Clear Sky Science · en
Serum CD73 activity as a biomarker of hypoxemia in COVID-19 patients
Why this matters for people with COVID-19
When someone with COVID-19 comes to the emergency room, doctors must quickly decide who will need extra oxygen, intensive care, or powerful anti-inflammatory drugs. This study explores whether a substance in the blood called CD73, which helps control both oxygen stress and inflammation, could act as a simple blood test to flag which patients are at highest risk for breathing problems and poor outcomes.
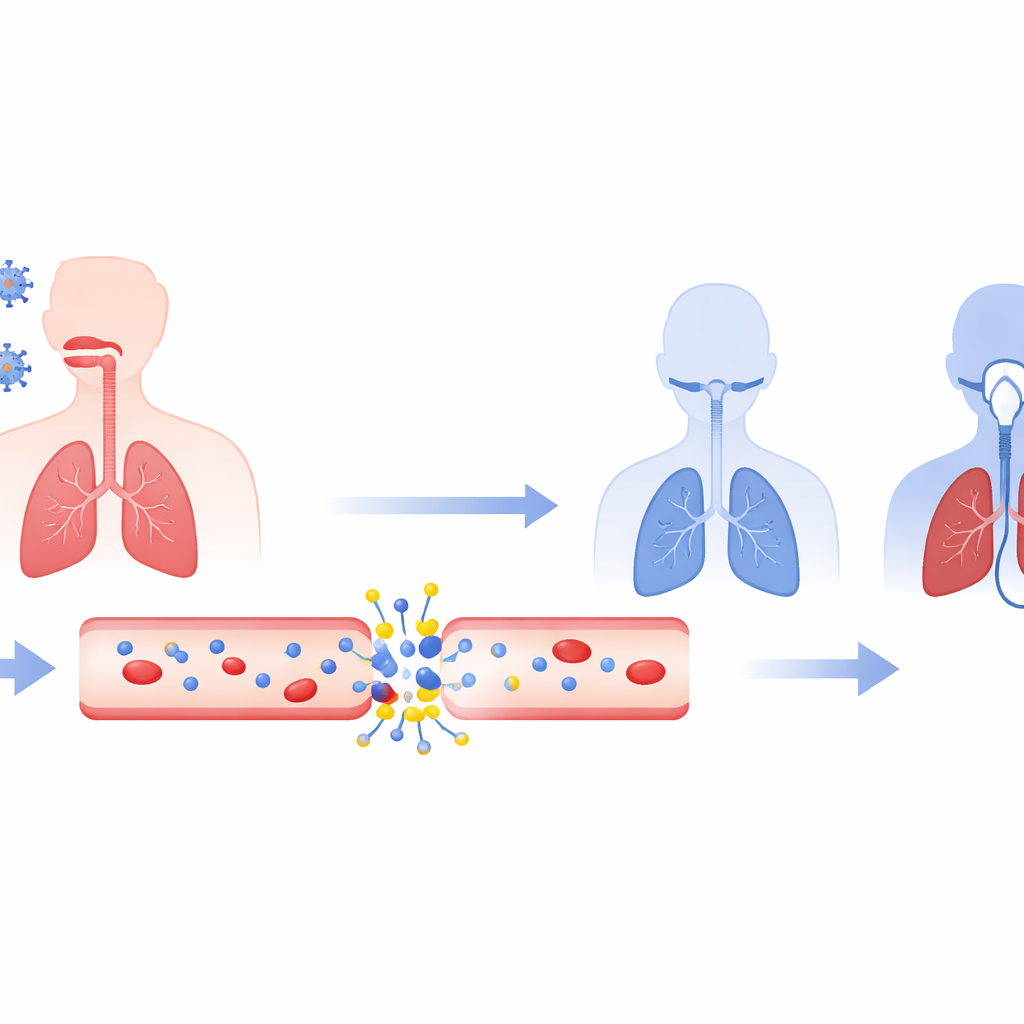
A blood signal linked to oxygen shortage
The researchers followed 85 patients with confirmed COVID-19 during the second and third waves of the pandemic in France, along with 30 healthy volunteers. Patients were grouped as having mild to moderate illness or severe to critical illness, based on World Health Organization criteria. Blood samples were taken on days 1, 3, and 7 after arrival in the emergency department. The team measured the activity of two enzymes in the blood, CD39 and CD73, that together transform danger signals released by damaged cells into a calming molecule that can ease inflammation, relax blood vessels, and help protect tissues.
What the study found in COVID-19 patients
Compared with healthy volunteers, people with COVID-19 had much higher blood CD73 activity, while CD39 showed no clear pattern and was often too low to measure. CD73 levels were especially high in patients who arrived with clear signs of low blood oxygen, such as fast breathing or a need for at least 6 liters of oxygen per minute. Patients who needed oxygen for many days tended to have higher CD73 activity, and in those admitted to intensive care, higher CD73 by the end of the first week was linked with a shorter stay. These patterns suggest that CD73 rises as the body responds to oxygen shortage, possibly to boost production of protective molecules in the lungs and blood vessels.
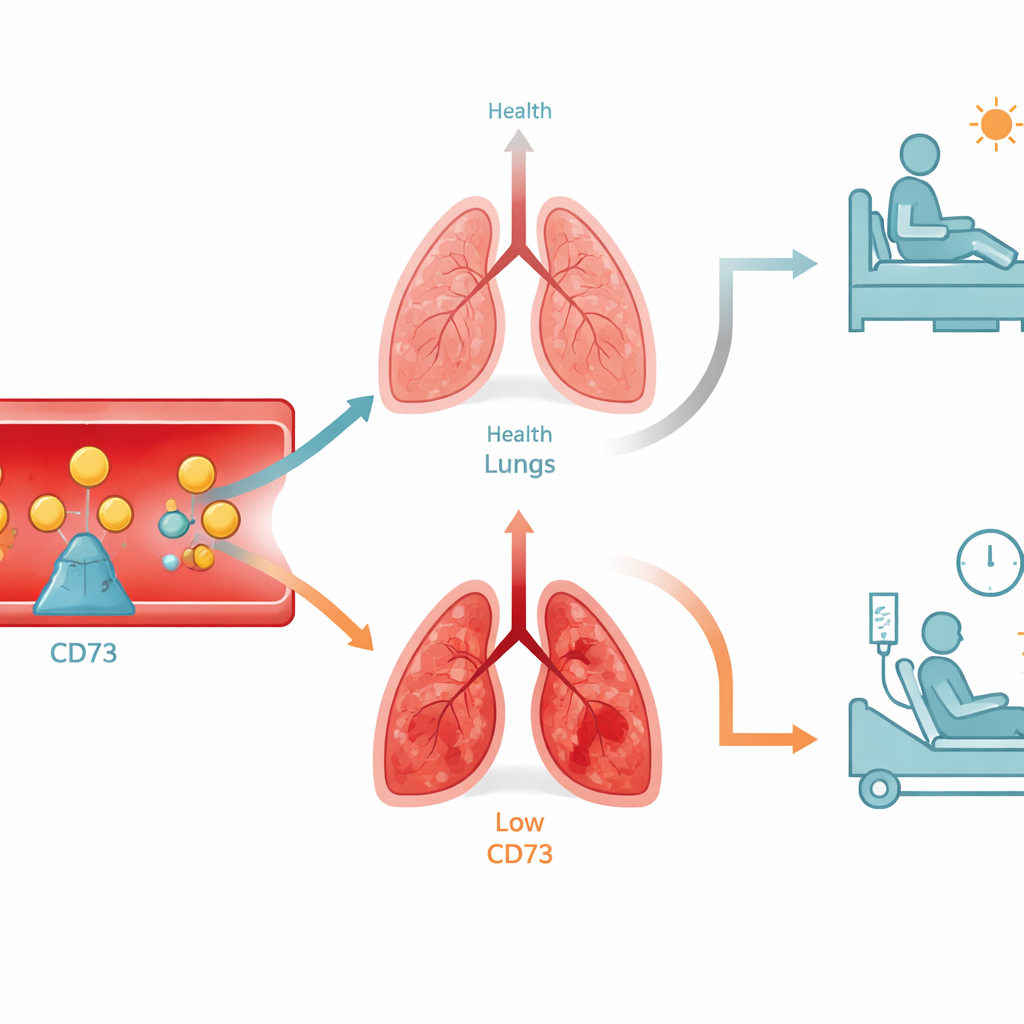
When inflammation overwhelms the system
The story changed in patients whose main problem was intense inflammation rather than oxygen shortage. Those who arrived with high fever and very elevated C-reactive protein, a standard marker of inflammation, had lower CD73 activity from day 1, and it stayed low over the week. Patients who died early or required extremely long hospital stays also showed some of the lowest and most stable CD73 levels. Instead of a strong rise that might help limit tissue damage, their blood signal looked blunted, as if this protective pathway was exhausted or shut down in the face of ongoing inflammation.
Why CD39 did not help doctors much
In contrast to CD73, CD39 activity in the blood was often undetectable and did not differ between healthy people and any group of COVID-19 patients. It also failed to track with key clinical signs such as oxygen needs, length of stay, or risk of death. This suggests that measuring the circulating activity of CD39, at least with the methods used here, does not capture the complex changes happening on the surfaces of immune and blood vessel cells during COVID-19 and is not useful as a bedside marker of severity.
What this could mean for future care
To a layperson, the main message is that CD73 behaves like a dynamic gauge of how the body is coping with COVID-19. When lungs are starved of oxygen, CD73 tends to rise, reflecting an active attempt to protect tissues. When runaway inflammation dominates, CD73 stays low, and patients are more likely to fare poorly. Although this test is not yet ready for routine use, the findings support CD73 as a promising blood marker that could one day help emergency teams separate patients who mainly need support for breathing from those at risk of dangerous inflammation, and guide more tailored treatment in COVID-19 and possibly other severe infections.
Citation: Le Borgne, P., Bilbault, P., Clere-Jehl, R. et al. Serum CD73 activity as a biomarker of hypoxemia in COVID-19 patients. Sci Rep 16, 11080 (2026). https://doi.org/10.1038/s41598-026-41023-2
Keywords: COVID-19 biomarkers, hypoxemia, CD73, inflammation, critical care