Clear Sky Science · en
Rosmarinic acid alleviates bleomycin-induced pulmonary fibrosis in mice by activating the Rap1 pathway
Why this matters for people with lung scarring
Pulmonary fibrosis is a serious lung disease where normal, springy lung tissue is slowly replaced by stiff scar tissue, making every breath a struggle. Current medicines can slow this process but often come with unpleasant side effects and do not fully stop the damage. This study explores whether a natural compound called rosmarinic acid, found in familiar herbs like rosemary and lemon balm, might help protect lungs from scarring in a widely used mouse model of the disease.
A common cancer drug and an unwanted side effect
To study lung scarring in the lab, researchers often rely on bleomycin, a chemotherapy drug known to damage the lungs as a side effect. When given directly into the windpipe of mice, bleomycin triggers inflammation and thick bands of scar tissue similar to those seen in pulmonary fibrosis. In this study, scientists first created this condition in mice and then waited three days to mimic an early treatment window. From that point, they gave the animals rosmarinic acid by mouth every day for 25 days at three different doses, or treated them with pirfenidone, one of the standard antifibrotic drugs used in people. This setup allowed the team to compare how well the herbal compound stacked up against an approved medicine.
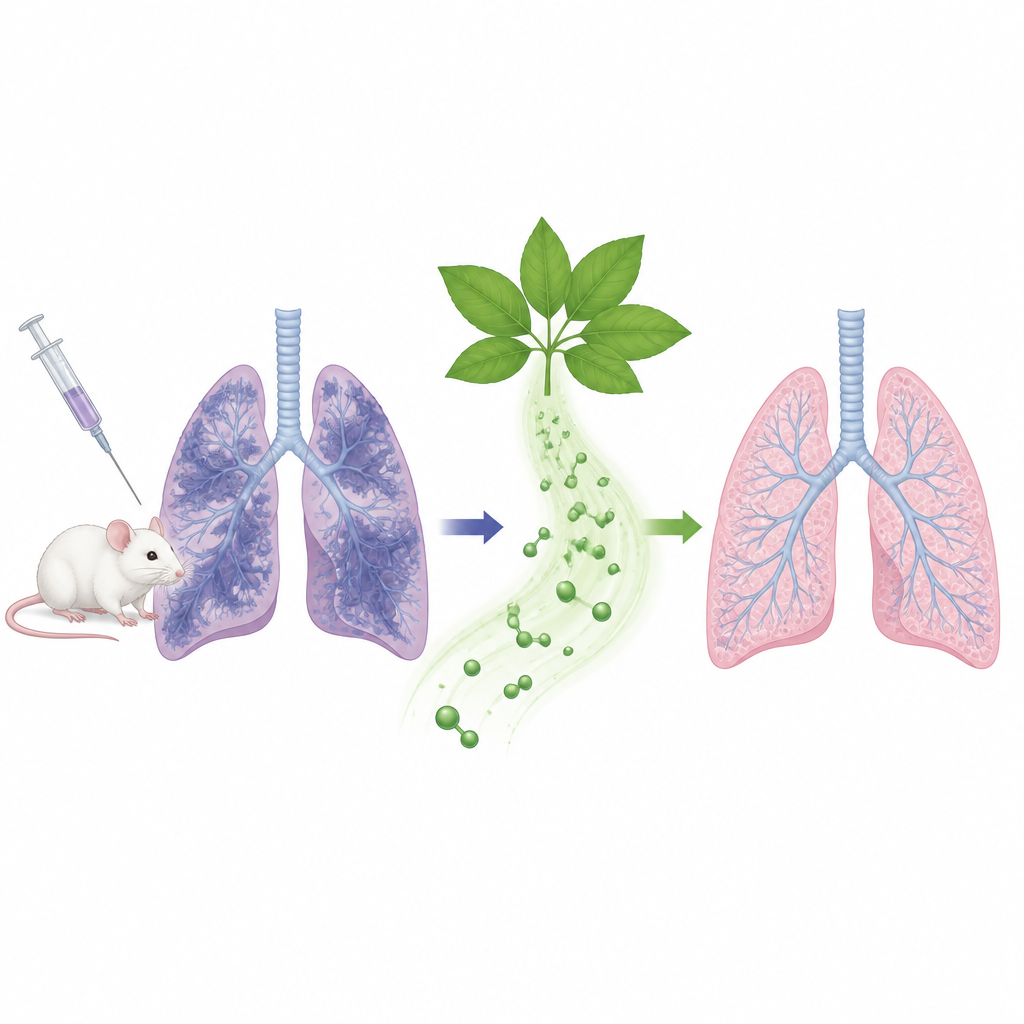
Seeing and measuring how the lungs respond
The team used medical imaging and lung function tests similar to those used in human clinics. Small-animal CT scans showed that bleomycin filled the mouse lungs with dense, patchy areas that look like fibrous cords or solid white patches. In mice given rosmarinic acid, especially at a middle dose of 40 milligrams per kilogram of body weight, these cloudy areas shrank, and the lungs looked more open and airy. Positron emission tomography, which tracks sugar use as a sign of inflammation, showed that bleomycin made the lungs highly active, while rosmarinic acid and pirfenidone both brought this signal back down. Breathing measurements confirmed the picture: volumes of air the mice could inhale and exhale, and how quickly they could move air, all dropped after bleomycin but improved after treatment with rosmarinic acid or pirfenidone.
Calming inflammation and limiting scar formation
Beyond images and breathing tests, the researchers examined the lung tissues and the immune response more closely. Bleomycin flooded the air spaces with white blood cells, including neutrophils and other inflammatory cells, and raised levels of well-known alarm signals such as IL-1β, IL-6, TNF-α, and TGF-β1 in lung fluid and blood. Rosmarinic acid treatment reduced these cells and signaling molecules, suggesting a calmer immune environment. Staining of lung sections revealed that bleomycin thickened the delicate walls of the air sacs and filled the spaces between them with blue collagen fibers, a hallmark of scarring. Rosmarinic acid at 40 and 80 milligrams per kilogram, and pirfenidone, all cut down both the overall inflammation score and the area covered by collagen, while the lowest dose of rosmarinic acid was less effective.
Digging into the cells’ control circuits
To understand how this plant compound was working inside the lungs, the team turned to a broad protein survey known as label-free quantitative proteomics. Comparing healthy, bleomycin-treated, and rosmarinic acid-treated mice, they identified hundreds of proteins whose levels changed with disease and were partially restored by treatment. Computer analysis of these protein shifts pointed to several signaling routes inside cells, with a pathway called Rap1 standing out. Within this pathway, four proteins involved in cell survival, growth, and attachment to their surroundings — FGF1, c-Kit, Kras, and Src — were sharply reduced after bleomycin but rose again when mice received rosmarinic acid. Follow-up tests using Western blotting and tissue staining confirmed these changes, and computer docking simulations suggested that rosmarinic acid can bind to these proteins in ways that are physically plausible.
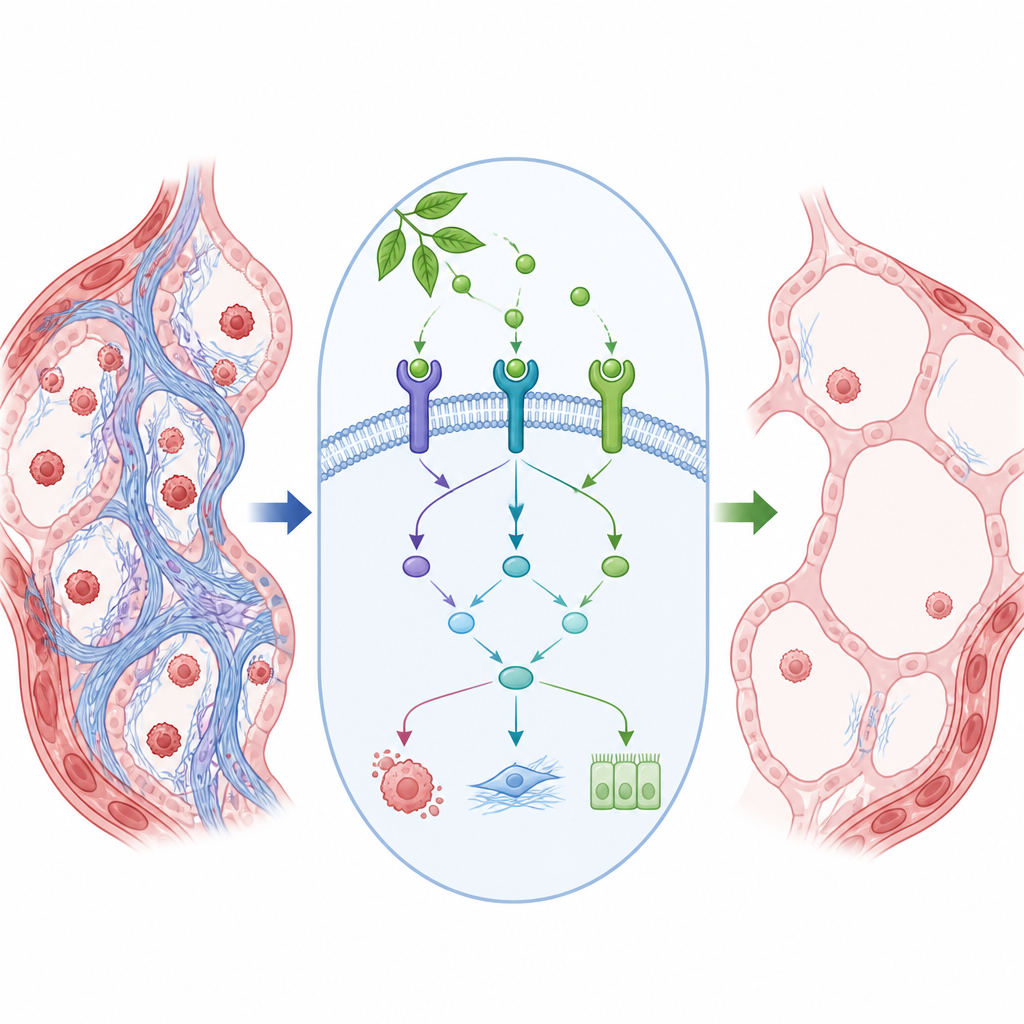
What this could mean for future treatments
In simple terms, the study suggests that rosmarinic acid helps damaged lungs in mice breathe more easily by easing inflammation and slowing the buildup of scar tissue. It appears to do this, at least in part, by nudging a cell signaling route, the Rap1 pathway, back toward a healthier state and boosting key proteins that support repair. While these findings do not yet show how rosmarinic acid will behave in people, and more work is needed to test safety, dosing, and long-term effects, the results add weight to the idea that certain plant-derived compounds can work alongside or one day complement existing drugs for lung fibrosis.
Citation: Gul, A., Zhong, Y., Aili, M. et al. Rosmarinic acid alleviates bleomycin-induced pulmonary fibrosis in mice by activating the Rap1 pathway. Sci Rep 16, 14995 (2026). https://doi.org/10.1038/s41598-026-45457-6
Keywords: pulmonary fibrosis, rosmarinic acid, bleomycin, Rap1 pathway, lung inflammation