Clear Sky Science · en
TRIM29 promotes epithelial–mesenchymal transition, angiogenesis, and stromal remodeling in lung adenocarcinoma: integrated validation at histologic, transcriptomic, and protein levels
Why this lung cancer study matters
Lung cancer is still one of the top causes of cancer death, and many patients do not benefit from today’s targeted drugs or immunotherapies. This study looks at a little-known protein called TRIM29 and asks a big question: does it help lung tumors become more aggressive and harder to treat? By tying together genetic data, microscope images of real tumors, cell experiments, and drug screens, the researchers show that TRIM29 marks—and may help drive—a more dangerous form of lung adenocarcinoma, the most common type of lung cancer.
A hidden helper of tumor spread
Our organs are built from orderly sheets of cells that stay in place. Cancer becomes deadly when these cells loosen their bonds, change shape, and start to migrate—a process often called a cell “identity switch.” The authors found that lung tumors with high levels of TRIM29 were strongly linked to this switch-like behavior. By analyzing large public datasets of tumor RNA, they showed that TRIM29-rich cancers were enriched for gene programs associated with cells losing their stable, epithelial traits and gaining more mobile, invasive ones. Patients whose tumors had more TRIM29 tended to live for a shorter time, suggesting that this protein is a marker of poor prognosis.
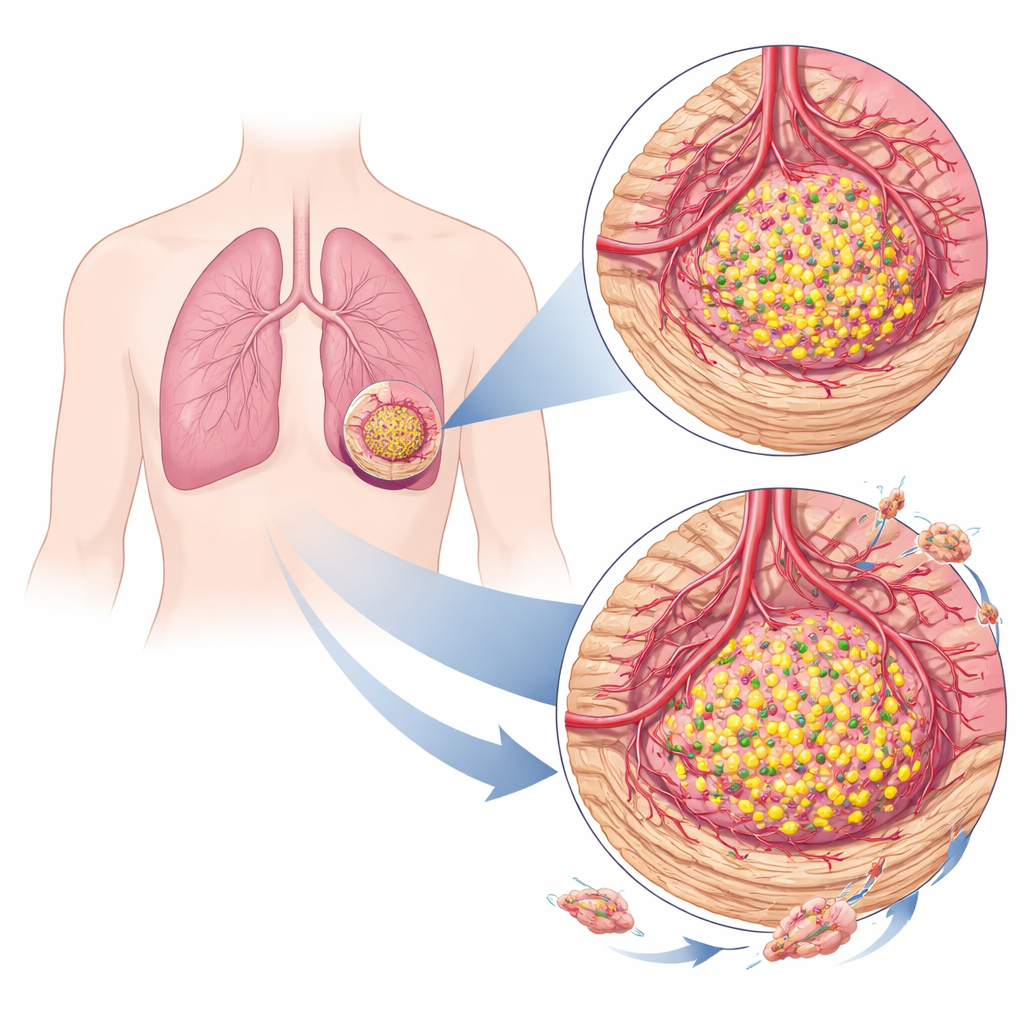
Shaping the tumor’s neighborhood
Tumors do not grow alone; they recruit blood vessels and supporting cells, and they remodel the tissue around them. Using computational tools that tease apart the mix of cells in bulk tumor samples, the team found that TRIM29-high lung tumors sat in a very different neighborhood from TRIM29-low tumors. Cancers rich in this protein tended to have more fibroblasts—cells that lay down scar-like tissue—and more endothelial cells, which line blood vessels. These tumors scored higher for “stromal” and “microenvironment” signals, indicating a thicker, more reactive supporting tissue and richer blood supply, both of which can foster tumor growth and spread.
Seeing the signals under the microscope
To move beyond computer predictions, the researchers examined tumor samples from 200 lung adenocarcinoma patients treated at a single hospital. They stained the tissues for TRIM29, key regulators of the cell identity switch (SNAIL and TWIST), small blood vessels, and the proportion of supportive tissue versus cancer cells. Tumors with higher TRIM29 showed more SNAIL and TWIST, denser networks of tiny blood vessels, and a larger stromal area, confirming that TRIM29 is tied to a blood vessel–rich, scar-like environment. Interestingly, classic end-stage markers of the cell switch, such as E-cadherin loss and vimentin gain, did not correlate as strongly, hinting that many tumors may sit in a “partial” transition state that is hard to capture with simple markers.
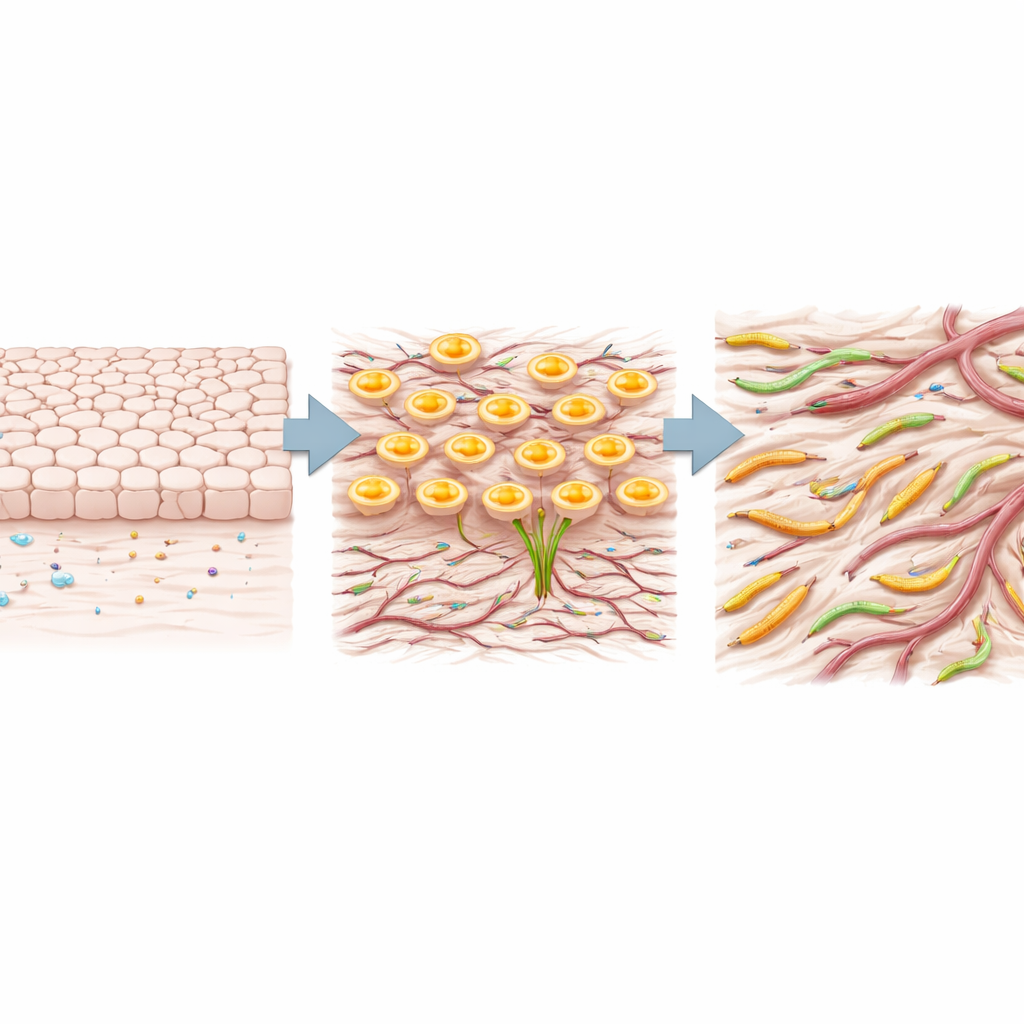
Testing TRIM29’s role in cancer cells and drugs
The team then asked whether TRIM29 is just a passenger or an active driver in cancer cells. In two lung adenocarcinoma cell lines, they used small RNA molecules to knock down TRIM29. When TRIM29 was reduced, the cells dialed down SNAIL and TWIST, increased the adhesion molecule E-cadherin, lowered N-cadherin, and migrated more slowly in wound-healing assays. These changes are consistent with cells reverting toward a more settled, less invasive state. Finally, by mining large drug response databases, the researchers looked for compounds that were especially effective in cell lines with high TRIM29. A clear pattern emerged: several inhibitors of mTOR, a major growth and survival pathway, were more active in TRIM29-high cells, pointing to a possible weak spot in these aggressive tumors.
What this means for patients
Taken together, the study paints TRIM29 as a hub connecting cell identity changes, blood vessel growth, and tissue remodeling in lung adenocarcinoma—and as a marker of worse outcomes. While more work in animals and clinical trials is needed, the findings suggest that measuring TRIM29 could help flag patients with particularly aggressive disease and that mTOR-blocking drugs might be especially useful for this group. In the long run, targeting TRIM29 itself, or the way it reshapes the tumor’s neighborhood, could open new paths to slow or stop the spread of this common and deadly cancer type.
Citation: Hwang, Y., Han, JH., Haam, S. et al. TRIM29 promotes epithelial–mesenchymal transition, angiogenesis, and stromal remodeling in lung adenocarcinoma: integrated validation at histologic, transcriptomic, and protein levels. Sci Rep 16, 14505 (2026). https://doi.org/10.1038/s41598-026-45469-2
Keywords: lung adenocarcinoma, TRIM29, tumor microenvironment, epithelial mesenchymal transition, mTOR inhibitors