Clear Sky Science · en
Persistence of alveolar fibroblast-derived ADAMTS4+ cells in a preclinical model of delayed pulmonary fibrosis resolution
Why lung scars matter
When lungs are injured, they can heal with scar tissue, much like skin after a deep cut. In some people, especially older adults, this scarring spirals out of control and hardens the lungs, a condition known as idiopathic pulmonary fibrosis. Breathing becomes increasingly difficult, and the damage rarely reverses. This study asks a deceptively simple question with big medical consequences: why do lung scars fade in some situations but stubbornly persist in others, and can we nudge the lung back toward healing instead of permanent scarring? 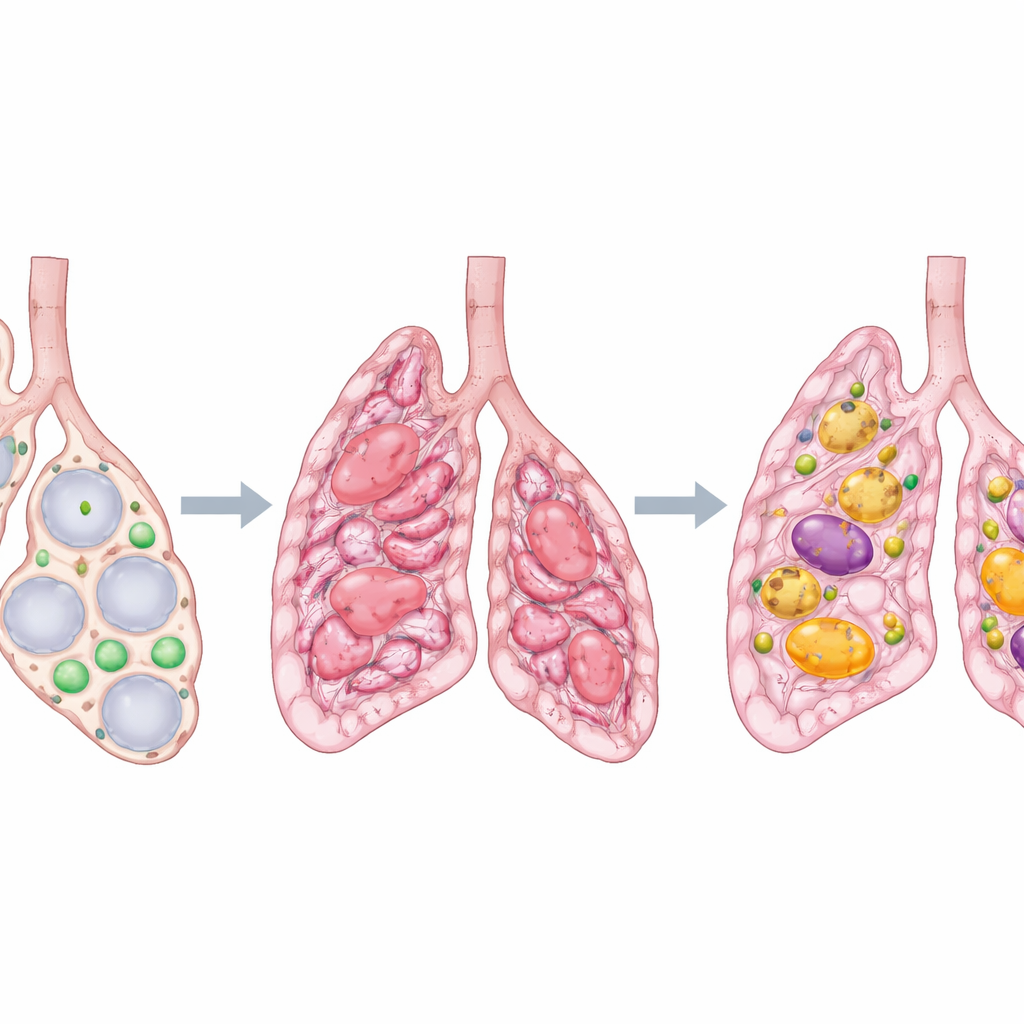
Hidden helpers in the air sacs
Deep in the lung’s tiny air sacs, special support cells live next to the cells that handle gas exchange. These support cells, called lipofibroblasts, store fat droplets and help keep the air sacs healthy. Earlier work showed that, when the lung is injured, lipofibroblasts can transform into myofibroblasts—cells that pull tissues tight and lay down thick fibers, forming scar tissue. In young mice, many of these scar-forming cells can later switch back into lipofibroblasts, helping the lung’s structure recover. But in human disease, this reversal seems to fail, and the scar keeps growing.
Studying scarring in aging lungs
To better mimic human disease, the researchers used older mice and tracked lipofibroblast-related cells over time after a chemical injury that causes lung fibrosis. With advanced microscopy and single-cell RNA sequencing, they followed how these cells changed identity during peak scarring and later recovery phases. They found that lipofibroblasts do indeed turn into myofibroblasts during active scarring, and that some later revert, helping to rebuild a more normal tissue. However, this recovery in aged mice was slow and incomplete, leaving behind patches of damaged lung even after structural improvements. 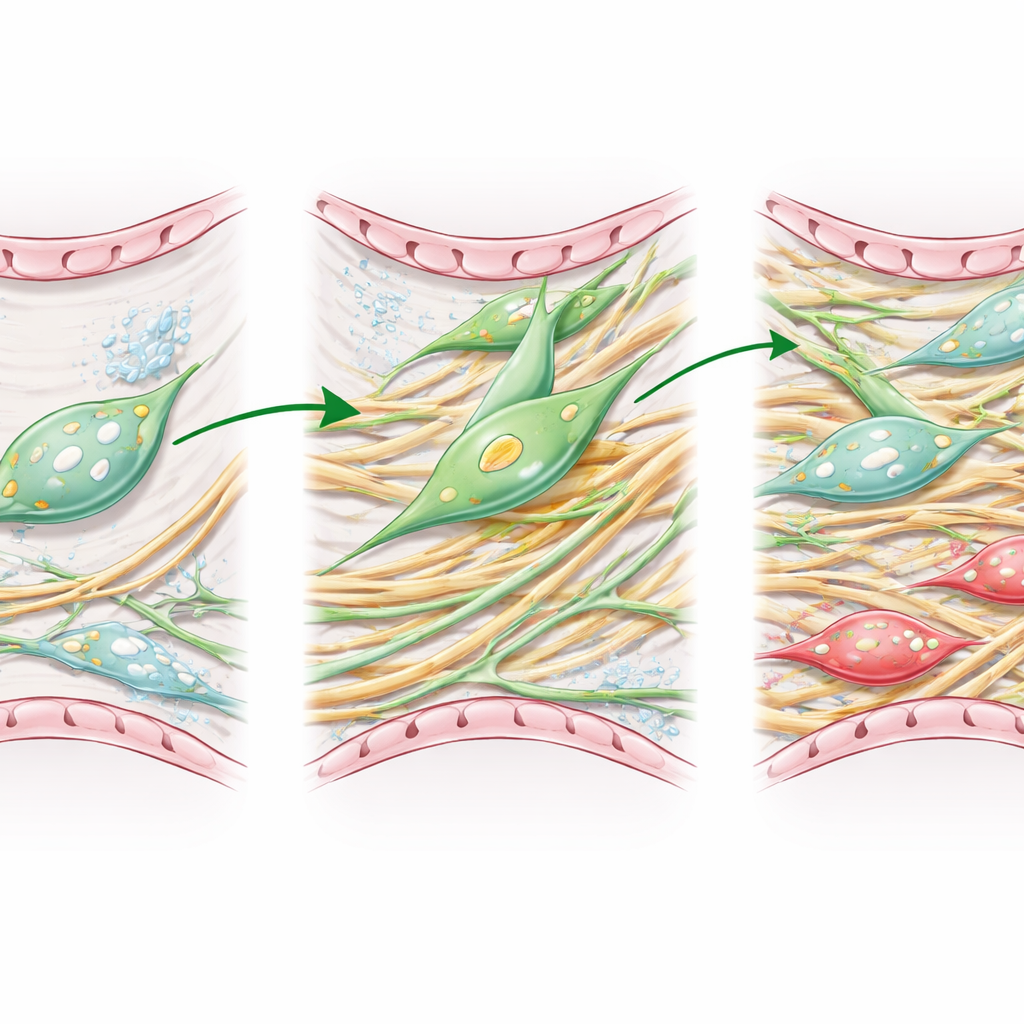
A persistent troublemaker cell type
Diving deeper into the cell data, the team noticed a group of fibroblast-derived cells marked by a protein-cutting enzyme called ADAMTS4. These ADAMTS4-positive cells appeared as scars formed and, crucially, stayed around during the delayed healing phase. Rather than being the classic contractile scar cells, they were more similar to the alveolar support cells but with a harmful twist: they carried high ADAMTS4, which can chop up a large matrix molecule called versican. That breakdown product is known to attract immune cells and sustain inflammation. The authors proposed that these persistent ADAMTS4-rich cells help maintain a damaging, inflammatory environment that keeps lung scars from fully resolving.
From mouse lungs to human disease
The researchers did not stop at mice. They examined lung tissue from patients with idiopathic pulmonary fibrosis and compared it with healthy donor lungs. In the diseased lungs, genes linked to healthy lipofibroblast identity were reduced, while genes tied to myofibroblasts and ADAMTS4 were increased. Single-cell and spatial transcriptomic maps of human lungs showed fewer normal alveolar support cells and more ADAMTS4-rich, scar-associated regions. In precision-cut lung slices from both mice and humans, the team then tested ways to block ADAMTS4 activity, either with a broad natural inhibitor protein (TIMP-3), extra versican, or small interfering RNA that reduced ADAMTS4 production. In each case, markers of scarring went down and markers of healthier lung tissue were partly restored.
Toward new ways to unwind lung scars
Put simply, this study shows that a reversible switch between fat-storing support cells and scar-forming cells helps decide whether lung fibrosis worsens or eases. In aging lungs, a subset of fibroblast-derived cells that carry high levels of the enzyme ADAMTS4 linger in damaged areas and seem to lock the lung into a state of chronic scarring and inflammation. By dialing down ADAMTS4 or altering its interaction with the surrounding matrix, the researchers could soften these scars in preclinical models. While more work is needed before treatments reach patients, the findings spotlight ADAMTS4-positive fibroblast-like cells as a promising target to help the lung move away from permanent scarring and back toward true repair.
Citation: Zabihi, M., Khadim, A., Lingampally, A. et al. Persistence of alveolar fibroblast-derived ADAMTS4+ cells in a preclinical model of delayed pulmonary fibrosis resolution. Nat Commun 17, 4205 (2026). https://doi.org/10.1038/s41467-026-72419-3
Keywords: idiopathic pulmonary fibrosis, lung fibroblasts, tissue scarring, aging lung, ADAMTS4