Clear Sky Science · en
Testing an inverse link between limbic alpha-synucleinopathy and myelin markers in mice and humans
Why this matters for brain health
Parkinson’s disease and related “Lewy body” disorders are known for their movement problems, but they also involve subtle changes in brain wiring long before symptoms appear. This study asks a deceptively simple question: are certain vulnerable brain regions hit hard in these diseases because their nerve fibers are poorly insulated by myelin, the fatty coating that helps signals travel quickly? By combining human brain samples with mouse experiments, the researchers test whether having less myelin actually causes more of the harmful protein clumps seen in Parkinson’s-like conditions.
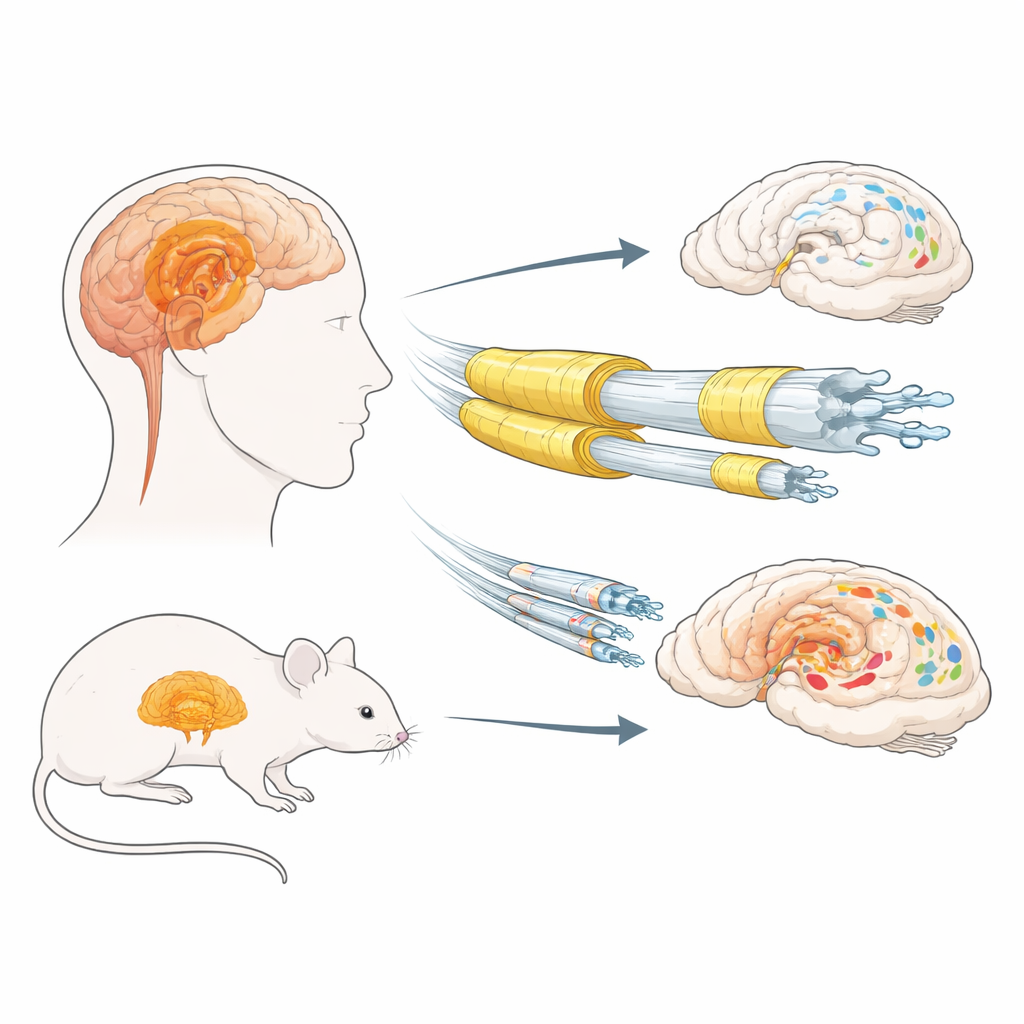
The brain’s insulation and protein clumps
In Lewy body disorders, a normal brain protein called alpha‑synuclein can misfold and pile up inside nerve cells, forming clumps called Lewy bodies and Lewy neurites. Earlier work had suggested that long, thin, poorly myelinated nerve fibers might be especially at risk. Myelin is made by support cells called oligodendrocytes and contains key structural proteins, including myelin basic protein (MBP) and proteolipid protein (PLP). The authors first examined postmortem tissue from the olfactory bulb and amygdala—limbic regions important for smell and emotion—from men and women with and without Lewy body disease. They measured several myelin markers and compared them with levels of insoluble, highly modified (hyperphosphorylated) alpha‑synuclein.
A sex‑linked pattern in human limbic tissue
The human data revealed a striking, sex‑specific pattern. In the amygdala of men with Lewy body disease, higher amounts of insoluble, hyperphosphorylated alpha‑synuclein were linked with lower levels of a particular PLP form (the 20 kilodalton isoform), and there were hints that other myelin‑related genes were also somewhat reduced. This inverse relationship was not seen in women. The findings suggest that, at least in men, worse Lewy‑type pathology in the amygdala tends to accompany weaker myelin signatures. However, these are correlations from end‑stage tissue: they cannot tell whether myelin loss makes alpha‑synuclein pathology worse, or whether the pathology gradually damages myelin.
Putting myelin to the test in mice
To move beyond correlation, the team turned to mouse models that allow myelin to be experimentally disturbed. They injected preformed fibrils of alpha‑synuclein—tiny seeds that trigger Lewy‑like aggregates—into olfactory‑limbic regions of the mouse brain. Some mice were fed cuprizone, a copper‑binding compound that disrupts myelin and causes animals to lose weight; others carried a genetic “shiverer” mutation that halves production of MBP. The idea was simple: if poor myelin truly makes neurons more vulnerable, these manipulations should dramatically amplify the spread of alpha‑synuclein clumps, nerve‑cell damage, and behavioral problems.
Myelin damage gives only a modest push
The results were more muted than expected. Cuprizone clearly reduced key myelin proteins and altered white‑matter structure in male mice, confirming that insulation was compromised. Yet, while fibril injections reliably produced Lewy‑like inclusions in gray‑matter regions, cuprizone only slightly increased the fraction of insoluble alpha‑synuclein that was hyperphosphorylated at one site (serine‑129). Overall amounts of insoluble alpha‑synuclein, measures of neuronal health, and a range of memory, exploration, and smell tests were not robustly worsened by the myelin insult. Similarly, mice with the shiverer mutation—despite having thinner myelin—did not show clear, systematic increases in limbic alpha‑synuclein pathology or in behavioral deficits compared with normal littermates, aside from a small increase in the average size of protein aggregates.
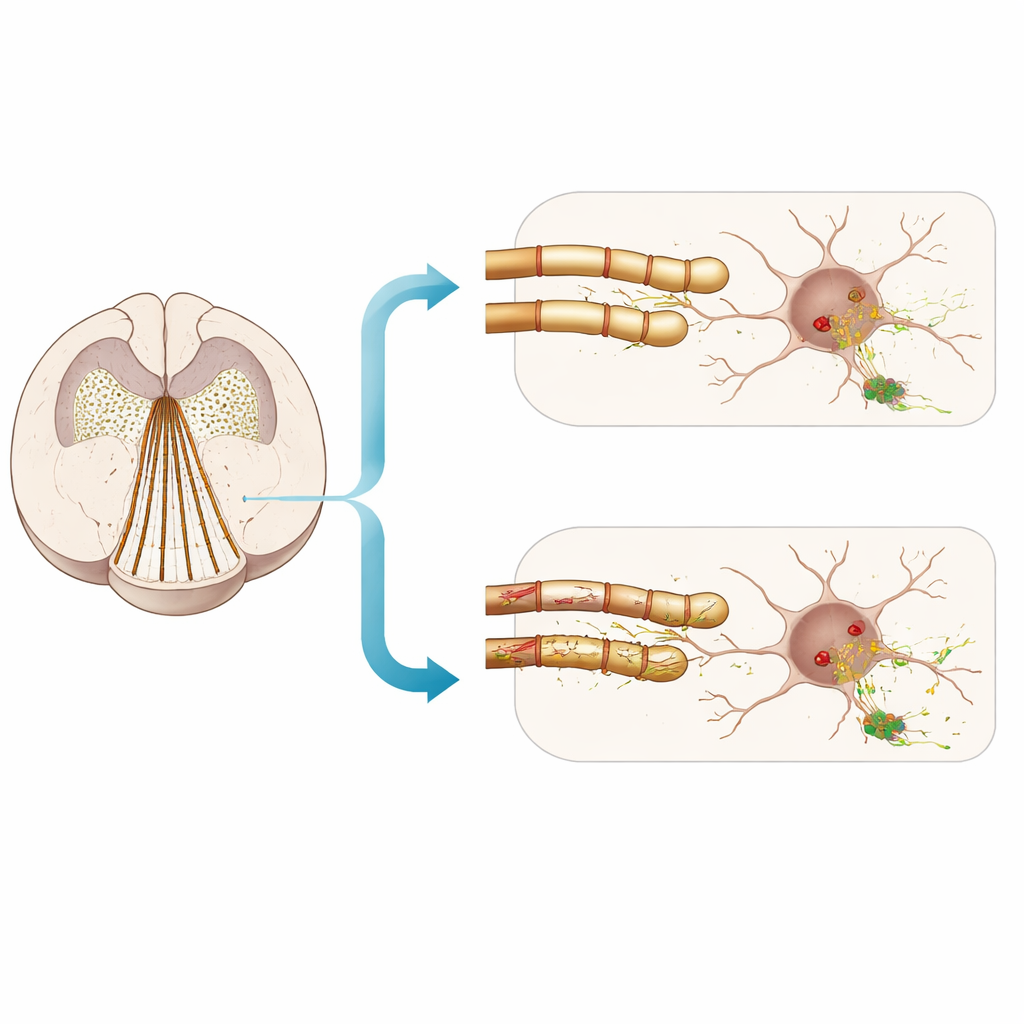
What this means for understanding risk
Taken together, the work supports a nuanced view. In both men with Lewy body disease and in fibril‑seeded mice, weaker myelin markers often accompany heavier alpha‑synuclein loads, especially in limbic areas. But when the researchers deliberately damaged myelin, they saw only modest, inconsistent aggravation of early pathology and no strong evidence of added nerve‑cell loss or major behavioral decline over the time frames studied. For a general reader, the takeaway is that myelin health is part of the story, but not the whole story: simply stripping insulation from nerve fibers does not automatically reproduce the selective vulnerability seen in Parkinson’s‑related conditions. Other features of at‑risk pathways—such as very fine axons, dense branching of synapses, and high energy demands—may interact with myelin status to shape where and when harmful protein clumps emerge.
Citation: Clark, R.N., Landes, R.E., Abbas, M. et al. Testing an inverse link between limbic alpha-synucleinopathy and myelin markers in mice and humans. npj Parkinsons Dis. 12, 77 (2026). https://doi.org/10.1038/s41531-026-01278-y
Keywords: Parkinson’s disease, Lewy body disorders, myelin, alpha-synuclein, limbic system