Clear Sky Science · en
The role of sperm DNA fragmentation testing in predicting IVF and PGT-A outcomes
Why this matters for couples trying to conceive
When in vitro fertilization (IVF) does not work, attention often turns to the woman’s age, hormones, or uterus. But this study looks closely at the often overlooked other half of the equation: the man’s sperm. Specifically, it asks whether tiny breaks in sperm DNA — too small to see under a normal microscope — can predict which embryos will be healthy and which IVF attempts will lead to a baby, even when embryos are carefully screened with advanced genetic testing.
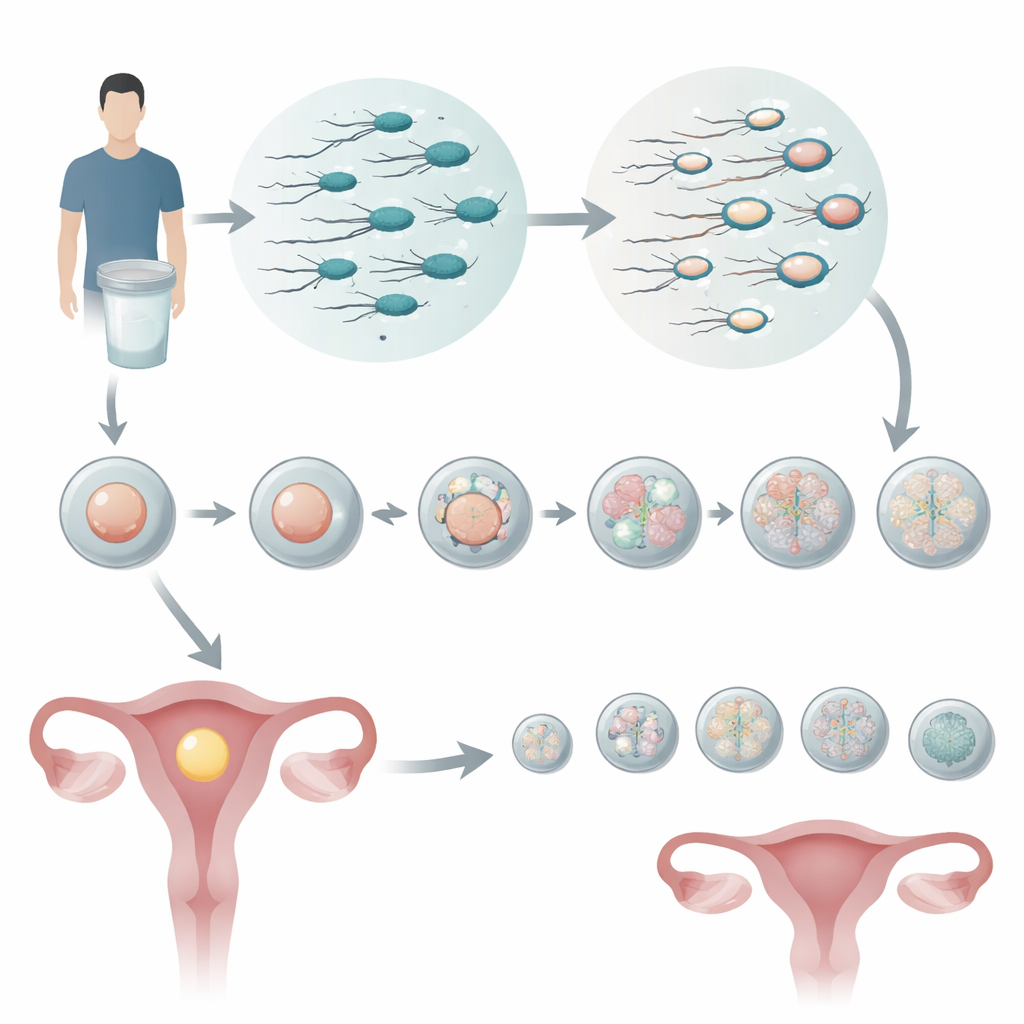
Looking beyond a basic sperm count
Most fertility clinics judge sperm mainly by how many there are, how well they swim, and how normal they look. These measurements are useful but crude, and two samples that look similar on paper can behave very differently in the lab. The researchers focused on a more subtle feature: how intact the sperm’s DNA is. They used a test that measures the DNA fragmentation index (DFI) — essentially, the percentage of sperm whose genetic material is broken. Men were grouped into low, medium, and high DFI, and their partners all underwent IVF along with preimplantation genetic testing for aneuploidy (PGT-A), a technique that checks embryos for the wrong number of chromosomes before transfer.
How the study was carried out
The team followed 124 couples treated at a single fertility center. All men had a DFI test, and all couples went through IVF cycles in which embryos were grown to the blastocyst stage, biopsied, and analyzed by next-generation sequencing. This allowed the scientists to link each man’s DFI level to several key steps: fertilization of eggs (by either conventional IVF or sperm injection), the number and quality of blastocysts formed, the rate of chromosomal abnormalities detected by PGT-A, and real-world outcomes such as implantation, clinical pregnancy, and live birth after transfer of chromosomally normal embryos.
What sperm DNA damage did and did not affect
Men with high DFI tended to be older and had poorer sperm motility. In these high-DFI cases, fertilization rates were lower when a single sperm was injected directly into the egg (ICSI), and fewer embryos developed into good-quality blastocysts suitable for freezing. This suggests that visible sperm traits like movement and shape do not fully reveal deeper DNA problems. Yet when the researchers looked at PGT-A results, a surprise emerged: the proportion of embryos with normal, mosaic, or abnormal chromosome numbers was similar across low, medium, and high DFI groups. In other words, among embryos that survived to biopsy, having started from more damaged sperm did not clearly translate into more chromosomal errors.
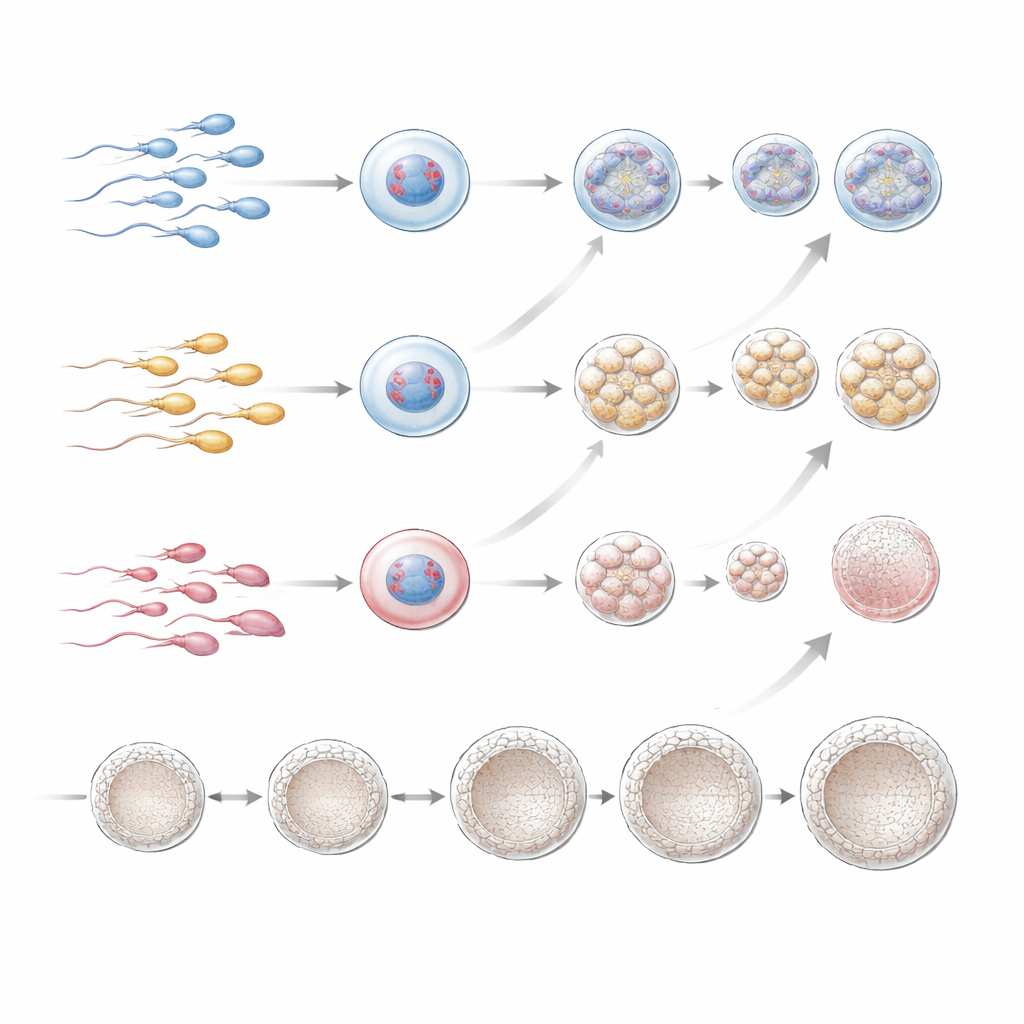
Do damaged sperm doom IVF attempts?
To answer the question couples care about most, the team tracked what happened after transfer of embryos that PGT-A had labeled as chromosomally normal (or low-level mosaic). Implantation, pregnancy, and live birth rates per embryo transfer were broadly comparable among all three DFI groups, even in the small high-DFI subgroup. While high DFI was linked to fewer good embryos in the freezer, once a healthy-looking, chromosomally normal blastocyst existed, its chance of leading to a baby did not seem strongly influenced by how fragmented the father’s sperm DNA had been in the original sample. The authors caution, though, that their study was retrospective, involved a highly selected group of mostly older women, and included relatively few men with very high DFI, so subtle effects could have been missed.
What this means for patients and clinics
For couples, the take-home message is twofold. First, a high level of sperm DNA damage can make it harder to reach the stage of having multiple good embryos to choose from, and it may modestly reduce success at fertilization and early development. Second, if IVF does yield chromosomally normal embryos, those embryos can still implant and produce babies at rates similar to those from men with lower DFI, possibly because the egg and early embryo can repair some paternal DNA damage. The authors suggest using sperm DNA fragmentation testing as an additional tool, not to rule out treatment, but to identify male-factor issues, guide sperm selection methods, and refine IVF strategies aimed at improving the number and quality of embryos available for transfer.
Citation: Okubo, T., Kobayashi, T., Hayashi, T. et al. The role of sperm DNA fragmentation testing in predicting IVF and PGT-A outcomes. Sci Rep 16, 14607 (2026). https://doi.org/10.1038/s41598-026-38974-x
Keywords: male infertility, sperm DNA fragmentation, IVF outcomes, embryo genetic testing, blastocyst development