Clear Sky Science · en
Repeated restraint stress-induced increase in post-surgical somatosensory hypersensitivity and affective responding is mediated by β-adrenergic receptor activation and spinal NLRP3-IL1β signalling in male rats
Why Stress Matters After Surgery
Many people feel stressed or low before an operation, and doctors know that such feelings can make recovery harder and more painful. This study used rats to explore a key question: how does long‑lasting stress before surgery change the body’s pain system so that pain after an operation becomes stronger, lasts longer, and feels more emotionally overwhelming?
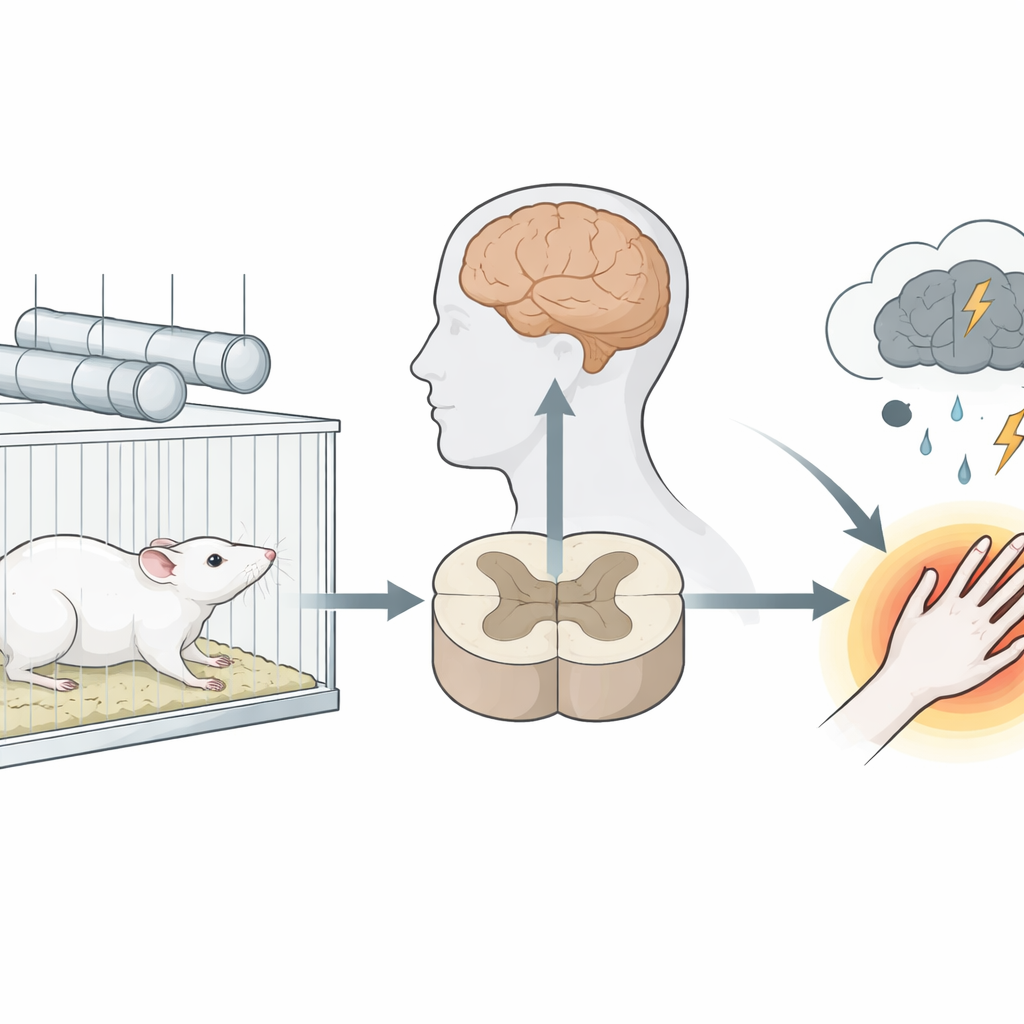
Building a Model of Stress and Surgery
To mimic chronic life stress, the researchers put male rats into snug restraining tubes for six hours a day over three weeks. This did not injure the animals, but it prevented normal movement and reliably triggered a stress response. The stressed rats showed several signs resembling aspects of human depression and chronic stress: they gained less weight, had higher levels of a stress hormone in their droppings, and spent more time immobile in a standard test of despair‑like behavior. After this stress period, all rats received a small cut on one hind paw, a well‑established model of surgical injury that normally causes soreness which fades within about a week.
Stronger Pain and Darker Moods
Compared with non‑stressed rats that had the same paw incision, the stressed animals reacted more strongly to touch and heat on the injured paw, and this sensitivity lasted several days longer. But the difference was not just in bodily sensation. Using a series of behavioral tests, the team showed that surgery made rats more anxious and more likely to avoid unpleasant touch, and that prior stress magnified these emotional responses. Stressed, operated rats were willing to leave a dark, safe area and spend more time in a bright, exposed zone if it allowed them to avoid painful stimulation, suggesting that pain had become more intensely aversive and emotionally charged.
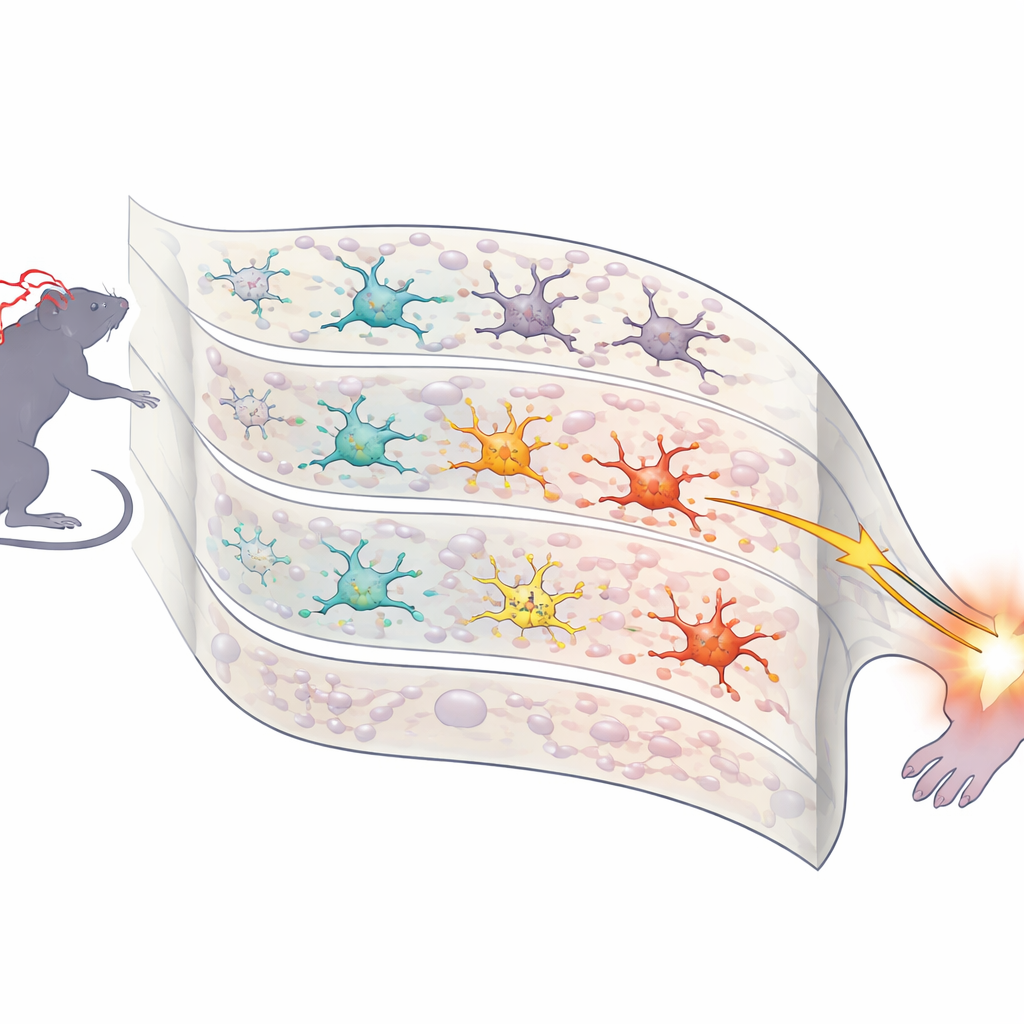
What Changes Inside the Spinal Cord
The spinal cord is a key relay between the body and the brain, and it contains immune‑like cells called microglia that help shape pain signals. By examining spinal tissue from the rats, the researchers found that combining chronic stress with surgery altered the activity of hundreds of genes, especially those linked to wound healing and the behavior of glial cells. A particular alarm system, known as the NLRP3–IL‑1β inflammasome, stood out. This pathway helps control the release of potent inflammatory messengers. In stressed, operated rats, markers of microglia and of this inflammasome were elevated, and microscopic images showed stronger staining of these cells on the side of the spinal cord connected to the injured paw.
Blocking the Pain‑Priming Pathway
To test whether this spinal alarm system actually drives the worse pain, the team injected drugs directly around the spinal cord. One drug blocked NLRP3, and another blocked the receptor for IL‑1, one of its key messengers. Both treatments reduced stress‑related increases in pain avoidance and touch sensitivity after surgery, without bluntly eliminating normal pain in non‑stressed animals. The scientists also probed how stress hormones shape this process. Blocking the classical stress hormone receptor for cortisol‑like signals prevented the despair‑like behavior caused by restraint, but did not stop stress from worsening post‑surgical pain. In contrast, blocking β‑adrenergic receptors—targets of adrenaline‑like signals—using the common drug propranolol eased both the emotional changes and the extra pain after surgery in stressed rats.
What This Means for People Facing Surgery
Taken together, the findings suggest that ongoing stress can “prime” spinal immune cells through adrenaline‑linked signals so that when a surgical injury occurs, these cells overreact, release inflammatory messengers, and amplify both the sharpness of pain and its emotional burden. While this work was done in male rats, and many steps remain before any direct treatment changes, it highlights biological links between mood, stress, and post‑surgical pain. In the future, carefully timed use of drugs that calm β‑adrenergic signaling or dampen specific spinal immune pathways might help protect vulnerable patients from developing long‑lasting, hard‑to‑treat pain after surgery.
Citation: Bella, A., Abdallah, K., Rodrigues-Amorim, D. et al. Repeated restraint stress-induced increase in post-surgical somatosensory hypersensitivity and affective responding is mediated by β-adrenergic receptor activation and spinal NLRP3-IL1β signalling in male rats. Neuropsychopharmacol. 51, 1032–1044 (2026). https://doi.org/10.1038/s41386-025-02305-x
Keywords: post-surgical pain, chronic stress, microglia, beta-adrenergic signaling, neuroinflammation