Clear Sky Science · en
Dasatinib and quercetin senolytic treatment delays early onset intervertebral disc degeneration in SM/J mice
Why this back story matters
Back pain is one of the most common reasons people miss work or struggle with daily tasks, and worn-out spinal discs are a major culprit. Yet current treatments mostly ease symptoms rather than slowing the damage itself. This study in mice explores a new idea: using drugs that selectively target "aged" or damaged cells inside spinal discs to delay early breakdown. The work suggests that a drug combination already being tested in humans for other conditions could one day help protect people who are genetically prone to disc-related back pain.
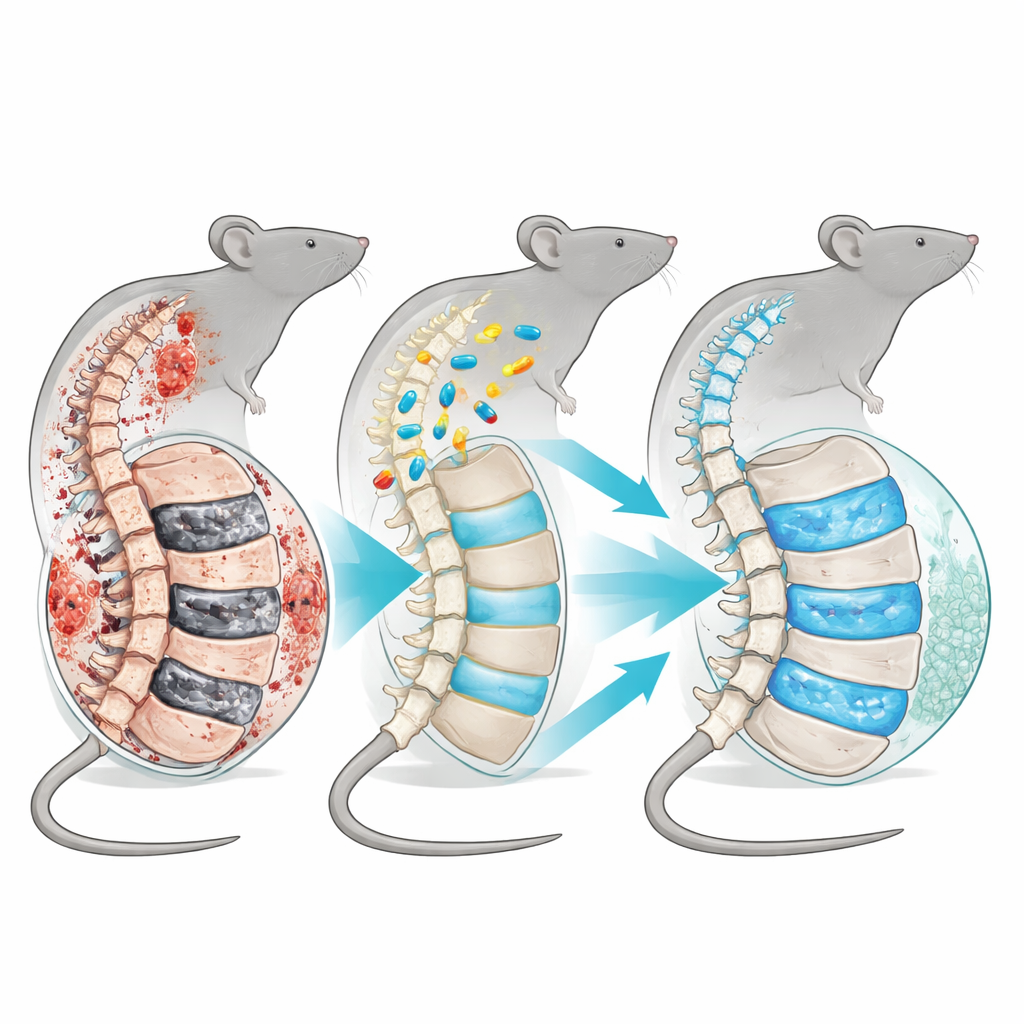
When spinal cushions wear out too soon
Between each pair of vertebrae in the spine sits a disc that acts like a tough, water-rich cushion. In the center is a gel-like core (the nucleus pulposus) surrounded by a fibrous ring and capped by thin endplates. In some mouse strains called SM/J, these discs begin to degenerate unusually early in life, mimicking aggressive, early-onset disc disease seen in some humans. By just 17 weeks of age—roughly young adulthood for a mouse—these animals already show features such as loss of normal disc structure, scarring of the soft core, and changes in cell behavior that resemble an aged or injured spine.
Old-before-their-time cells inside the disc
The researchers focused on cellular senescence, a state where cells stop dividing, resist dying, and release a stew of inflammatory and tissue-remodeling molecules known as the senescence-associated secretory phenotype (SASP). In SM/J mouse discs, they found high levels of senescence markers, including proteins called p19 and p21, well before obvious structural damage appeared. Large-scale gene activity profiling showed that the disc tissues shared many features with established “senescent” gene signatures: changes in cell-cycle control, stress-response pathways, and signals linked to inflammation, blood vessel growth, and scarring. Together, these data suggest that prematurely senescent cells are a driving force behind early disc breakdown in this model.
Testing drugs that clear or calm senescent cells
The team then tested two systemic (body-wide) “senolytic” approaches—drugs designed to remove or weaken senescent cells. One group of young SM/J mice received weekly injections of navitoclax, and another received a cocktail of dasatinib plus quercetin (often abbreviated DQ). Treatment began at four weeks of age, before severe damage was present, and continued until 17 weeks. Navitoclax, despite success in other tissues and when injected directly into discs in past work, did not improve disc structure or reduce markers of senescence in these mice. By contrast, dasatinib plus quercetin led to noticeably healthier discs: the central core and outer ring were better preserved, scarring was reduced, and fewer discs reached the most severe grades of degeneration.
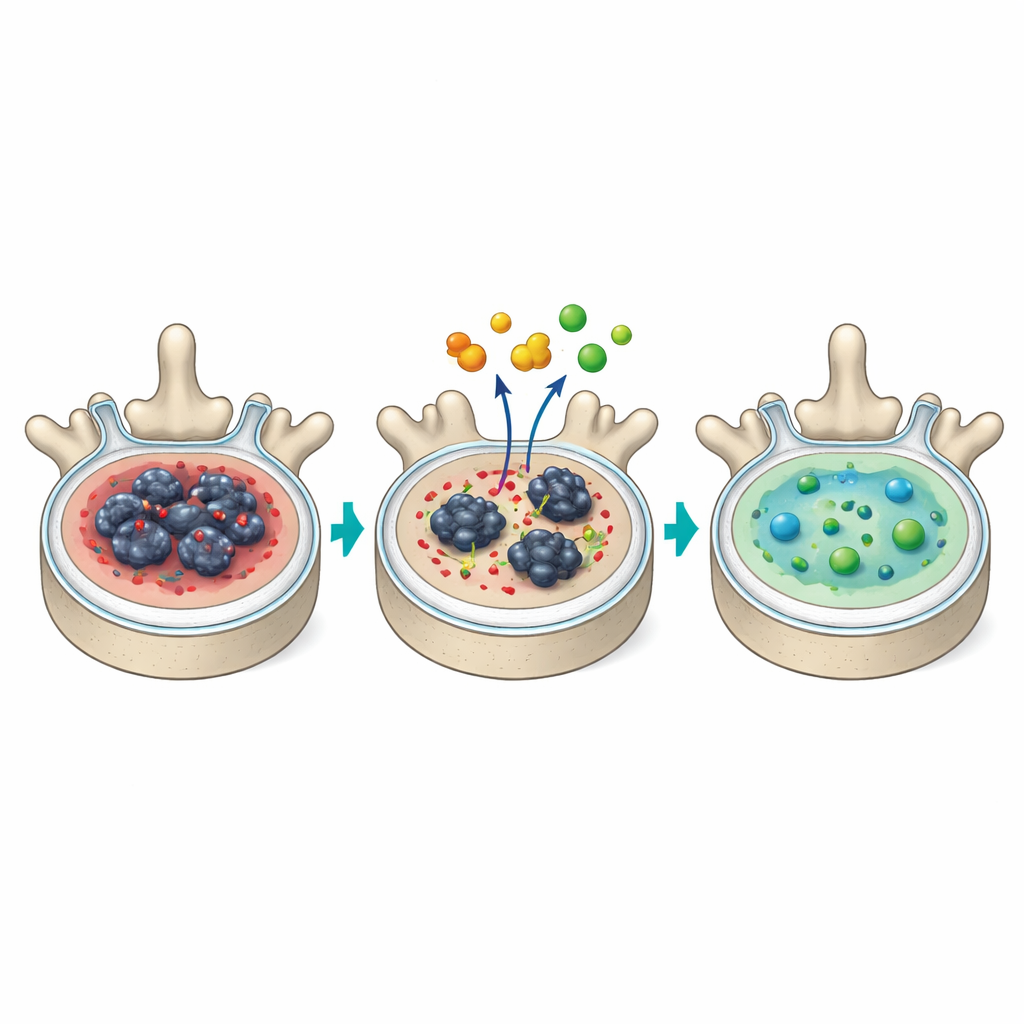
Healthier matrix, healthier cells
Discs from DQ-treated mice showed fewer senescent cells, lower levels of key SASP molecules such as IL-6 and MMP13, and less of the scarring protein TGF-β. The central core contained fewer thick collagen fibers—a hallmark of fibrosis—and more of the thin, organized fibers seen in healthier tissue. Cells in the core more often retained features typical of youthful disc cells and were less likely to resemble hypertrophic cartilage cells associated with end-stage damage. Importantly, DQ-treated discs contained more living cells and fewer dying (TUNEL-positive) cells over time, suggesting that this regimen helps existing cells survive in a more balanced, less inflammatory environment rather than simply wiping them out. At the whole-body level, the treatment modestly reduced certain inflammatory signals in the blood but left the vertebral bones largely unchanged, hinting at a favorable safety profile in the spine.
Uncovering the control switches inside
To understand how DQ reshapes disc biology, the authors compared gene activity in treated and untreated discs. They found coordinated changes in pathways that govern the cell cycle, DNA damage responses, and stress-signaling networks, particularly those involving JNK and a transcription factor family called JUN. When they compared these results with an earlier study in standard aging mice, a common pattern emerged: in both genetic early-onset and age-related disc degeneration, DQ consistently dialed down genes such as Junb and Zfp36l1, which are tied to senescence, inflammation, and fibrosis. In human disc cells grown in the lab, blocking JUN with a separate drug mimicked many of DQ’s benefits, including reduced senescence markers and dampened SASP genes, further linking JUN signaling to the protective effect.
What it could mean for future back pain care
Altogether, the study shows that in a mouse model prone to early disc breakdown, senescent cells appear early and help drive disease, and that systemic treatment with dasatinib plus quercetin can slow structural damage, limit scarring, and preserve more youthful disc cells. The findings also point to JUN-related pathways as key control knobs that these drugs may turn down. While these results are preclinical and do not yet translate directly into a therapy for people, they strengthen the case for senolytic-style strategies as a way to modify disc disease itself, rather than just treating pain after the damage is done.
Citation: Novais, E.J., Ottone, O.K., Jagannath, S. et al. Dasatinib and quercetin senolytic treatment delays early onset intervertebral disc degeneration in SM/J mice. Bone Res 14, 42 (2026). https://doi.org/10.1038/s41413-026-00526-4
Keywords: intervertebral disc degeneration, cellular senescence, senolytic therapy, dasatinib and quercetin, back pain