Clear Sky Science · en
Uterine rupture risk during trial of labor after one cesarean in a population-based cohort study of induction method and labor management
Why this matters for growing families
More and more babies around the world are born by cesarean section, which means many women face a key decision in a later pregnancy: try for a vaginal birth or plan another cesarean. One rare but serious complication during a vaginal birth after a previous cesarean is a tear in the scar on the uterus, called uterine rupture. This Swedish study asks a question that matters deeply to parents and clinicians alike: when labor needs to be started or helped along, which methods appear safer for the scarred uterus?
A closer look at birth after a previous cesarean
The researchers used detailed medical records from all eight delivery units in the Stockholm–Gotland region of Sweden between 2008 and mid‑2020. They focused on 11,947 women who had exactly one prior cesarean, were carrying a single baby in head‑down position, had reached full term, and chose to attempt labor rather than schedule a repeat operation. In this real‑world group, about 2 in 100 women experienced a uterine rupture, a rate higher than that seen in broader mixed populations but likely more realistic for first‑time attempts at vaginal birth after cesarean.
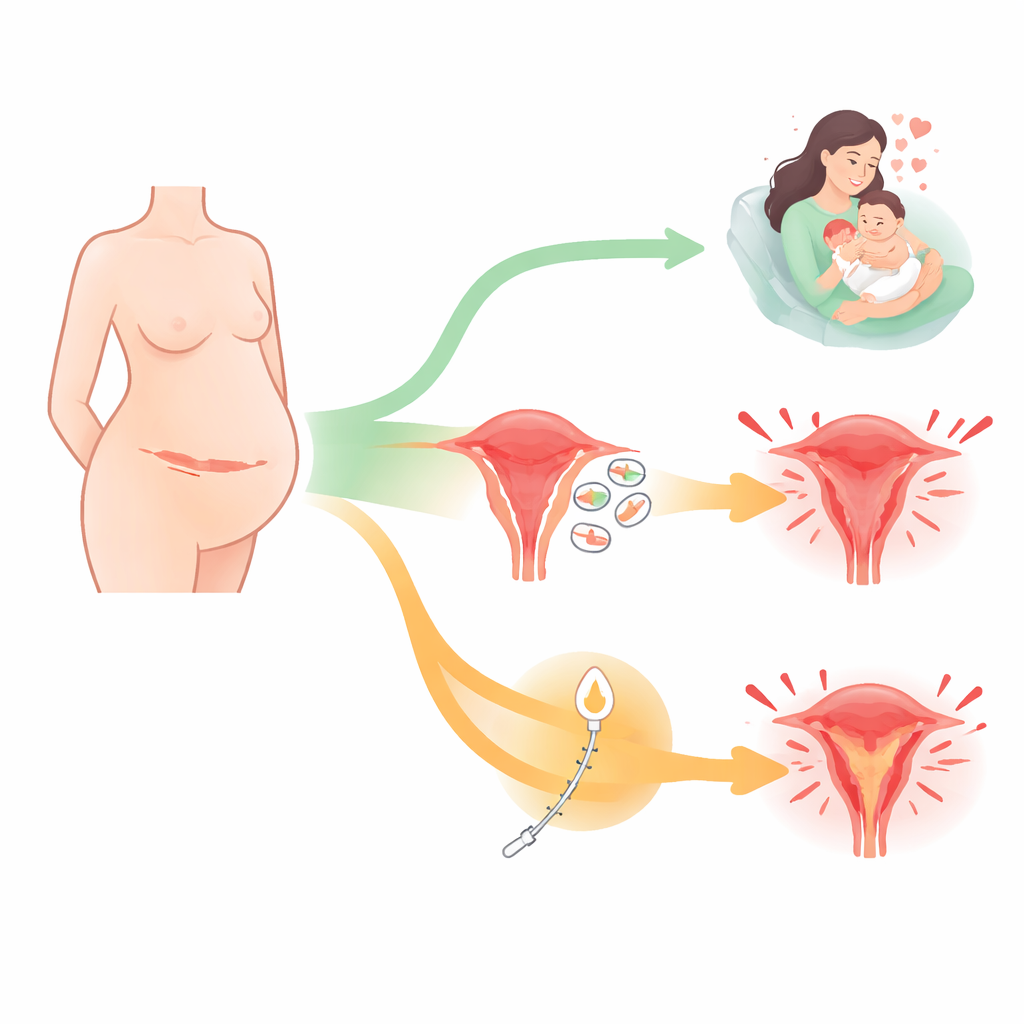
How labor was started or supported
Most women in the study went into labor on their own; just over one in five had labor induced. Doctors used two broad approaches to induction: medications called prostaglandins, which soften the cervix and stimulate contractions, and a mechanical technique using a small balloon catheter placed through the cervix. Many women, regardless of how labor began, also received oxytocin, a drug that strengthens contractions. The team compared women who labored spontaneously with those who were induced, and then looked more closely at the different induction methods.
Which methods carried more risk
When the researchers adjusted for factors such as age, body size, pregnancy length, and hospital, women whose labor was induced had about 1.6 times higher odds of uterine rupture than those who went into labor naturally. The type of induction mattered. Among women given prostaglandins, about 4 in 100 had a rupture, and their adjusted odds were roughly two and a half times higher than those with spontaneous labor. In contrast, women induced with a balloon catheter had a rupture rate similar to spontaneous labor. When the two induction methods were compared directly, prostaglandin use was linked to about three times higher odds of rupture than balloon induction, even after accounting for how “ready” the cervix was at the start.
What this meant for newborns and mothers
When a uterine rupture did occur, the consequences for babies could be severe. Newborns whose mothers had a rupture were far more likely to have signs of oxygen shortage around birth, including very low Apgar scores, dangerously low blood pH, seizures, and brain injury due to lack of oxygen. The odds of these problems were often 10 to 20 times higher than in births without rupture. Mothers with rupture also had more heavy bleeding and were more likely to need removal of the uterus to control the situation. These patterns held even when the researchers used a stricter definition focusing only on the most serious ruptures.
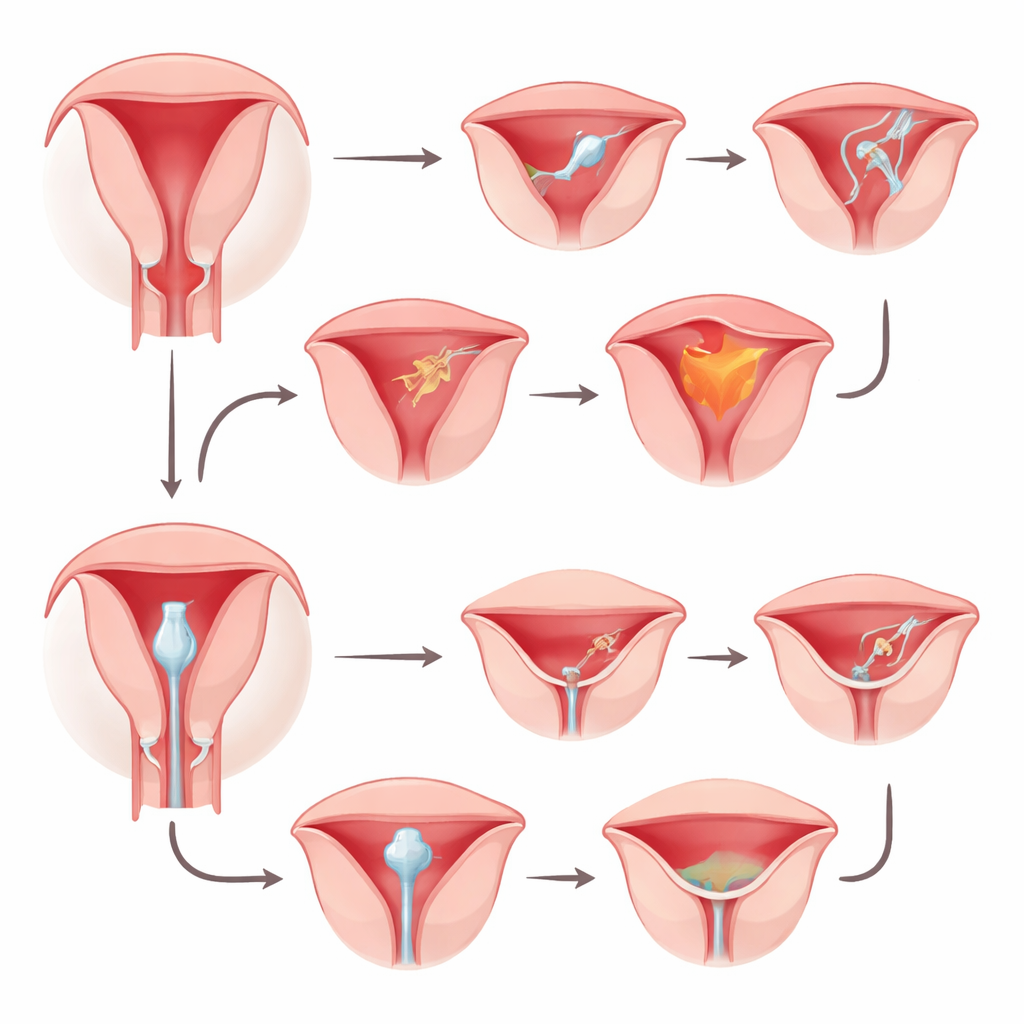
What this means for birth planning
For women with one previous cesarean who hope for a vaginal birth, this study suggests that going into labor naturally is the safest path for the scar on the uterus. When induction is truly necessary, methods that gently open the cervix with a balloon appear less risky for the old scar than prostaglandin medications, although careful monitoring remains essential in all cases. While no approach can eliminate risk, these findings help doctors and families have more informed conversations about how to start labor and balance safety for both mother and baby.
Citation: Roeck Hansen, C., Mantel, Ä., Hulthén-Varli, I. et al. Uterine rupture risk during trial of labor after one cesarean in a population-based cohort study of induction method and labor management. Sci Rep 16, 12473 (2026). https://doi.org/10.1038/s41598-026-48444-z
Keywords: uterine rupture, vaginal birth after cesarean, labor induction, prostaglandins, balloon catheter