Clear Sky Science · en
Antisense oligonucleotide-mediated knockdown therapy in two infants with severe KCNT1 epileptic encephalopathy
Why this study matters for families
Some of the most devastating epilepsies begin in the first days of life and do not respond to standard medicines, leaving infants with constant seizures and profound developmental disability. This study explores a highly personalized kind of genetic medicine—an antisense oligonucleotide drug—designed to dial down the activity of a single overactive brain channel in two young girls. It offers a glimpse of how precision therapies might tame otherwise untreatable seizures, while also revealing serious risks that must be understood before such approaches become widely used.
The problem of relentless early-life seizures
Epilepsy of infancy with migrating focal seizures is a rare but extremely severe condition. Babies develop seizures within hours or days of birth, often experiencing dozens every day despite trying many anti-seizure drugs. In about half of these children, the cause is a new mutation in a gene called KCNT1, which encodes a channel that lets potassium ions flow through the membranes of brain cells. The specific mutation studied here, called p.R474H, makes the channels far more active than normal, pushing networks of neurons into a constantly overexcited state. These children typically show almost no developmental progress, have a high risk of early death and currently have no reliably effective treatments.
A gene-targeted drug built in the lab
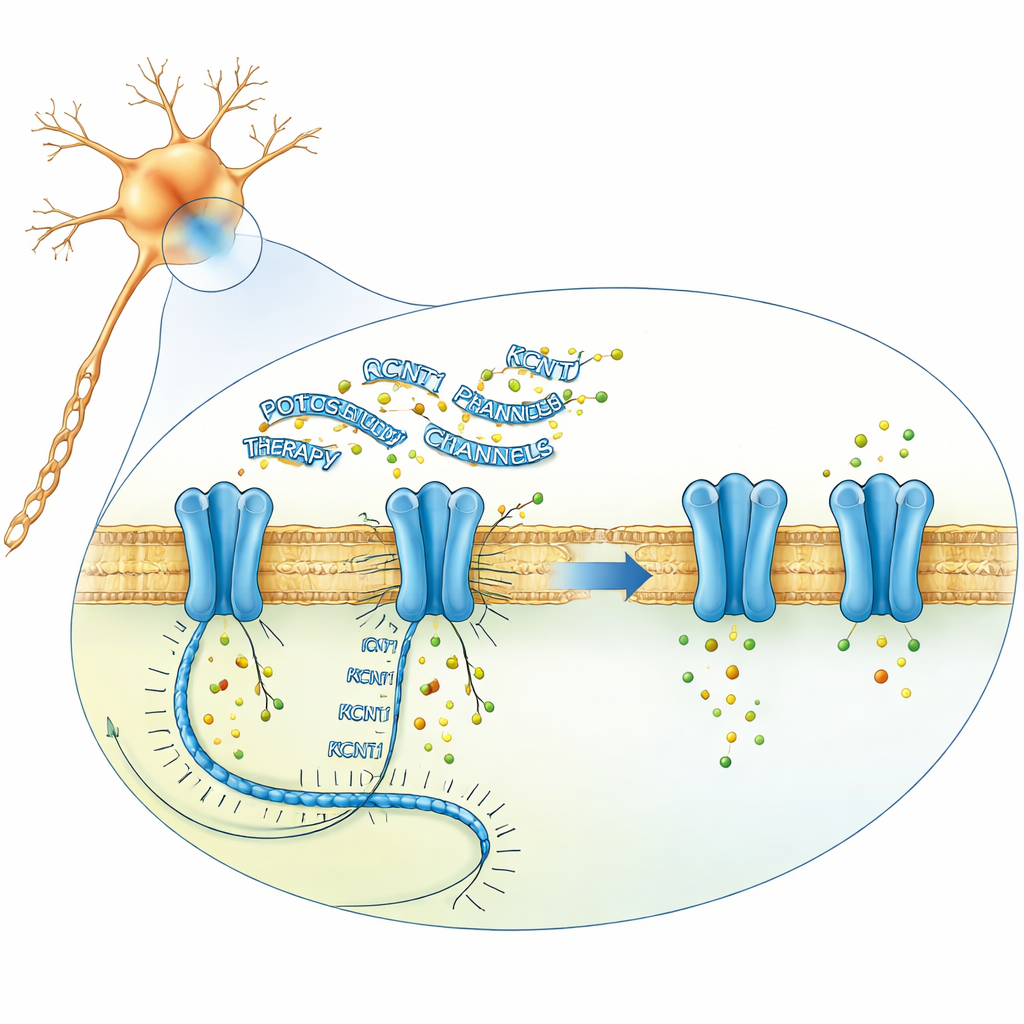
The research team set out to reduce the amount of faulty KCNT1 message inside neurons using antisense oligonucleotides: short, chemically modified strands of genetic material that can bind to a chosen RNA and trigger its destruction. Starting from more than 250 candidate sequences, they progressively narrowed down designs in cultured human nerve-like cells, in neurons grown from patient stem cells and in mouse cells. Their lead compound, later named valeriasen, sharply lowered KCNT1 RNA and protein levels in patient-derived neurons and in a mouse line carrying the corresponding disease mutation, without broadly disturbing other genes. Electrophysiology experiments showed that the drug normalized the abnormally large potassium currents and brought the firing patterns of mutant neurons much closer to those of healthy cells, suggesting that toning down the channel could correct the underlying electrical imbalance.
Testing in animal models before humans
Before considering use in children, the researchers evaluated the drug in several rodent models. In mice engineered to express human KCNT1, injections into the brain fluid reduced both mouse and human KCNT1 RNA in a dose-dependent manner. In a separate mouse strain that naturally develops severe seizures, neurocognitive problems and early death due to a different KCNT1 mutation, treatment with the lead drug extended median lifespan from about six weeks to many months and improved simple behavioral measures such as nest building. Studies in rats using repeated spinal injections helped establish doses that appeared generally tolerated based on behavior, neurological exams and tissue analysis, while still achieving substantial KCNT1 knockdown in brain regions. These findings supported moving forward with cautious, closely monitored use in patients under a special investigational protocol.
Early experience in two children
Two three-year-old girls with the KCNT1 p.R474H mutation, both with seizures from the newborn period and minimal developmental progress, received escalating doses of valeriasen delivered by lumbar puncture into the fluid surrounding the spinal cord. In both, seizure counts recorded by families and confirmed by repeated electroencephalograms fell considerably after several doses, and one child showed improvements in head control, swallowing and ability to self-soothe. The drug levels in spinal fluid and blood behaved as expected from the animal work. However, after months of treatment at relatively high cumulative doses, both children developed a serious complication: progressive enlargement of the brain’s fluid-filled spaces with increased pressure, a form of hydrocephalus. One child’s family chose palliative care, and she later died; the other required a surgically implanted shunt to drain excess fluid.
Balancing promise and risk
Faced with this unexpected side effect, the team paused dosing and carefully reviewed animal and laboratory data. Hydrocephalus had not appeared in mouse models lacking KCNT1 or carrying disease mutations, and genetic surveys suggest that people can tolerate losing one copy of KCNT1, arguing against simple on-target toxicity. Some other antisense drugs used in neurological diseases have been linked to rare cases of raised brain pressure or ventricular enlargement, especially at higher doses, hinting that the issue may stem from how certain compounds interact with the fluid-producing and fluid-draining structures of the brain. After a two-year break, the second patient resumed treatment on a revised, lower-dose schedule with extra MRI scans and pressure checks; under this cautious regimen, she again experienced about a two-thirds reduction in seizures without new fluid buildup so far.
What this means going forward
For families and clinicians confronting catastrophic genetic epilepsies, this work shows that directly quieting an overactive ion channel with a tailored genetic drug can genuinely reduce seizures, even in children who have failed every conventional medication. At the same time, the emergence of hydrocephalus in both treated patients underlines that such powerful therapies can carry serious, still poorly understood risks. The authors conclude that inhibiting the KCNT1 channel is a valid and promising strategy, but that dosing must be approached gradually, with careful brain imaging and clinical monitoring built into future trials. More broadly, the study highlights both the transformative potential and the ethical responsibility that come with designing individualized genetic medicines for some of the sickest patients.
Citation: Nakayama, T., El Achkar, C.M., Burbano, L.E. et al. Antisense oligonucleotide-mediated knockdown therapy in two infants with severe KCNT1 epileptic encephalopathy. Nat Med 32, 1411–1420 (2026). https://doi.org/10.1038/s41591-026-04314-9
Keywords: KCNT1 epilepsy, antisense oligonucleotide, precision medicine, infantile seizures, hydrocephalus