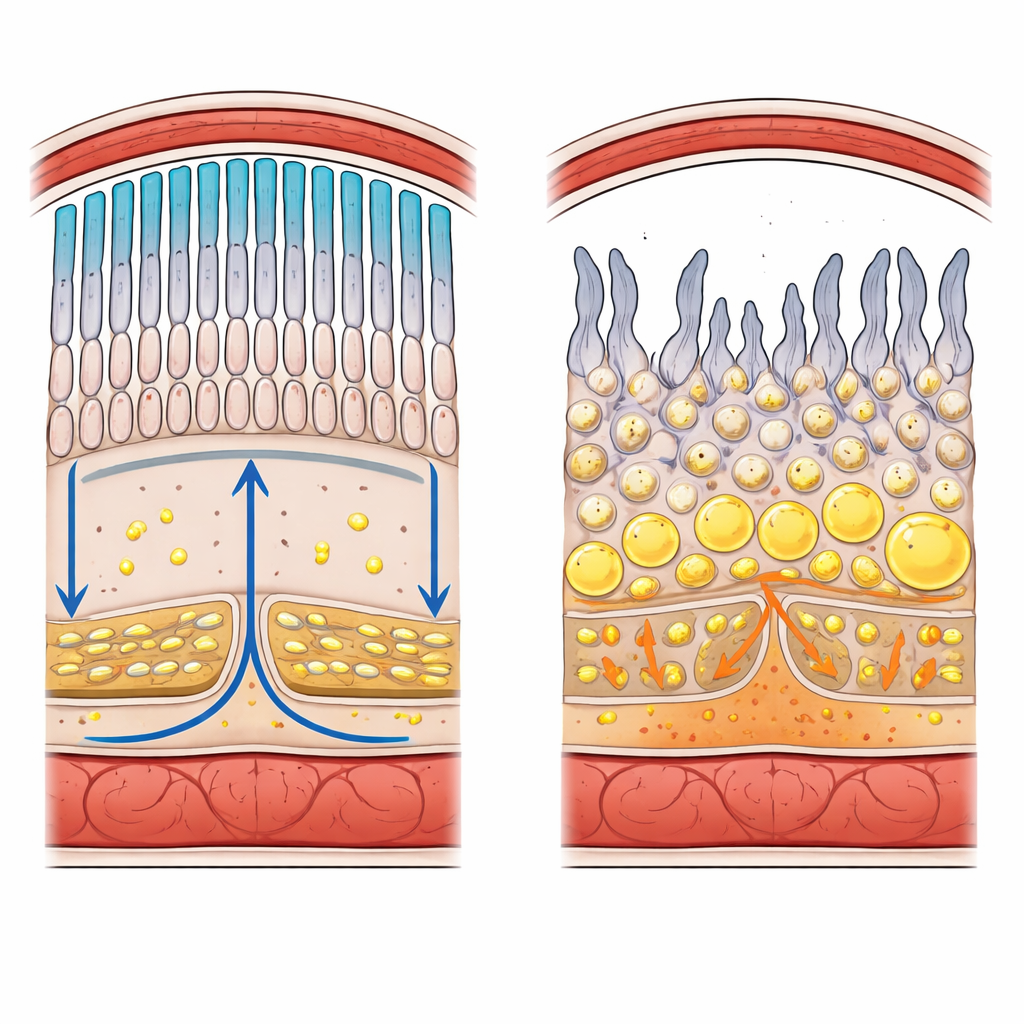
How the Back of the Eye Is Built
The retina is a layered sheet of nerve cells that turns light into electrical signals for the brain. At its outer edge sit rods and cones, the photoreceptors that detect dim light and color. Just beneath them lies a single layer of support cells called the retinal pigment epithelium (RPE), resting on a thin barrier membrane and a bed of blood vessels. Tight junctions between cells form a blood–retina barrier that carefully controls which substances, including lipids, can move from the circulation into the light-sensitive tissue. Photoreceptors shed about 10% of their membrane each day and rebuild it, creating an enormous demand for fresh phospholipids, cholesterol, and special omega-3 fats.
Recycling Light into Vision
Every time a photon hits the eye, a vitamin A–based molecule in photoreceptors changes shape, triggering the visual signal. To keep vision going, this molecule must be recycled in a loop known as the visual cycle. After activation, it travels from the photoreceptor to the RPE, where enzymes convert it back into its light-sensitive form. Along the way, it is temporarily stored in tiny fat-filled droplets called retinosomes. These droplets act as safe warehouses for vitamin A esters and other neutral lipids, preventing toxic byproducts from building up. Specialized proteins help build, grow, and break down these droplets so that the right amount of visual pigment is always available.
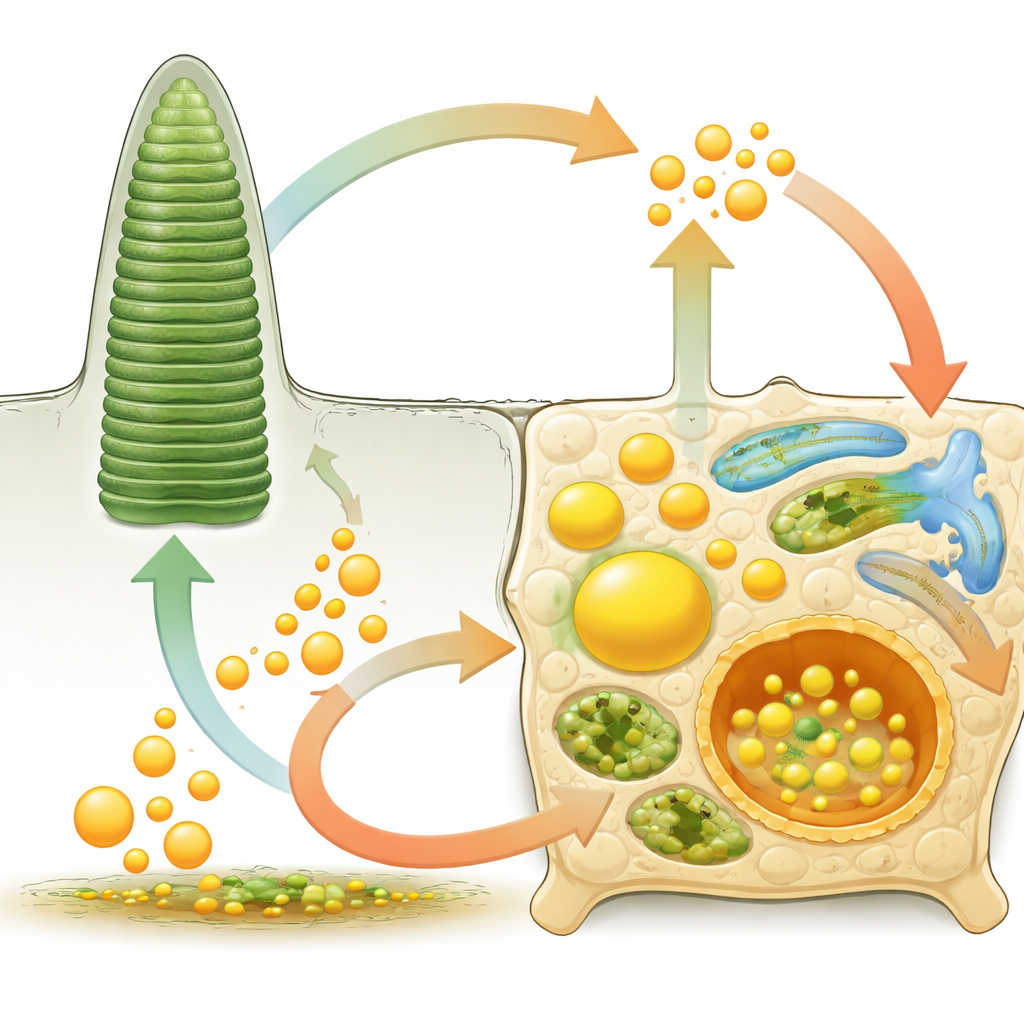
Balancing Lipid Traffic Between Support Cells and Sensors
The RPE is a busy logistics hub for fats. From the blood side, it pulls in lipoprotein particles that carry cholesterol and other lipids and channels them into storage droplets or sends them on toward the photoreceptors. From the retinal side, it eats the discarded tips of photoreceptor outer segments, digests their membranes, and recycles the component lipids. A network of membrane transporters and receptors governs this two-way traffic, including proteins that import dietary fats such as the omega‑3 docosahexaenoic acid (DHA) and others that pump cholesterol out. When these systems fail—because of inherited gene mutations or acquired metabolic stress—lipids can pile up in the wrong places, trigger inflammation and oxidative damage, and gradually kill retinal cells.
When Lipid Control Fails: From Rare Syndromes to Common Blindness
Many retinal diseases trace back, at least in part, to disturbed lipid handling. In Stargardt disease, a faulty transporter in photoreceptors cannot clear a toxic vitamin A byproduct, leading to buildup of lipofuscin, a harmful fatty pigment in RPE cells, and loss of central vision. Mutations in lipid-processing enzymes or peroxisomes disrupt very long–chain fatty acids and can cause early-onset degeneration. In retinitis pigmentosa, changes in genes for visual pigments, lipoprotein assembly, or omega‑3 metabolism leave photoreceptors structurally fragile and short on key fatty acids like DHA. In diabetic retinopathy and age-related macular degeneration, chronic high blood sugar, cholesterol imbalance, and inflammatory lipids contribute to leaky or abnormal blood vessels, thickened support membranes, and fatty deposits under the RPE known as drusen.
New Ways to Protect Sight Through Lipids
Because lipid imbalance threads through so many eye diseases, it has become a promising therapeutic target. Drugs that activate nuclear receptors such as PPARα and liver X receptor can boost cholesterol efflux, tame inflammation, and limit harmful vessel growth in diabetic and age-related disease models. Fenofibrate, a triglyceride-lowering medicine, has already been shown in large trials to slow diabetic retinopathy. Other approaches aim to normalize toxic sphingolipids like ceramides, supplement protective omega‑3 and very long–chain fatty acids, or use statins and related agents to fine-tune cholesterol handling. In parallel, stem cell–derived RPE sheets and retinal tissue are being tested to replace cells already lost. Together, these strategies suggest that maintaining or restoring healthy lipid homeostasis could preserve vision across a wide spectrum of inherited and acquired retinal disorders.
What This Means for Patients and Prevention
Seen from a distance, the message of this review is straightforward: the retina’s ability to see depends on a delicate balance of fats. When that balance is disrupted—by genes, aging, diabetes, or poor systemic lipid control—the eye slowly loses its capacity to renew and protect its light-sensing cells. By understanding the key pathways that move, store, and detoxify lipids in the retina, researchers are uncovering new ways to predict risk, intervene earlier, and design therapies that support the eye’s natural housekeeping systems. For patients, this points not only to future gene and cell therapies, but also to practical measures today—such as managing blood sugar and cholesterol, and consuming protective fatty acids—that may help keep their retinas healthier for longer.
Citation: Bhattacharyya, A., Choudhary, V. Lipid homeostasis plays a critical role in inherited and acquired retinal diseases. Commun Biol 9, 536 (2026). https://doi.org/10.1038/s42003-026-10025-1
Keywords: retinal lipids, age-related macular degeneration, diabetic retinopathy, retinitis pigmentosa, omega-3 fatty acids