Clear Sky Science · en
Trifluoperazine causes mast cell apoptosis through a secretory granule-mediated pathway
Turning a Mental Health Drug into an Allergy Fighter
People with allergies, asthma, or certain inflammatory diseases often suffer because of a single type of immune cell: the mast cell. This study explores an unexpected idea—repurposing an old antipsychotic medicine, trifluoperazine, to selectively remove harmful mast cells while sparing most other cells. By uncovering exactly how this drug makes mast cells self‑destruct, the work opens a potential new path for treating allergic and mast cell–driven conditions.
The Trouble-Making Immune Cell
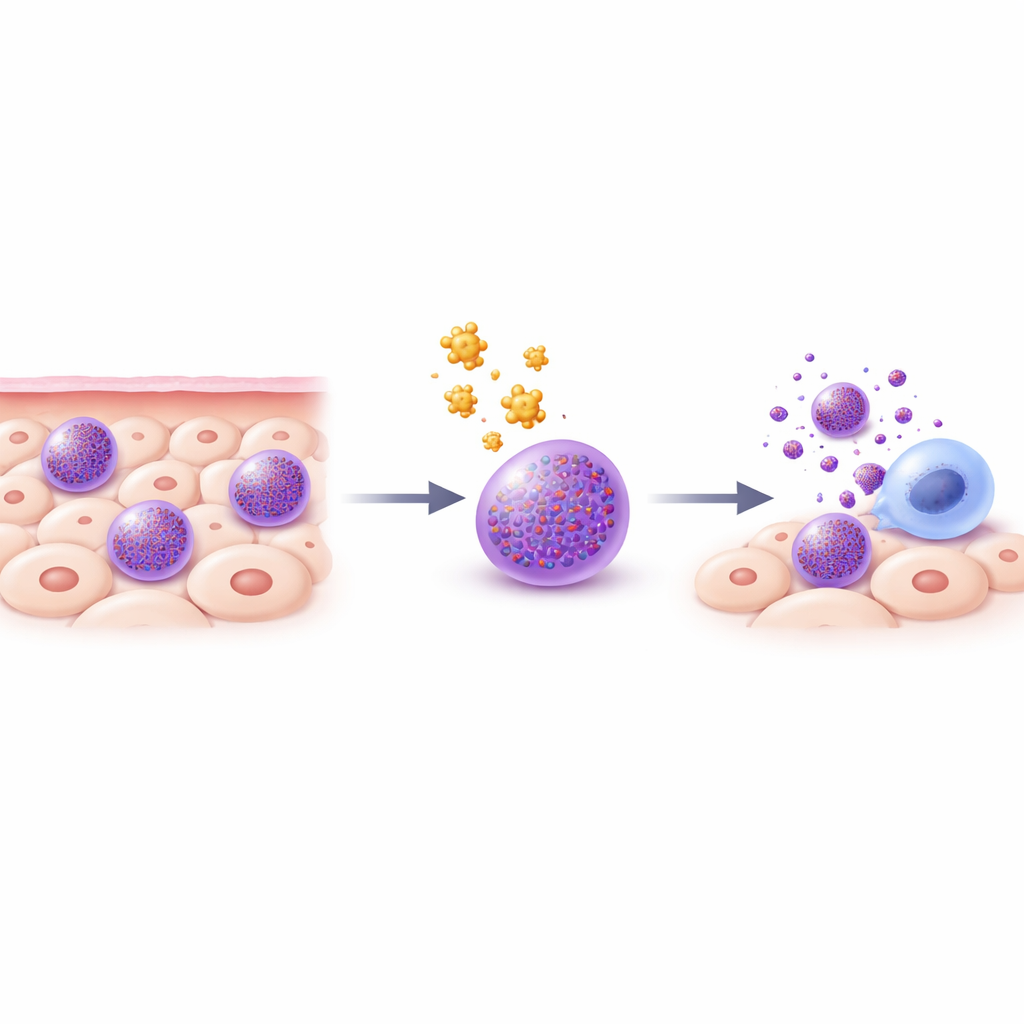
Mast cells are immune sentinels that sit in tissues like the skin, lungs, and gut. They are packed with tiny acidic storage sacs called granules, which contain powerful substances such as histamine, enzymes, and inflammatory molecules. When mast cells are activated—for example during an allergic reaction—they rapidly empty these granules, triggering swelling, itching, and other symptoms. Existing treatments, like antihistamines or mast cell–stabilizing drugs, only block a fraction of the many chemicals mast cells can release. Because disease often results from the combined action of multiple mast cell mediators, the authors considered a bolder strategy: to selectively trigger controlled cell death in mast cells themselves.
A Surprising Candidate from Psychiatry
The team focused on “lysosomotropic” drugs—small, weakly basic molecules that build up inside acidic compartments such as lysosomes and mast cell granules. At high enough levels, these drugs can weaken granule membranes and cause them to leak, sometimes leading to cell death. Trifluoperazine, long used to treat schizophrenia and anxiety, belongs to a drug family already known to accumulate in such acidic compartments. The researchers tested trifluoperazine on a range of mouse and human cells, including airway smooth muscle cells, fibroblasts, epithelial cells, neutrophils, eosinophils, and several mast cell populations. They found that clinically relevant doses were strikingly toxic to mast cells, but left most other cell types largely unharmed; only eosinophils, another granule-rich immune cell type, showed some sensitivity at higher doses.

How the Drug Triggers Self-Destruction
To understand what happens inside mast cells exposed to trifluoperazine, the scientists tracked changes in granules and cell health over time. Soon after treatment, many mast cells displayed classic hallmarks of apoptosis, a tidy, non-inflammatory form of programmed cell death: they bound Annexin V, showed DNA fragmentation, shrank in size, and developed membrane blebs while keeping their outer membrane intact. Measurements with pH-sensitive dyes revealed that trifluoperazine made the granules less acidic and, at the same time, made the surrounding cell fluid more acidic—evidence that protons and other contents were leaking out of the granules. A key mast cell enzyme, tryptase, normally locked inside granules, was detected in the cell’s interior fluid shortly after drug exposure, confirming that granule membranes had become permeable.
Granules at the Heart of the Action
Microscopy provided a visual window into this process. Under the electron microscope, untreated mast cells showed dense, well‑structured granules. After trifluoperazine treatment, these granules swelled, lost much of their inner material, and sometimes showed visible breaks in their membranes, consistent with leakage into the cell. When the researchers blocked the acid‑pumping V‑ATPase, which normally keeps granules acidic, trifluoperazine could no longer efficiently deacidify the granules, move tryptase into the cytosol, fragment DNA, or kill the mast cells. This strong protection showed that granule acidity is crucial for the drug’s destructive effect. Surprisingly, enzymes called caspases—central executioners in many forms of apoptosis—played only a minor role here. Instead, other proteases, especially a subset of serine proteases, appeared to influence whether the cells died in an orderly apoptotic fashion or in a more damaging necrosis-like way.
What This Could Mean for Future Treatments
Overall, the study reveals that trifluoperazine can selectively kill mast cells by destabilizing their acidic granules, causing their own toxic contents to leak out and drive a largely caspase‑independent, apoptosis‑like death. Because mast cells are key culprits in many allergic and inflammatory diseases, and because trifluoperazine is already an approved drug, this granule‑mediated pathway suggests a promising route to repurpose or refine such compounds for clinical use. In principle, carefully targeted dosing might reduce mast cell numbers in affected tissues—such as the airways in asthma or nasal polyps—without broadly harming neighboring cells, offering a new strategy to dial down mast cell–driven disease.
Citation: Vraila, M., Hu Frisk, J.M., Mayavannan, A. et al. Trifluoperazine causes mast cell apoptosis through a secretory granule-mediated pathway. Cell Death Discov. 12, 185 (2026). https://doi.org/10.1038/s41420-026-03122-x
Keywords: mast cells, trifluoperazine, allergy therapy, granule-mediated apoptosis, lysosomotropic drugs