Clear Sky Science · en
Excessive gamma and beta oscillations in manic states across mood and psychotic disorders
Why racing thoughts matter
Many people with mood or psychotic disorders experience periods when their thoughts speed up, their energy soars, and sleep seems optional. These "high" phases, known as manic states, can be thrilling but also dangerous, leading to risky decisions, strained relationships, and hospitalization. Clinicians currently diagnose and track these states almost entirely through conversation, which can miss subtle warning signs. This study asks a simple but powerful question: can we detect manic states directly from brain activity, across different psychiatric labels such as depression, bipolar disorder, and schizophrenia?
Looking beyond diagnostic labels
Traditional psychiatric diagnoses, like bipolar disorder or schizophrenia, do not always match what patients are actually feeling and doing at a given time. Someone diagnosed with depression may be quietly manic; a person with schizophrenia may be more depressed than psychotic. To cut through this complexity, the researchers pooled 159 adults with schizophrenia spectrum disorders, bipolar disorder, major depression, or no psychiatric history. Rather than sorting people by diagnosis alone, they measured specific symptoms—such as sadness, grandiose ideas, hallucinations, or lack of pleasure—using standard clinical questionnaires and then let a computer search for patterns in these symptom profiles.
Finding hidden symptom patterns
Using unsupervised machine learning, a data-driven clustering method, the team asked the algorithms to group together symptoms that tended to rise and fall in tandem. Out of dozens of questionnaire items, three natural clusters emerged that echoed classic psychiatry: a manic domain (elevated mood, increased energy, impulsivity), a depressive domain (sadness, fatigue, hopelessness), and a psychotic domain (hallucinations, delusions, emotional withdrawal). Next, they used these three domains to sort the patients themselves into four broad "state" groups: manic, depressive, psychotic, and remission (relatively few current symptoms). Importantly, these groups cut across diagnoses: for example, people with bipolar disorder appeared in all four states, and some individuals with schizophrenia landed in the manic group.
Listening to the brain at rest
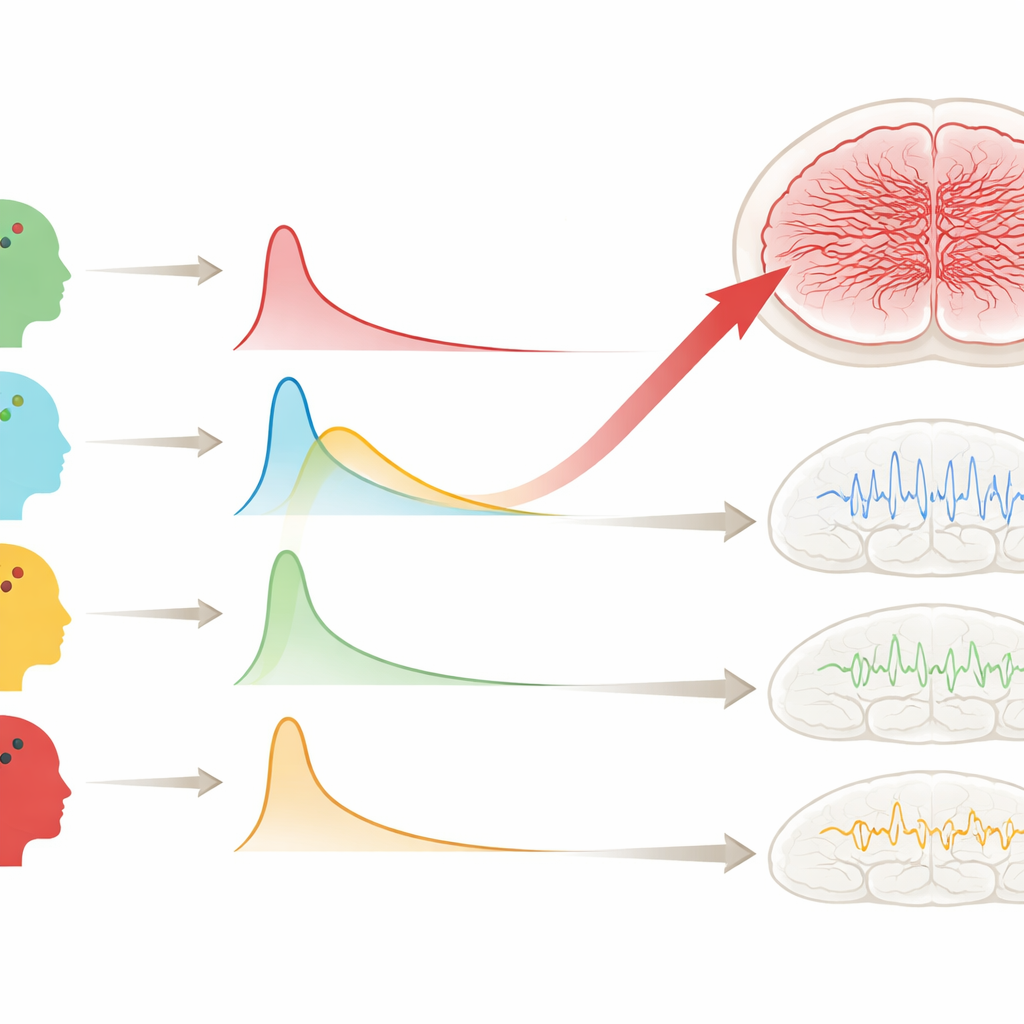
After sorting participants by symptom state, the researchers recorded brain activity using electroencephalography (EEG) from two electrodes over the left and right frontal regions. They collected two kinds of data. First, they measured resting-state activity while participants sat quietly with eyes closed, capturing natural brain rhythms from very slow waves to fast "gamma" waves. Second, they played rapid click sounds at 20 and 40 times per second to trigger so‑called auditory steady-state responses, which reveal how precisely the brain can synchronize to rhythmic sounds. The goal was to see whether any symptom state showed a distinctive electrical signature.
Mania and the fast brain waves
The standout pattern came from people in a manic state. At rest, they showed markedly stronger high‑frequency activity—specifically beta and gamma oscillations—in the frontal electrodes than all other groups, including healthy volunteers, patients in remission, and those in depressive or psychotic states. By contrast, when the brain was challenged with rhythmic sounds, manic patients did not show more precise or stronger responses than others at 20 or 40 clicks per second. In other words, their brains were buzzing with fast activity on their own, but this did not translate into sharper processing of incoming sounds. People in a primarily psychotic state, on the other hand, showed stronger slow "theta" waves, a pattern previously linked to schizophrenia, but without the pronounced high‑frequency boost seen in mania.
What this could mean for care
For a layperson, these findings can be likened to an engine that is revving too high while idling. In manic states, the frontal regions of the brain appear to run at high speed even at rest, generating plenty of fast activity but not necessarily handling outside information more accurately. This overactive yet imprecise pattern could help explain manic features such as pressured speech, racing thoughts, and impulsive actions. If confirmed in larger and more detailed studies, excessive frontal gamma and beta activity could serve as a state-dependent biomarker—a measurable brain signal—that alerts clinicians to emerging mania, even when the formal diagnosis or self-report is unclear. Such a marker might one day help guide earlier intervention and more tailored treatment across mood and psychotic disorders.
Citation: Yanagi, M., Iwasaki, T., Iwamura, Y. et al. Excessive gamma and beta oscillations in manic states across mood and psychotic disorders. Sci Rep 16, 11855 (2026). https://doi.org/10.1038/s41598-026-40673-6
Keywords: manic state, brain waves, EEG, bipolar disorder, psychosis