Clear Sky Science · en
Effectiveness of platelet-rich plasma therapy in promoting wound healing and shoulder function recovery after shoulder surgery
Why this matters for everyday shoulders
Shoulder surgery is often the last resort for people whose pain and stiffness keep them from simple daily tasks like combing their hair or reaching a shelf. But even when surgery goes well, recovery can be slow and uncomfortable. This study asks a practical question that many patients and surgeons care about: can using a small portion of a patient’s own blood, called platelet-rich plasma, help shoulder wounds heal faster, ease pain, and get people moving sooner?
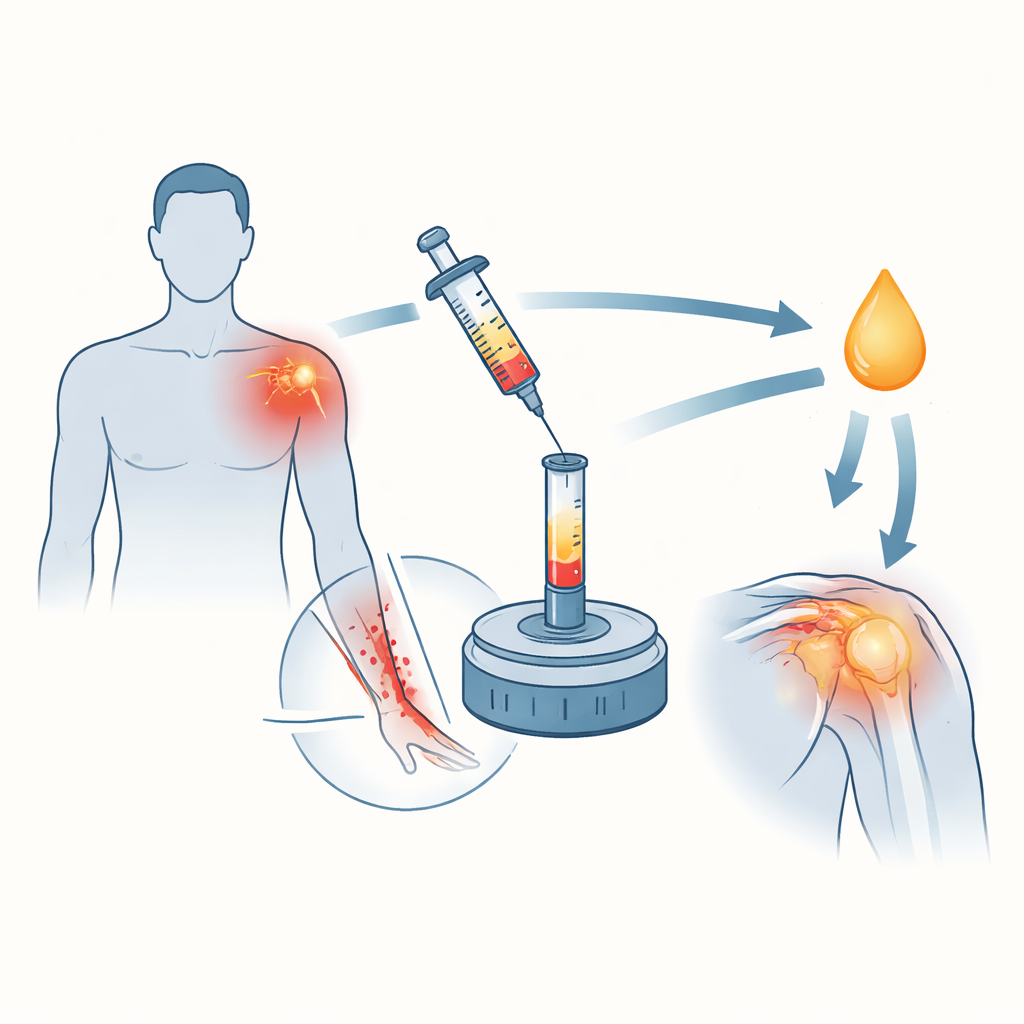
A boost from your own blood
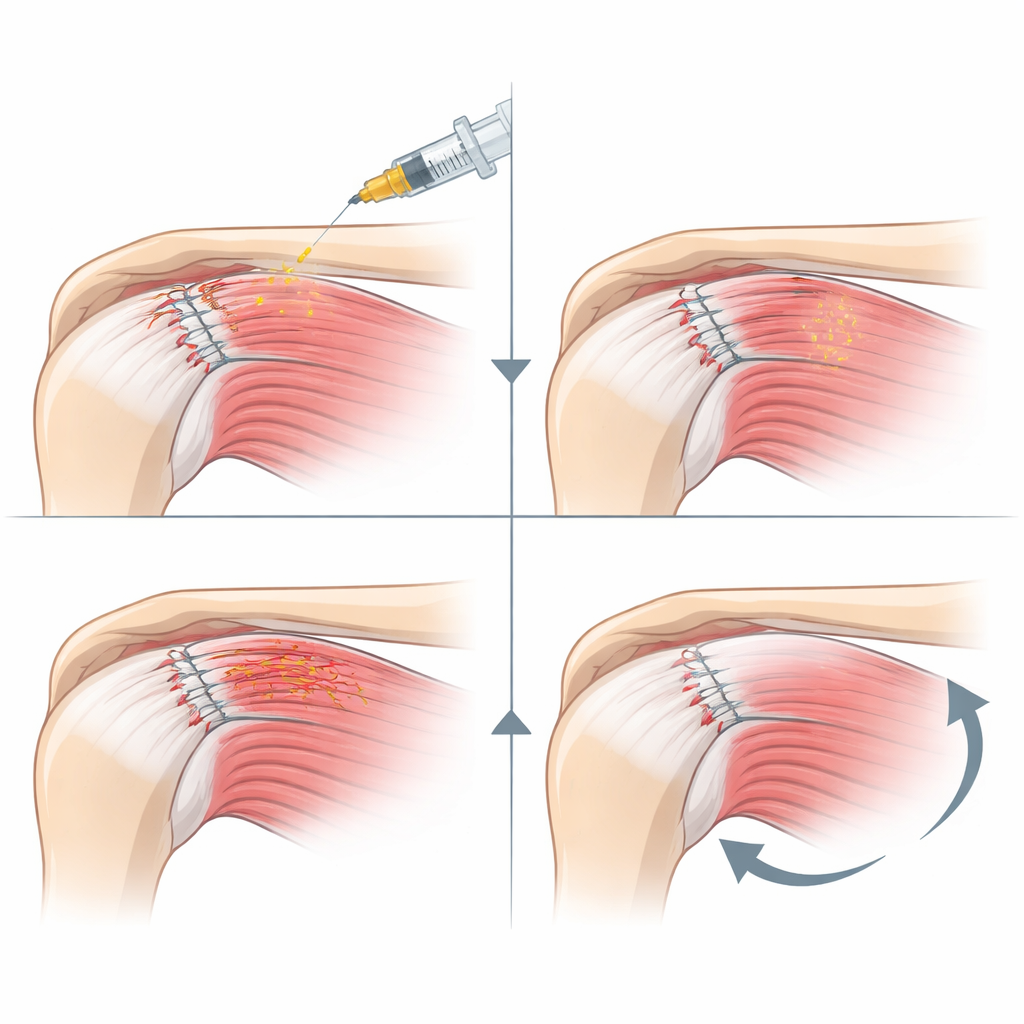
Platelet-rich plasma (PRP) is made from a sample of the patient’s blood spun in a centrifuge so that platelets and helpful growth factors become concentrated. These natural ingredients are known to encourage tissue repair, new blood vessel growth, and the rebuilding of collagen, a major component of tendons and skin. In this hospital in Changsha, China, surgeons began placing a small volume of PRP around the surgical cut and repaired tissues at the end of several types of shoulder operations. The idea was simple: deliver the body’s own healing tools exactly where they are needed, right when the injury from surgery is fresh.
How the study was set up
Because the researchers were working with existing patient records from 2018 to 2023, they could not randomly assign people to PRP or no PRP. Instead, they carefully matched each person who received PRP with a similar person who did not, based on age, sex, other health problems, and how much pain they had before surgery. They focused on three common procedures: rotator cuff repair (100 patients), shoulder replacement (40 patients), and subacromial decompression, an arthroscopic surgery to relieve impingement (30 patients). Altogether, 170 patients formed matched pairs, which helped make the comparison between the PRP group and the standard-care group fairer.
Faster wound closure and less pain
Across all three kinds of surgery, wounds in patients who received PRP closed several days sooner than in those who did not. The biggest difference appeared after rotator cuff repair: on average, PRP-treated wounds were judged healed in about four and a half days, compared with nearly seven days without PRP. Patients who received PRP also reported less pain six months after surgery, using a standard scale where higher numbers mean more pain. For example, after rotator cuff repair, average pain scores fell to under 2 out of 10 in the PRP group but remained above 3 in the comparison group. Shoulder replacement and decompression patients also experienced modest but consistent pain reductions with PRP.
Better movement, fewer days in the hospital
The study tracked shoulder function using a widely used score that combines pain, strength, and range of motion. In every type of surgery, patients who received PRP had higher scores over time, suggesting smoother recovery. Again, the clearest edge appeared in the rotator cuff group, where PRP patients gained several more points on this scale by six months than those without PRP. Hospital stays told a similar story: people treated with PRP went home earlier, often several days sooner, which may reflect quicker wound healing, better comfort, or both. Complication rates were low in all groups, with a hint of fewer problems after rotator cuff repair when PRP was used, and overall patient satisfaction was higher among those who received PRP.
Caution and next steps
For patients wondering whether PRP is a magic bullet, the message is more measured. This research suggests that adding PRP at the end of shoulder surgery is linked with faster wound healing, less lingering pain, and slightly better shoulder function, especially in operations that disturb more tissue, such as rotator cuff repair and shoulder replacement. However, the study was retrospective and from a single hospital, so hidden differences between groups and variations in how PRP was prepared could still influence the results. Larger, carefully randomized trials with standardized PRP methods are needed to confirm how big these benefits truly are and which patients are most likely to gain from this promising, blood-based boost to healing.
Citation: Hu, Z., Wei, L., Hu, W. et al. Effectiveness of platelet-rich plasma therapy in promoting wound healing and shoulder function recovery after shoulder surgery. Sci Rep 16, 10894 (2026). https://doi.org/10.1038/s41598-026-44844-3
Keywords: platelet-rich plasma, shoulder surgery, wound healing, rotator cuff repair, postoperative pain