Clear Sky Science · en
Cationic biocide susceptibility and tolerance-associated genes in clinical, environmental, and commensal Enterococcus isolates
Why cleaning chemicals do not always win
Hospitals rely on disinfectants and antiseptics to keep dangerous germs in check, yet some bacteria manage to hang on and spread. This study looks at Enterococcus, a common gut bacterium that can cause serious infections, and asks how well it withstands two widely used disinfectants, as well as antibiotics. Understanding where stronger, more tolerant strains come from helps explain why hospital infections can be so stubborn and how hygiene practices might be improved.
Where the bacteria come from
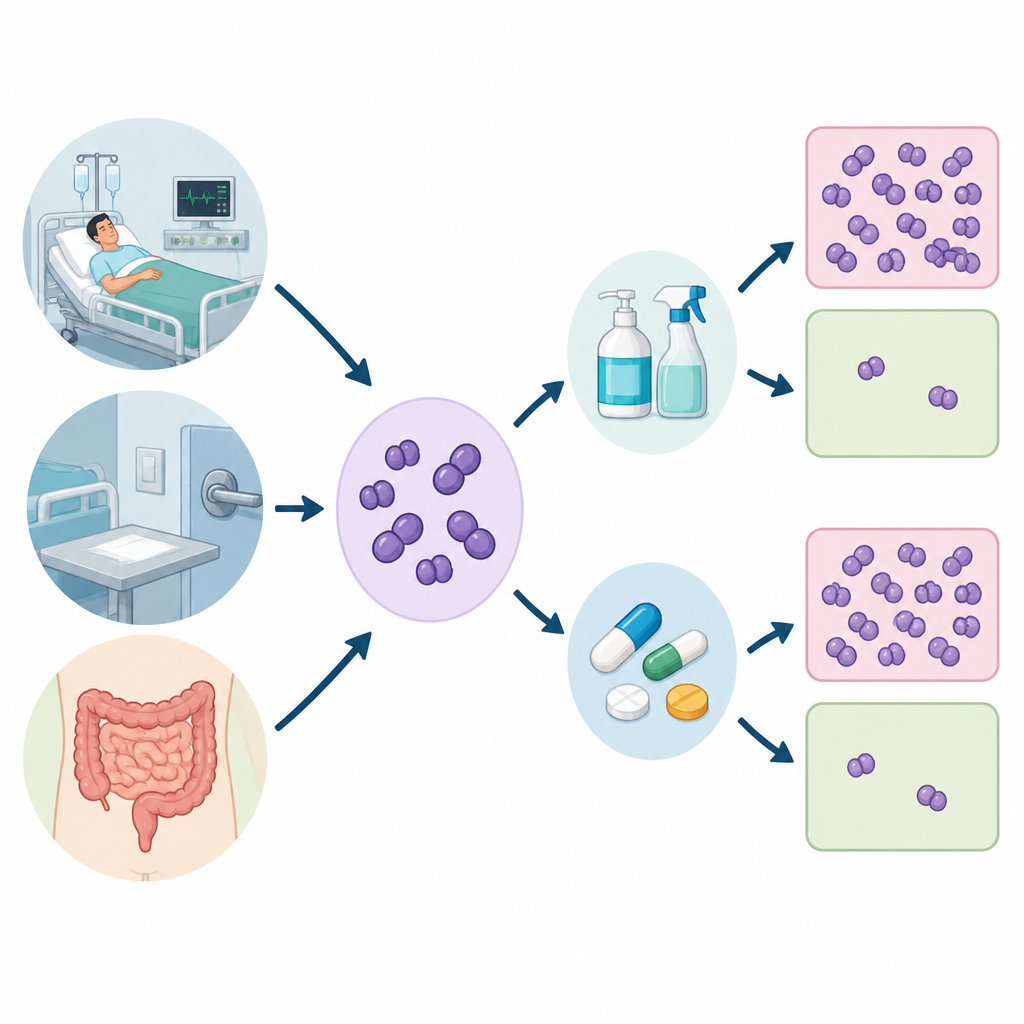
The researchers collected 520 samples from three places: hospital patients, hospital surfaces such as beds and equipment, and the stool of healthy volunteers. From these, they isolated 120 strains of Enterococcus, focusing on the two species most often linked to human disease. They then tested how easily each strain was killed by several antibiotics and by two common cleaning chemicals, chlorhexidine and benzalkonium chloride, which are used in hand scrubs, surface disinfectants, and many everyday hygiene products.
How the team measured toughness
To gauge how tough the bacteria were, the team determined the minimum inhibitory concentration, or MIC, for each disinfectant, which is the lowest amount needed to stop bacterial growth under lab conditions. They also tested whether the bacteria formed slimy communities called biofilms, which can cling to surfaces and shield cells from harm. Finally, they looked for specific genetic elements that act like tiny pumps inside the cell membrane, pushing out antibiotics and disinfectant molecules before they can do damage.
Hospital strains prove harder to kill
The results showed a clear pattern. Enterococcus strains taken from patients were more resistant to key antibiotics, especially gentamicin and ciprofloxacin, than those from hospital surfaces or healthy people. These clinical strains also tended to need higher doses of chlorhexidine and benzalkonium chloride to be controlled, signaling reduced susceptibility. Two thirds of all isolates could form biofilms, and this ability was much more common and stronger among the clinical strains, suggesting that hospital bacteria are better equipped to stick around and survive cleaning efforts.
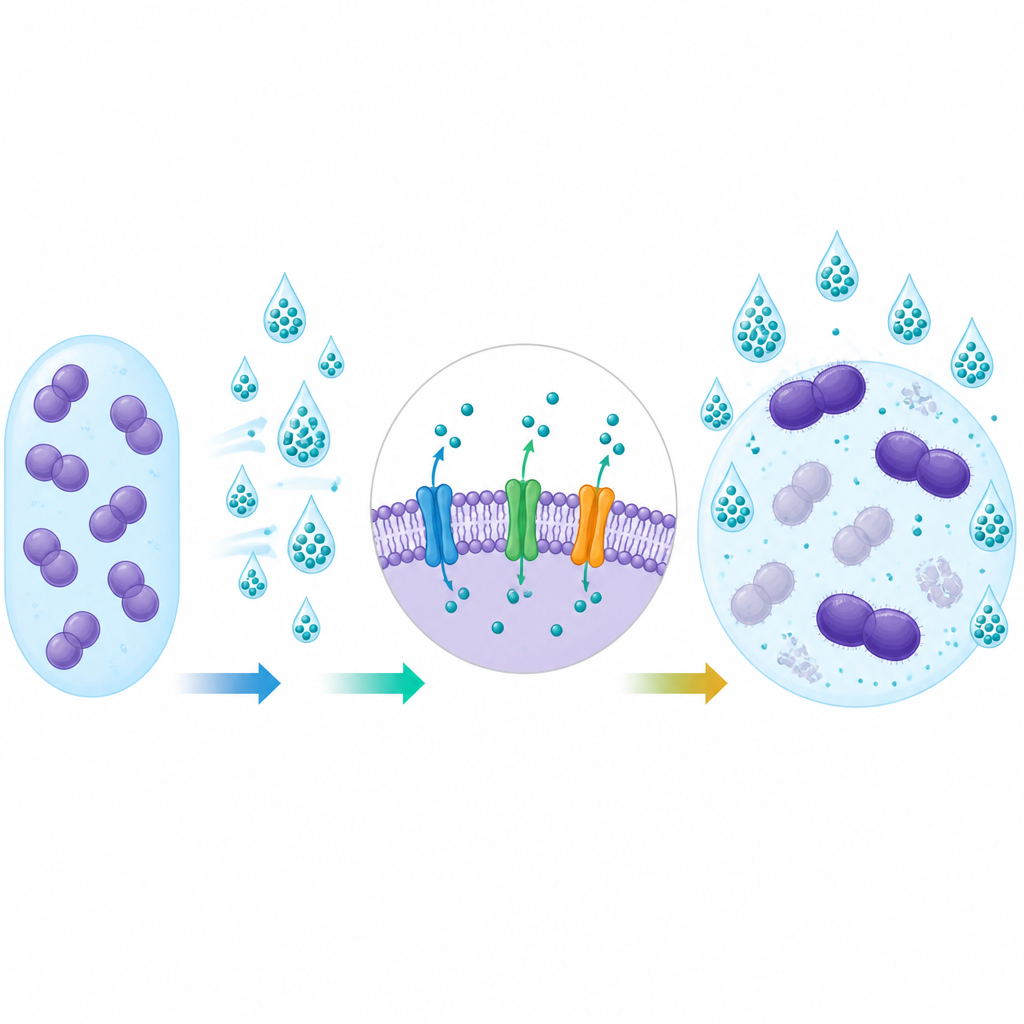
Genes that help bacteria shrug off chemicals
When the researchers examined the bacteria’s DNA, they frequently found two efflux pump genes, called efrAB and emeA. These genes were much more common in strains from patients than in those from the environment or healthy volunteers. Strains carrying these genes tended to show higher disinfectant MIC values and were far more often resistant to the antibiotic gentamicin. This link supports the idea that the same mechanisms that help bacteria tolerate disinfectants can also make them less sensitive to certain drugs, although the relationship was not perfect in every test.
What this means for infection control
For a lay reader, the take-home message is that some hospital Enterococcus are learning to cope with both antibiotics and cleaning chemicals, helped by sticky biofilms and genetic pumps that spit out harmful substances. The study does not suggest that disinfectants are useless, but it does show that heavy and sometimes uneven use can favor tougher strains. Paying attention to how disinfectants are used, and to bacterial traits such as biofilm formation and efflux genes, may help hospitals design cleaning and treatment strategies that slow the rise of these hardier microbes.
Citation: Eldahshan, M.M., Amer, A.K., Genena, D.E. et al. Cationic biocide susceptibility and tolerance-associated genes in clinical, environmental, and commensal Enterococcus isolates. Sci Rep 16, 15063 (2026). https://doi.org/10.1038/s41598-026-51663-z
Keywords: Enterococcus, biocide resistance, chlorhexidine, benzalkonium chloride, efflux pump genes