Clear Sky Science · en
Drug-induced inflammatory colitis: a review of novel agents
Why Some Medicines Can Upset the Gut
Modern drugs have transformed the treatment of cancer and immune diseases, but they can sometimes bring hidden side effects. This review article looks at a serious but often overlooked problem: certain new medicines can inflame the large intestine and cause a severe form of colitis. For patients and families, understanding this risk helps explain sudden bouts of stomach pain or diarrhea that appear after starting powerful therapies, and shows why doctors watch bowel symptoms so closely.
What Colitis Is and Why Drugs Matter
Colitis simply means inflammation of the inner lining of the large bowel. It can arise from infections, reduced blood flow, long‑standing conditions like Crohn’s disease and ulcerative colitis, or from medications. Drug‑induced colitis is still relatively uncommon, but it can be dangerous, sometimes even leading to bowel perforation (a hole in the intestine) if ignored. As new targeted drugs and biologic therapies enter routine care, doctors are seeing more cases where the gut reacts badly to these treatments. The challenge is that drug‑induced colitis can look and feel almost identical to classic inflammatory bowel disease, making it hard to pinpoint the true cause.
New Cancer Tablets and Gut Side Effects
The authors first examine tyrosine kinase inhibitors and phosphatidylinositol 3‑kinase (PI3K) inhibitors, tablet medicines that block key growth and survival signals in cancer cells. These drugs often cause diarrhea; in some people they trigger true colitis. Tyrosine kinase inhibitors may irritate the bowel lining directly or disturb protective growth factors, and in the case of dasatinib, may awaken latent viral infections in the gut. Most patients experience mild symptoms that improve with dose reduction or stopping the drug, but a small number can develop bleeding or even bowel perforation. PI3K inhibitors tend to cause later‑onset, more severe diarrhea that frequently requires hospital care, and perforation is notably more common in this group.
Immune‑Targeting Drugs That Disturb Gut Balance
Other medicines work by dialing down specific immune signals, but in doing so can upset the delicate balance that protects the bowel. The review discusses tocilizumab, a drug that blocks the immune messenger IL‑6, commonly used in rheumatologic diseases. IL‑6 normally helps repair the gut lining after injury, so blocking it may slow healing and make erosions and ulcers more likely. The authors also describe drugs that block IL‑17, widely used in psoriasis and arthritis. IL‑17 helps maintain the gut’s barrier function; when it is blocked, the intestinal wall can become leaky and more vulnerable to inflammation. Reported cases range from mild loose stools to full‑blown colitis resembling Crohn’s disease or ulcerative colitis, sometimes in people with no previous gut problems.
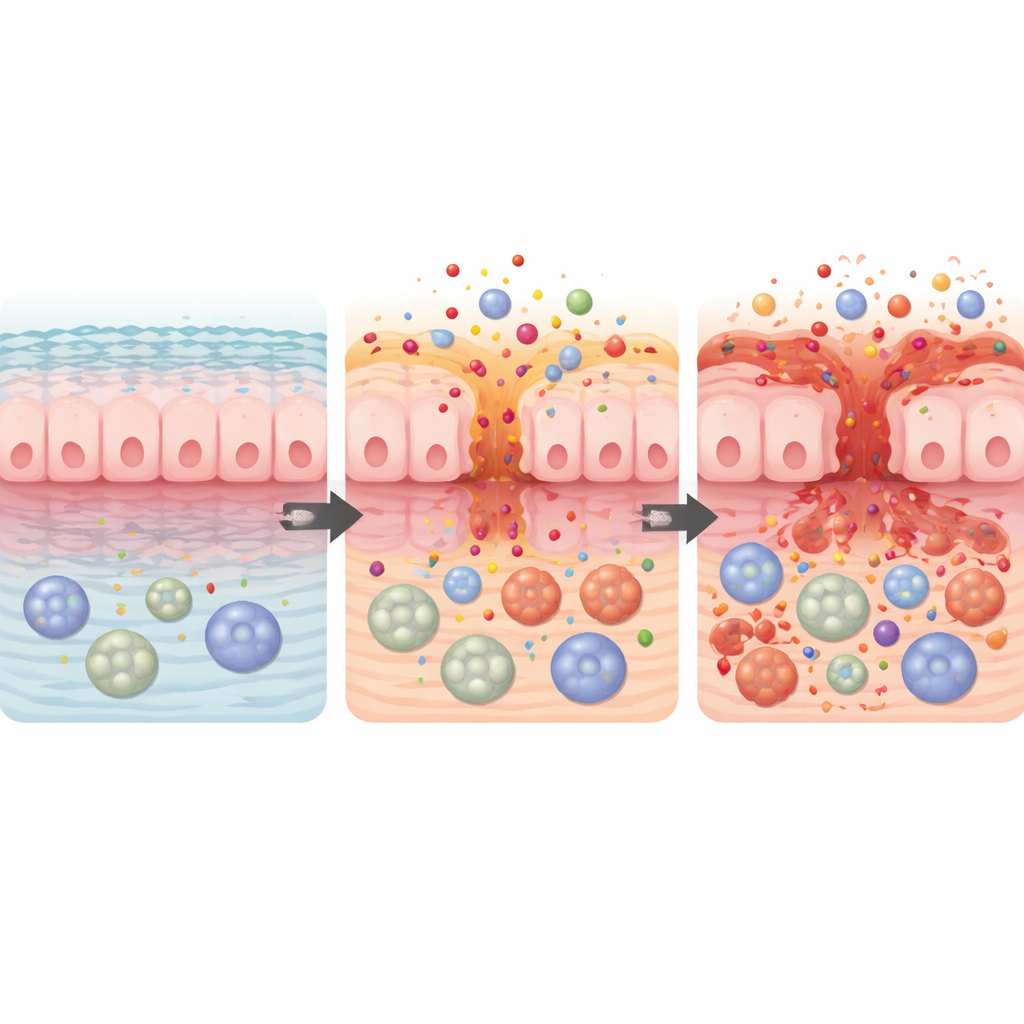
Antibody Therapies and the Loss of Gut Protection
The review highlights a final group: anti‑CD20 monoclonal antibodies, such as rituximab and ocrelizumab, which deplete B cells, a type of white blood cell. These therapies are mainstays in blood cancers and multiple sclerosis. B cells normally help defend the gut surface by producing protective antibodies and calming signals. When they are stripped away, the gut’s “peacekeeping” system can fail, leading to inflammation that closely mimics long‑term bowel disease. Symptoms often emerge months after treatment starts and may continue until B cells slowly return. In many patients, stopping the drug and using standard anti‑inflammatory treatments brings remission, but a subset need surgery or long courses of immune‑targeting medicines.
Finding and Treating the Problem Early
To a lay reader, the key message is that some powerful modern medicines can unintentionally inflame the large intestine. Because drug‑induced colitis can look exactly like classic bowel disease, doctors rely on careful timing of symptoms, stool tests, endoscopy, and tissue samples to separate one from the other. Stopping the culprit medicine is usually the first and most important step, often combined with steroids or other gut‑focused treatments when symptoms are severe. The authors call for better studies and clearer guidelines so that, as new therapies continue to improve survival and quality of life, their hidden impact on the gut can be recognised and managed before it leads to serious harm.
Citation: Terlato, M., Dimovski, S., Burkhardt, M. et al. Drug-induced inflammatory colitis: a review of novel agents. npj Gut Liver 3, 12 (2026). https://doi.org/10.1038/s44355-026-00063-1
Keywords: drug-induced colitis, targeted cancer therapy, biologic drugs, inflammatory bowel disease, gut side effects