Clear Sky Science · en
RASIP1-positive TECs in pancreatic adenocarcinoma: a potential novel type of endothelial cells correlated with “hot” tumors
Why Blood Vessels Matter in Pancreatic Cancer
Pancreatic cancer is one of the deadliest cancers, in part because the body’s own immune defenses struggle to reach and attack the tumor. Unlike some cancers that are packed with immune cells and respond well to modern immunotherapies, many pancreatic tumors are “cold” — poor in helpful T cells. This study explores an unexpected ally inside the tumor’s own blood vessels: a special type of vessel-lining cell that seems to invite cancer-fighting T cells in, potentially helping turn a “cold” tumor into a “hot” one that is easier to treat.
A Closer Look at Tumor Blood Vessels
Blood vessels are more than simple pipes. They are lined by endothelial cells that decide what enters and leaves the bloodstream, including immune cells. Pancreatic tumors are usually poorly supplied with blood vessels, creating a barrier to both drugs and immune cells. Using advanced single-cell RNA sequencing — a technique that reads out the activity of individual cells — the researchers mapped many cell types inside pancreatic tumors. They confirmed that normal, healthy vessel cells become rarer as the cancer progresses, while the remaining tumor-associated endothelial cells change their behavior and gene activity.
Discovering a Helpful Vessel Cell Type
Among these tumor blood vessel cells, the team identified a distinct subgroup marked by high levels of a protein called RASIP1. These RASIP1-positive tumor endothelial cells had a very different gene signature from other vessel cells. They were enriched in genes involved in helping white blood cells cross the vessel wall — a critical step that lets T cells leave the bloodstream and enter the tumor. Patients whose tumors had higher RASIP1 expression in endothelial cells tended to live longer, and this signal did not simply reflect how advanced their cancer was, suggesting that this special vessel state itself may be beneficial.
Linking Special Vessels to Immune “Hot Spots”
To see where these cells sit in real tumors, the researchers used spatial transcriptomics, a technology that shows which genes are active in precise locations on a tissue slice. Spots rich in RASIP1-positive endothelial cells overlapped with regions showing strong signals from active T cells and interferon-gamma, a hallmark molecule of “hot” tumors. In actual patient tissue sections stained under the microscope, blood vessels rich in RASIP1 were surrounded by dense rings of CD8 and Granzyme B–positive cytotoxic T cells, whereas vessels with little RASIP1 had very few nearby immune cells. Analyses across large cancer datasets also linked higher RASIP1 levels to better responses to certain immunotherapies.
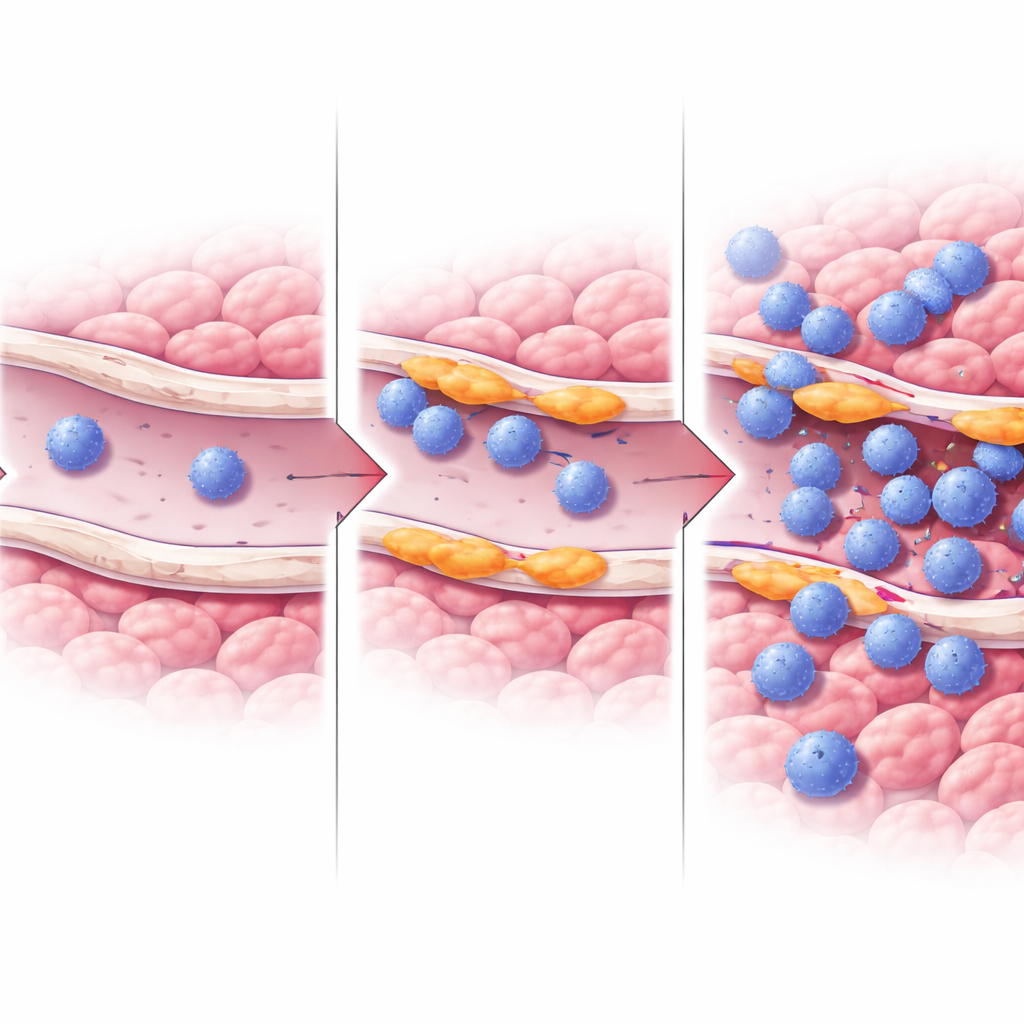
How These Vessels May Help T Cells Enter Tumors
To probe the mechanism, the team turned to cultured human endothelial cells and artificially dialed RASIP1 up or down. When they reduced RASIP1, genes and proteins involved in attracting and gripping immune cells, such as ICAM1 and other junction molecules, went down, and pathways tied to T cell activation and movement were dampened. Overexpressing RASIP1 had the opposite effect, boosting ICAM1. The work also pointed to changes in ERK signaling, a key communication pathway inside cells, as part of how RASIP1 maintains this T cell–friendly vessel state. Together, these experiments support the idea that RASIP1 helps blood vessels form “landing pads” that allow T cells to stick, squeeze through the vessel wall, and accumulate in the tumor.
What This Could Mean for Future Treatments
In simple terms, this study suggests that not all tumor blood vessels are bad. A specific subset, marked by RASIP1, appears to act as a gateway that lets cancer-killing T cells into pancreatic tumors, and patients with more of these gateway vessels seem to fare better. While more work in animal models and direct functional tests is needed, the findings raise an intriguing possibility: instead of only trying to cut off a tumor’s blood supply, future therapies might also aim to nurture or recreate RASIP1-positive vessels to “warm up” pancreatic tumors and make immunotherapies more effective.
Citation: Zhang, S., He, Y., Chang, H. et al. RASIP1-positive TECs in pancreatic adenocarcinoma: a potential novel type of endothelial cells correlated with “hot” tumors. Sci Rep 16, 11946 (2026). https://doi.org/10.1038/s41598-026-40948-y
Keywords: pancreatic cancer, tumor blood vessels, immunotherapy, T cell infiltration, tumor microenvironment