Clear Sky Science · en
2’-5’ Oligoadenylate Synthetase-Like 1- (OASL1-) deficient mice promote antiviral protection against pseudorabies virus infection associated with enhanced production of type I interferon
Why this matters for people and animals
Pseudorabies virus may sound like a curiosity of farm life, but it is a major killer of piglets, a threat to the global pork industry, and an occasional cause of severe brain infections in people. This study uncovers how one of the body’s own "brake" proteins, called OASL1, can actually make this virus more dangerous by dampening early antiviral defenses. By removing this brake in mice, the authors show it is possible to dramatically improve survival, reduce brain damage, and lower viral levels, offering clues for better treatments and vaccines against pseudorabies virus and related herpesviruses.
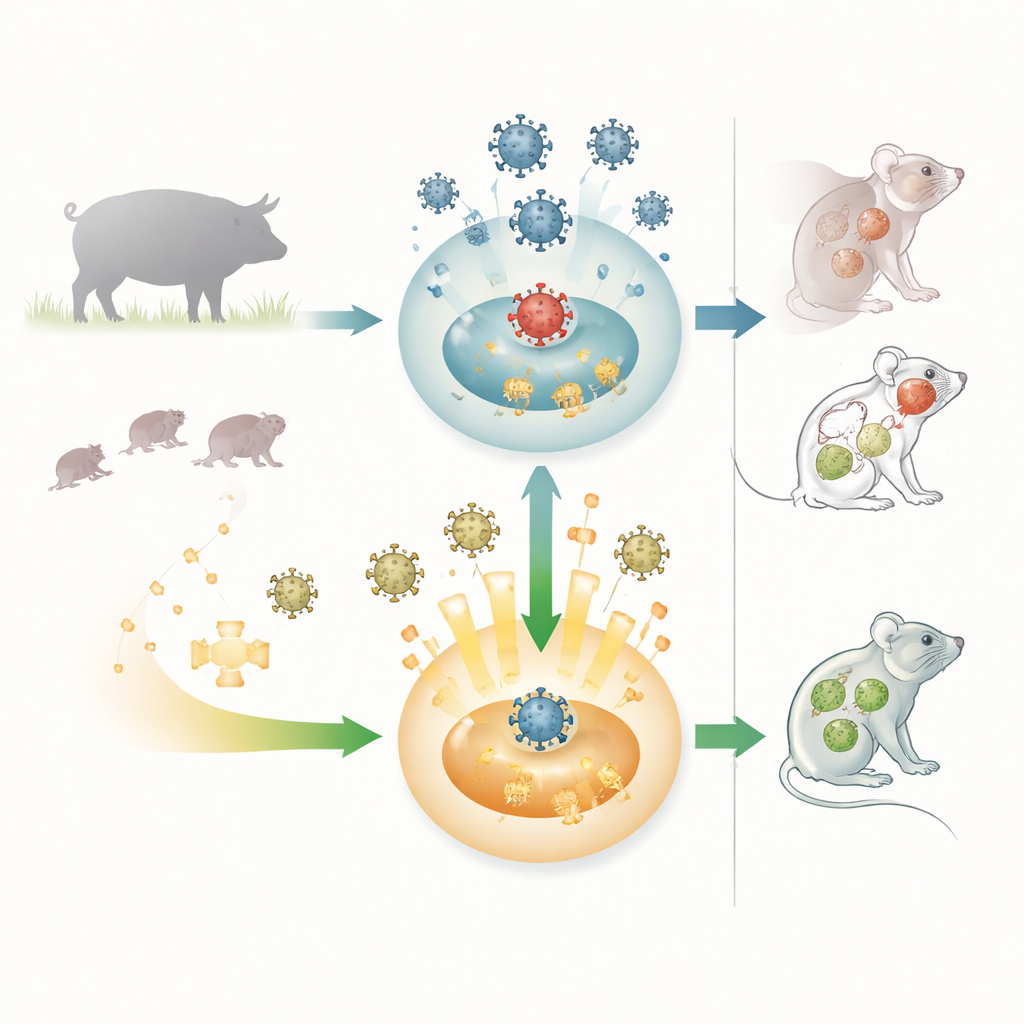
A tough virus with wide reach
Pseudorabies virus is a herpesvirus whose natural home is pigs, where it can cause breathing problems, reproductive failure, and almost certain death in newborn piglets. The virus can also infect many other mammals, including farm animals, pets, and laboratory mice, and nearly all of these accidental hosts die. Recent reports of human brain infections linked to pseudorabies virus variants have raised concern that this animal pathogen may occasionally spill over into people. Because of this broad host range and severe disease, researchers are keen to understand how the body’s first line of defense, the innate immune system, fights this virus—and how the virus pushes back.
The body’s alarm system and a built-in brake
When a DNA virus like pseudorabies enters cells, specialized sensors detect viral genetic material and trigger production of type I interferons, a family of powerful antiviral alarm molecules. These interferons switch on hundreds of defensive genes. Among them is OASL1, a protein that does not directly destroy viruses but instead fine‑tunes the response. Earlier work showed that OASL1 can hold back production of IRF7, a key control switch for interferon production, forming a negative feedback loop that prevents the alarm system from staying on too long. The central question of this study was what happens during pseudorabies infection if this brake, OASL1, is removed.
Removing the brake protects mice
The researchers compared normal mice with mice genetically engineered to lack OASL1. Both groups were given a dose of pseudorabies virus that is usually lethal. All normal mice developed intense itching, skin wounds, seizures, and paralysis, and every one of them died. In striking contrast, most OASL1‑deficient mice survived and maintained body weight with far milder symptoms. When the team measured virus levels in the spleen, lungs, and brain, they found that mice without OASL1 had far lower viral loads. Blood tests showed that these mice produced higher amounts of type I interferons early in infection, suggesting that a stronger, faster alarm response helped control the virus before it could spread widely.
Less runaway inflammation, less organ damage
Severe viral infections can trigger a "cytokine storm," an overwhelming inflammatory reaction that damages organs. The scientists measured several key inflammatory molecules in tissues and blood. Normal mice infected with pseudorabies virus showed high levels of these factors in the spleen, lungs, and brain, along with heavy inflammatory cell infiltration. By contrast, OASL1‑deficient mice had much lower levels of these inflammatory signals. Under the microscope, their spleens retained immune cells instead of losing them to cell death, their lungs had milder inflammatory changes, and their brains showed far less nerve cell degeneration in the hippocampus, a region critical for memory. Thus, removing OASL1 not only helped clear the virus but also prevented excessive inflammation and tissue injury.
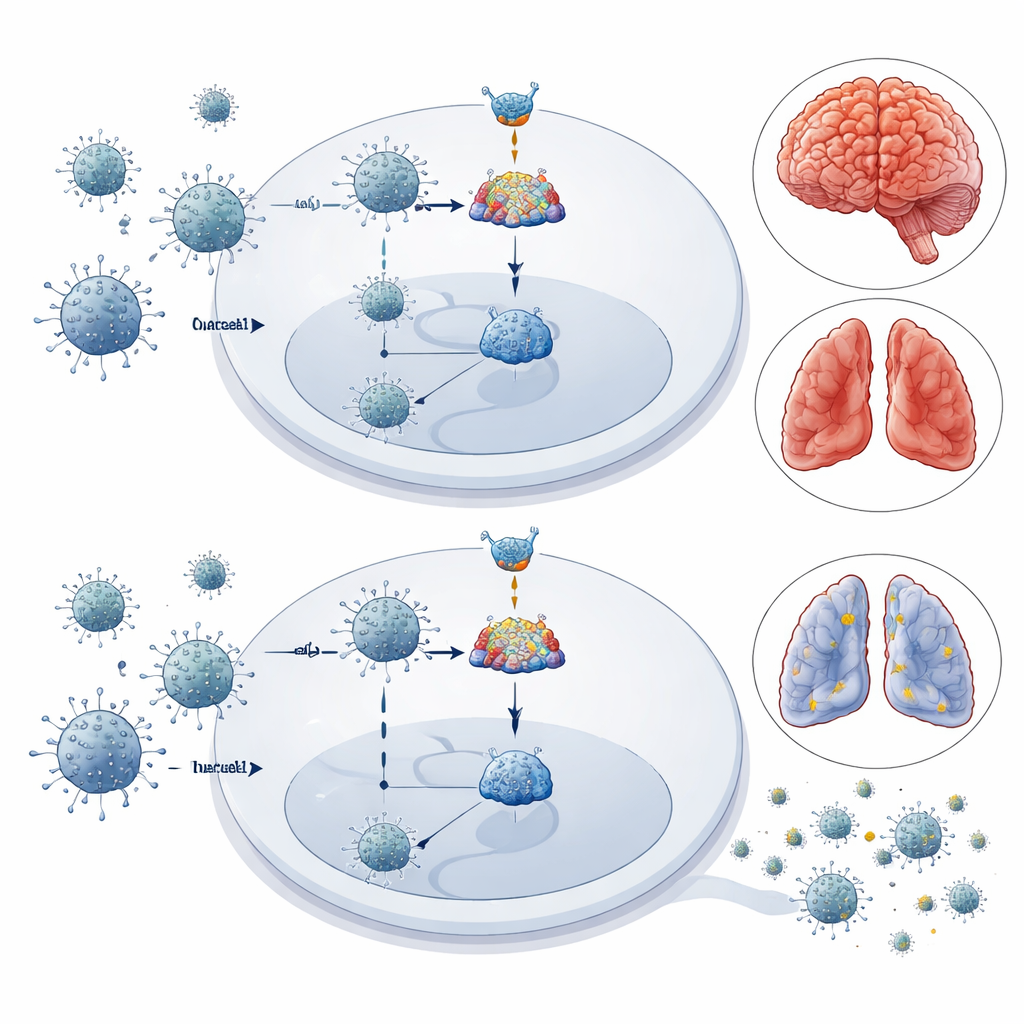
Zooming in on the key control switch
To understand how OASL1 shapes this response, the team examined IRF7, the control switch that drives interferon production. In mice lacking OASL1, IRF7 levels were consistently higher in the spleen, lungs, brain, and in cultured immune cells such as macrophages and microglia after infection, while a related factor, IRF3, changed little. These cells secreted more type I interferons and supported less viral replication. When the researchers used small interfering RNA to specifically knock down IRF7 in OASL1‑deficient macrophages, the boosted interferon response disappeared and virus levels rebounded. This experiment showed that the protective effect of losing OASL1 depends mainly on freeing IRF7 to fully activate the antiviral program.
What this means going forward
In everyday terms, OASL1 acts like an internal safety brake that keeps the antiviral alarm from blaring too long. During pseudorabies virus infection, that brake engages too early and too strongly, giving the virus room to multiply and contributing to severe disease. Mice that lack OASL1, or whose OASL1 is temporarily silenced in key immune cells, mount a brisk, IRF7‑driven interferon response that clears virus more effectively while avoiding a damaging cytokine storm. These findings suggest that carefully timed drugs that loosen this brake—only during the critical early window of infection—might help protect pigs and possibly humans from pseudorabies and related herpesviruses. Any such therapy would need to be finely tuned, however, to avoid swinging from too little immune response to too much.
Citation: Bao, T.H.T.N., Leya, M., Van, T.P. et al. 2’-5’ Oligoadenylate Synthetase-Like 1- (OASL1-) deficient mice promote antiviral protection against pseudorabies virus infection associated with enhanced production of type I interferon. Sci Rep 16, 13205 (2026). https://doi.org/10.1038/s41598-026-43144-0
Keywords: pseudorabies virus, innate immunity, type I interferon, OASL1, IRF7