Clear Sky Science · en
A new candidate tumor suppressor tRF-Ser inhibits gastric cancer progression by regulating the CNBP/HSPA8 axis
Why this matters for stomach cancer
Stomach (gastric) cancer remains one of the deadliest cancers worldwide, in part because tumors often resist chemotherapy and spread aggressively. This study uncovers a previously unknown natural defense inside stomach cells: a tiny RNA fragment called tRF-Ser that helps keep tumors in check. By showing how this molecule slows cancer growth, encourages a form of iron‑driven cell death, and makes chemotherapy work better, the research points to fresh strategies for treating patients whose tumors are hard to control.
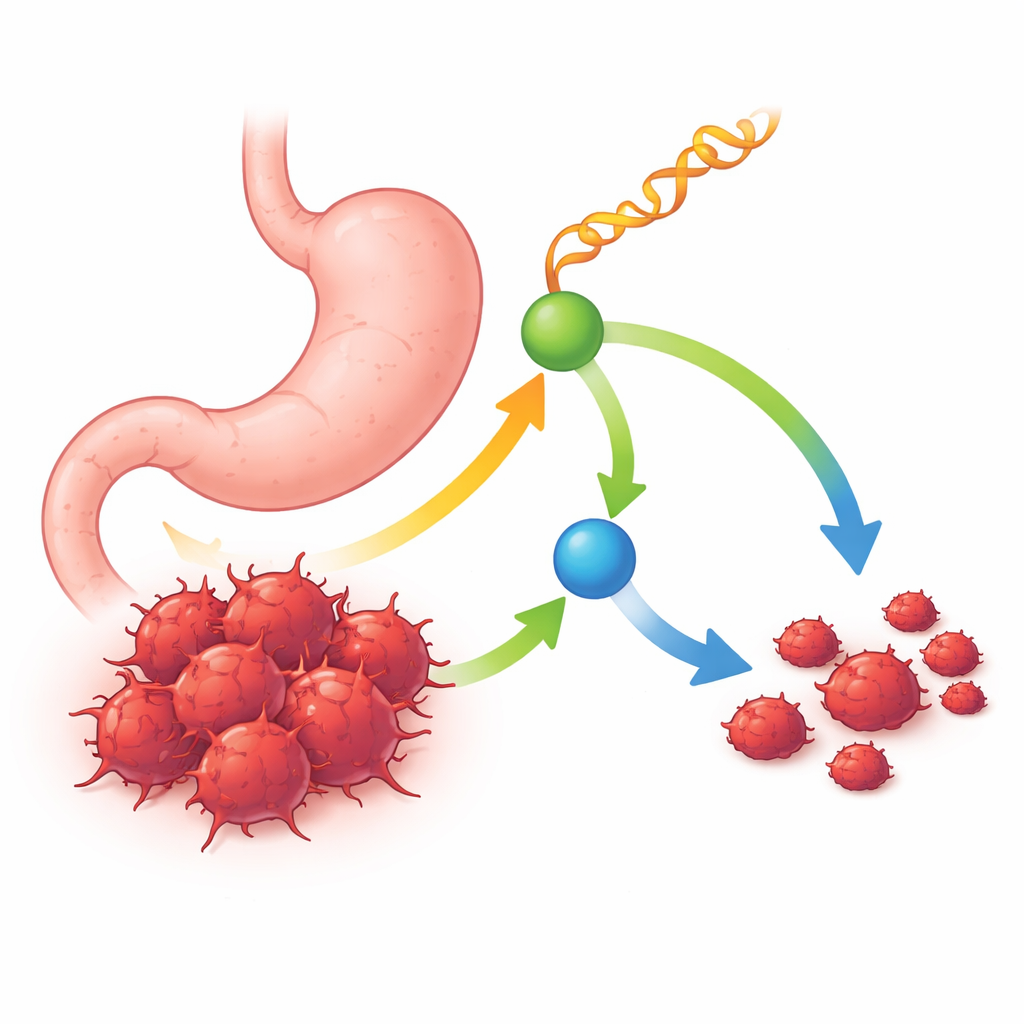
A small RNA with a big protective role
The researchers began by comparing small RNA molecules in human stomach tumors and nearby healthy tissue. They focused on a special class called tRNA‑derived fragments—short pieces cut from the cell’s protein‑building adapter RNAs. Among many candidates, one fragment stood out: tRF-Ser, which was consistently lower in tumor samples and stomach cancer cell lines than in normal tissue. Patients whose tumors had more tRF-Ser tended to live longer and had smaller, less advanced cancers with fewer lymph node metastases. These patterns suggested that tRF-Ser acts as a natural tumor suppressor that is lost as the disease worsens.
How tRF-Ser slows tumor growth and spread
To test what tRF-Ser actually does, the team boosted or blocked its levels in stomach cancer cells grown in the lab. When tRF-Ser was increased, cancer cells divided more slowly, formed fewer colonies, and were more likely to be halted early in the cell cycle, before copying their DNA. Their ability to migrate and invade through membranes was also reduced, and key markers of a shape‑shifting program called epithelial‑mesenchymal transition (EMT)—which helps tumors spread—went down. When tRF-Ser was reduced, the opposite happened: cells grew faster, became more invasive, and showed stronger EMT features. In mice, tumor cells engineered to make extra tRF-Ser formed smaller subcutaneous tumors and fewer lung metastases, confirming that this small RNA can restrain cancer in living organisms.
Rewiring cancer’s stress and death pathways
Beyond simply slowing growth, tRF-Ser pushes cancer cells toward a form of iron‑dependent, lipid‑driven cell death known as ferroptosis. Under treatment with a ferroptosis‑triggering drug, cells rich in tRF-Ser showed more oxidative damage, more disrupted mitochondria, and lower levels of a key protective enzyme called GPX4, while an opposite pattern appeared when tRF-Ser was scarce. The study also examined responses to 5‑fluorouracil, a standard chemotherapy for gastric cancer. Cells with more tRF-Ser were more easily killed by the drug, whereas cells with less tRF-Ser were more resistant. Combining tRF-Ser overexpression with both 5‑fluorouracil and a ferroptosis inducer produced the strongest tumor‑shrinking effects in mice, along with clear biochemical signs of heightened oxidative injury inside the tumors.
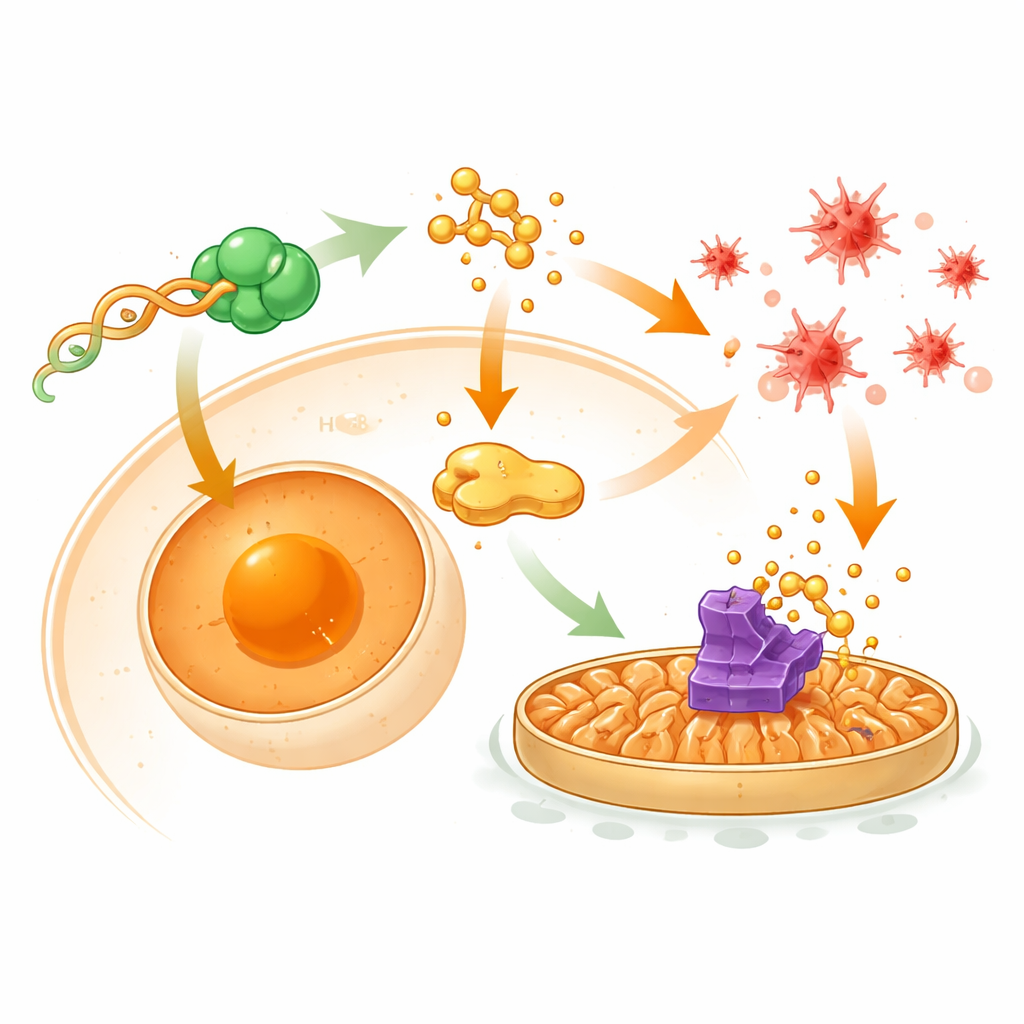
The hidden control circuit inside tumor cells
To understand the wiring behind these effects, the researchers mapped how tRF-Ser interacts with proteins and downstream genes. They found that tRF-Ser physically binds a DNA‑binding protein called CNBP and keeps more of it trapped in the cell’s cytoplasm instead of the nucleus. When CNBP reaches the nucleus, it normally switches on a chaperone gene called HSPA8, which in turn helps maintain GPX4 and supports EMT‑driving signals involving the protein β‑catenin. By holding CNBP outside the nucleus, tRF-Ser lowers HSPA8 levels, weakens β‑catenin’s movement into the nucleus, and allows another protein, STUB1, to tag GPX4 for destruction. This cascade simultaneously dampens invasion‑linked EMT and removes a brake on ferroptosis, making cancer cells more vulnerable to oxidative damage and chemotherapy.
What this means for future treatments
Taken together, the work reveals a compact regulatory axis—tRF-Ser, CNBP, and HSPA8—that ties together tumor growth, metastatic behavior, cell death, and drug response in gastric cancer. In everyday terms, tRF-Ser acts like a molecular traffic officer, diverting a pro‑growth factor (CNBP) away from the cell’s control center so it cannot flip on a survival program (via HSPA8 and GPX4). Restoring or mimicking tRF-Ser, or targeting its downstream partners, could therefore make existing drugs such as 5‑fluorouracil more effective and help overcome treatment resistance. While further work is needed before clinical use, this study highlights how tiny pieces of RNA can hold the keys to tipping cancer cells from survival toward self‑destruction.
Citation: Jiao, J., Wang, G., Liu, J. et al. A new candidate tumor suppressor tRF-Ser inhibits gastric cancer progression by regulating the CNBP/HSPA8 axis. Cell Death Dis 17, 379 (2026). https://doi.org/10.1038/s41419-026-08608-1
Keywords: gastric cancer, tumor suppressor RNA, ferroptosis, chemoresistance, HSPA8 CNBP axis