Clear Sky Science · en
Junction opener enables CAR T cell treatment of solid tumors
Breaking Down Cancer’s Hidden Walls
Many of the most dangerous cancers form solid lumps deep inside the body, where powerful new immune therapies often struggle to reach. This study explores a clever way to temporarily “unzip” the tight seams between tumor cells so that cancer-fighting immune cells, known as CAR T cells, can finally get inside and do their job. The work suggests a strategy that could make a promising class of therapies, currently successful mainly in blood cancers, far more effective against common solid tumors.
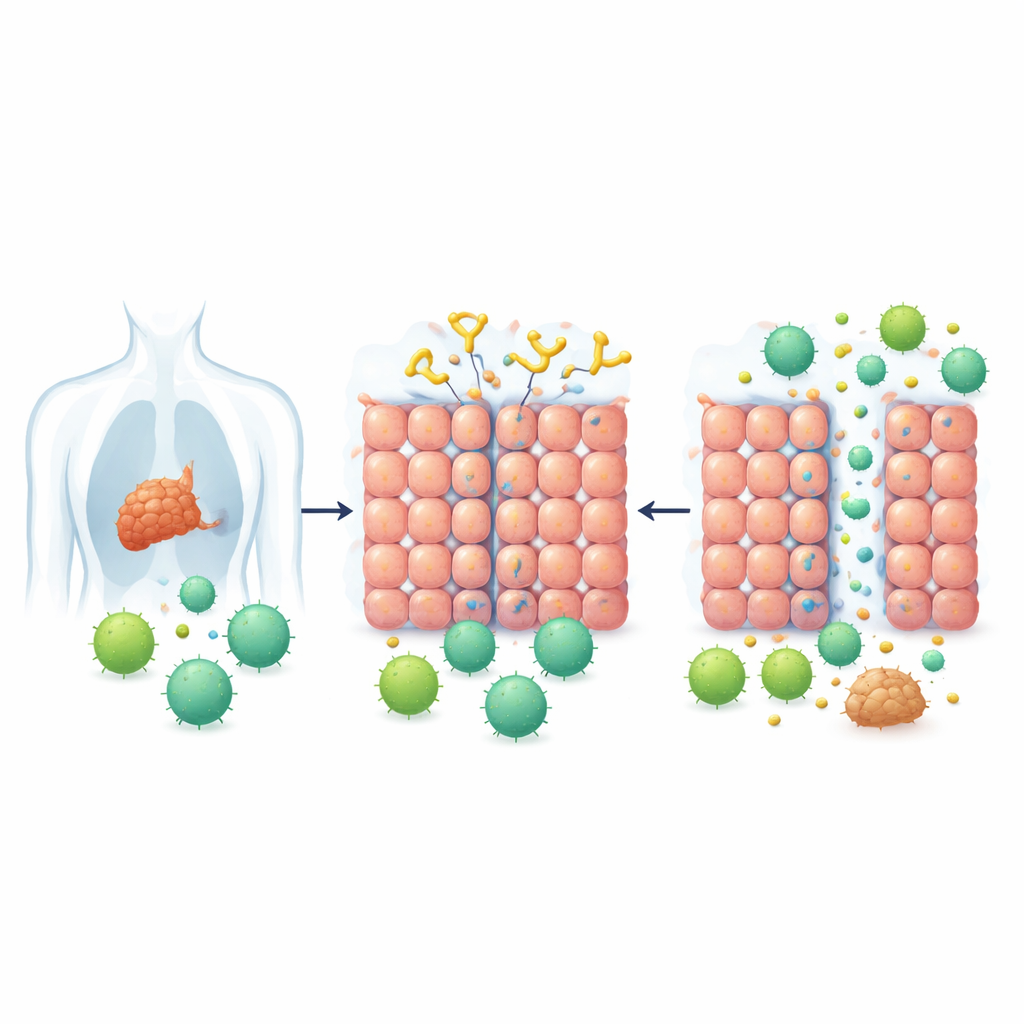
Why Some Tumors Keep Treatments Out
Solid tumors don’t just grow; they also build defenses. One of the most important defenses is a layer of tightly connected cells that form a kind of biological brick wall. These cell–cell connections, or junctions, are especially strong in many cancers that arise from epithelial tissues, such as breast, lung, skin, cervical, and colon cancers. A protein called desmoglein 2 (DSG2) helps lock these junctions together. High levels of DSG2 are common in several tumor types and are linked with resistance to treatment, making tumors harder for both drugs and immune cells to penetrate.
A Keyhole Opened by a Viral-Inspired Tool
Inspired by how certain cold-like viruses slip between cells, researchers previously designed a series of proteins called Junction Openers. These proteins bind DSG2 and briefly loosen the junctions between cells. In this study, the team focused on an improved version called JO-4, which has a much stronger grip on DSG2 and had already shown good safety and tumor-targeting behavior in animal tests. The central idea was straightforward: if JO-4 could crack open the junctions in solid tumors for a short time, then CAR T cells—engineered immune cells that recognize a specific cancer marker—might finally be able to enter the tumor mass in large numbers.
Testing the Idea in Mini-Tumors and Mice
To model real tumors, the scientists grew breast cancer cells into three-dimensional spheroids, tiny balls of cells that naturally form tight junctions like those in human tumors. They used CAR T cells designed to recognize HER2, a protein found at high levels on these cancer cells. When the spheroids were pretreated with JO-4, HER2-targeted CAR T cells infiltrated much more deeply and in greater numbers than without JO-4, while off-target CAR T cells that did not recognize HER2 showed no such benefit. Importantly, JO-4 by itself did not kill tumor cells or boost CAR T activity on flat cell layers lacking tight junctions, indicating that its main effect was to open physical barriers rather than to directly poison cells or generally overstimulate T cells.
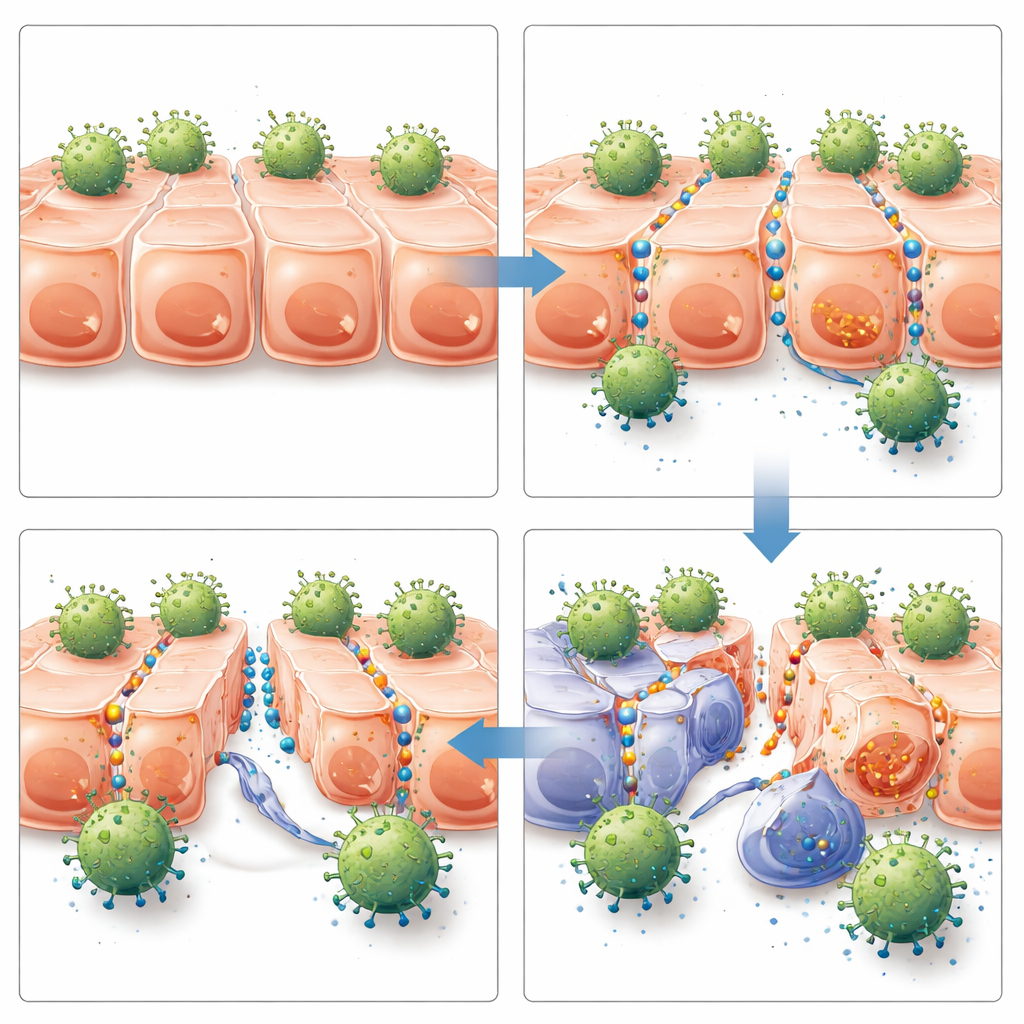
From Better Access to Better Tumor Control
The next question was whether this improved access would matter in living animals. The team implanted human breast and ovarian tumor cells into immune-deficient mice to form solid tumors. After tumors reached a measurable size, the mice received either HER2-specific CAR T cells, off-target CAR T cells, or no CAR T cells—combined with JO-4 or control treatments. Only the combination of HER2-directed CAR T cells plus JO-4 produced strong and lasting control of tumor growth in both cancer models. Mice given this combination had more CAR T cells inside their tumors, higher signs of T cell activation in the tumor but not in the spleen, slower tumor growth, and significantly longer survival. JO-4 alone, or partnered with off-target CAR T cells, did not provide meaningful benefit, reinforcing that the effect depended on targeted immune attack once the junctions were opened.
What This Could Mean for Future Cancer Care
Together, the findings show that temporarily loosening the seams between tumor cells can transform how well CAR T cells work against solid tumors. By allowing targeted CAR T cells to flood into the tumor core and stay active there, JO-4 combination therapy improved tumor destruction and survival in animal models. If similar results hold in humans, this approach could reduce the doses of CAR T cells needed, shorten complex manufacturing steps, and possibly work alongside other immunotherapies such as checkpoint inhibitors. In simple terms, the study suggests that opening the physical doors of a tumor may be just as important as arming the immune system to fight it.
Citation: Reed, S.J., Sharma, S., Novák, C. et al. Junction opener enables CAR T cell treatment of solid tumors. Sci Rep 16, 12529 (2026). https://doi.org/10.1038/s41598-026-43093-8
Keywords: CAR T cells, solid tumors, tumor barriers, junction opener, cancer immunotherapy