Clear Sky Science · en
c-MYC enhances transcription of the type 1 diabetes mellitus associated gene BATF3 via promoter binding
Why this research matters to families
Type 1 diabetes in children arises when the immune system mistakenly destroys the insulin-making cells of the pancreas. Insulin therapy keeps children alive but does not cure the disease or stop long term complications. This study looks inside immune cells to understand what drives them to attack, focusing on a pair of molecular switches called c-MYC and BATF3. By mapping how these switches interact, the researchers hope to point the way toward better markers for disease activity and, in time, more precise treatments.
A closer look at an overactive immune army
In type 1 diabetes, certain white blood cells known as T cells play a central role in harming the pancreas. The team concentrated on CD8 T cells, a subset that can directly kill other cells. Earlier work in mice suggested that a protein called BATF3 helps shape immune cells that trigger diabetes. Here, the scientists asked whether BATF3, and the factors that control it, are altered in children with the disease. They analyzed blood samples from young patients and healthy peers, and combined these measurements with large public gene expression databases.
Finding the key molecular switches
Using computer based screening of thousands of genes, the researchers narrowed in on four potential regulators that might switch on BATF3. Among these, c-MYC stood out. Both c-MYC and BATF3 were present at higher levels in blood immune cells from children with type 1 diabetes than in those from healthy children, while another candidate, EGR1, was reduced. These patterns suggest that a c-MYC to BATF3 chain of events is active in the immune systems of affected children and may reflect their ongoing autoimmune response.
How c-MYC turns up BATF3
To test whether c-MYC truly controls BATF3, the team moved into cell culture experiments. They inserted extra copies of the c-MYC gene into human kidney cells commonly used in the lab and watched what happened. When c-MYC levels rose, BATF3 levels rose as well, both at the RNA and protein stages. When c-MYC was dialed down with small interfering RNA, BATF3 dropped. The scientists then examined the BATF3 gene’s control region and showed that c-MYC binds to a specific stretch of DNA about 1.2 thousand bases upstream of where BATF3 is read, acting like a finger pressing on a molecular light switch.
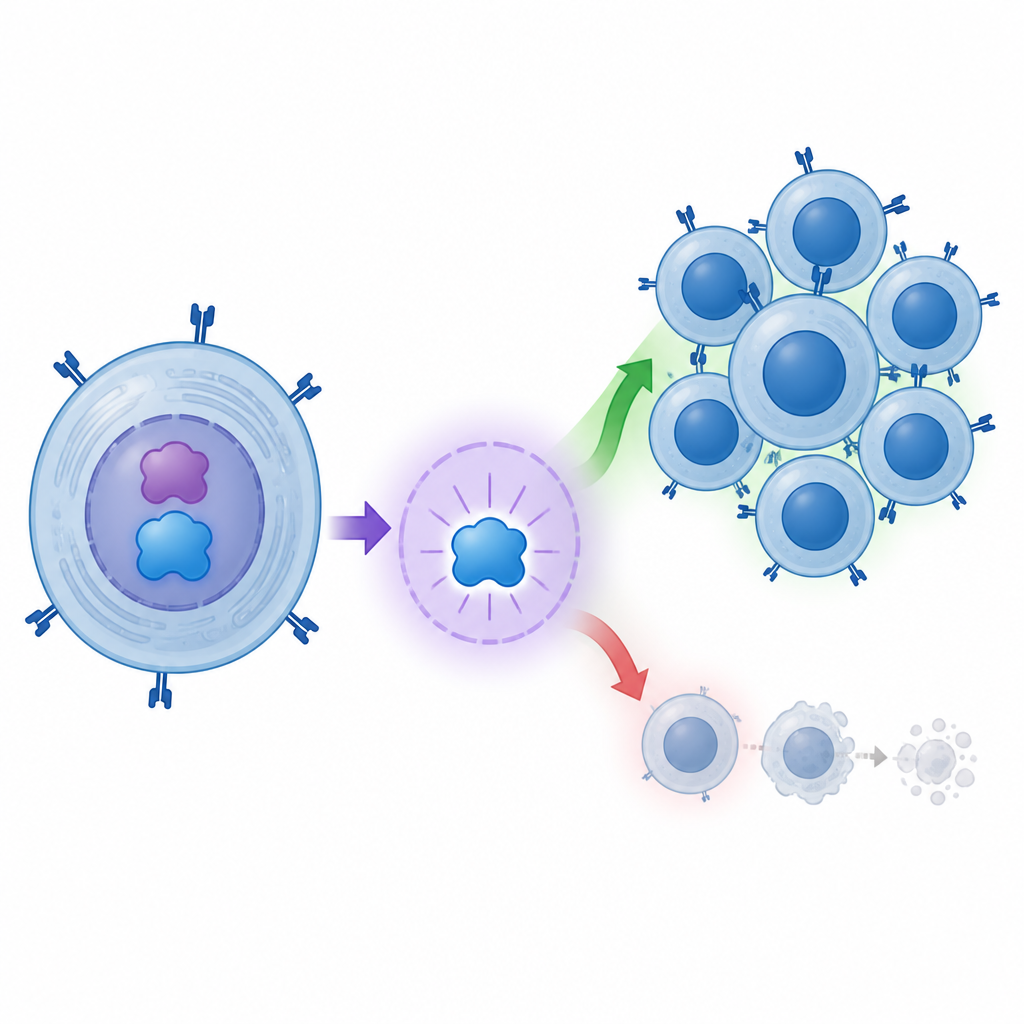
Impact on killer T cells
The story does not stop at molecules. The group also studied human CD8 T cells grown from blood. When they boosted c-MYC in these cells, the cells divided more and died less. In other words, c-MYC helped expand the pool of potentially harmful T cells. Because BATF3 is one of the main targets that c-MYC activates, the work outlines a chain that runs from c-MYC to BATF3 to stronger, longer lived CD8 T cells. This fits with the idea that a sustained, aggressive immune attack helps drive the loss of insulin producing cells in children with type 1 diabetes.
What this means for future care
The authors conclude that an overactive c-MYC–BATF3 pathway is likely part of the machinery that fuels type 1 diabetes in children. Their data do not yet prove that blocking this pathway will halt the disease, and directly shutting down c-MYC could be unsafe because it is important for many normal processes. Still, measuring c-MYC and BATF3 activity in blood might help track how the disease is unfolding or how a child responds to new immune therapies. In the longer term, targeting steps around this pathway, rather than the switches themselves, could offer new strategies to tame the immune system while preserving its vital protective roles.
Citation: Zhao, Y., Tang, Z., Tao, Y. et al. c-MYC enhances transcription of the type 1 diabetes mellitus associated gene BATF3 via promoter binding. Sci Rep 16, 14976 (2026). https://doi.org/10.1038/s41598-026-45579-x
Keywords: type 1 diabetes, c-MYC, BATF3, CD8 T cells, autoimmunity