Clear Sky Science · en
IL-8 contributes to postoperative adhesion formation through the crosstalk of neutrophils and mesothelial cells
Why scar bands after surgery matter
Many people who undergo abdominal surgery later develop internal scar bands, called adhesions, that can twist the bowel, cause chronic pain, or interfere with fertility. Despite their impact, doctors have few reliable ways to prevent these sticky strands from forming. This study explores a powerful immune signal called IL-8 and shows how it drives the early chain of events that leads from a clean surgical cut to tough internal scar tissue—and how blocking IL-8 with an antibody can markedly reduce these adhesions in a primate model.
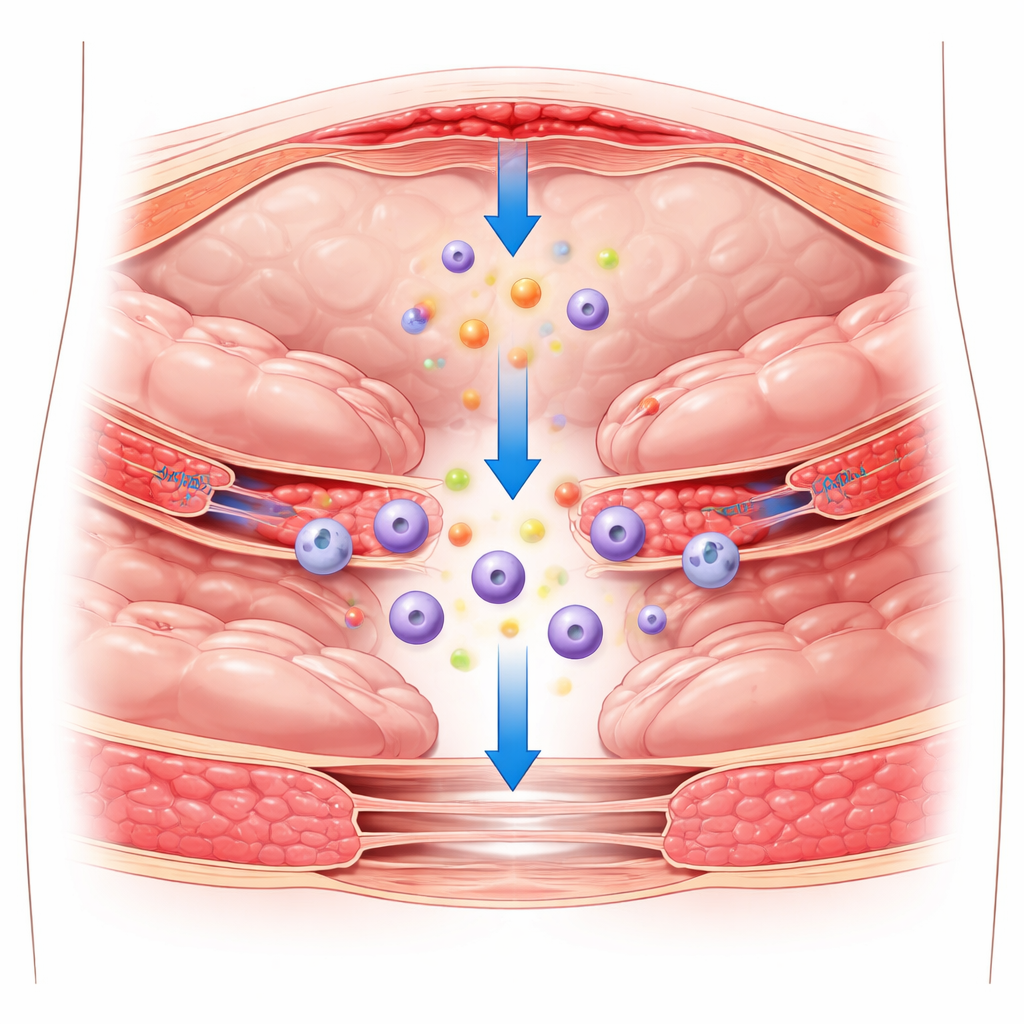
The hidden scars left by surgery
After an operation in the abdomen, the smooth lining that covers organs and the abdominal wall can be damaged. Normally that lining, made of a thin sheet of cells called mesothelial cells, helps organs glide past each other without sticking. When injured, it responds with inflammation: immune cells flood in, blood clotting pathways switch on, and a temporary protein mesh called fibrin forms. If this early response is not tightly controlled, the fibrin can become the backbone for permanent fibrous bands that tie organs together, creating postoperative adhesions. Existing prevention methods mostly use physical films or gels to keep tissues apart, but these barriers only partly work and have not solved the problem.
A key signal that summons first responders
The researchers focused on IL-8, a chemical signal that quickly rises when tissue is injured and that is known to attract neutrophils, one of the body’s main “first responder” white blood cells. Unlike mice, which do not have the IL-8 gene, humans and cynomolgus monkeys do, making these monkeys useful stand-ins for people. In laboratory tests with human cells, IL-8 activated both of its main receptors on neutrophils and drew far more of these cells toward it than a related chemokine, CXCL1, which uses only one of the receptors. This superior pulling power suggests IL-8 is a dominant switch for bringing neutrophils into the surgical field, where they can help fight danger but also lay the groundwork for excessive scarring.
A vicious loop between lining cells and immune cells
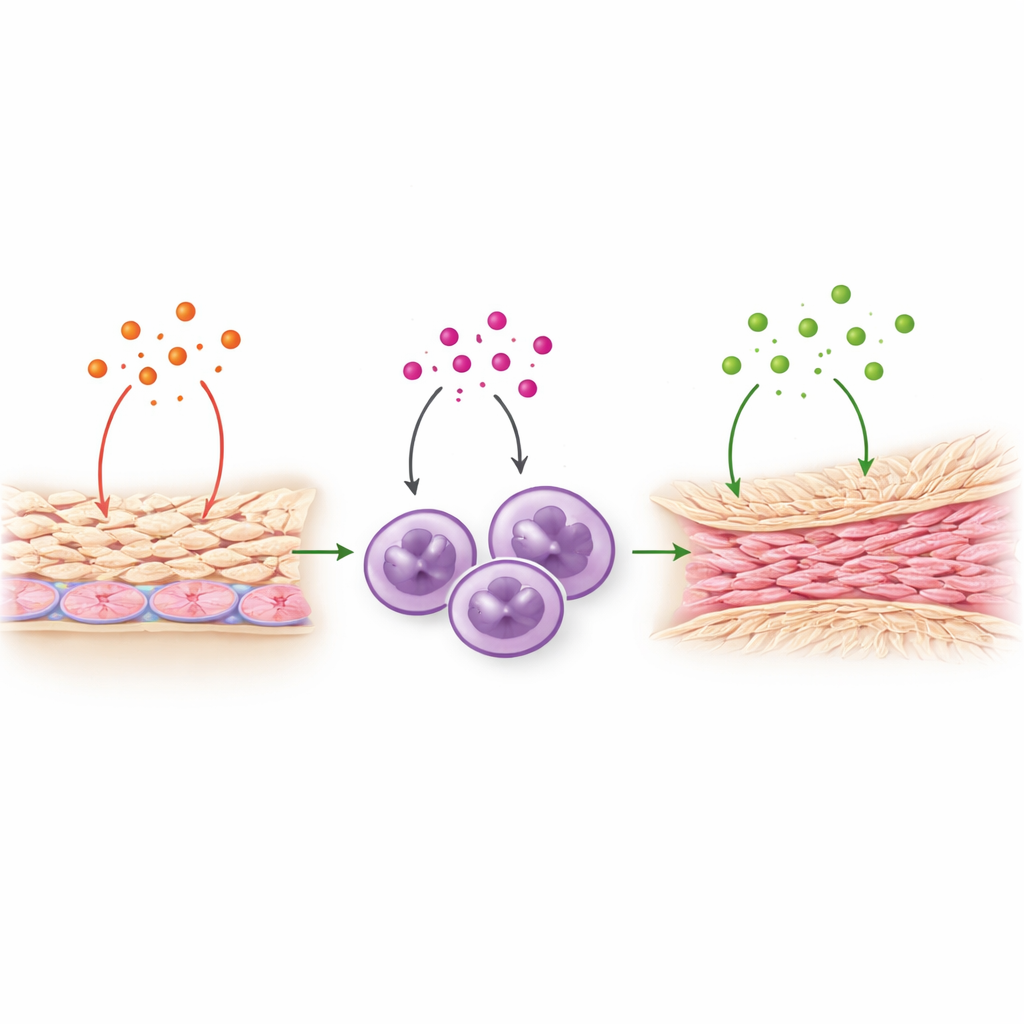
IL-8 turned out to do more than just call neutrophils. The team showed that IL-8 can act directly on mesothelial cells, which line the inner abdomen. When exposed to IL-8, these lining cells released higher amounts of TNF‑alpha, another potent inflammatory signal already implicated in adhesion formation. In turn, TNF‑alpha pushed the mesothelial cells to make more IL-8, setting up a self-reinforcing loop. TNF‑alpha also stimulated neutrophils to increase production of TGF‑beta1, a master controller of fibrosis that encourages tissue to lay down long-lasting collagen fibers. Together, these steps outline a relay: IL-8 → mesothelial activation and TNF‑alpha release → neutrophil activation and TGF‑beta1 release → buildup of fibrous scar tissue. Importantly, IL-8 itself did not directly switch on fibrosis genes, but it amplified the signals that do.
Testing an IL-8 blocker in monkeys
To see how this pathway behaves in a living organism, the scientists used cynomolgus monkeys that underwent standardized abdominal and uterine injury to trigger adhesions. IL-8 levels in the injured abdominal wall spiked within six hours of surgery and declined toward baseline within a week, marking a narrow early window when IL-8 is most active. The team then gave some monkeys a single intravenous dose of AMY109, a long‑acting antibody that neutralizes IL‑8, two days before surgery. When the animals were examined 26 days later with a laparoscope, those that had received AMY109 had markedly smaller and fewer adhesions on the abdominal wall than untreated animals. Adhesions on the uterus also tended to be milder, and in two treated monkeys were absent altogether, suggesting that dampening IL-8 can protect multiple sites inside the abdomen without obvious harm to normal wound healing.
What this could mean for patients
Taken together, the findings cast IL-8 as a central organizer of early inflammation and later fibrosis after abdominal surgery. By strongly recruiting neutrophils and driving a feedback loop with mesothelial cells that boosts TNF‑alpha and TGF‑beta1, IL-8 helps transform a short‑lived healing response into stubborn internal scar bands. Blocking IL-8 with an antibody like AMY109 in monkeys substantially reduced these adhesions, pointing to a potential new drug strategy that targets biology rather than relying only on physical barriers. If similar results are confirmed in people, patients might one day receive a short course of IL-8–blocking treatment around the time of surgery to lower their risk of painful, life‑altering postoperative adhesions.
Citation: Nakagawa, K., Tanimura, H., Yamazaki, M. et al. IL-8 contributes to postoperative adhesion formation through the crosstalk of neutrophils and mesothelial cells. Sci Rep 16, 14221 (2026). https://doi.org/10.1038/s41598-026-42159-x
Keywords: postoperative adhesions, interleukin-8, neutrophils, fibrosis, monkey model