Clear Sky Science · en
Ref-1 drives ulcerative colitis induced systemic defects in hematopoietic cells
Why gut disease can affect your blood
Ulcerative colitis is usually thought of as a disease of the large intestine, causing pain, bleeding, and frequent trips to the bathroom. This study shows that the impact of long lasting gut inflammation can reach all the way to the bone marrow, the factory that makes new blood cells. By tracing how signals from an inflamed colon reshape blood formation, the researchers also test drugs that may help restore balance in both the gut and the blood.
When gut trouble talks to bone marrow
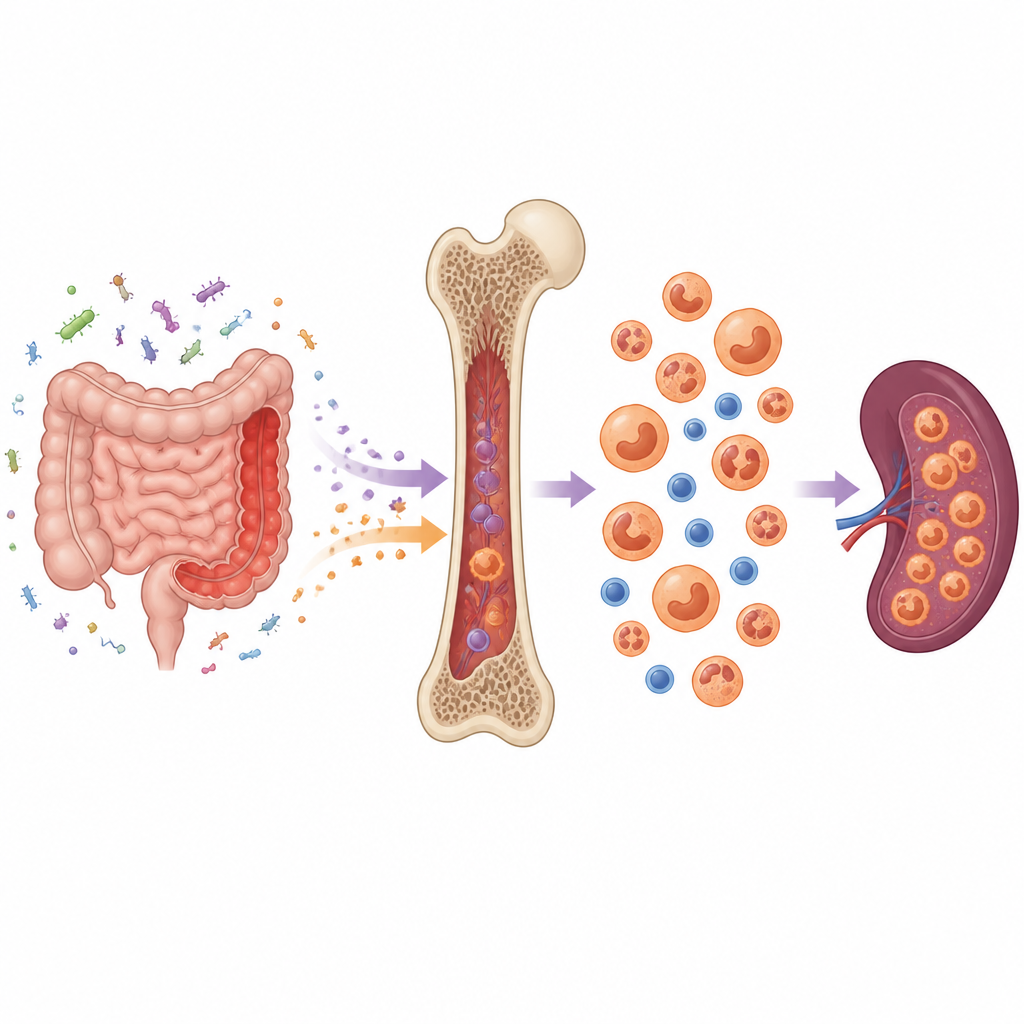
In ulcerative colitis, the immune system overreacts to microbes in the gut, damaging the intestinal lining and allowing bacterial products and inflammatory molecules to leak into the bloodstream. The team used a mouse model that mimics chronic ulcerative colitis in people. They found that this ongoing intestinal inflammation caused the bone marrow to become overloaded, with more total cells and an enlarged pool of early blood forming cells. Instead of quietly renewing themselves, these stem and progenitor cells became more active, cycling faster and dying less often.
From balanced blood to a myeloid tilt
Normally, stem cells in the marrow generate a mix of white blood cells, red blood cells, and platelets. In the colitis prone mice, this balance shifted. Early precursors were pushed to make more myeloid cells, such as neutrophils and inflammatory monocytes, at the expense of other lineages like lymphocytes and red cell precursors. Similar changes appeared in the spleen, which became enlarged and began acting as a backup site of blood production. These changes created a feedback loop, feeding more inflammatory cells back to the diseased intestine.
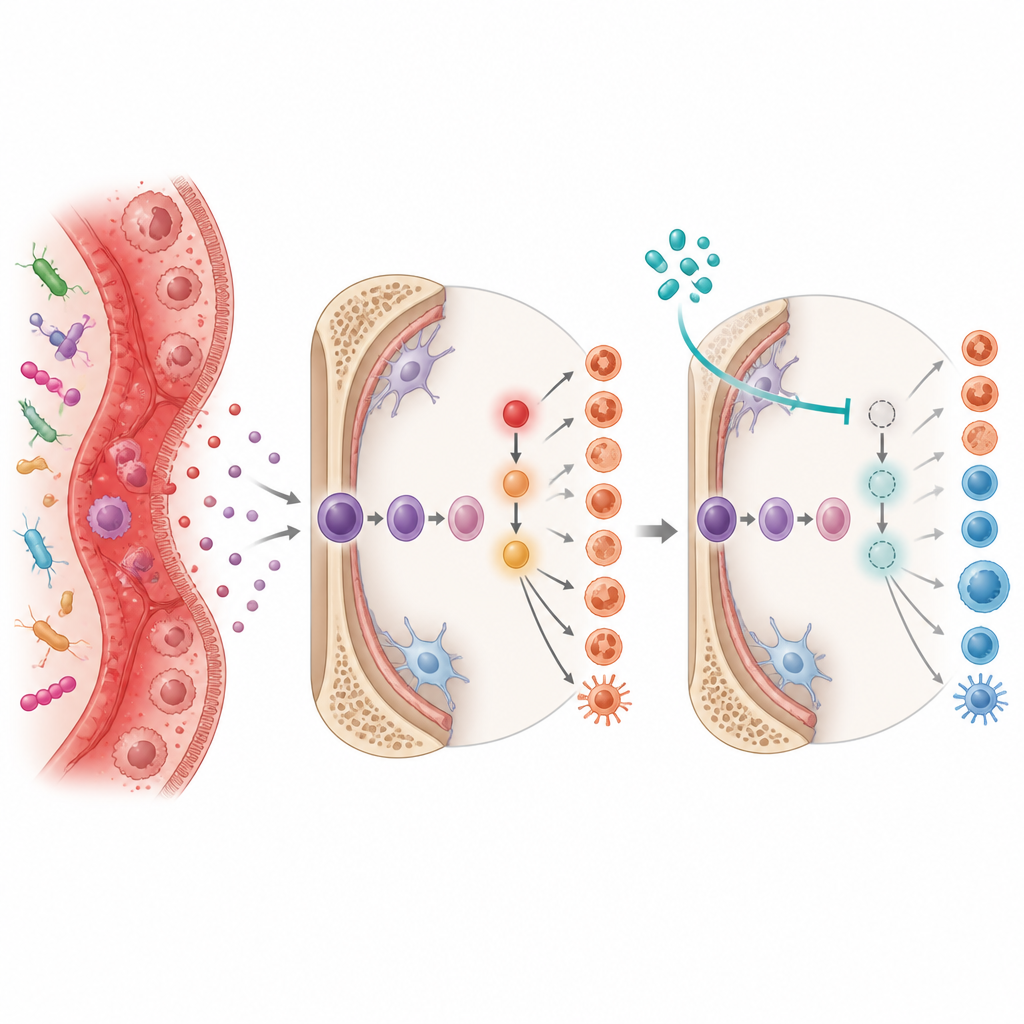
A redox switch at the heart of the problem
The researchers dug into the molecular switches behind this skewed blood production. They focused on a protein called Ref 1, which helps control how other proteins respond to changes in the cell’s chemical environment. In colitis, Ref 1 activity was linked to high levels of the growth factor G CSF and to the activation of HIF 1 alpha, a sensor of low oxygen that also responds to inflammation. Together these signals turned on receptors for the alarm molecule interleukin 1 on stem and progenitor cells, nudging them toward repeated cycles of inflammatory myeloid production.
Turning the switches back down
To see if this signaling cascade could be interrupted, the team treated colitis mice with two drugs. APX3330 blocks the redox, or oxidation reduction, function of Ref 1, while echinomycin interferes with HIF 1 alpha. Both treatments were given during the development of chronic colitis. In each case, the drugs reduced signs of gut disease, shrank enlarged spleens, and restored a healthier mix of stem cells and mature blood cells in bone marrow and spleen. In transplant experiments, bone marrow from drug treated colitis mice engrafted better and led to longer, healthier colons in recipient animals, showing that correcting stem cell behavior alone could ease intestinal damage.
What this means for people with ulcerative colitis
Overall, this work reveals a pathway by which chronic gut inflammation can reprogram the body’s blood forming system into a self reinforcing inflammatory state. By identifying Ref 1, HIF 1 alpha, and the interleukin 1 receptor as key steps in this chain, the study suggests that drugs targeting these molecules might one day help not only calm intestinal symptoms but also reset unhealthy blood cell production. While these findings are in mice and not yet treatments for patients, they highlight how closely the gut and bone marrow are connected and point toward new ways to think about managing long term inflammatory bowel disease.
Citation: Kumar, R., Kanumuri, R., Burns, S.S. et al. Ref-1 drives ulcerative colitis induced systemic defects in hematopoietic cells. Commun Biol 9, 635 (2026). https://doi.org/10.1038/s42003-026-09860-z
Keywords: ulcerative colitis, bone marrow, hematopoiesis, inflammation, stem cells