Clear Sky Science · en
OGT mediates O-GlcNAcylation of MEIS2 and affects palatal osteogenic development
Why this research matters for growing faces
Cleft palate is one of the most common birth defects affecting babies’ mouths and faces. It can make feeding, speech, and later dental health much more difficult, and today doctors can only treat it after it appears. This study asks a deeper question: what goes wrong at the microscopic level while the palate bones are forming in the embryo, and could understanding those hidden processes one day help prevent clefts from forming in the first place?
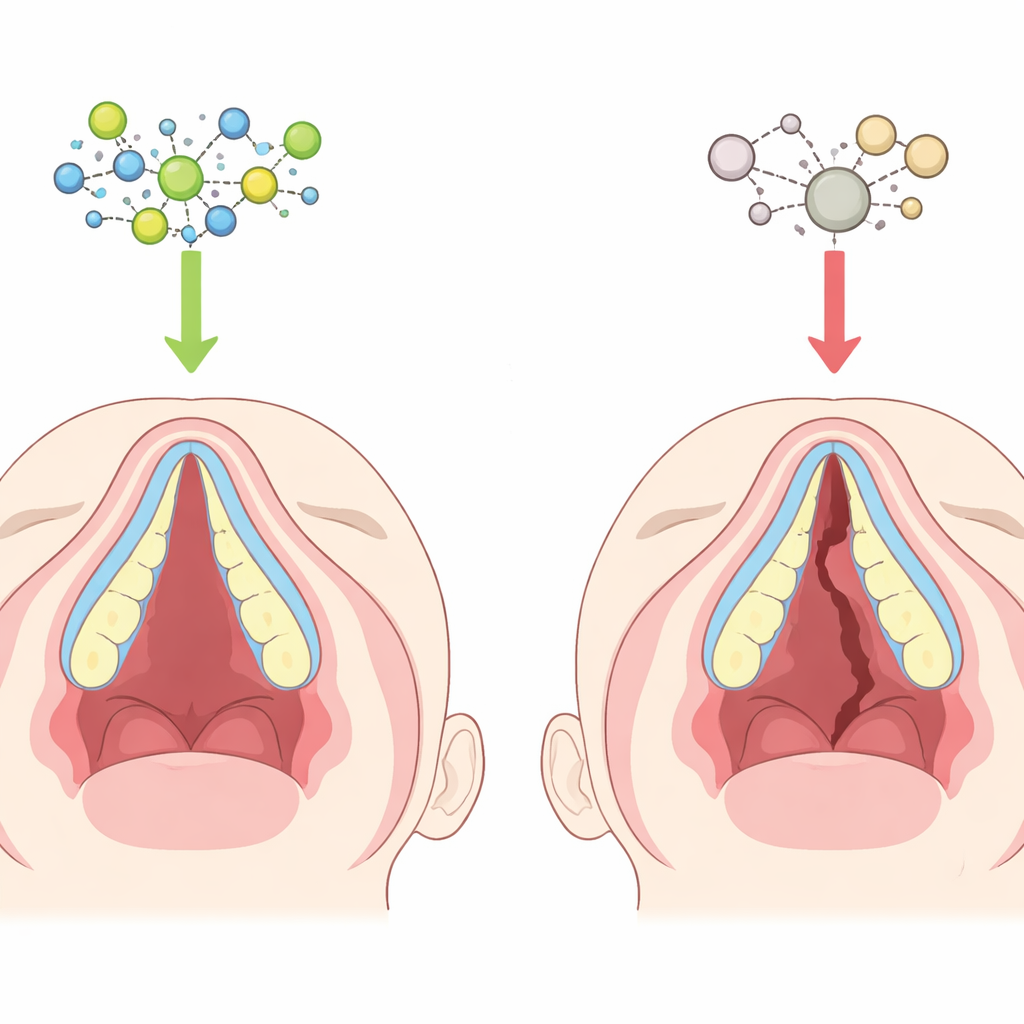
How the palate normally takes shape
In early development, two shelves of tissue grow inward from the sides of the upper jaw, rise up beside the tongue, and then meet and fuse in the middle to create the roof of the mouth. Inside these shelves, soft embryonic cells gradually turn into bone cells that build the hard palate. If the shelves fail to grow, move, meet, or harden properly, a gap can remain, producing a cleft. The front part of the palate forms directly from soft tissue turning into bone, a process that must be timed and controlled very precisely. Subtle disruptions in this timing can leave the palate covered by skin and mucosa but poorly supported by bone.
A tiny sugar tag with a big developmental role
The authors focus on a chemical "tag" called O-GlcNAc, a small sugar that cells can attach to many different proteins to fine-tune their behavior. A single enzyme, O-GlcNAc transferase (OGT), adds this tag, acting as a kind of molecular switchboard that responds to the cell’s nutrient and stress status. In mouse embryos exposed to all-trans retinoic acid, a compound that reliably causes cleft palate, the team found that both O-GlcNAc tags and OGT levels were sharply reduced in the developing palate. This suggested that when this sugar-tagging system is dialed down, the palate may struggle to form normal bone.
Lessons from fish and human palate cells
To test whether this sugar tag is truly important for building the palate, the researchers turned to zebrafish, whose craniofacial development closely mirrors key aspects of mammals. When they blocked OGT or chemically inhibited O-GlcNAc in zebrafish embryos, the fish developed much higher rates of cleft-like gaps in the palate area and weaker mineralization of a central cranial bone. Supplying extra ogt genetic material partially rescued these defects, strengthening the link between O-GlcNAc and healthy palate formation. In parallel, the team used human embryonic palatal mesenchymal (HEPM) cells—cells similar to those that form the human hard palate. Reducing OGT in these cells did not stop them from dividing, but it did blunt their ability to turn into bone-forming cells and to lay down mineral deposits, confirming that the sugar-tagging system is directly tied to bone-building capacity.
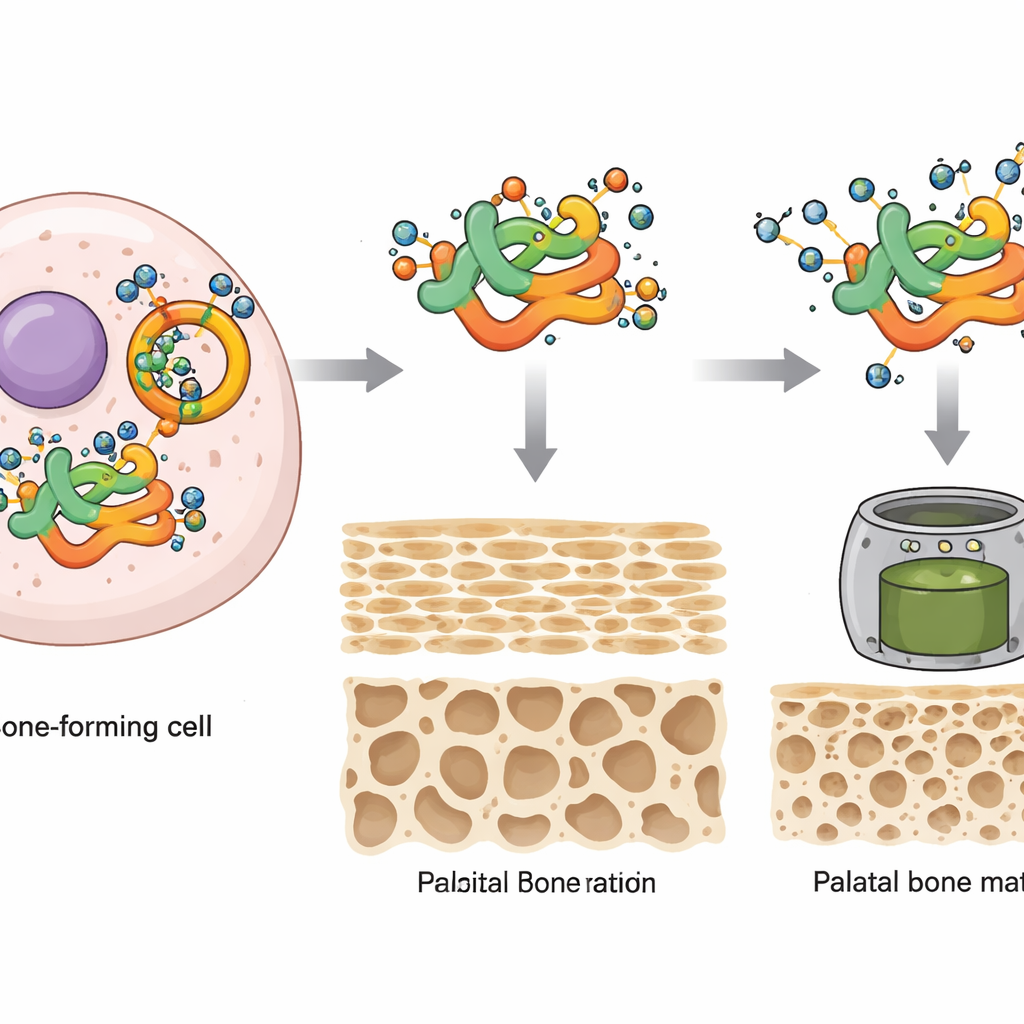
Protecting a key “architect” protein from being trashed
The study then zoomed in on a specific protein called MEIS2, a DNA-binding factor already known to be crucial for craniofacial development and linked to cleft palate in children when mutated. The authors discovered that MEIS2 physically associates with OGT and carries O-GlcNAc tags at a particular amino-acid position (called Ser237 in mammals). When this site was altered so that it could no longer be tagged, MEIS2 lost most of its sugar modification. Without proper O-GlcNAc tagging, MEIS2 protein levels fell rapidly, not because its gene was turned off, but because the protein was more heavily marked for destruction by the cell’s ubiquitin–proteasome “shredder” system. Tagging by O-GlcNAc therefore acts as a shield that stabilizes MEIS2 and prevents it from being prematurely broken down.
Connecting the dots to bone-building genes
Stabilized MEIS2 does more than just exist—it turns on other genes. One of its important targets is SHOX2, another regulator strongly implicated in hard palate development. The team showed that MEIS2 binds to the control region of the SHOX2 gene and boosts its activity, while loss of OGT, or mutation of the MEIS2 sugar-tagging site, weakens this activation. In HEPM cells lacking OGT, reintroducing normal MEIS2 restored bone-forming markers and mineral deposits, but a MEIS2 version that could not carry the sugar tag did not. In zebrafish, extra meis2 mRNA could rescue palatal bone defects caused by ogt loss, whereas a tag-deficient version again failed. Together, these experiments outline a clear chain: OGT adds sugar tags to MEIS2, which keeps MEIS2 stable, which in turn activates SHOX2 and other bone genes, allowing palate bone to form properly.
What this means for future cleft palate care
In everyday terms, this work identifies a microscopic quality-control system that helps embryonic palate cells keep a key “architect” protein on the job long enough to build a solid bony roof of the mouth. When the sugar-tagging enzyme OGT is weakened—by genetic changes or environmental stresses—the MEIS2 protein is stripped and destroyed too quickly, bone-building instructions are not fully carried out, and the risk of cleft palate rises. While any clinical application is still far off, understanding this OGT–MEIS2–SHOX2 chain offers a new framework for thinking about how genes, nutrition, and chemical exposures intersect during facial development, and points toward molecular targets that might one day be used to better diagnose, predict, or even prevent some cases of cleft palate.
Citation: Zhang, Z., Shan, Z., Chen, X. et al. OGT mediates O-GlcNAcylation of MEIS2 and affects palatal osteogenic development. Int J Oral Sci 18, 32 (2026). https://doi.org/10.1038/s41368-026-00431-w
Keywords: cleft palate, craniofacial development, post-translational modification, O-GlcNAcylation, MEIS2